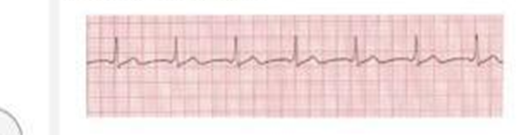
A patient's ECG monitor shows an accelerated junctional rhythm at a rate of 78 beats/minute. What is the nurse's priority intervention?
Administer ordered digoxin
Begin a continuous diltiazem infusion
Prepare for cardioversion
Continue monitoring the patient
The Correct Answer is D
A. Administer ordered digoxin: Digoxin enhances vagal tone and slows conduction through the AV node, primarily used for atrial fibrillation or heart failure with reduced ejection fraction. An accelerated junctional rhythm at 78 beats/min is within normal heart rate range and often does not require pharmacologic suppression.
B. Begin a continuous diltiazem infusion: Diltiazem is a calcium channel blocker that slows AV nodal conduction and is indicated for atrial tachyarrhythmias. An accelerated junctional rhythm at 78 beats/min is not tachycardic and is typically hemodynamically stable. Initiating a diltiazem infusion could lead to unnecessary bradycardia or hypotension.
C. Prepare for cardioversion: Synchronized cardioversion is reserved for unstable tachyarrhythmias such as atrial fibrillation with rapid ventricular response or supraventricular tachycardia causing hemodynamic compromise. An accelerated junctional rhythm at 78 beats/min is generally benign and often transient. Electrical cardioversion is not indicated in a stable patient with this rhythm.
D. Continue monitoring the patient: An accelerated junctional rhythm (rate 60–100 beats/min) often occurs due to increased automaticity of the AV junction, sometimes related to digoxin toxicity, ischemia, or post-cardiac surgery. If the patient is hemodynamically stable and asymptomatic, close monitoring and assessment for underlying causes are appropriate. Immediate intervention is not required unless instability develops.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
A. Stabilize the penetrating object: Stabilizing the object is important to prevent further internal injury and bleeding. However, immediate assessment of the patient’s vital signs takes priority to determine hemodynamic stability and guide emergent interventions. Life-threatening conditions must be identified before procedural measures.
B. Contact the health care provider: Notifying the provider is necessary for treatment planning, but it should occur after the nurse has rapidly assessed the patient’s condition. Vital signs provide critical information to communicate effectively about the patient’s urgency and status.
C. Obtain the client’s vital signs: Assessing vital signs is the priority because the patient’s agitation, disorientation, and altered memory may indicate hypovolemic shock, internal hemorrhage, or head injury. Early detection of hypotension, tachycardia, or hypoxia is essential to initiate lifesaving interventions immediately.
D. Have the unlicensed assistive personnel place wrist restraints: Restraints may be considered only if the patient poses a danger to self or others, and only after safety measures and assessments are completed. Applying restraints prematurely does not address potentially life-threatening physiologic instability.
Correct Answer is D
Explanation
A. Decorticate posturing involves flexion of the arms, wrists, and fingers with extension of the legs, indicating damage to the corticospinal tract above the brainstem. In the image, positioning 1 shows the patient with arms flexed at the elbows and wrists, hands toward the chest, and legs extended, which is characteristic of decorticate posturing. This occurs in response to noxious stimuli in patients with cortical or corticospinal tract injury.
B. This shows the decerebrate posturing involves extension and pronation of the arms and legs, indicating more severe brainstem injury. It usually occurs in people who are unconscious and unable to control their movements. It reflects serious injury to the brainstem or widespread brain dysfunction.
C. Decorticate posturing is an abnormal reflex body position that indicates severe brain injury or disruption of brain activity. Key Features include arms flexed tightly toward the chest, wrists and fingers clenched, legs extended straight and rigid as shown in image 1.
D. Decorticate posturing involves flexion of the arms, wrists, and fingers with extension of the legs, indicating damage to the corticospinal tract above the brainstem. In the image, positioning 1 shows the patient with arms flexed at the elbows and wrists, hands toward the chest, and legs extended, which is characteristic of decorticate posturing. This occurs in response to noxious stimuli in patients with cortical or corticospinal tract injury.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
