The nurse is preparing to suction the endotracheal tube (ETT) of a patient who is on a ventilator using a closed in-line system (see image below or in attachments). What action does the nurse take first?
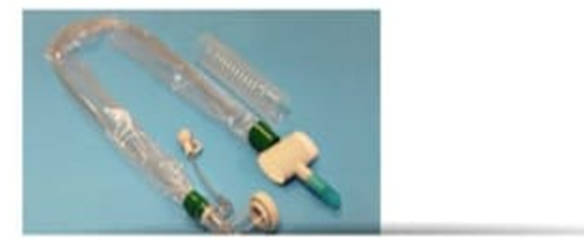
Remove the in-line suction system and use a sterile tracheostomy suctioning catheter
Place the in-line suction catheter into the ET tube and suction for 10 seconds
Disconnect the patient from the ventilator and oxygenate with the bag valve mask
Assess the patient’s respiratory status and oxygen saturation before suctioning
The Correct Answer is D
A. Remove the in-line suction system and use a sterile tracheostomy suctioning catheter: Removing the closed in-line suction system is unnecessary and breaks sterility. The closed system is designed to allow suctioning without disconnecting the ventilator, minimizing infection risk and oxygen desaturation.
B. Place the in-line suction catheter into the ET tube and suction for 10 seconds: Suctioning before assessing the patient could cause unnecessary hypoxia, trauma, or arrhythmias. The nurse must first determine the need for suctioning based on clinical assessment and oxygenation status.
C. Disconnect the patient from the ventilator and oxygenate with the bag valve mask: Disconnecting the ventilator is not indicated when using a closed in-line suction system. The closed system allows suctioning without loss of positive pressure or oxygenation, which prevents hypoxemia.
D. Assess the patient’s respiratory status and oxygen saturation before suctioning: The first step is to evaluate the patient’s respiratory condition, including auscultation, respiratory rate, work of breathing, and SpO₂. This assessment ensures suctioning is indicated, identifies any potential complications, and allows for safe and effective removal of secretions.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["B","C","D"]
Explanation
A. Check the patient's temperature: Although assessing temperature is part of a full evaluation, fever is not the priority concern in this scenario. The patient’s moist cough, jugular venous distention, and dyspnea suggest acute fluid overload and worsening heart failure rather than infection. Immediate cardiopulmonary assessment takes precedence.
B. Assess the pulse oximetry reading: Dyspnea and signs of volume overload raise concern for pulmonary edema and impaired oxygenation. Measuring oxygen saturation provides rapid, objective data about respiratory compromise and guides urgent interventions such as oxygen therapy. Hypoxemia must be identified promptly to prevent respiratory failure.
C. Auscultate the lungs: Lung auscultation is essential to assess for crackles, which indicate fluid accumulation in the alveoli due to left-sided heart failure. Detecting pulmonary congestion supports clinical suspicion of fluid overload and helps determine severity, guiding immediate treatment decisions.
D. Contact the provider: The patient is exhibiting signs of acute decompensated heart failure while receiving IV fluids. Prompt provider notification is necessary to obtain orders to adjust or discontinue fluids and initiate diuretic therapy or other interventions to prevent worsening pulmonary edema.
E. Change the fluids to 0.45% sodium chloride: The nurse should not independently change the IV solution without a provider order. Additionally, switching to hypotonic fluids does not address the underlying issue of volume overload and could further complicate the patient’s condition.
F. Administer furosemide as ordered: Although loop diuretics are commonly used in fluid overload, administration depends on an existing order. Since the question prioritizes immediate assessment and escalation, verifying oxygenation and lung status and notifying the provider are the top initial actions unless a standing order is already in place.
Correct Answer is C
Explanation
A. Gemfibrozil: Gemfibrozil is a lipid-lowering medication used to treat hypertriglyceridemia. It has no role in reversing anticoagulation or controlling acute bleeding and would not be appropriate.
B. Vitamin K: Vitamin K is the antidote for warfarin (Coumadin) toxicity but does not reverse the effects of heparin. Administering vitamin K would not stop heparin-induced bleeding and could delay proper treatment.
C. Protamine sulfate: Protamine sulfate is the specific antidote for heparin. It binds to heparin, neutralizing its anticoagulant effect, and is indicated in cases of serious bleeding, such as frank hematuria, as seen in this patient. Prompt administration can prevent further hemorrhagic complications.
D. Thromboplastin: Thromboplastin is used in laboratory testing to assess coagulation (PT/INR or aPTT) but is not a therapeutic agent for reversing anticoagulation. It cannot be administered to stop heparin-induced bleeding and is not appropriate in this clinical situation.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
