A 40 week primipara client is currently being monitored by external fetal monitoring. The monitor alerts for an ominous sign of fetal hypoxia. The nurse is assessing the strip. Based on the following strip, how would the nurse document the fetal heart rate?
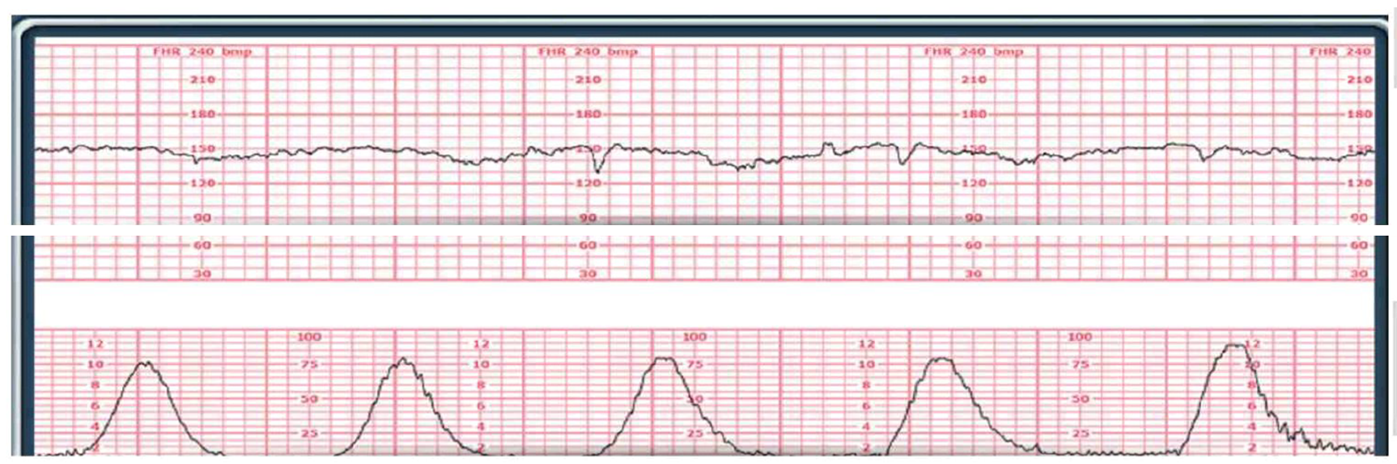
Bradycardia, Moderate variability, Present accelerations, Late decelerations.
Normal baseline, Moderate variability, Absent accelerations, Early decelerations.
Normal baseline, Minimal variability, Present accelerations, Early decelerations.
Normal baseline, Minimal variability, Absent accelerations, Late decelerations.
The Correct Answer is D
Choice A rationale: This is incorrect because the baseline FHR is approximately 140–145 bpm, which falls within the normal range of 110–160 bpm and is not bradycardia (defined as less than 110 bpm). Although late decelerations are present—an ominous sign of uteroplacental insufficiency and fetal hypoxia—the variability is minimal rather than moderate, and there are no accelerations visible on the tracing.
Choice B rationale: This is incorrect because the baseline FHR variability is minimal, with an amplitude range of ≤5 bpm, not moderate (6–25 bpm). The fluctuations are barely perceptible. In addition, the decelerations are late, not early. Early decelerations are symmetric, gradual dips in FHR that mirror contractions and are generally benign, caused by fetal head compression.
Choice C rationale: This is incorrect because there are no accelerations (abrupt increases of ≥15 bpm lasting ≥15 seconds) present on the strip. Furthermore, the decelerations are late, not early. Late decelerations are symmetric, gradual decreases in FHR that begin after the peak of the contraction and return to baseline only after the contraction ends, which is indicative of uteroplacental insufficiency.
Choice D rationale: This is the most accurate documentation. The baseline FHR is 140–145 bpm, which is normal. The tracing shows minimal variability (≤5 bpm), and when this finding is coupled with late decelerations, it is highly concerning for fetal hypoxemia or acidemia, consistent with a Category III tracing. The absence of accelerations further supports the presence of uteroplacental insufficiency and fetal compromise.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Choice A rationale
Early decelerations are not indicative of increased fetal intracranial pressure. They are characterized by a gradual decrease in fetal heart rate (FHR) that mirrors the contraction, with the nadir of the deceleration occurring at the peak of the contraction. This pattern is considered benign and is caused by fetal head compression during a uterine contraction, which stimulates the vagus nerve and results in a transient, brief decrease in FHR.
Choice B rationale
The term "present decelerations" is not a recognized classification for fetal heart rate patterns. Fetal heart rate (FHR) decelerations are categorized as early, late, or variable, each corresponding to a different underlying physiological cause. Passage through the cervix is a mechanical process; while it causes head compression, the resulting FHR change is the early deceleration pattern.
Choice C rationale
The term "absent deceleration" is not a specific fetal heart rate pattern. A baseline fetal heart rate that remains within the normal range of 110 to 160 beats per minute (bpm) with no periodic changes (decelerations or accelerations) is a normal finding. Fetal movement is primarily assessed by accelerations in the FHR, which are increases of at least 15 bpm lasting 15 seconds or more.
Choice D rationale
Variable decelerations are characterized by an abrupt decrease in FHR, often V or W-shaped, varying in duration and depth, and not consistently related to uterine contractions. They are the most common pattern in the second stage and indicate a transient occlusion of the umbilical cord, leading to a temporary decrease in umbilical blood flow and thus fetal oxygenation.
Correct Answer is C
Explanation
Choice A rationale
Moving the client to the operating room for a cesarean section is an invasive, definitive intervention reserved for cases where conservative measures have failed to resolve non-reassuring fetal status or in the case of a fetal heart rate category III tracing. This is not the priority initial action for uteroplacental insufficiency, which can often be corrected by less invasive maneuvers to optimize fetal oxygenation. The initial steps are less aggressive.
Choice B rationale
Administering oxygen to the mother via a non-rebreather face mask at a high flow rate (e.g., 8-10 L/min) can mildly increase the partial pressure of oxygen in the maternal blood, thus potentially improving the amount of oxygen crossing the placenta to the fetus. While often a component of intrauterine resuscitation, optimizing the maternal-fetal blood flow via position change is typically the initial, most effective action.
Choice C rationale
Turning the client to the left or right lateral position (or asking the client to turn) is the priority action because it relieves compression of the vena cava and aorta by the gravid uterus. This action, known as intrauterine resuscitation, increases venous return to the heart, thus enhancing cardiac output, improving placental perfusion, and subsequently increasing oxygen delivery to the fetus, which is compromised in uteroplacental insufficiency.
Choice D rationale
Increasing the rate of a non-glucose-containing intravenous fluid such as Lactated Ringer's or normal saline (a bolus) is an intervention to improve maternal hydration and expand intravascular volume, which can help increase placental perfusion if hypotension is contributing to the insufficiency. However, volume expansion is generally secondary to the position change, which more directly addresses the mechanical compression causing decreased blood flow.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
