A nurse is educating a client with a flaccid bladder. Which focus is the nurse most likely to teach this client?
Habit training: Attempt voiding at specific time periods.
Bladder training: Delay voiding according to a preschedule timetable.
Credé’s maneuver: Apply gentle manual pressure to the lower abdomen.
Kegel exercises: Contract the pelvic muscles.
The Correct Answer is C
A flaccid bladder, also called a hypotonic or atonic bladder, is a condition where the bladder loses muscle tone and cannot contract effectively, leading to incomplete emptying and urinary retention. It is often caused by damage to the sacral spinal cord, peripheral nerves, or conditions such as diabetes mellitus and spinal cord injury. Because the bladder cannot generate enough pressure to expel urine, patients may experience overflow incontinence, frequent dribbling, and increased risk of urinary tract infections.
Rationale for correct answer:
3. Credé’s maneuver: Apply gentle manual pressure to the lower abdomen. A flaccid bladder, often caused by lower motor neuron spinal cord injuries, lost its muscle tone (detrusor areflexia) and cannot contract to push urine out. Credé’s maneuver involves manually pressing down on the bladder to physically force the urine out.
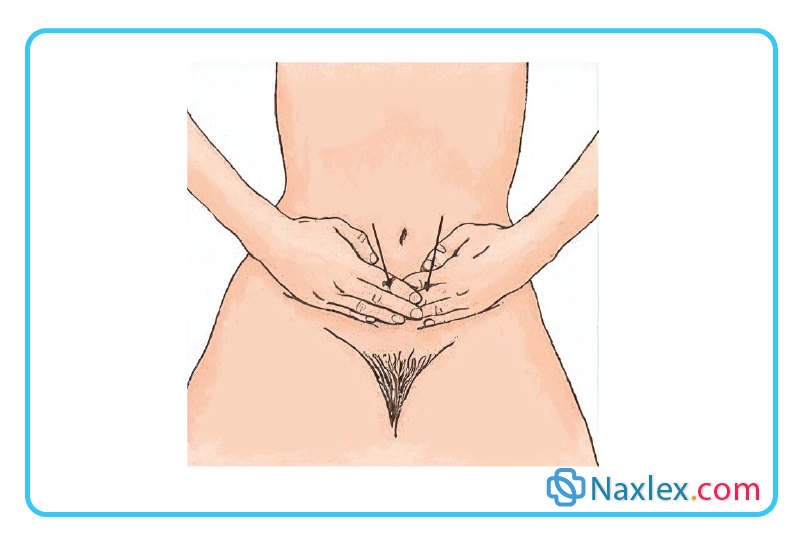
Rationale for incorrect answers:
1. Habit training: Attempt voiding at specific time periods. Habit training (or timed voiding) is typically used for clients with functional incontinence or those with cognitive impairments (like dementia). It relies on a schedule to keep the client dry but does not solve the physical emptying problem of a flaccid bladder.
2. Bladder training: Delay voiding according to a prescheduled timetable. Bladder training is the primary intervention for urge incontinence (overactive bladder). The goal is to “teach” the bladder to hold more urine for longer periods. In a flaccid bladder, the muscle is already too relaxed (underactive), so delaying voiding would only lead to dangerous over-distention.
4. Kegel exercises: Contract the pelvic muscles. Kegel exercises strengthen the pelvic floor to help with stress incontinence (leakage during coughing or sneezing). While healthy, they do not assist the detrusor muscle in a flaccid bladder to actually empty.
Test taking strategy:
- When you see the word “flaccid,” think “weak/no contraction.” If the muscle won't contract, you need an outside force to help.
- Options 1, 2, and 4 all require the bladder or pelvic muscles to have some level of functional snap or control.
- Only Option 3 provides a mechanical, external solution for a muscle that cannot move on its own.
Take home points:
- The priority for a flaccid bladder is preventing urinary retention and the resulting kidney damage due to hydronephrosis.
- In a flaccid bladder, the “pump” is broken. One must use external force (Credé’s maneuver) or a catheter to empty it.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["A","B","D","E"]
Explanation
Urinary incontinence is the involuntary leakage of urine, a common condition especially among women and older adults, caused by factors such as weakened pelvic muscles, overactive bladder, or obstruction, and it can present as stress, urge, mixed, overflow, or continuous incontinence; though not life-threatening, it significantly impacts quality of life and is managed through lifestyle changes, pelvic floor exercises, medications, or surgical interventions depending on severity and type.
Rationale for correct answers:
1. Perineal skin irritation: Chronic exposure to urine changes the skin's pH and creates a moist environment. This leads to incontinence-associated dermatitis, characterized by redness, itching, and skin breakdown. Assessing the skin is a priority to prevent secondary fungal infections or pressure ulcers.
2. Fluid Intake of Less than 1,500 mL/day: While it seems counterintuitive, patients with incontinence often restrict fluids to avoid “accidents.” However, low fluid intake leads to concentrated urine, which acts as a bladder irritant, increasing urgency and frequency. A healthy intake is typically 1,500–2,000 mL/day unless contraindicated.
4. History of frequent urinary tract infections (UTIs): A UTI is a leading cause of “transient” or acute incontinence. Inflammation of the bladder wall (cystitis) causes the bladder to become hyperactive, leading to a sudden, uncontrollable urge to void. Conversely, chronic incontinence can increase the risk of UTIs due to the use of pads or catheters.
5. A fecal impaction: The rectum and the bladder share the same pelvic floor space. An impacted mass of stool in the rectum can physically press against the bladder neck, obstructing flow (leading to overflow incontinence) or irritating the bladder (leading to urge incontinence). Relieving constipation often resolves the urinary issue.
Rationale for incorrect answers:
3. History of antihistamine intake: Many over-the-counter antihistamines have anticholinergic effects. These drugs can cause the bladder muscle (detrusor) to relax too much or the urethral sphincter to contract, leading to urinary retention.
Test taking strategy:
When faced with a “Select all that apply” (SATA) question regarding a symptom like incontinence, treat each option as a True/False statement and categorize them into two groups:
- Complications: Ask, “Is this a physical result of being incontinent?” (Choice 1 fits here).
- Etiologies (Causes): Ask, “Could this factor actually trigger or worsen bladder leakage?” (Choices 2, 4, and 5 fit here).
Take home points:
- Urinary incontinence assessment includes skin integrity, hydration, medications, infections, and bowel function.
- Many causes of incontinence are reversible, making thorough nursing assessment essential. Always look for the DIAPPERS acronym to find treatable causes.
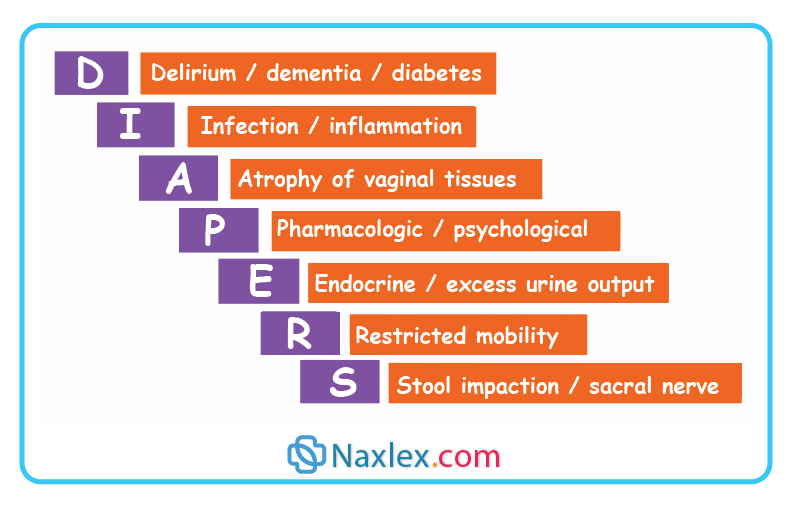
Correct Answer is B
Explanation
Collecting a urine specimen for routine urinalysis involves obtaining a clean, midstream sample to ensure accuracy and reduce contamination; the patient is instructed to wash their hands, cleanse the genital area, begin urinating into the toilet, then collect the midstream portion in a sterile container, sealing it promptly and labeling it correctly. The specimen should be delivered to the laboratory as soon as possible - ideally within one hour - or refrigerated if delayed, since prolonged standing can alter results.
Rationale for correct answer:
2. Results may be altered if a sample is left standing at room temperature for a long time: If urine sits at room temperature for longer than 1 hour, it begins to decompose. Bacteria multiply, the pH becomes more alkaline as urea converts to ammonia, and glucose levels may drop as bacteria consume it. If the sample cannot be sent to the lab immediately, it must be refrigerated.
Rationale for incorrect answers:
1. A sterile specimen is required for collection: A routine urinalysis does not require a sterile specimen. It is a clean procedure, not a surgical one. A sterile specimen is only required for a urine culture and sensitivity to identify specific bacteria.
3. The external meatus requires cleaning with antiseptic soap and water before voiding: While the area should be generally clean, the formal “antiseptic wipe” procedure is specifically for a clean-catch midstream specimen. For a routine urinalysis, the client can simply void into a clean container.
4. A clean-catch midstream specimen is necessary: While a clean-catch is the “gold standard” for avoiding contamination, it is not strictly necessary for a routine screening urinalysis. A simple “random” specimen is usually sufficient unless the provider specifically orders a clean-catch or a culture.
Test taking strategy
- In nursing exams, look for the answer that addresses specimen integrity.
- Options 1, 3, and 4 are “best practice” for cultures, but Option 2 is a universal rule for all urine samples.
Take home points:
- Urine is a living medium; to get accurate results for pH, nitrites, and bacteria, the lab must receive the specimen within 1 hour or it must be cooled to pause bacterial growth.
- Always distinguish between a routine urinalysis (tests for chemistry/blood/protein) and a culture (tests for specific bacteria).
- Cultures require sterile technique; routine urinalysis do not.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
