A nurse is preparing to collect a comprehensive general history from a patient scheduled for surgery. Which approach best demonstrates the nurse's application of effective data collection and prioritization during the assessment phase?
Begin by asking about the patient's current illness, including onset and symptoms, then proceed to review prior illnesses, surgeries, and hospitalizations before exploring psychosocial factors.
Ask only about medications and allergies since these directly affect surgical risk, leaving other history components for post-operative assessment.
Start with detailed questions about the patient's family medical history to identify genetic risks, then ask about lifestyle habits such as alcohol and tobacco use.
Focus primarily on objective data like vital signs and auscultation findings before gathering subjective information about symptoms and medical history.
The Correct Answer is A
Choice A reason: This structured approach follows the standard medical model for a comprehensive history, beginning with the Chief Complaint and History of Present Illness. Prioritizing the current condition and surgical history provides the most relevant data for immediate perioperative safety while ensuring that psychosocial factors are eventually addressed.
Choice B reason: While medications and allergies are high-priority items, focusing exclusively on them is insufficient for a comprehensive pre-operative assessment. Neglecting the patient's prior surgical experiences or chronic conditions could lead to missed complications, such as a history of malignant hyperthermia or undiagnosed respiratory or cardiovascular issues that affect anesthesia.
Choice C reason: Family history and lifestyle habits are important components of a health history, but they are generally lower in priority than the patient's current illness and past medical/surgical history when preparing for an imminent procedure. The assessment should be focused on identifying immediate risks to the patient's surgical outcome.
Choice D reason: The nursing process usually begins with gathering subjective data through the interview before proceeding to the objective physical examination. Subjective symptoms often guide the nurse on which objective assessments require more focus. Reversing this order may lead to an incomplete understanding of the patient's physiological and psychological state.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A reason: Active listening is a foundational component of all nursing interactions, but it requires the client to be verbalizing thoughts. When a client is tearful and struggling to find words (indecisive), the immediate priority is to provide a safe emotional space. Active listening should be paired with silence to allow the client the necessary time to process their emotions before they are expected to continue speaking.
Choice B reason: Therapeutic silence is the most appropriate intervention for an emotionally overwhelmed client. It demonstrates patience and empathy without pressuring the client to perform or answer questions immediately. This technique allows the client to regain composure and organize their thoughts, signaling that the nurse is comfortable with the client's emotional expression and is fully present in the moment to support them.
Choice C reason: Sharing information is a cognitive intervention that is often poorly timed when a client is in an emotional state. Providing facts or medical data while a client is tearful can be perceived as dismissive of their emotional distress. Information sharing should occur only after the client’s emotional needs have been acknowledged and they are in a more receptive psychological state.
Choice D reason: Clarifying questions are used to resolve ambiguities in communication, but asking them while a client is tearful and indecisive may increase their anxiety. Pressing for clarification when a client is struggling to articulate their feelings can be counterproductive, potentially leading the client to shut down further rather than opening up about the underlying cause of their distress.
Correct Answer is B
Explanation
Choice A reason: Auscultation is the process of listening to sounds produced within the body, typically using a stethoscope. In an abdominal exam, it is used to assess bowel sounds and vascular bruits. It follows inspection but must precede percussion and palpation to ensure that bowel motility is not artificially stimulated.
Choice B reason: Inspection is the systematic visual observation of the patient, which is always the first step in a physical assessment. In the abdomen, the nurse inspects for contour, symmetry, skin integrity, pulsations, and the presence of striae or scars. This non-invasive step provides immediate clues regarding underlying pathology.
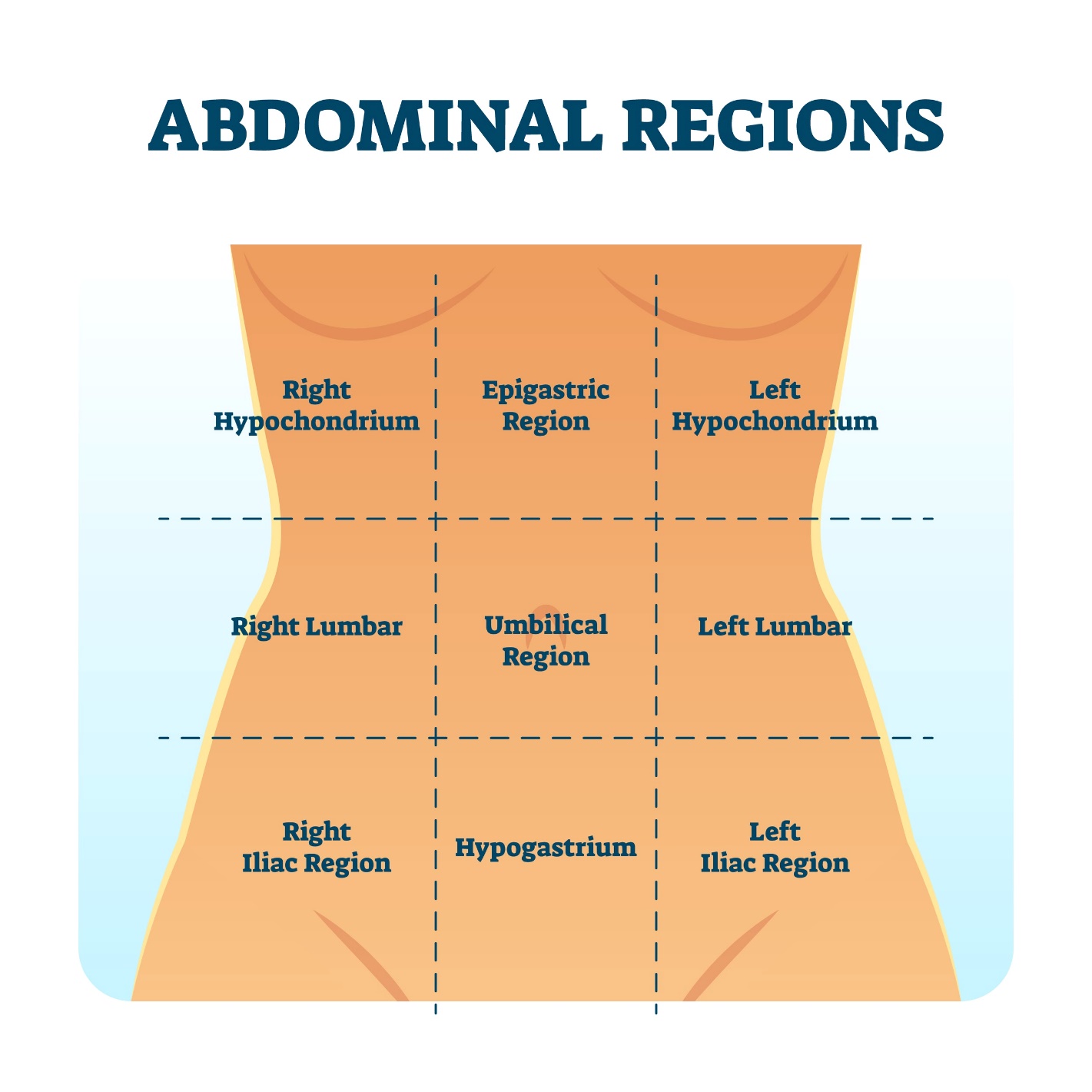
Shutterstock
Explore
Choice C reason: Percussion involves tapping the body surface to produce vibrations and sounds. This technique helps determine the density of underlying organs and the presence of fluid or gas. It is performed after inspection and auscultation to map out organ boundaries like the liver or spleen.
Choice D reason: Palpation is the use of touch to assess organ size, location, and the presence of tenderness or masses. It is the final step in the abdominal assessment sequence because deep pressure can alter bowel sounds and cause patient guarding, which would interfere with the accuracy of the preceding steps.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
