The fetal monitor strip below is from a client receiving oxytocin augmentation for labor.
What would the nurse do first for this client?
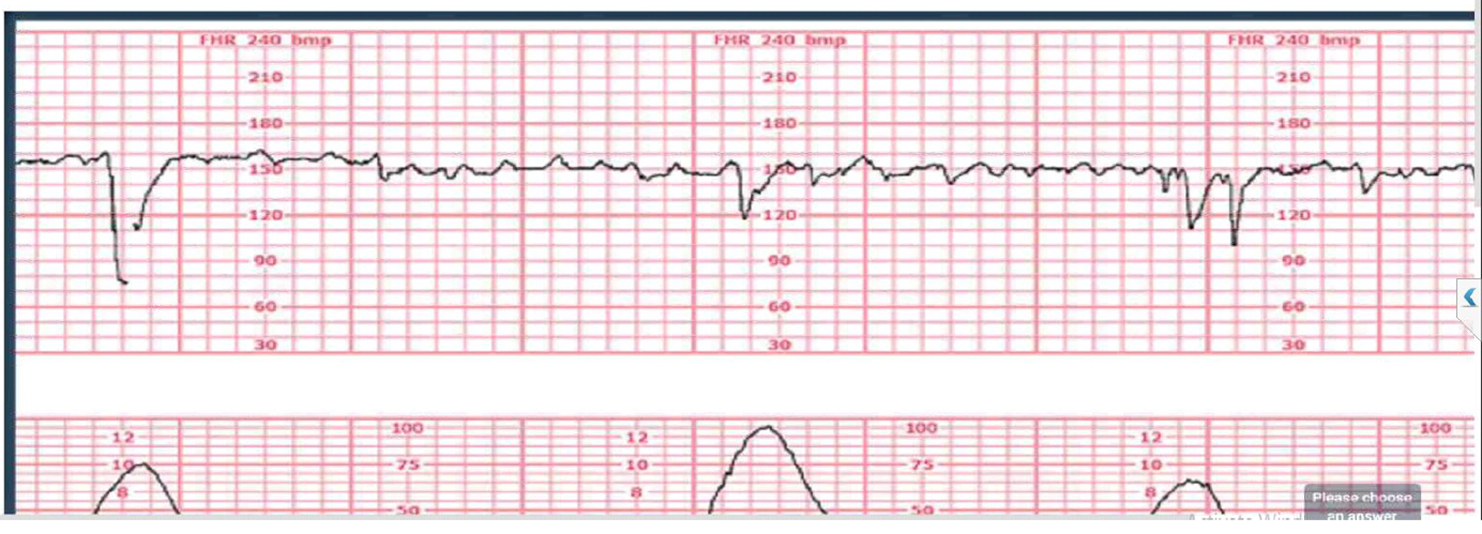
Continue to monitor contraction duration every one hour.
Discontinue the oxytocin infusion.
Slow the infusion until a decrease in contractions are seen.
Increase the flow rate of the fluid line infusion.
The Correct Answer is B
Choice A rationale: Monitoring contraction duration only once every hour is inadequate and inappropriate in the presence of variable decelerations on the fetal heart rate (FHR) tracing. Variable decelerations are abrupt drops in FHR, often caused by umbilical cord compression. The nursing priority is to act immediately to relieve the compression and improve fetal oxygenation, not to observe the uterus infrequently.
Choice B rationale: Discontinuing the oxytocin infusion is the most critical and immediate intervention for this tracing. Oxytocin increases both the frequency and intensity of contractions, which can worsen cord compression and reduce the fetus’s recovery time between contractions. Stopping the uterine stimulation is the fastest way to relieve stress on the fetus.
Choice C rationale: Slowing the oxytocin infusion is a reasonable intervention, but it is not the first step. Because the variable decelerations are recurrent and pronounced, with FHR dropping below 90 bpm, the immediate and most effective action is to discontinue the infusion entirely. This should then be followed by other intrauterine resuscitation measures, such as repositioning the client laterally.
Choice D rationale: Increasing the flow rate of the main IV fluid line (a bolus) is a common intervention during fetal distress, as it can improve maternal blood volume, placental perfusion, and fetal oxygenation. However, in this case, the primary issue is recurrent variable decelerations likely caused by cord compression worsened by contractions. Therefore, the oxytocin must be stopped first to prevent further stress on the fetus.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A rationale
The position Left Occiput Anterior (LOA) means the fetal occiput (the presenting part) is on the maternal left side and toward the anterior pelvis. The station of +4 indicates the presenting part is significantly below the ischial spines (the point of 0 station), almost at the perineum, which does not align with the description of "at the level of the ischial spines.”.
Choice B rationale
The designation Left Shoulder Anterior (LSA) would mean the shoulder is the presenting part, which typically signifies a transverse lie and not the fetal head being well-flexed as described. A station of -2 means the head is above the ischial spines, which contradicts the description of the head being "at the level of the ischial spines" (0 station).
Choice C rationale
Right Occiput Anterior (ROA) correctly describes the fetal position. The fetal head is the presenting part, well flexed, the occiput is on the maternal right side ("fetal back is on the maternal right side between the midline and lateral surface"), and toward the anterior pelvis. The station of 0 accurately indicates the head is "at the level of the ischial spines.”.
Choice D rationale
Right Shoulder Transverse (RST) indicates the shoulder is the presenting part and is in the transverse position on the maternal right side, which is inconsistent with the description of the fetal head being the presenting part and well-flexed. A station of -3 means the presenting part is still high in the pelvis, 3 cm above the ischial spines.
Correct Answer is A
Explanation
Choice A rationale
The statement is incorrect because many herbal remedies and supplements are not regulated by the FDA and lack rigorous safety and efficacy data for use in pregnancy. Some herbs contain compounds that can be abortifacient, teratogenic, or affect uterine tone and clotting, posing significant risks to the developing fetus or the pregnancy itself, requiring cautious avoidance.
Choice B rationale
This statement is correct. Many allergy medications and other prescription/over-the-counter drugs have established safety profiles in pregnancy, and a healthcare provider is best positioned to weigh the therapeutic benefits against potential fetal risks. Consulting a doctor ensures a risk-benefit analysis based on current medical evidence and the specific stage of gestation.
Choice C rationale
This statement is correct. Folic acid supplementation (400 to 800 mcg daily) is crucial, ideally starting before conception and continuing throughout the first trimester (12 weeks). Adequate intake is essential for early fetal neural tube development to prevent defects like spina bifida and anencephaly, as the neural tube closes within the first 28 days post-conception.
Choice D rationale
This statement is correct. X-rays expose the developing fetus to ionizing radiation, which carries a risk of teratogenic effects, especially in the first trimester. While necessary diagnostic procedures are often modified or shielded, the principle of ALARA (As Low As Reasonably Achievable) is followed, and the provider must be informed of the pregnancy.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
