When caring for a laboring client with epidural anesthesia, the nurse should be alert for which complication?
Hypotension
Hypervolemia
Hyperemia
Hyponatremia
The Correct Answer is A
A. Hypotension: Regional anesthesia causes sympathetic blockade, leading to peripheral vasodilation and a rapid decrease in systemic vascular resistance. This often results in a significant drop in maternal blood pressure, which can reduce uteroplacental perfusion and cause fetal bradycardia. It is the most frequent and serious side effect of epidural placement.
B. Hypervolemia: This condition is characterized by an excess of fluid in the intravascular compartment, which is not a side effect of epidural administration. In fact, patients often require a fluid bolus to counteract the relative hypovolemia caused by vasodilation. Epidural anesthesia does not trigger fluid retention or volume overload.
C. Hyperemia: This term refers to an increased blood flow to a specific organ or tissue, which is not a systemic complication associated with spinal or epidural blocks. While local vasodilation occurs, the primary clinical concern is the systemic drop in blood pressure rather than localized tissue congestion. It lacks relevance as a major anesthetic complication.
D. Hyponatremia: Low serum sodium levels are typically associated with excessive free water administration or oxytocin-induced water intoxication. Epidural anesthesia does not directly alter electrolyte balance or renal water excretion. Monitoring focuses on hemodynamic stability and respiratory status rather than acute changes in serum sodium concentration.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
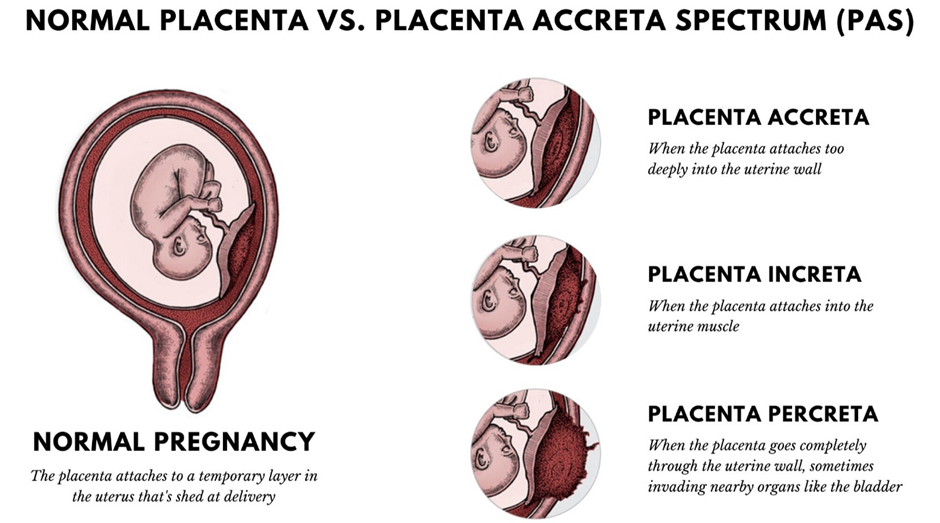
A. Accreta: This refers to the simplest form of morbidly adherent placenta where the chorionic villi attach directly to the myometrium. The placenta does not penetrate the muscle layer but lacks an intervening decidua basalis. It is the most common but least invasive of the three types.
B. Plancreta: This term is not a recognized medical diagnosis in obstetrics or pathology for placental attachment disorders. The standard nomenclature for invasive placentation includes accreta, increta, and percreta based on depth. Using incorrect jargon can lead to clinical errors in surgical planning.
C. percreta: This represents the most severe form of abnormal placentation where villi penetrate through the entire thickness of the myometrium and serosa. The placental tissue can invade adjacent pelvic structures, most commonly the urinary bladder. It carries the highest risk for massive obstetric hemorrhage.
D. increta: In this condition, the placental villi invade deeply into the myometrium but do not breach the outer uterine serosa. While more invasive than accreta, it does not involve the penetration of extrauterine organs like the bladder. It still requires significant surgical management, often a hysterectomy.
Correct Answer is A
Explanation
A. assess the fetal heart rate (FHR) pattern: The sudden release of amniotic fluid can cause the umbilical cord to wash down ahead of the fetal part, leading to prolapse. Monitoring the heart rate immediately detects any sudden bradycardia or variable decelerations caused by cord occlusion. This is the highest priority for fetal safety.
B. perform a vaginal examination: A digital exam can confirm a cord prolapse or check cervical progress, but it is not the first action required. The fetal heart rate provides immediate data on fetal status and the urgency of the situation. Physical assessment follows the electronic confirmation of fetal stability or distress.
C. inspect the characteristics of the fluid: Checking for meconium staining or foul odor provides information about fetal maturity, stress, or infection risk. While important for long-term planning, these findings do not present the immediate life-threat that a cord prolapse does. Fluid inspection is secondary to heart rate assessment.
D. assess maternal temperature: Monitoring for pyrexia is essential to screen for chorioamnionitis following the rupture of protective membranes. However, infection typically takes hours to develop and manifest clinically. The immediate risk of mechanical cord compression requires a more urgent response via heart rate monitoring.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
