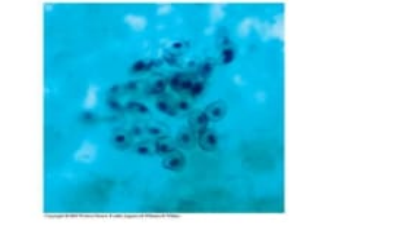
A 36-year-old man with AIDS presents with fever, dry cough, and dyspnea. A chest x-ray shows bilateral and diffuse infiltrates. Laboratory studies reveal a low CD4+ cell count. A lung biopsy discloses a chronic interstitial pneumonitis and an intra-alveolar foamy exudate. A silver stain of a bronchoalveolar lavage is shown. Which of the following organisms is the most likely responsible for these pulmonary findings?
Cryptococcus neoformans
Mycoplasma pneumoniae
Pneumocystis jirovec
Streptococcus pyogenes
The Correct Answer is C
A. Cryptococcus neoformans: Cryptococcus infection usually affects immunocompromised patients, particularly causing meningoencephalitis. Pulmonary involvement can occur, but it typically presents with localized nodules or consolidations, not diffuse interstitial infiltrates with foamy intra-alveolar exudate.
B. Mycoplasma pneumoniae: Mycoplasma pneumoniae causes atypical pneumonia, often in young, otherwise healthy adults. It produces mild interstitial infiltrates and dry cough but is not associated with severe immunosuppression or the foamy alveolar exudate seen in AIDS patients with low CD4+ counts.
C. Pneumocystis jirovecii: Pneumocystis jirovecii is an opportunistic fungus causing Pneumocystis pneumonia (PCP) in immunocompromised patients, especially those with AIDS and CD4+ counts <200 cells/µL. Histologically, it produces diffuse interstitial pneumonitis with intra-alveolar foamy exudates, which can be highlighted by silver staining (Gomori methenamine silver), consistent with the biopsy findings in this patient.
D. Streptococcus pyogenes: Streptococcus pyogenes typically causes pharyngitis, skin infections, and occasionally severe bacterial pneumonia. It presents with lobar consolidation and purulent exudate rather than diffuse interstitial infiltrates and foamy alveolar material, making it unlikely in this scenario.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
A. Bronchial asthma:Asthma is characterized by episodic wheezing, reversible airway obstruction, and airway hyperresponsiveness. It usually presents with intermittent symptoms rather than a chronic productive cough and persistent hypoxia with CO₂ retention, making it less consistent with this patient’s history.
B. Chronic bronchitis:Chronic bronchitis, a form of chronic obstructive pulmonary disease (COPD), is defined by a productive cough lasting at least three months per year for two consecutive years. Heavy smoking is the primary risk factor. The patient’s chronic cough, sputum production, frequent infections, hypoxia, and CO₂ retention are classic features of chronic bronchitis, reflecting chronic airway inflammation and airflow obstruction.
C. Diffuse alveolar damage (ARDS):ARDS presents acutely with severe hypoxemia and bilateral pulmonary infiltrates following trauma, sepsis, or inhalation injury. It does not produce a 3-year history of chronic cough or sputum production and is not a chronic condition.
D. Goodpasture syndrome:Goodpasture syndrome is an autoimmune disorder targeting the lungs and kidneys, causing hemoptysis and rapidly progressive glomerulonephritis. It does not typically present with chronic productive cough or CO₂ retention from chronic airway disease.
E. Usual interstitial pneumonia:Usual interstitial pneumonia, seen in idiopathic pulmonary fibrosis, causes progressive dyspnea and dry cough, not productive cough. It also leads to restrictive lung disease rather than the obstructive pattern and CO₂ retention seen in chronic bronchitis.
Correct Answer is D
Explanation
A. Ascites:Ascites refers to the accumulation of fluid in the peritoneal cavity, typically due to liver disease, heart failure, or malignancy. It does not describe localized swelling of the leg as seen in elephantiasis.
B. Effusion:Effusion is the collection of fluid within a body cavity, such as the pleural, pericardial, or joint spaces. While it involves fluid accumulation, it does not specifically apply to interstitial swelling of the extremities caused by lymphatic obstruction.
C. Fibrinous exudate:Fibrinous exudate contains fibrinogen and forms in severe inflammation, often coating serous surfaces. It is typically associated with pleuritis or pericarditis rather than chronic soft tissue swelling of the leg.
D. Lymphedema:Lymphedema is the accumulation of protein-rich fluid in the interstitial spaces due to impaired lymphatic drainage. In this patient, chronic lymphatic obstruction, often from filarial infection, leads to elephantiasis, causing massive swelling of the leg and thickened skin.
E. Purulent exudate:Purulent exudate is composed of neutrophils, dead cells, and infectious debris, seen in bacterial infections and abscess formation. Elephantiasis involves sterile lymphatic fluid accumulation rather than pus.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
