A 37-week client is stating she is having severe back pain and is placed on an external monitor. The monitor shows the following fetal and contraction tracing.
How would the nurse document the client's contractions?
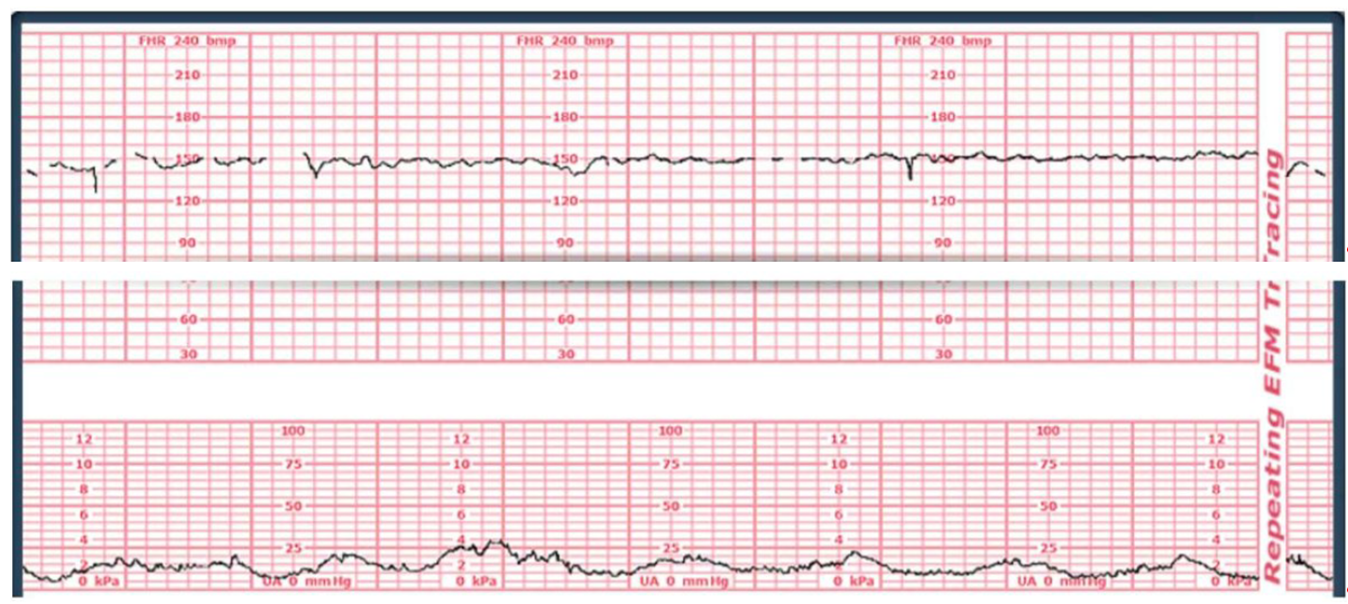
Indeterminate.
Tachysystole.
Normal.
Bradycardia.
The Correct Answer is B
Choice A rationale
Indeterminate is a term primarily used to classify Fetal Heart Rate (FHR) tracings that fall into Category II, meaning they do not meet the criteria for Category I (normal) or Category III (abnormal). This term is not used to document uterine contraction frequency or intensity. Uterine activity is typically quantified by the number of contractions in a 10-minute window, averaged over 30 minutes, or by intensity..
Choice B rationale
Tachysystole is defined as having more than five contractions in 10 minutes, averaged over a 30-minute window. This can lead to decreased fetal oxygen supply due to inadequate uterine resting time, causing fetal hypoxemia. By counting the contractions in a typical 10-minute segment on the provided tracing, there are only about 3 or 4 contractions, which is not tachysystole..
Choice C rationale
Normal uterine activity is defined as five or fewer contractions in 10 minutes, averaged over a 30-minute window. By observing the lower tracing (uterine activity/UA), there are 3 to 4 contractions within a typical 10-minute segment. This falls within the expected range for a laboring client. The contractions are spaced appropriately, allowing for adequate uterine resting tone and placental perfusion..
Choice D rationale
Bradycardia is a term used to describe a slow Fetal Heart Rate (FHR), specifically a baseline FHR less than 110 beats per minute (bpm). This is a measure of the fetus's heart rate, not a descriptor for uterine contraction frequency or pattern. The uterine activity is described by frequency, duration, and intensity, not heart rhythm terms like bradycardia.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A rationale
At 20 weeks gestation, the uterine fundus typically reaches the level of the umbilicus (navel). This standardized landmark is due to the uterus's growth pattern, where it rises out of the pelvis and becomes an abdominal organ. Measuring fundal height from the symphysis pubis to the top of the fundus, it usually correlates with the weeks of gestation ± 2 cm between 18 and 32 weeks, making 20 cm at the umbilicus the expected finding.
Choice B rationale
Two finger-breadths below the umbilicus corresponds to approximately 18 weeks gestation. Before 20 weeks, the fundus is lower in the abdomen as the uterus continues its upward expansion from the pelvic cavity. At this stage, the measurement would be slightly less than 20 cm, indicating a smaller uterine size than expected for a 20-week pregnancy.
Choice C rationale
Halfway between the symphysis pubis and the umbilicus indicates a fundal height consistent with approximately 16 weeks gestation. At this point, the uterus is palpably in the abdomen, but its superior edge is still significantly lower than the umbilicus. This position reflects earlier growth before the rapid ascent to the umbilicus at 20 weeks.
Choice D rationale
Fundal height at the level of the xyphoid process is expected around 36 weeks gestation as the uterus reaches its highest point in the abdomen. This significantly higher position reflects a near-term pregnancy, where the large fetus and uterus displace the abdominal contents superiorly toward the diaphragm, much later than 20 weeks.
Correct Answer is D
Explanation
Choice A rationale
Green-stained amniotic fluid in a fetus, especially one who is post-term (41 weeks), is highly suggestive of meconium staining. This occurs when the fetus passes its first stool (meconium) in utero. While the meconium is expelled, its presence in the amniotic fluid is often a sign of fetal stress or compromise, which can lead to complications such as meconium aspiration syndrome.
Choice B rationale
Although green or foul-smelling amniotic fluid can indicate intrauterine infection (chorioamnionitis), particularly if accompanied by maternal fever or uterine tenderness, meconium staining is a more common cause in a post-term pregnancy with a breech presentation. Chorioamnionitis involves ascending infection of the membranes and fluid, not solely the color change due to meconium.
Choice C rationale
Neural tube defects, like spina bifida or anencephaly, are congenital structural abnormalities resulting from incomplete closure of the embryonic neural tube. While they can sometimes be associated with oligohydramnios or specific markers, they do not typically cause the amniotic fluid to turn green. Green fluid is a sign of a physiological event, not an anatomical malformation.
Choice D rationale
Meconium passage in utero, resulting in green amniotic fluid, is frequently an indicator of fetal distress or compromise, often due to hypoxia (oxygen deprivation) or umbilical cord compression. The fetus may pass meconium secondary to vagal nerve stimulation from stress. Therefore, the nurse's finding immediately alerts the team that fetal well-being may be acutely threatened, necessitating close monitoring and potential intervention.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
