A nurse is caring for a client who has multiple sclerosis and is being evaluated for progressive multifocal leukoencephalopathy (PML). Which of the following findings should the nurse recognize as manifestations of this condition?
(Select All that Apply.)
Memory loss
Clumsiness
Tardive dyskinesia
Seizures
Vision difficulty
Correct Answer : A,B,D,E
Choice A Reason:
Memory loss is correct. Memory loss can occur in individuals with PML due to damage to the white matter of the brain caused by the JC virus infection. This damage can affect cognitive function, including memory.
Choice B Reason:
Clumsiness is correct. Clumsiness or lack of coordination is a common neurological symptom of PML. It can result from damage to areas of the brain responsible for motor function and coordination.
Choice C Reason:
Tardive dyskinesia is incorrect. Tardive dyskinesia is a movement disorder characterized by involuntary, repetitive movements, often involving the face, lips, tongue, and limbs. While tardive dyskinesia can occur as a side effect of certain medications, it is not typically associated with PML.
Choice D Reason:
Seizures is correct. Seizures can occur in individuals with PML due to the involvement of the brain's white matter by the JC virus infection. Seizures may present as sudden, uncontrolled movements, altered consciousness, or other neurological symptoms.
Choice E Reason:
Vision difficulty is correct. Vision difficulties, including blurred vision, visual field deficits, and other visual disturbances, are common manifestations of PML. Damage to the optic nerves or areas of the brain involved in visual processing can result in vision difficulties.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A Reason:
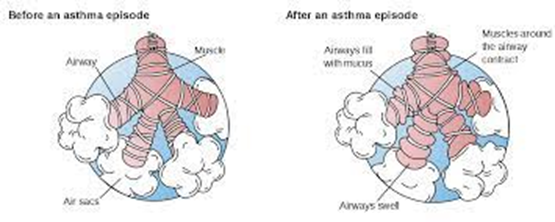
Decreased mucus production contributes to airway constriction: This statement is incorrect. Bronchospasm does not decrease mucus production; instead, it primarily affects the smooth muscles surrounding the bronchioles, leading to their constriction and narrowing of the airways. Increased mucus production, often accompanied by inflammation, can contribute to airway obstruction in conditions like asthma.
Choice B Reason:
Inflammation is reduced due to airway diameter: This statement is incorrect. Bronchospasm typically occurs in the setting of inflammation in conditions such as asthma. Constriction of the airways during bronchospasm exacerbates the inflammation and can further narrow the airways, leading to symptoms such as wheezing and dyspnea.
Choice C Reason:
Bronchospasm occurs when there is inflammation, edema, and excess mucus: This statement is partially correct. Bronchospasm often occurs in the presence of inflammation, edema, and excess mucus production, as seen in conditions like asthma. These factors contribute to airway hyperresponsiveness, leading to bronchospasm and airway narrowing.
Choice D Reason:
Airway obstruction occurs due to thinning mucus: This statement is incorrect. Airway obstruction in conditions like asthma is primarily due to bronchospasm, inflammation, and excessive mucus production, rather than thinning mucus. Thinning of mucus would not typically contribute to airway obstruction.
Correct Answer is B
Explanation
Choice A Reason:
"I have signed up for an aerobics class three times a week." This statement is incorrect. Participating in aerobics classes three times a week may not be suitable for someone with spinal stenosis, as certain movements and high-impact activities common in aerobics classes can exacerbate symptoms and increase the risk of injury to the spine.
Choice B Reason:
"I ride my bicycle every day." This statement is correct. Cycling is generally considered a low-impact exercise that can be beneficial for individuals with spinal stenosis, as it helps improve cardiovascular fitness without placing excessive stress on the spine. Riding a bicycle regularly may be a suitable exercise option for this client.
Choice C Reason:
"I like to jog a half a mile every day." This statement is incorrect. Jogging involves repetitive impact and can place significant stress on the spine, which may exacerbate symptoms of spinal stenosis. It is generally not recommended for individuals with spinal stenosis due to the high-impact nature of the activity.
Choice D Reason:
"I enjoy doing circuit training once a week.": Circuit training typically involves a combination of aerobic and strength-training exercises performed in rapid succession. While some components of circuit training, such as strength training, can be beneficial for individuals with spinal stenosis, the intensity and variety of exercises in circuit training may not be suitable for everyone with this condition.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
