A nurse is reviewing the laboratory results of a client who has bulimia nervosa. The nurse should notify the provider of which of the following results?
Potassium 3.2 mEq/L
WBC 5,200/mm3
Hgb 14 g/dL
Magnesium 1.6 mEq/L
The Correct Answer is A
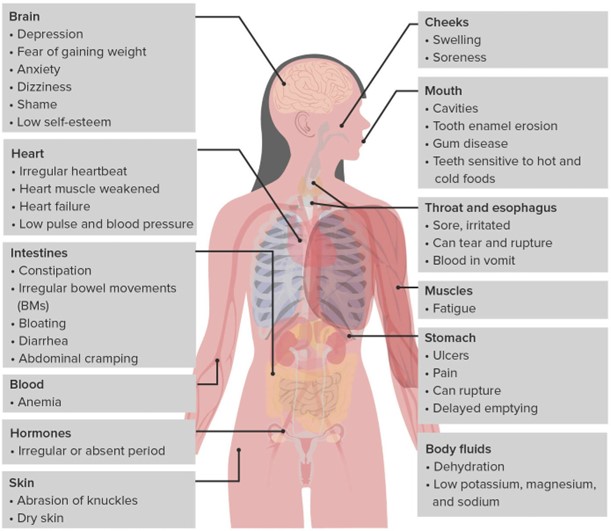
Low potassium levels, known as hypokalemia, can be a significant concern in individuals with bulimia nervosa due to the frequent purging behaviors associated with the condition. Purging, such as self-induced vomiting or misuse of laxatives or diuretics, can lead to excessive loss of potassium from the body. Hypokalemia can have serious consequences, including cardiac arrhythmias, muscle weakness, fatigue, and even life-threatening complications.
The normal range for potassium is typically around 3.5-5.0 mEq/L. With a potassium level of 3.2 mEq/L falling below the normal range, it indicates a low potassium level and requires prompt attention.
The other laboratory results mentioned in the question are within normal ranges:
● A WBC (white blood cell) count of 5,200/mm3 falls within the normal range (typically between 4,500 and 11,000/mm3) and indicates a normal white blood cell count.
● An Hgb (hemoglobin) level of 14 g/dL falls within the normal range (typically between 12 and 16 g/dL) and indicates a normal hemoglobin level.
● A magnesium level of 1.6 mEq/L, although slightly low, is still within the normal range (typically between 1.5 and 2.5 mEq/L). The nurse should monitor it closely and assess for symptoms associated with hypomagnesemia. If the client's symptoms or other clinical indications suggest a significant magnesium imbalance, the healthcare provider should be notified.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
The nurse should expect the client to have a weight loss rate of 0.45 kg (1 lb) per week when reducing their calorie intake by 500 calories per day. A general guideline for weight loss is that a calorie deficit of 500 calories per day can lead to a weight loss of approximately 0.45 kg (1 lb) per week. This estimate is based on the notion that 1 pound of body weight is roughly equivalent to 3,500 calories. By creating a calorie deficit of 500 calories per day (500 calories x 7 days = 3,500 calories), the client can expect to lose around 0.45 kg (1 lb) of weight per week.
It is important to note that individual factors, such as metabolism and activity level, can influence weight loss rates. Therefore, the actual rate of weight loss may vary among individuals. It is generally recommended to aim for gradual and sustainable weight loss rather than rapid or extreme weight loss.
Correct Answer is A
Explanation
Folate, also known as vitamin B9, is an essential nutrient during pregnancy as it plays a crucial role in the development of the baby's neural tube. When teaching a client about increasing folate in their diet during pregnancy, it's important to recommend foods that are rich in this nutrient.
1/2 cup cooked asparagus: Asparagus is a good source of folate, and 1/2 cup of cooked asparagus contains approximately 134 micrograms of folate.
1/2 cup plain low-fat yogurt: While yogurt is a healthy food choice, it is not a significant source of folate.
1 medium apple: Apples are generally low in folate content and not considered a rich source of this nutrient.
1 small banana: Bananas are also not known for their folate content and do not provide a significant amount of this nutrient.
Given the options provided, 1/2 cup cooked asparagus is the best source of folate. It is important to note that other food sources rich in folate include dark leafy greens, legumes, fortified cereals, and citrus fruits. Encouraging a varied and balanced diet that incorporates these folate-rich foods can help ensure adequate folate intake during pregnancy.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
