A nurse is caring for a patient on the third day following abdominal surgery.
The nurse notes the absence of bowel sounds, abdominal distention, and the patient has not passed any flatus. Which postoperative complication is the patient likely experiencing?
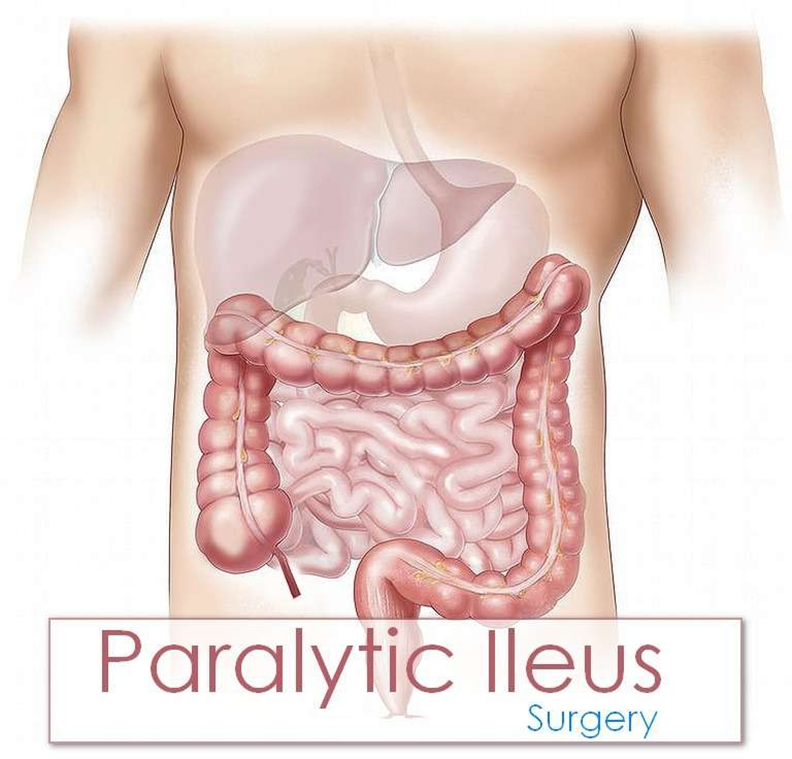
Paralytic ileus
Incisional infection
Fecal impaction
Health care-associated Clostridium difficile
The Correct Answer is A
Choice A rationale:
Paralytic ileus is a common postoperative complication that occurs when the normal movement of the intestines (peristalsis) is slowed or stopped. This can lead to a buildup of gas and fluids in the intestines, causing abdominal distention, nausea, vomiting, and constipation. The absence of bowel sounds, abdominal distention, and the inability to pass flatus are all classic signs of paralytic ileus.
Here are some of the factors that can contribute to paralytic ileus: Manipulation of the intestines during surgery
Anesthesia
Pain medications, especially opioids Electrolyte imbalances
Dehydration
Underlying medical conditions, such as diabetes or kidney disease Treatment for paralytic ileus typically involves:
Resting the bowel by not eating or drinking anything by mouth
Using a nasogastric (NG) tube to suction out gas and fluids from the stomach Providing intravenous (IV) fluids and electrolytes
Encouraging early ambulation
Using medications to stimulate bowel movement, such as metoclopramide or erythromycin
Choice B rationale:
Incisional infection is an infection of the surgical wound. It would typically present with redness, warmth, swelling, and pain at the incision site. The patient may also have a fever. While incisional infections can occur after abdominal surgery, they are not typically associated with the absence of bowel sounds, abdominal distention, and the inability to pass flatus.
Choice C rationale:
Fecal impaction is a severe form of constipation in which a large, hard mass of stool becomes trapped in the rectum. It can cause abdominal pain, bloating, and difficulty passing stool. However, it is not typically associated with the absence of bowel sounds or abdominal distention.
Choice D rationale:
Health care-associated Clostridium difficile (C. difficile) is a bacterial infection that can cause severe diarrhea, abdominal pain, and cramping. It is often associated with antibiotic use. While C. difficile can occur after abdominal surgery, it is not typically associated with the absence of bowel sounds, abdominal distention, and the inability to pass flatus.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Rationale for Choice A: Obtain vital signs
While obtaining vital signs is important in assessing a patient's overall condition, it is not the first priority in a suspected transfusion reaction.
Vital signs can provide valuable information about the severity of the reaction, but they should not delay the immediate action of stopping the transfusion.
Delaying the cessation of the transfusion could allow for further infusion of incompatible blood or allergens, potentially worsening the reaction and leading to more serious complications.
Rationale for Choice B: Notify the registered nurse
Involving other healthcare professionals is crucial in managing transfusion reactions, but it should not precede stopping the transfusion.
The nurse should prioritize stopping the transfusion to prevent further exposure to potential triggers and then promptly notify the registered nurse for further assessment and interventions.
Timely communication with the registered nurse is essential for coordinating care and ensuring appropriate treatment measures are implemented.
Rationale for Choice C: Administer diphenhydramine
Diphenhydramine, an antihistamine, can be used to treat allergic reactions, but it should not be administered as the first response in this scenario.
The priority is to halt the infusion of the blood product that is potentially causing the reaction.
Administering diphenhydramine before stopping the transfusion could mask the symptoms of the reaction, making it more difficult to assess its severity and progression.
Rationale for Choice D: Stop the transfusion
This is the correct and most immediate action to take when a patient develops itching and hives during a blood transfusion.
These symptoms are indicative of a possible allergic or transfusion reaction, and stopping the transfusion is essential to prevent further complications.
It's critical to act quickly to minimize the amount of incompatible blood or allergens that enter the patient's circulation.
By stopping the transfusion, the nurse can potentially prevent the reaction from worsening and safeguard the patient's well- being.
Correct Answer is D
Explanation
Choice A rationale:
Notifying the facility's security department may be necessary in some cases, but it should not be the nurse's first action. This could escalate the situation and make the patient feel threatened or coerced. It's important to first attempt to de-escalate the situation and understand the patient's reasons for wanting to leave. Involving security prematurely could damage the nurse- patient relationship and make it more difficult to provide care in the future.
Security should be involved if the patient is a danger to themselves or others, or if they are attempting to leave in a way that could cause harm. However, in most cases, it is best to try to resolve the situation through communication and understanding.
Choice B rationale:
Calling the patient's family may be helpful in some cases, but it is not always necessary or appropriate. The nurse should first assess the patient's decision-making capacity and their understanding of the risks of leaving against medical advice. If the patient is capable of making their own decisions, the nurse should respect their autonomy and not involve family members without their consent.
Involving family members without the patient's consent could breach confidentiality and erode trust. It's important to balance the patient's right to privacy with the potential benefits of involving family members.
Choice C rationale:
Insisting that the patient exit the hospital via a wheelchair is not necessary in most cases. If the patient is able to walk and does not pose a safety risk, they should be allowed to leave on their own terms. Requiring a wheelchair could be seen as patronizing or controlling, and it could further upset the patient.
The use of a wheelchair should be based on the patient's individual needs and preferences, not on a blanket policy.
Choice D rationale:
Making sure the patient understands that they are leaving against medical advice is the most important action the nurse can take. This ensures that the patient is aware of the potential risks of leaving the hospital, and it protects the nurse from liability. The nurse should document the patient's decision in the medical record and have the patient sign an Against Medical Advice (AMA) form.
By ensuring informed consent, the nurse respects the patient's autonomy while also fulfilling their professional obligations.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
