A nurse is reinforcing teaching with a client who is at 34 weeks of gestation and at risk for placental abruption. Does the nurse recognize that which of the following is the most common risk factor for a placental abruption?
Maternal hypertension.
Maternal cocaine use.
Maternal cigarette smoking.
Maternal battering.
The Correct Answer is A
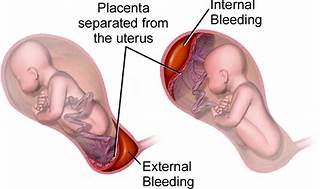
The correct answer is choice A, Maternal hypertension.
Choice A rationale:
Maternal hypertension is widely recognized as the most common risk factor for placental abruption. High blood pressure can cause the placenta to detach from the uterine wall, leading to abruption. In summary, while all the listed factors can contribute to the risk of placental abruption, maternal hypertension stands out as the most common cause, supported by multiple health sources. It’s important for nurses to recognize and manage hypertension in pregnant clients to minimize the risk of this serious complication.
Choice B rationale:
While maternal cocaine use is a significant risk factor for placental abruption due to its vasoconstrictive effects, which can compromise the placental blood flow, it is not as common as maternal hypertension.
Choice C rationale:
Maternal cigarette smoking is also a risk factor for placental abruption. Smoking can lead to a variety of complications in pregnancy, including placental problems, but again, it is less common than hypertension as a cause for abruption.
Choice D rationale:
Maternal battering can lead to trauma which may result in placental abruption. However, it is not considered the most common risk factor when compared to maternal hypertension.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A rationale:
Excessive uterine enlargement. Rationale: The nurse should monitor the client for excessive uterine enlargement, as a hydatidiform mole is a rare condition in pregnancy where abnormal placental tissue forms instead of a fetus. This abnormal growth can lead to uterine enlargement beyond the expected size for gestational age.
Choice B rationale:
Rapidly dropping human chorionic gonadotropin (hCG) levels. Rationale: The nurse should also monitor the client's hCG levels. In a normal pregnancy, hCG levels typically rise steadily during the early stages. However, in the case of a hydatidiform mole, hCG levels may either plateau or drop rapidly due to the abnormal placental growth.
Choice C rationale:
Fetal heart rate irregularities. Rationale: Although a hydatidiform mole does not involve a viable fetus, the nurse should still assess for fetal heart rate irregularities. In some rare cases, the presence of abnormal placental tissue can cause confusion in the diagnosis, and there may be coexisting fetal development. Fetal heart rate irregularities may indicate potential complications.
Choice D rationale:
Whitish vaginal discharge. Rationale: Whitish vaginal discharge is not typically associated with a hydatidiform mole. Instead, this finding is more commonly seen in other vaginal infections or conditions unrelated to a molar pregnancy. The nurse should be cautious not to misinterpret this symptom as a definitive sign of a hydatidiform mole.
Correct Answer is A
Explanation
Choice A: The correct answer is (a) Bleeding. The purpose of administering vitamin K to a newborn following delivery is to prevent bleeding complications. Vitamin K plays a crucial role in the synthesis of blood clotting factors, specifically factors II, VII, IX, and X. Newborns have low levels of vitamin K at birth, and it takes a few days for their bodies to start producing it. This places them at risk of developing vitamin K deficiency bleeding (VKDB), which can lead to serious bleeding problems, including bleeding into the brain (intracranial haemorrhage). By giving the newborn a vitamin K injection, this deficiency is corrected, reducing the risk of bleeding complications.
Choice B rationale
(b) Infection. Administering vitamin K to a newborn is not intended to prevent infections. Vitamin K is essential for blood clotting and does not have a direct role in preventing or treating infections. Infection prevention measures involve proper hygiene practices and vaccination, but vitamin K is unrelated to this aspect of care.
Choice C rationale
(c) Potassium deficiency. Administering vitamin K to a newborn has no impact on potassium levels. Potassium is a different essential nutrient that plays a vital role in various physiological processes, but it is not related to blood clotting. The administration of vitamin K is specific to preventing bleeding complications, not addressing potassium deficiency.
Choice D rationale
(d) Hyperbilirubinemia. The correct answer is not (d) Hyperbilirubinemia. Vitamin K administration is not aimed at preventing or treating hyperbilirubinemia, a condition characterized by elevated levels of bilirubin in the blood. Hyperbilirubinemia is related to the breakdown of red blood cells and the liver'sability to process bilirubin, whereas vitamin K's primary role is in the clotting cascade.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
