A client is on a ventilator. Alarms are sounding, indicating an increase in peak airway pressure. The nurse assesses first for what?
Malfunction of the alarm button.
A cut or slice in the tubing from the ventilator.
Higher than normal endotracheal cuff pressure.
A kink in the ventilator tubing.
The Correct Answer is D
Choice A Reason:
Malfunction of the alarm button is unlikely to be the cause of increased peak airway pressure. The alarm is designed to alert the nurse to a problem with the ventilator or the patient’s airway, not to malfunction itself. Therefore, this is not the first thing the nurse should assess.
Choice B Reason:
A cut or slice in the tubing from the ventilator could cause a loss of pressure or air leak, but it would not typically result in increased peak airway pressure. Instead, it would likely cause a decrease in pressure and potentially trigger a different alarm.
Choice C Reason:
Higher than normal endotracheal cuff pressure can contribute to increased peak airway pressure. However, it is not the most immediate concern compared to a kink in the tubing, which can completely obstruct airflow and rapidly compromise the patient’s ventilation.
Choice D Reason:
A kink in the ventilator tubing is a common and immediate cause of increased peak airway pressure. It obstructs the flow of air, leading to a buildup of pressure in the system. This is the first thing the nurse should assess and correct to ensure the patient is receiving adequate ventilation.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["A","B","C"]
Explanation
Choice A reason: A 22-year-old client with asthma is considered a priority for pneumonia vaccination. Asthma is a chronic respiratory condition that can increase the risk of complications from pneumonia. Vaccination helps protect against pneumococcal infections, which can be particularly severe in individuals with underlying respiratory conditions.
Choice B reason: A healthy 72-year-old client is also a priority for pneumonia vaccination. The Centers for Disease Control and Prevention (CDC) recommends pneumococcal vaccination for all adults aged 65 years and older. Older adults are at higher risk for pneumococcal disease due to age-related decline in immune function.
Choice C reason: A client with well-controlled diabetes should be prioritized for pneumonia vaccination. Diabetes can weaken the immune system, making individuals more susceptible to infections, including pneumonia. Vaccination is an important preventive measure for individuals with chronic health conditions.
Choice D reason: A client who is taking medication for hypertension is not necessarily a priority for pneumonia vaccination based solely on their hypertension. While hypertension is a common condition, it does not directly increase the risk of pneumococcal disease. However, if the client has other risk factors or comorbidities, they may still be considered for vaccination.
Choice E reason: A client who had a cholecystectomy last year is not a priority for pneumonia vaccination based on this surgical history alone. A cholecystectomy, which is the removal of the gallbladder, does not increase the risk of pneumococcal disease. Priority for vaccination is typically given to individuals with chronic health conditions, older adults, and those with weakened immune systems.
Correct Answer is A
Explanation
Choice A: Metformin
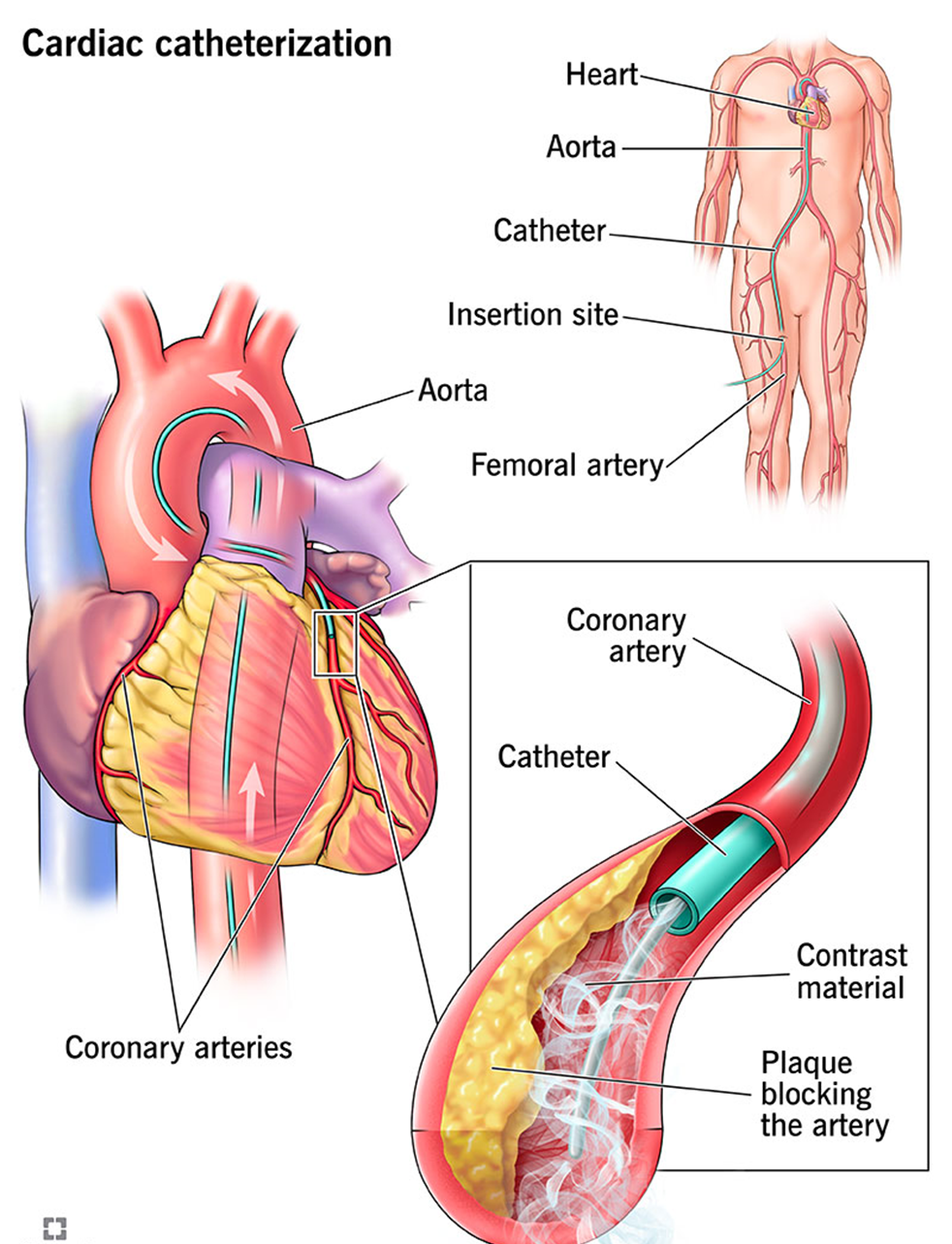
Reason: Metformin is known to interact with contrast material, particularly iodinated contrast media, and can increase the risk of acute kidney injury (AKI). This interaction can lead to a condition known as contrast-induced nephropathy (CIN) or contrast-induced acute kidney injury (CI-AKI). Metformin is primarily excreted by the kidneys, and impaired renal function can lead to its accumulation, increasing the risk of lactic acidosis, a rare but serious complication. Therefore, it is generally recommended to withhold metformin before and after the administration of contrast media until renal function is confirmed to be normal.
Choice B: Carvedilol
Reason: Carvedilol is a beta-blocker used to treat high blood pressure and heart failure. It does not have a known interaction with contrast media that would increase the risk of acute kidney injury. Carvedilol primarily affects the cardiovascular system and does not significantly impact renal function or interact with contrast agents.
Choice C: Nitroglycerin
Reason: Nitroglycerin is used to treat angina and other heart conditions by dilating blood vessels. It does not interact with contrast media in a way that would increase the risk of acute kidney injury. Nitroglycerin’s primary effects are on the cardiovascular system, and it does not have nephrotoxic properties.
Choice D: Atorvastatin
Reason: Atorvastatin is a statin used to lower cholesterol levels. While it can have effects on liver enzymes and muscle tissue, it does not interact with contrast media to increase the risk of acute kidney injury. Atorvastatin is metabolized by the liver and does not significantly impact renal function.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
