A nurse in a provider’s office is caring for a client who is at 34 weeks of gestation and at risk for placental abruption. The nurse should recognize that which of the following is the most common risk factor for abruption?
Cocaine use
Blunt force trauma
Hypertension
Cigarette smoking
The Correct Answer is C
Choice A reason:
Cocaine use: Cocaine use during pregnancy is a significant risk factor for placental abruption. Cocaine causes vasoconstriction, which can reduce blood flow to the placenta and lead to its premature separation from the uterine wall. However, it is not the most common risk factor.
Choice B reason:
Blunt force trauma: Trauma to the abdomen, such as from a car accident or a fall, can cause placental abruption. This type of trauma can lead to the separation of the placenta from the uterine wall, resulting in bleeding and potential complications for both the mother and the fetus.
Choice C reason:
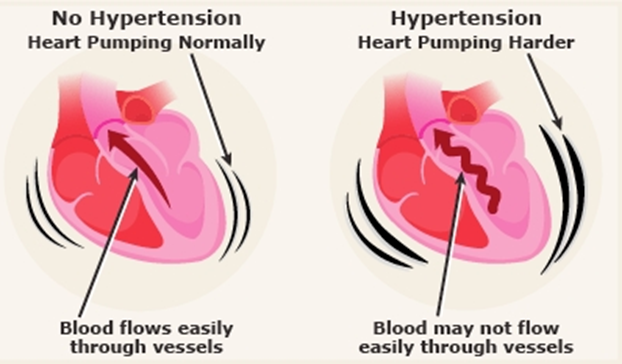
Hypertension: Hypertension, or high blood pressure, is the most common risk factor for placental abruption. Chronic hypertension or pregnancy-induced hypertension (preeclampsia) can damage the blood vessels in the placenta, leading to its premature separation. This condition can significantly increase the risk of placental abruption and is a critical factor to monitor in pregnant women.
Choice D reason:
Cigarette smoking: Smoking during pregnancy is another risk factor for placental abruption. Nicotine and other harmful substances in cigarettes can affect placental blood flow and increase the risk of abruption. However, like cocaine use, it is not the most common risk factor.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Choice A Reason:
Using the intercostal space as a landmark for measuring chest circumference is not standard practice. The intercostal spaces are the spaces between the ribs, and using them as a reference point can lead to inconsistent measurements due to variations in rib spacing and positioning.
Choice B Reason:
The xiphoid process is the lower part of the sternum. While it is a significant anatomical landmark, it is not used for measuring chest circumference in newborns. The xiphoid process is located too low on the chest to provide an accurate and consistent measurement of chest circumference.
Choice C Reason:
The sternal notch, also known as the jugular notch, is the upper part of the sternum. Similar to the xiphoid process, it is not used for measuring chest circumference in newborns. The sternal notch is located too high on the chest and does not provide a consistent reference point for chest circumference measurements.
Choice D Reason:
The nipple line is the correct anatomical landmark for measuring the chest circumference of a newborn. This method ensures that the measurement is taken at a consistent and reproducible location across different individuals, providing an accurate assessment of the chest size relative to growth and development standards.
Correct Answer is D
Explanation
Choice A reason:
A large amount of vaginal bleeding is not typically associated with an ectopic pregnancy. While some vaginal bleeding can occur, it is usually light and not the primary symptom. Heavy bleeding is more commonly associated with other complications such as miscarriage or placental issues.
Choice B reason:
Uterine enlargement greater than expected for gestational age is not a characteristic of ectopic pregnancy. In fact, the uterus may not enlarge significantly because the pregnancy is occurring outside the uterine cavity. This symptom is more indicative of conditions like molar pregnancy.
Choice C reason:
Severe nausea and vomiting are common symptoms of a normal pregnancy due to hormonal changes but are not specific to ectopic pregnancy. While some women with ectopic pregnancies may experience nausea and vomiting, these symptoms alone are not diagnostic.
Choice D reason:
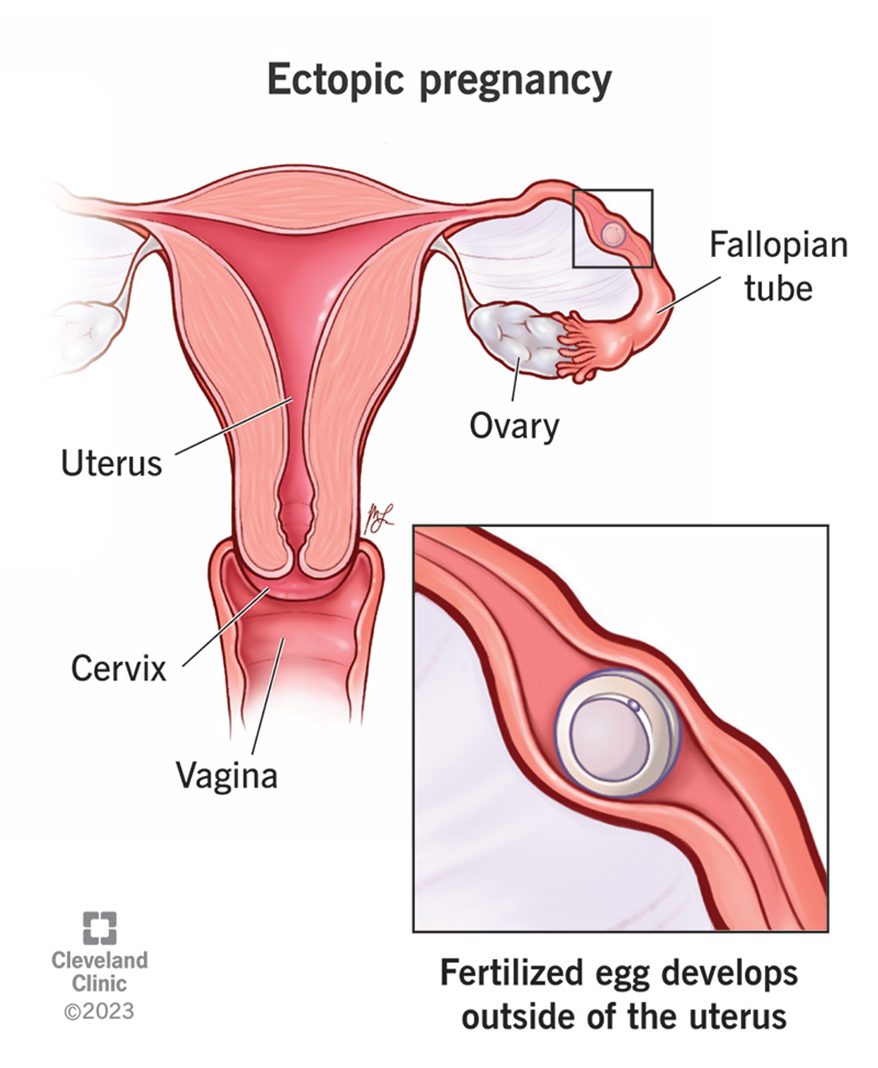
Unilateral, cramp-like abdominal pain is a hallmark symptom of ectopic pregnancy. This pain typically occurs on one side of the abdomen, corresponding to the location of the ectopic implantation, usually in a fallopian tube. The pain can become severe and is often accompanied by light vaginal bleeding. If the fallopian tube ruptures, the pain can become intense and may be accompanied by signs of internal bleeding, such as dizziness, shoulder pain, and shock.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
