A nurse is assessing a client’s cranial nerves. Which methods should the nurse use to assess cranial nerve V?
Ask the client to clench their teeth and assess facial sensation.
Ask the client to identify scented aromas.
Ask the client to read a Snellen chart.
Ask the client to raise his eyebrows.
The Correct Answer is A
Choice A Reason:
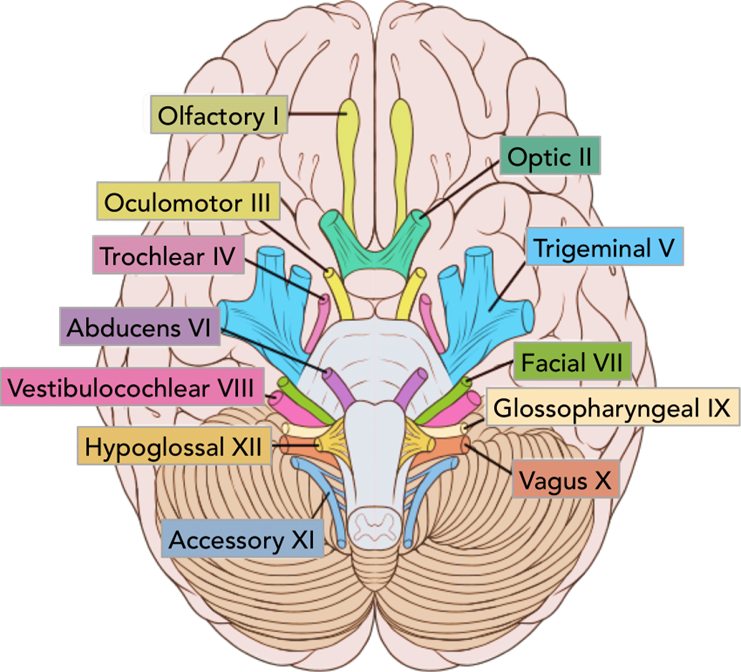
Cranial nerve V is the trigeminal nerve, which has both motor and sensory functions: Motor function: The nurse can assess this by asking the client to clench their teeth while palpating the masseter and temporalis muscles for strength. Sensory function: The nurse can assess this by lightly touching the client's face in different areas (forehead, cheeks, and jaw) with a cotton ball or sharp/dull object to check for sensation.
Choice B Reason:
Asking the client to identify scented aromas is a method used to assess cranial nerve I (Olfactory), not cranial nerve V. Cranial nerve V (Trigeminal) is assessed by testing facial sensation and motor functions such as chewing.
Choice C Reason:
Asking the client to read a Snellen chart is a method used to assess cranial nerve II (Optic), which is responsible for vision. This method does not assess cranial nerve V
Choice D Reason:
Asking the client to raise his eyebrows is a method used to assess cranial nerve VII (Facial), which controls facial expressions. This method is not used to assess cranial nerve V.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A reason: Apple juice is an appropriate choice for a full liquid diet. It is a clear liquid that provides hydration and some nutrients without putting strain on the digestive system. Apple juice is easily digestible and does not contain any solid particles that could be problematic for a client recovering from abdominal surgery.
Choice B reason: Smoothies can be included in a full liquid diet as long as they are well-blended and do not contain any solid chunks. Smoothies can provide essential nutrients and calories, which are important for recovery. They can be made with fruits, vegetables, and protein supplements to ensure a balanced intake.
Choice C reason: Mashed potatoes and gravy are not suitable for a full liquid diet. Although mashed potatoes are soft, they are not liquid and can be difficult to digest for someone on a full liquid diet. The gravy may also contain small particles or thickeners that are not appropriate for this diet. A full liquid diet is intended to include only foods that are completely liquid or will turn to liquid at room temperature.
Choice D reason: Chicken broth is an excellent choice for a full liquid diet. It is a clear liquid that provides hydration and some nutrients without adding any solid particles to the diet. Chicken broth is gentle on the digestive system and can help maintain electrolyte balance.
Correct Answer is ["1"]
Explanation
We know:
- The prescribed dose is 25 mg.
- The available concentration is 125 mg per 5 mL.
Step 2 is to set up the calculation.
We will use the formula: (Desired Dose in mL) = (Prescribed Dose in mg × Volume Available in mL) ÷ Concentration Available in mg
Step 3 is to plug in the values into the formula.
(Desired Dose in mL) = (25 mg × 5 mL) ÷ 125 mg
Step 4 is to perform the multiplication first.
25 mg × 5 mL = 125
Step 5 is to perform the division.
125 ÷ 125 mg = 1 mL
Step 6 is the result.
The nurse should administer 1 mL per dose.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
