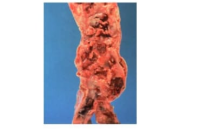
The luminal surface of the abdominal aorta is examined during the autopsy of a 72-year-old woman (shown). Which of the following terms best describes this pathologic finding?
Deep venous thrombosis
Fatty streak
Pulmonary saddle embolus
Severe complicated atherosclerosis
Varicose vein
The Correct Answer is D
A. Deep venous thrombosis: Deep venous thrombosis is the formation of a clot in the deep veins of the lower extremities. It affects the venous system rather than the arterial system, and it does not produce the plaque-laden, irregular arterial surface described in this case.
B. Fatty streak: Fatty streaks are early, flat lesions of atherosclerosis composed primarily of lipid-laden foam cells within the intima. They appear smooth and yellow, lacking the ulceration, thrombus, and irregular surface characteristic of advanced or complicated atherosclerosis.
C. Pulmonary saddle embolus: A pulmonary saddle embolus refers to a large thrombus lodged at the bifurcation of the main pulmonary arteries. It is not related to chronic arterial plaque formation or luminal irregularity in the aorta.
D. Severe complicated atherosclerosis: Complicated atherosclerosis occurs when plaques progress to include ulceration, thrombosis, calcification, and fibrosis. The “cobblestoned” luminal surface, yellow-white plaques, ulcerations, and superimposed thrombus observed in this patient are hallmarks of advanced, complicated atherosclerotic disease.
E. Varicose vein: Varicose veins are dilated, tortuous superficial veins, most commonly in the lower extremities. They are venous abnormalities and do not affect the abdominal aorta or produce a plaque-laden, ulcerated luminal surface.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
A. Atherosclerosis:Atherosclerosis is a chronic disease characterized by plaque buildup in large and medium-sized arteries, leading to reduced blood flow. It commonly manifests as angina pectoris when coronary arteries are involved and intermittent claudication when peripheral arteries are affected. Risk factors such as obesity further increase susceptibility, making atherosclerosis the most likely underlying cause.
B. Deep venous thrombosis:Deep venous thrombosis involves clot formation in the deep veins, usually of the lower extremities, leading to unilateral leg swelling, pain, and redness. It does not cause angina or chronic intermittent claudication, as it affects the venous rather than the arterial system.
C. Diabetes mellitus:Diabetes is a risk factor for atherosclerosis but is not in itself the primary disease process causing angina or intermittent claudication. While it contributes to endothelial dysfunction and accelerated vascular disease, the direct pathology is still atherosclerotic plaque formation.
D. Necrotizing vasculitis:Necrotizing vasculitis involves inflammation and destruction of vessel walls, often causing systemic symptoms like fever, malaise, and organ-specific ischemia. It is uncommon and typically does not present with classic angina or peripheral artery disease patterns seen in this patient.
E. Systemic hypertension:Hypertension is a major risk factor for atherosclerosis and cardiovascular disease, but it is a contributing factor rather than the direct cause of angina or intermittent claudication. The arterial obstruction in this patient is primarily due to plaque buildup rather than elevated blood pressure alone.
Correct Answer is C
Explanation
A. Fat vacuoles within the alveolar capillaries:Fat embolism typically occurs after long bone fractures and manifests with respiratory distress, petechial rash, and neurologic changes. This patient’s fracture was limited to the ankle, a smaller bone, and the rapid cardiovascular collapse suggests a massive occlusive event rather than fat embolism.
B. Thromboembolus occluding the branch of the left pulmonary artery to the left upper lobe:A segmental pulmonary embolus would cause localized hypoxemia and pleuritic pain but is unlikely to produce sudden unresponsiveness and pulseless electrical activity. The severity of this patient’s collapse suggests a more proximal obstruction.
C. Saddle pulmonary thromboembolus occluding the bifurcation of the pulmonary trunk:Massive pulmonary embolism, often termed a “saddle” embolus, can occlude the main pulmonary artery bifurcation, abruptly increasing pulmonary vascular resistance. This results in right ventricular failure, severe hypoxemia, pulseless electrical activity, and rapid death, consistent with this patient’s sudden deterioration four days post-surgery, with multiple risk factors including obesity and oral contraceptive use.
D. Acute myocardial infarct of the anterior wall of the left ventricle:Acute myocardial infarction can cause sudden death but typically presents with chest pain, ST-segment changes, or preceding ischemic symptoms. The immediate post-operative context and massive pulmonary compromise favor pulmonary embolism as the underlying cause.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
