A nurse is admitting a client to a medical-surgical unit.
When performing medication reconciliation for the client, which of the following actions should the nurse take?
A. Compare new prescriptions with the list of medications the client reports
B. Encourage the client to make his own list after he returns to his home
Include any adverse effects of the medications the client might develop
Exclude nutritional supplements from the list of medications the client reports
The Correct Answer is A
The correct answer is choice A. The nurse should compare new prescriptions with the list of medications the client reports. This is part of the medication reconciliation process, which is done to avoid medication errors such as omissions, duplications, dosing errors, or drug interactions. It should be done at every transition of care in which new medications are ordered or existing orders are rewritten.
Choice B is wrong because the nurse should not encourage the client to make his own list after he returns to his home. The nurse should provide the client with an updated and accurate list of medications before discharge and instruct the client to keep it with him at all times.
Choice C is wrong because the nurse should not include any adverse effects of the medications the client might develop. The nurse should include any known allergies or adverse reactions the client has experienced in the past, but not potential adverse effects that have not occurred.
Choice D is wrong because the nurse should not exclude nutritional supplements from the list of medications the client reports. The nurse should include all prescription medications, herbals, vitamins, nutritional supplements, over-the-counter drugs, vaccines, diagnostic and contrast agents, radioactive medications, parenteral nutrition, blood derivatives, and intravenous solutions in the medication reconciliation process.
Some of these products may interact with prescribed medications or affect laboratory results.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Enoxaparin is a blood thinner that helps prevent the formation of blood clots in people who have certain medical conditions or who are undergoing certain procedures. Enoxaparin can increase the risk of bleeding, especially if taken with other medications that affect blood clotting, such as nonsteroidal anti-inflammatory drugs (NSAIDs) or aspirin.
Therefore, the nurse should instruct the client to avoid taking pain relievers such as naproxen sodium (choice A), ibuprofen (choice B), or aspirin (choice D) while on enoxaparin. These pain relievers can make the client more likely to bleed when on enoxaparin. Acetaminophen (choice C) is a pain reliever that does not affect blood clotting and can be taken safely with enoxaparin. However, the client should follow the directions on the box to make sure they do not take more than the recommended amount of acetaminophen, as it can cause liver damage in high doses.
Correct Answer is D
Explanation
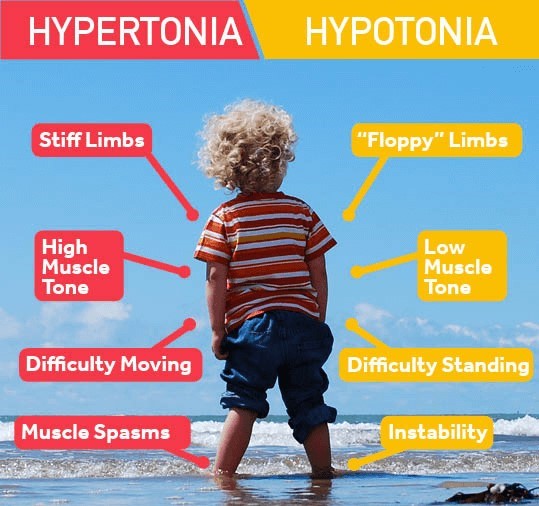
Hypertonicity is a sign of increased muscle tone and stiffness, which can indicate that the newborn is experiencing withdrawal from methadone exposure in utero. Methadone is an opioid medication that can cross the placenta and cause neonatal abstinence syndrome (NAS) in the newborn.
Choice A, acrocyanosis, is wrong because it is a normal finding in newborns.
Acrocyanosis is a bluish discoloration of the hands and feet due to immature peripheral circulation. It usually resolves within the first 24 to 48 hours of life.
Choice B, bradycardia, is wrong because it is not a typical sign of withdrawal.
Bradycardia is a slow heart rate, usually less than 100 beats per minute in newborns. It can be caused by hypoxia, hypothermia, hypoglycemia, or vagal stimulation.
Choice C, bulging fontanels, is wrong because it is a sign of increased intracranial pressure, not withdrawal. Bulging fontanels can be caused by meningitis, hydrocephalus, or hemorrhage.
Normal ranges for newborn vital signs are as follows:
- Heart rate: 120 to 160 beats per minute
- Respiratory rate: 30 to 60 breaths per minute
- Temperature: 36.5 to 37.5°C (97.7 to 99.5°F)
- Blood pressure: 60 to 80 mm Hg systolic and 40 to 50 mm Hg diastolic
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
