A nurse is caring for a 7-year-old child who has a fever, tachycardia, and low oxygen saturation. The nurse reviews the child's laboratory results and notes the following:
- WBC count 15,000/mm^3^ (normal range: 5,000 to 10,000/mm^3^)
- Hgb 8 g/dL (normal range: 10 to 15.5 g/dL)
- Hct 32% (normal range: 32% to 44%)
The nurse should suspect that the child has which of the following conditions?
Leukemia.
Sickle cell anemia.
Hemophilia.
Iron deficiency anemia.
The Correct Answer is B
Choice A reason: Leukemia is not a probable condition, as it is a cancer of the white blood cells that causes abnormal proliferation and accumulation of immature or dysfunctional white blood cells. The child has a high WBC count, which can indicate leukemia, but not necessarily. The child does not have other signs of leukemia, such as bleeding, bruising, bone pain, or lymphadenopathy.
Choice B reason: Sickle cell anemia is a possible condition, as it is an inherited disorder that affects the shape and function of the red blood cells, causing them to become sickle-shaped and rigid. The child has a low Hgb and Hct, which can indicate anemia, and a fever, tachycardia, and low oxygen saturation, which can indicate a sickle cell crisis. A sickle cell crisis is a condition where the sickle-shaped red blood cells block the blood flow and cause tissue ischemia and inflammation.
Choice C reason: Hemophilia is not a likely condition, as it is an inherited disorder that affects the clotting factors, causing impaired blood clotting and increased risk of bleeding. The child has a low Hgb and Hct, which can indicate anemia, but not necessarily hemophilia. The child does not have other signs of hemophilia, such as bleeding, bruising, hemarthrosis, or hematuria.
Choice D reason: Iron deficiency anemia is not a definite condition, as it is a type of anemia that occurs when the body does not have enough iron to produce hemoglobin, the protein that carries oxygen in the blood. The child has a low Hgb and Hct, which can indicate iron deficiency anemia, but not necessarily. The child does not have other signs of iron deficiency anemia, such as pallor, fatigue, weakness, or pica.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
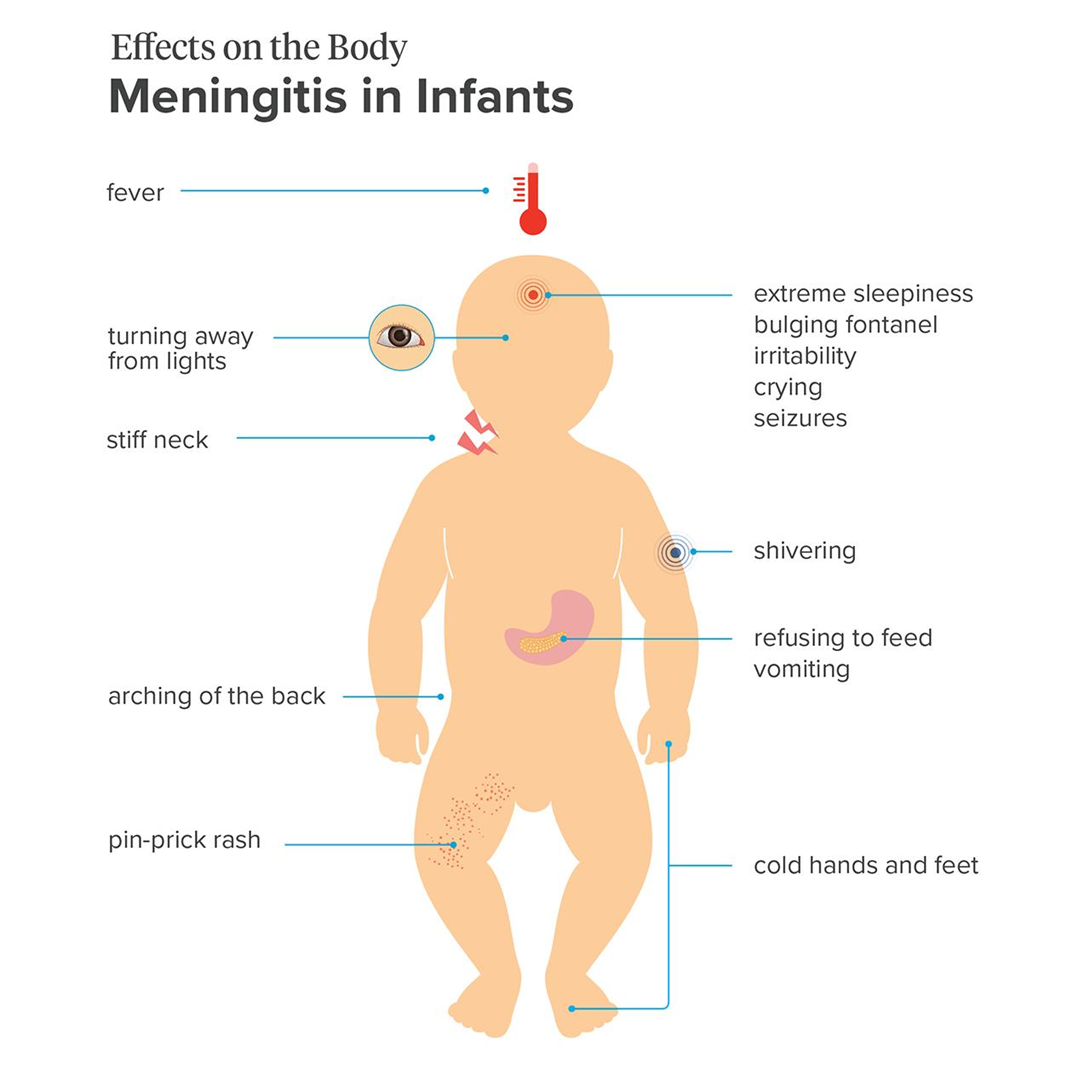
Choice A reason: Meningitis is a possible condition, as it is an inflammation of the membranes that cover the brain and spinal cord. It can be caused by various microorganisms, such as bacteria, viruses, or fungi. The infant has many signs and symptoms of meningitis, such as fever, irritability, lethargy, bulging fontanel, and clear cerebrospinal fluid from the lumbar puncture.
Choice B reason: Hydrocephalus is not a likely condition, as it is an accumulation of cerebrospinal fluid in the brain, which causes increased intracranial pressure and enlargement of the head. The infant has a bulging fontanel, which can indicate increased intracranial pressure, but not necessarily hydrocephalus. The infant does not have other signs of hydrocephalus, such as a rapidly increasing head circumference, prominent scalp veins, or sunset eyes.
Choice C reason: Intracranial hemorrhage is not a probable condition, as it is a bleeding within the skull, which can result from trauma, vascular malformation, or coagulation disorder. The infant has retinal hemorrhages, which can indicate intracranial hemorrhage, but not necessarily. The infant does not have other signs of intracranial hemorrhage, such as seizures, vomiting, or altered mental status.
Choice D reason: Sepsis is not a definite condition, as it is a systemic inflammatory response to an infection, which can cause organ dysfunction and shock. The infant has a fever, which can indicate sepsis, but not necessarily. The infant does not have other signs of sepsis, such as tachycardia, tachypnea, hypotension, or poor perfusion.
Correct Answer is B
Explanation
Choice A reason: A protective environment is a type of isolation precaution that is used for patients who are immunocompromised and at high risk of infection from environmental sources, such as fungi or bacteria. It involves using a private room with positive air pressure, high-efficiency particulate air (HEPA) filtration, and strict hand hygiene. It is not indicated for patients who have measles, as they are the source of infection, not the susceptible host.
Choice B reason: Airborne is a type of isolation precaution that is used for patients who have diseases that are transmitted by small droplets that can remain suspended in the air and travel over long distances, such as tuberculosis, chickenpox, or measles. It involves using a private room with negative air pressure, HEPA filtration, and respiratory protection for health care workers and visitors. It is the appropriate isolation precaution for patients who have measles, as it prevents the spread of the virus to others.
Choice C reason: Contact is a type of isolation precaution that is used for patients who have diseases that are transmitted by direct or indirect contact with the patient or their environment, such as Clostridioides difficile, scabies, or impetigo. It involves using a private room or cohorting with similar patients, wearing gloves and gowns, and using dedicated equipment. It is not indicated for patients who have measles, as the disease is not spread by contact.
Choice D reason: Droplet is a type of isolation precaution that is used for patients who have diseases that are transmitted by large droplets that are generated by coughing, sneezing, or talking, such as influenza, pertussis, or meningitis. It involves using a private room or cohorting with similar patients, wearing a surgical mask, and maintaining a distance of at least 3 feet from the patient. It is not indicated for patients who have measles, as the disease is spread by airborne transmission.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
