A nurse is caring for a patient after a radical neck dissection.
What should be the nurse’s priority in the immediate postoperative period?
Ineffective airway clearance related to thick, copious secretions.
Impaired verbal communication related to the tracheostomy.
High risk for infection related to surgical incisions.
Malnourishment related to NPO Status and dysphagia.
The Correct Answer is A
Rationale for Choice A:
Ineffective airway clearance is the most immediate and life-threatening concern in the postoperative period following a radical neck dissection. This procedure involves extensive removal of lymph nodes and tissues in the neck, which can significantly disrupt normal respiratory function and airway patency. Here's a detailed explanation of the factors contributing to this risk:
Altered Respiratory Anatomy: The surgical resection of tissues and lymph nodes can directly impact the structure and function of the airway. This includes potential narrowing of the trachea, vocal cord dysfunction, and impaired laryngeal movement, all of which can hinder effective airflow.
Thick, Copious Secretions: The surgical trauma and manipulation of tissues often lead to increased production of thick, tenacious secretions in the respiratory tract. These secretions can obstruct the airway, making it difficult for the patient to clear them effectively.
Impaired Cough Reflex: The surgical dissection may disrupt the nerves involved in the cough reflex, which is a crucial mechanism for clearing secretions from the airway. This further impedes the patient's ability to maintain a patent airway.
Risk of Aspiration: Accumulation of secretions in the airway elevates the risk of aspiration, which can lead to pneumonia and other serious complications.
Potential for Edema: Postoperative swelling in the neck tissues can further compress the airway, exacerbating the risk of obstruction.
Nursing Interventions for Ineffective Airway Clearance:
Prompt recognition and management of ineffective airway clearance are essential to prevent respiratory compromise and ensure patient safety. Here are key nursing interventions that should be prioritized:
Frequent Assessment: Continuously monitor respiratory rate, effort, breath sounds, oxygen saturation, and level of consciousness for any signs of respiratory distress.
Positioning: Elevate the head of the bed to 30-45 degrees to promote lung expansion and facilitate drainage of secretions. Suctioning: Regularly suction the airway to remove secretions, using aseptic technique and proper suctioning pressure.
Deep Breathing and Coughing Exercises: Encourage and assist the patient with deep breathing and coughing exercises to mobilize secretions.
Humidification: Provide humidified oxygen or use a nebulizer to help thin secretions and make them easier to expectorate.
Chest Physiotherapy: Perform chest physiotherapy techniques, such as percussion and vibration, to loosen secretions and promote their removal.
Monitoring Fluid Balance: Maintain adequate hydration to help thin secretions, while closely monitoring fluid intake and output to prevent fluid overload.
Addressing Other Choices:
While the other choices may also be relevant concerns in the postoperative period, they do not pose the same immediate threat to life as ineffective airway clearance.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
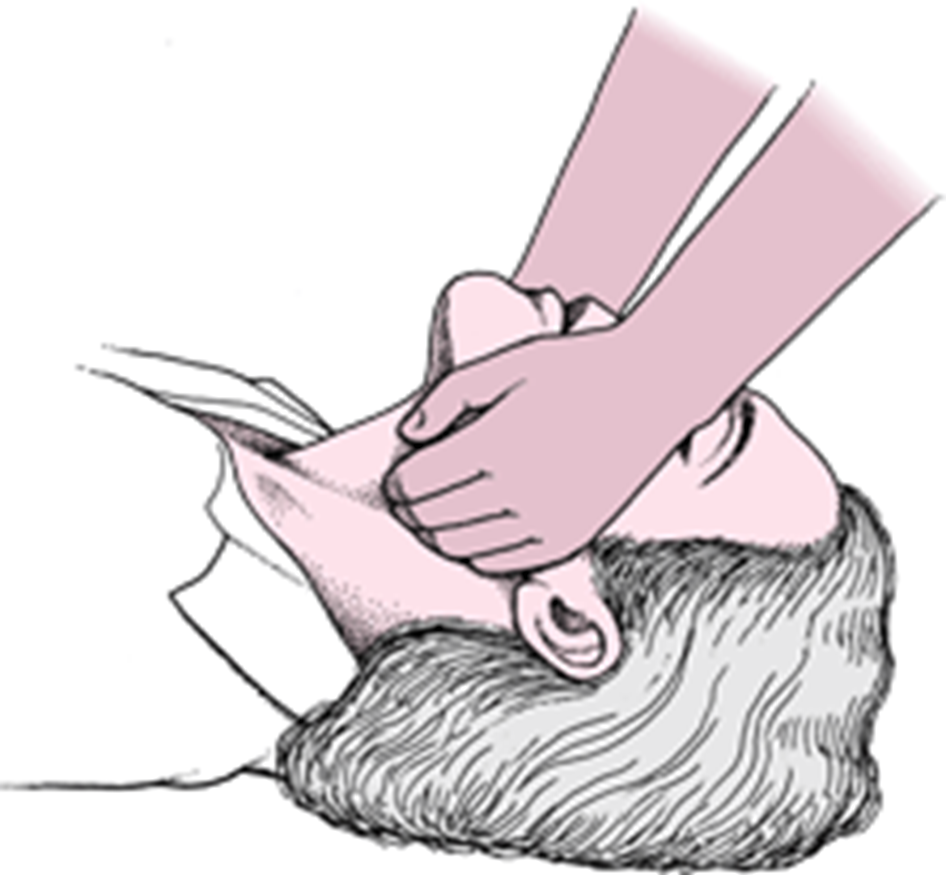
Establishing an open airway is the most crucial and immediate action in any respiratory arrest situation, including when a client has heart failure. Here's a detailed explanation: 1. Airway patency is paramount for survival: Oxygen, the essential element for life, cannot reach the lungs and bloodstream without a clear and unobstructed airway. Brain cells are extremely sensitive to oxygen deprivation and start to die within minutes without it, leading to irreversible brain damage or death. 2. Respiratory arrest in heart failure: Heart failure often leads to fluid buildup in the lungs (pulmonary edema), which can significantly impair breathing. Respiratory arrest can occur due to: Excessive fluid accumulation in the lungs. Weakening of respiratory muscles due to fatigue or heart failure itself. Arrhythmias or heart blocks affecting heart's ability to pump effectively. 3. Steps to establish an open airway: Head tilt-chin lift maneuver: Gently tilt the head back and lift the chin to open the airway. Jaw thrust maneuver: If a neck injury is suspected, use the jaw thrust maneuver to avoid further injury. Removal of any visible obstructions: Clear any visible foreign objects or fluids from the mouth or throat. Use of airway adjuncts: Consider using oral or nasal airways to maintain airway patency, especially if the patient is unconscious.
4. Rationale for other choices:
A. Auscultating for breath sounds: While important for assessment, it does not address the immediate need to establish airflow.
C. Establishing IV access: IV access is necessary for medications and fluids, but airway takes priority in respiratory arrest.
D. Feeling for a carotid pulse: Checking for a pulse is essential, but only after ensuring an open airway and attempting to restore breathing.
5. Importance of prioritizing airway: Establishing an open airway allows for potential rescue breaths and ventilation, which can help restore oxygen levels and prevent further deterioration. Even if a pulse is present, without a clear airway, oxygen cannot reach the vital organs, leading to organ failure and death.
Correct Answer is D
Explanation
Choice A rationale:
Distended neck veins are not a reliable indicator of dehydration in adults. They can be caused by other factors, such as heart failure or fluid overload.
In cases of dehydration, the veins in the neck may actually be less visible due to decreased blood volume.
It's important to assess for other signs and symptoms of dehydration, such as urine output, skin turgor, and vital signs, to make an accurate diagnosis.
Choice B rationale:
A bounding pulse can be a sign of dehydration, but it can also be caused by other factors, such as anxiety, exercise, or fever. It's important to assess the pulse rate and rhythm in conjunction with other signs and symptoms to determine the cause.
A normal pulse rate is 60-100 beats per minute in adults. A bounding pulse is typically a strong, forceful pulse that can be easily felt.
Choice C rationale:
A blood pressure of 146/94 mm Hg is considered elevated, but it is not necessarily a sign of dehydration. Blood pressure can be elevated due to other factors, such as stress, pain, or underlying medical conditions. It's important to assess blood pressure in conjunction with other signs and symptoms to determine the cause. Choice D rationale:
Urine specific gravity is a measure of the concentration of solutes in the urine. A higher urine specific gravity indicates more concentrated urine, which is a sign of dehydration.
A normal urine specific gravity is 1.005-1.030. A urine specific gravity of 1.034 is considered high and is a strong indicator of dehydration.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
