A patient has been prescribed levothyroxine (Synthroid) for hypothyroidism. The patient inquires if the medication should be taken with food.
What would be the most appropriate response from the nurse?
Always consume this medication with food.
This medication should be taken with a glass of milk.
Consume this medication with juice and crackers.
This medication should be taken on an empty stomach.
The Correct Answer is D
Rationale for Choice A:
It is not recommended to always consume levothyroxine with food. In fact, food can interfere with the absorption of levothyroxine, leading to decreased efficacy of the medication.
Consuming levothyroxine with food can decrease its absorption by up to 30%, which can significantly impact its ability to manage hypothyroidism symptoms.
Certain foods, such as those high in fiber, calcium, or iron, can be particularly problematic, as they can bind to levothyroxine in the gut and further reduce its absorption.
While taking levothyroxine with a small amount of food may be necessary for some individuals who experience gastrointestinal side effects, it's generally recommended to take it on an empty stomach for optimal absorption.
Rationale for Choice B:
Milk is not an ideal beverage to take with levothyroxine, as it can also interfere with absorption. Milk contains calcium, which can bind to levothyroxine and reduce its absorption.
It's best to avoid consuming milk or other calcium-rich beverages within a few hours of taking levothyroxine.
Rationale for Choice C:
Similar to milk, juice and crackers are not ideal choices to take with levothyroxine.
Juice, especially those high in acidity, can affect the absorption of levothyroxine in the gut.
Crackers, often made with refined grains, can be high in fiber, which can also interfere with absorption.
Rationale for Choice D:
Taking levothyroxine on an empty stomach, typically 30-60 minutes before breakfast, is generally recommended to ensure optimal absorption.
This allows the medication to be absorbed more efficiently in the small intestine without being affected by the presence of food.
By taking levothyroxine on an empty stomach, patients can maximize its effectiveness in treating hypothyroidism.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Choice A rationale:
Uncontrolled diabetes mellitus: Corticosteroids can have a hyperglycemic effect, meaning they can raise blood sugar levels. This makes them generally unsuitable for use in patients with uncontrolled diabetes mellitus. In fact, corticosteroids might even worsen glycemic control in these patients. While corticosteroids might be used in some cases of diabetes mellitus, such as to treat diabetic retinopathy or nephropathy, they would be used cautiously and with close monitoring of blood sugar levels.
Choice B rationale:
A recent diagnosis of lung cancer: Corticosteroids are not a primary treatment for lung cancer. They might be used in some cases to help manage symptoms or side effects of other treatments, such as chemotherapy or radiation therapy. However, they would not typically be used as a first-line treatment for lung cancer itself.
Choice C rationale:
Acute exacerbation of COPD: Corticosteroids are a mainstay of treatment for acute exacerbations of COPD. They work by reducing inflammation in the airways, which helps to improve airflow and relieve symptoms such as wheezing, shortness of breath, and chest tightness. Corticosteroids can be given orally, intravenously, or by inhalation. The dose and duration of treatment will depend on the severity of the exacerbation.
Choice D rationale:
Chronic asthma: Corticosteroids are often used as a long-term control medication for chronic asthma. However, they are typically used at lower doses than those used for acute exacerbations of COPD. Inhaled corticosteroids are the preferred form of treatment for chronic asthma, as they deliver the medication directly to the airways and have fewer systemic side effects.
Correct Answer is D
Explanation
Choice A rationale:
Stevens-Johnson syndrome (SJS) is a rare, serious skin condition that is typically caused by an allergic reaction to medication. While amiodarone has been associated with a few cases of SJS, it is not considered a common long-term side effect.
Choice B rationale:
Ventricular tachycardia (VT) is a type of fast heart rhythm that originates in the ventricles of the heart. Amiodarone is actually used to treat VT, so it would be counterintuitive to list it as a long-term side effect.
Choice C rationale:
Pulmonary fibrosis is a condition characterized by scarring of the lung tissue. While amiodarone can cause pulmonary toxicity, which includes pulmonary fibrosis, this is a relatively rare side effect. Moreover, it's usually associated with high doses or
long-term use of the medication.
Choice D rationale:
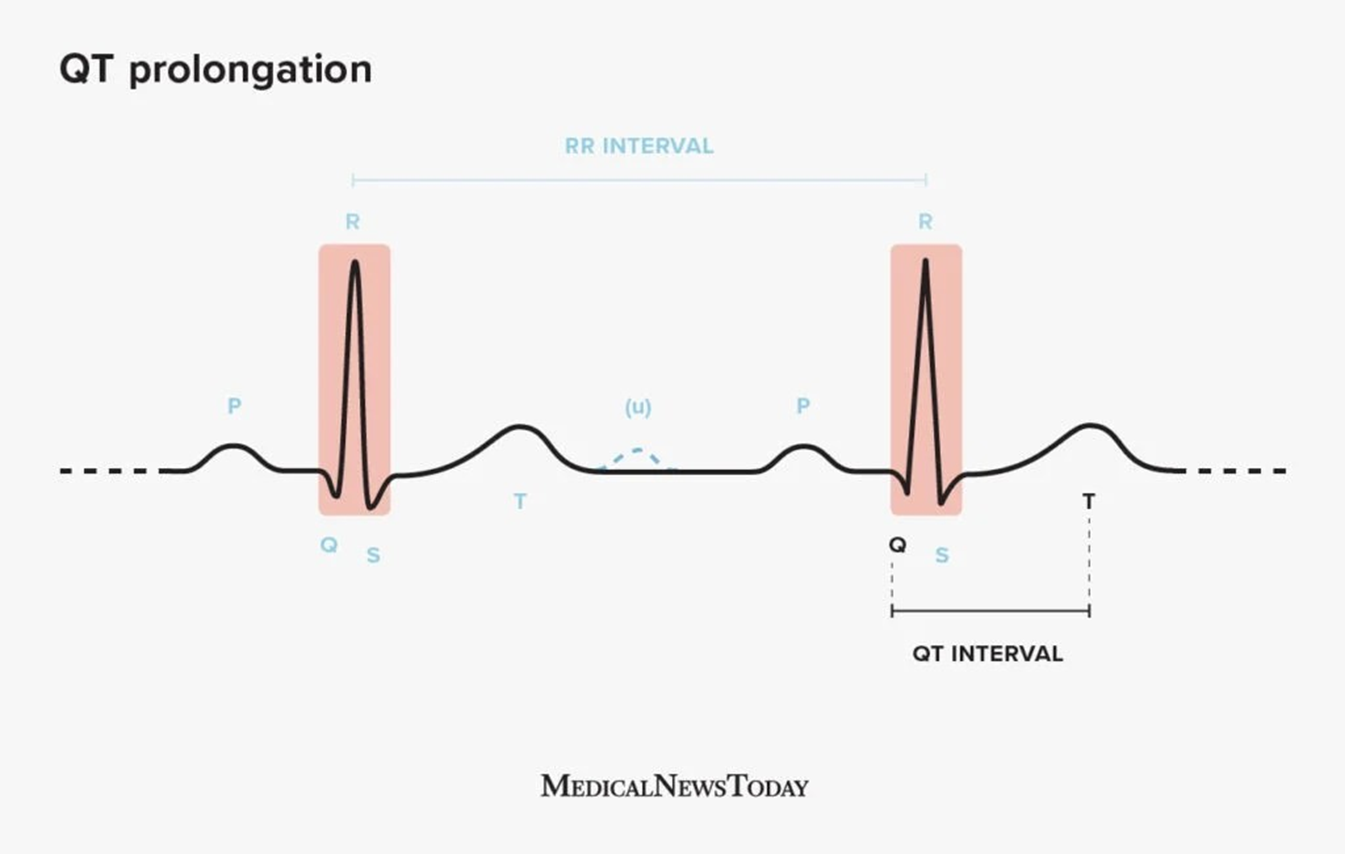
QT prolongation is a condition in which the heart's electrical activity takes longer than normal to recharge between beats. This can lead to a potentially fatal arrhythmia called torsades de pointes. Amiodarone is known to prolong the QT interval, and this is considered one of its most significant long-term side effects. It's important to monitor patients on amiodarone for QT prolongation and to adjust the dose or discontinue the medication if necessary.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
