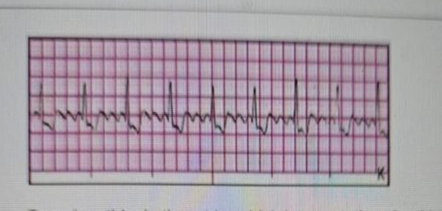
Based on this rhythm strip, which interpretation should the nurse make?
Junctional tachycardia.
Second degree Type II atrioventricular (AV) block (3 to 1).
Ventricular fibrillation.
Atrial flutter.
The Correct Answer is D
A. Junctional tachycardia: Junctional tachycardia originates from the AV node, typically with a narrow QRS, absent or inverted P waves, and a rate of 100–180 bpm. The strip does not show these features.
B. Second-degree Type II AV block (3:1).Type II AV block (Mobitz II) shows dropped QRS complexes with constant PR intervals before conducted beats. This strip does not show missing QRS complexes in a 3:1 pattern.
C. Ventricular fibrillation. VF is characterized by a chaotic, disorganized rhythm with no discernible P waves, QRS complexes, or T waves, completely different from this organized flutter pattern.
D. Atrial flutter is characterized by regular, rapid atrial depolarizations (flutter waves) at a rate of 250–350 bpm. These waves create a "sawtooth" pattern on the ECG.The ventricular response may be regular or irregular, depending on AV conduction. This is different from atrial fibrillation (which has irregularly irregular R-R intervals and no discrete P waves).
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
A. Turn off the pacemaker. Turning off the pacemaker is not appropriate because the client has a third-degree heart block, which means their heart is not conducting impulses properly. Disabling the pacemaker could lead to severe bradycardia or asystole. The goal is to troubleshoot the issue rather than stopping pacing altogether.
B. Check the sensitivity control. Loss of sensing means the pacemaker is not detecting the client's intrinsic heart activity, which can lead to inappropriate pacing or failure to respond to the heart’s natural rhythm. Adjusting the sensitivity setting ensures that the pacemaker can recognize the client's heartbeats and pace appropriately. This is the first step in troubleshooting pacemaker malfunctions related to sensing issues.
C. Increase the milliamps (mA). Increasing the milliamps (mA) is used when there is failure to capture, meaning the pacemaker is delivering impulses but the heart is not responding. Since the problem here is failure to sense, adjusting the sensitivity setting is the correct first action.
D. Position the client on the left side. Repositioning the client is sometimes recommended for displacement of a transvenous pacemaker lead, but in this case, the issue is sensing failure, not lead displacement. Checking and adjusting the pacemaker settings is a more appropriate first step before considering repositioning.
Correct Answer is D
Explanation
A. Administer furosemide IV over ten minutes. While slow IV administration is recommended to prevent ototoxicity, the priority concern is that milrinone and furosemide are incompatible when administered in the same IV line. The nurse must first ensure separate IV access before considering the administration rate.
B. Notify the healthcare provider (HCP) of the incompatibility of the two drugs. The nurse does not need to notify the HCP but should instead use a separate IV line or flush the line thoroughly before and after administration if only one access is available. Milrinone and furosemide should never be mixed, as their combination can cause precipitation, leading to catheter occlusion or embolization.
C. Infuse furosemide through a central line to prevent extravasation. Furosemide can be given peripherally or centrally, but the concern here is drug incompatibility, not extravasation. Furosemide is not a vesicant, so central line administration is not required unless no peripheral access is available.
D. Give furosemide through a separate IV access. Milrinone is incompatible with furosemide due to pH differences, which can lead to precipitation and potential catheter occlusion. To ensure safe administration, furosemide should be given through a separate IV line or, if no secondary access is available, the line should be flushed thoroughly before and after administration.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
