A nurse is collecting data from a client who is 12 hours postpartum following a spontaneous vaginal delivery.
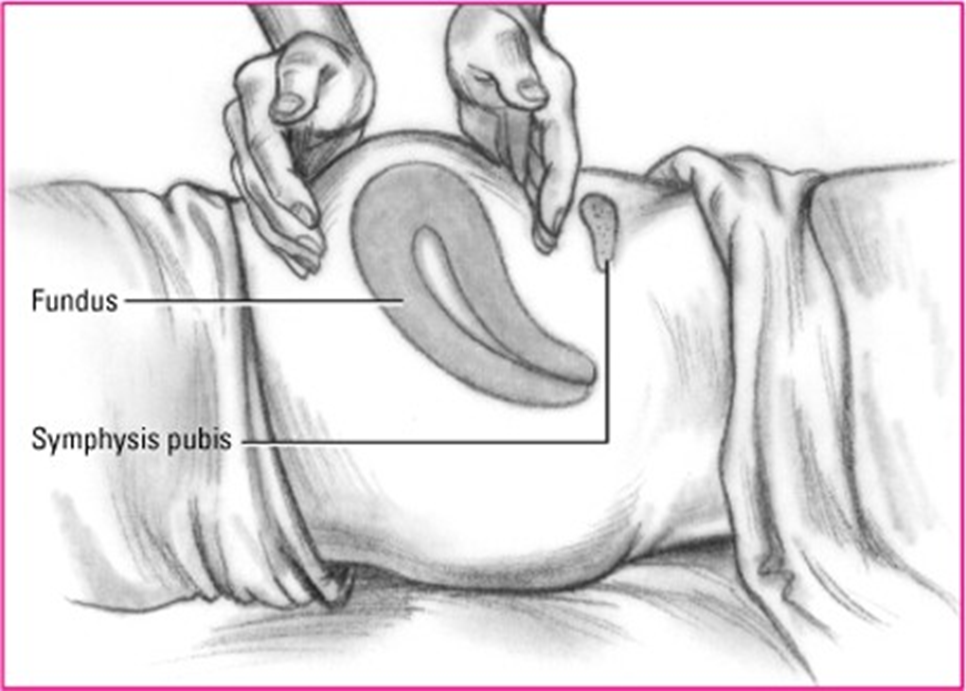
The nurse should expect to find the uterine fundus at which of the following positions on the client’s abdomen?
Three fingerbreadths above the umbilicus
At the level of the umbilicus
One fingerbreadth above the symphysis pubis
One fingerbreadth below the umbilicus
The Correct Answer is B
Choice A rationale:
Three fingerbreadths above the umbilicus is too high for the uterine fundus to be at 12 hours postpartum. Immediately after delivery, the fundus is typically at the level of the umbilicus. It then descends approximately one fingerbreadth per day.
If the fundus is found to be three fingerbreadths above the umbilicus at 12 hours postpartum, it could be a sign of uterine atony, which is a serious condition that can lead to postpartum hemorrhage.
Choice C rationale:
One fingerbreadth above the symphysis pubis is too low for the uterine fundus to be at 12 hours postpartum. This would be more consistent with a woman who is several days postpartum.
Choice D rationale:
One fingerbreadth below the umbilicus is also too low for the uterine fundus to be at 12 hours postpartum. This would be more consistent with a woman who is 1-2 days postpartum.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A rationale:
Placing the mother in Trendelenburg's position would not correct the uterine displacement. Trendelenburg's position involves
lowering the head of the bed and raising the feet, which can actually worsen uterine displacement by increasing pressure on
the uterus from the abdominal organs.
It is not indicated for uterine displacement and could potentially have adverse effects on the patient's hemodynamic status
and respiratory function.
Choice C rationale:
Notifying the physician is important, but it is not the first action the nurse should take.
The nurse should assess the patient and attempt to correct the displacement before notifying the physician.
Choice D rationale:
Recording the findings is important for documentation, but it is not an intervention that will correct the uterine displacement.
Choice B rationale:
Massaging the fundus is the correct action to take when a postpartum uterus is displaced.
The fundus is the top of the uterus, and massaging it can help to stimulate the uterine muscles to contract and return to their
normal position.
This is often effective in correcting mild to moderate uterine displacements.
Here are the steps involved in massaging the fundus:
Locate the fundus: The nurse should first locate the fundus by palpating the abdomen just below the umbilicus.
Apply gentle pressure: Once the fundus is located, the nurse should apply gentle pressure with the fingertips in a circular
motion.
Continue massaging: The massage should be continued for several minutes, or until the uterus is felt to be firm and in the
midline position.
Additional notes:
If the uterine displacement is severe, or if the patient is experiencing pain or bleeding, the nurse should notify the physician
immediately.
Other interventions that may be used to correct uterine displacement include:
Assisting the patient to empty her bladder
Straight catheterization
Administration of oxytocin to stimulate uterine contractions
Correct Answer is A
Explanation
Choice A rationale:
A full bladder can displace the uterus to the right and interfere with its ability to contract properly. This can lead to
postpartum hemorrhage, a serious complication that can occur after childbirth.
Emptying the bladder helps to reposition the uterus in the midline and allows it to contract more effectively. This helps to
prevent postpartum hemorrhage and promotes uterine involution, the process by which the uterus returns to its pre-
pregnancy size.
In this case, the client's fundus is firm, which indicates that it is contracting well. However, it is slightly deviated to the right,
which suggests that the bladder may be full.
Asking the client to empty her bladder is a simple and effective way to address this potential problem.
Choice B rationale:
Repeating the client's temperature evaluation is not a priority action in this case. The client's vital signs are within normal
limits, and there is no indication of infection.
A temperature elevation could be a sign of infection, but it is not the most likely cause of the uterine deviation in this case.
Choice C rationale:
Encouraging the client to nurse more frequently may be helpful in stimulating milk production and uterine contractions.
However, it is not the most immediate priority in this case.
The client's breasts are soft, which suggests that she is not yet producing a significant amount of milk.
The priority is to address the potential problem of a full bladder, which could interfere with uterine involution.
Choice D rationale:
Checking for signs of a urinary tract infection is not a priority action in this case. The client does not have any urinary
symptoms, such as dysuria or frequency.
A urinary tract infection could cause a uterine deviation, but it is not the most likely cause in this case.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
