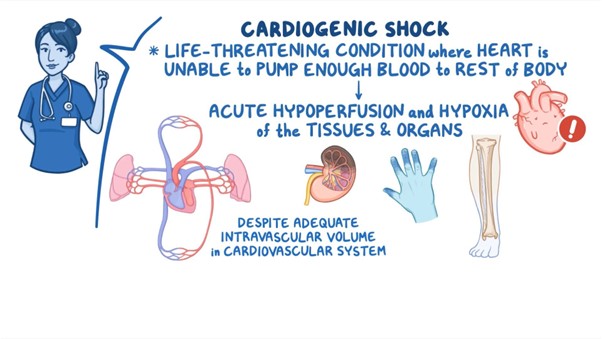
The cardiac ICU nurse is assessing a patient who is in cardiogenic shock. Which hemodynamic manifestations and/or signs and symptoms do the nurse expect? Select all that apply.
Narrowed pulse pressure.
Tachycardia.
Elevated SBP.
Pulmonary congestion.
Pulmonary artery wedge pressure
Correct Answer : A,B,D,E
A. Narrowed pulse pressure: In cardiogenic shock, the cardiac output is compromised, resulting in reduced stroke volume and subsequent narrowed pulse pressure. The pulse pressure is the difference between systolic and diastolic blood pressure.
B. Tachycardia: Tachycardia is a compensatory response in cardiogenic shock, as the body attempts to increase cardiac output to maintain tissue perfusion despite decreased stroke volume. Increased heart rate is a common finding in this condition.
D. Pulmonary congestion: Cardiogenic shock is often associated with impaired left ventricular function, leading to an inadequate pump mechanism. This can result in fluid accumulation and congestion in the pulmonary circulation, leading to pulmonary edema and congestion. Patients may experience symptoms such as dyspnea, crackles on lung auscultation, and increased work of breathing.
E. Elevated pulmonary artery wedge pressure (PAWP): PAWP is a measurement obtained during invasive hemodynamic monitoring. In cardiogenic shock, the impaired left ventricular function leads to increased left atrial pressure, which is reflected by an elevated PAWP. Elevated PAWP indicates increased fluid volume and congestion in the left side of the heart.
C. Elevated SBP in (option C) is incorrect because Elevated systolic blood pressure (SBP) is not a typical finding in cardiogenic shock. Instead, hypotension or decreased blood pressure is commonly observed due to reduced cardiac output.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
Septic shock is a life-threatening condition characterized by severe infection, systemic inflammation, and inadequate tissue perfusion. Hypotension, as indicated by a low blood pressure reading, is a significant concern in septic shock. It reflects inadequate perfusion to vital organs and tissues, leading to potential organ dysfunction and damage.
While all the assessment data provided may be important and require attention, the low blood pressure (BP) reading indicates impaired systemic perfusion and can contribute to end-organ damage. The nurse should prioritize interventions aimed at improving perfusion and stabilizing the patient's blood pressure.
A. Arterial oxygen saturation is 90% in (option A) is incorrect because While an arterial oxygen saturation of 90% is below the desired range, it is not as immediately life-threatening as low blood pressure. Oxygen therapy and interventions to improve oxygenation should still be initiated, but addressing hypotension takes priority.
B. Urine output of 15 ml for 2 hours in (option B) is incorrect because Decreased urine output is a concerning sign, as it may indicate impaired renal perfusion. However, the immediate concern in septic shock is addressing the low blood pressure to improve overall perfusion, including renal perfusion.
C. Apical pulse 110 beats/min in (option C) is incorrect because: Tachycardia is a common finding in septic shock and represents the body's compensatory response to maintain cardiac output. While it requires monitoring and consideration, low blood pressure is a more significant concern.
Correct Answer is C
Explanation
This method, known as the 6-second method, involves counting the number of QRS complexes in a 6-second interval on the electrocardiogram (ECG) strip and then multiplying that number by 10 to calculate the heart rate per minute. The advantage of this method is that it provides a relatively quick estimate of the heart rate.
A. Printing a 1-minute ECG strip and counting the number of QRS complexes in (option A) is incorrect because it can be time-consuming and may not be practical in situations where a quick estimate is needed.
B. Calculating the number of small squares between one QRS complex and the next and dividing into 1500 in (option B) is incorrect because it is a method used to calculate heart rate, known as the "1500 method," but it is not as quick as the 6-second method and requires more time and measurement precision.
D. Counting the number of large squares in the R-R interval and dividing by 300 is another method used to calculate heart rate, known as the "300 method," but it is also less quick and less accurate for assessing heart rate in patients with regular rhythms.
It's important to note that if the heart rhythm is irregular, these methods may not provide an accurate estimate of the heart rate, and a longer monitoring period or a different approach may be necessary.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
