The client was admitted to the medical floor. Upon arrival, the client was assessed: He is difficult to arouse but follows commands. He has a peripheral IV which is infusing normal saline at 145 mL/hr. No redness or edema at the site. Breath sounds are clear and equal bilaterally. He appears pink and well-perfused.
The client had a tonic-clonic seizure that lasted for 3 minutes and 5 seconds. The client became apneic during the seizure and the oxygen saturation dropped to 48%. The client was manually ventilated at 100% oxygen and padding was placed around the vent for safety. After the seizure, the client was turned to his left for recovery.
The physician comes to the bedside following the seizure and prescribes phenytoin. The PN administers the phenytoin as prescribed.
What are the possible toxic effects of phenytoin that the PN should closely monitor the client for after administration?
Select all that apply
Ataxia
Drowsiness
Altered blood coagulation
Anxiety
Aphasia
Vertigo
Visual disturbances
Vomiting
Correct Answer : A,B,C,F,G
Ataxia: Phenytoin can cause problems with coordination and balance, leading to ataxia. The PN should monitor the client for unsteady gait or difficulty with movements.
Drowsiness: Phenytoin can cause drowsiness or sedation. The PN should observe the client for excessive sleepiness or difficulty staying awake.
Altered blood coagulation: Phenytoin can affect blood clotting factors, potentially leading to altered blood coagulation. The PN should assess the client for any signs of bleeding or bruising.
Vertigo: Phenytoin can cause dizziness or vertigo, which is a spinning sensation. The PN should be alert for complaints of dizziness or any difficulty with balance.
Visual disturbances: Phenytoin can cause visual disturbances, such as blurred vision or double vision. The PN should monitor the client's vision and report any changes.
The following options are incorrect regarding the toxic effects of phenytoin:
- Anxiety: Anxiety is not a recognized toxic effect of phenytoin. However, it is important to assess the client for any signs of anxiety or emotional changes.
- Aphasia: Aphasia refers to a language impairment and is not typically associated with the toxic effects of phenytoin.
- Vomiting: While phenytoin can cause gastrointestinal side effects, such as nausea and vomiting, it is not directly related to its toxic effects. However, the PN should still monitor the client for any signs of nausea or vomiting.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
The action the practical nurse (PN) should take in this situation is to administer a prescribed PRN (as needed) dose of analgesic.
Severe burning pain along the right side of the trunk is a common symptom of herpes zoster (shingles). Managing the client's pain is an important aspect of care to provide comfort and promote healing. Administering a prescribed PRN dose of analgesic will help alleviate the client's pain and improve their overall well-being. It is crucial to follow the client's prescribed medication regimen and provide pain relief as needed.
The other options are not the most appropriate actions in this situation:
B. Notifying the nursing supervisor of uncontrolled pain may be necessary if the client's pain persists despite appropriate interventions. However, the first step should be to administer an analgesic to address the immediate pain.
C. Giving the next prescribed dose of antiviral medication is important in the treatment of herpes zoster, but it does not directly address the client's current severe burning pain. Analgesics are specifically designed to alleviate pain symptoms.
D. Obtaining an oxygen tank for home administration is not indicated for the management of pain associated with herpes zoster. Oxygen therapy is typically used for respiratory or circulatory conditions and would not be the appropriate intervention for the client's symptom of severe burning pain.
Correct Answer is D
Explanation
The vital sign trends that indicate increased intracranial pressure (ICP) and should be reported to the charge nurse are:
Bradycardia: A slow heart rate can be a sign of increased ICP.
Irregular respiratory patterns: Abnormal breathing patterns, such as irregular or Cheyne-Stokes respirations, can be indicative of increased ICP.
Widening pulse pressure: An increased difference between systolic and diastolic blood pressure (widening pulse pressure) can be a sign of increased ICP.
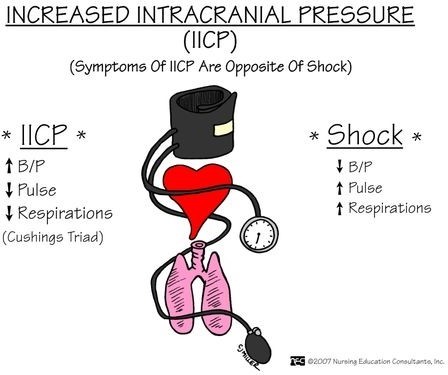
A- Heart rate above 110 beats/minute, elevated respiratory rate, and hypotension: While an elevated heart rate and respiratory rate can be associated with increased ICP, hypotension (low blood pressure) is not typically seen in this condition. Hypotension can be a sign of other factors, such as hypovolemia or shock, which may or may not be related to the head injury.
B- Bounding pulse rate, groaning respiratory effort, and elevated blood pressure: Bounding pulse rate and elevated blood pressure are not specific to increased ICP. They can be influenced by other factors such as pain, anxiety, or medications. Groaning respiratory effort may indicate respiratory distress, but it is not directly related to increased ICP.
C- Thready rapid pulse, trembling, perspiration, weakness, and irritability: These signs and symptoms can be associated with various conditions such as anxiety, stress, or other physiological responses. While they may occur in the context of increased ICP, they are not specific to this condition alone.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
