The nurse is conducting client teaching about cholesterol levels. When discussing the client's elevated LDL and lowered HDL levels, the client shows an understanding of the significance of these levels by making what statement?
"Increased LDL and decreased HDL increase my risk of coronary artery disease."
"Increased LDL has the potential to decrease my risk of heart disease."
"The decreased HDL level will increase the amount of cholesterol moved away from the artery walls."
"The increased LDL will decrease the amount of cholesterol deposited on the artery walls."
The Correct Answer is A
Elevated levels of LDL (low-density lipoprotein) cholesterol are associated with an increased risk of coronary artery disease (CAD). LDL cholesterol is often referred to as "bad" cholesterol because it can contribute to the formation of plaque in the arteries, leading to narrowing and blockage of the arteries supplying the heart. This increases the risk of developing CAD and related complications such as heart attack and stroke.
On the other hand, HDL (high-density lipoprotein) cholesterol is often referred to as "good" cholesterol. HDL cholesterol helps remove excess cholesterol from the bloodstream and transport it back to the liver for processing and excretion. Higher levels of HDL cholesterol are associated with a decreased risk of CAD because it helps to prevent the accumulation of cholesterol on artery walls.
Therefore, understanding that increased LDL and decreased HDL levels increase the risk of coronary artery disease demonstrates a good understanding of the significance of cholesterol levels and their impact on cardiovascular health.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
The client statement that supports the information of intermittent claudication is: "My legs get a painful cramp when I walk over 30 minutes.": Intermittent claudication is a symptom of peripheral artery disease (PAD) characterized by pain, cramping, or fatigue in the muscles of the lower extremities, typically the calves, thighs, or buttocks. This pain is usually triggered by physical activity, such as walking, and is relieved with rest. The pain is caused by inadequate blood flow and oxygen supply to the muscles due to narrowed or blocked arteries.
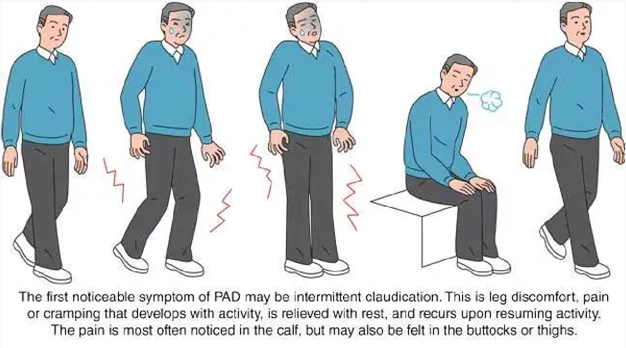
The other client statements do not specifically indicate intermittent claudication:
"My feet feel like I have pins and needles": This sensation of pins and needles is often associated with peripheral neuropathy, which is a condition involving nerve damage and does not directly relate to intermittent claudication.
"When I stand or sit too long, my feet swell": This statement suggests the possibility of venous insufficiency rather than intermittent claudication. Venous insufficiency involves impaired blood return from the legs to the heart and may result in swelling, aching, or heaviness in the legs.
"I get short of breath when I climb a lot of stairs": This symptom is more indicative of cardiovascular or respiratory issues, such as heart or lung disease, rather than intermittent claudication. It suggests that the client may experience exercise intolerance due to cardiopulmonary limitations.
Correct Answer is C
Explanation
The most important finding to report to the health care provider would be the serum potassium level of 3.0 mEq. This is an extremely low potassium level (normal range is typically 3.5-5.0 mEq/L), which can indicate a potentially life-threatening condition called hypokalemia. Furosemide (Lasix) is a diuretic medication that can cause potassium loss in the urine, and a low potassium level can lead to serious cardiac and muscle abnormalities. It is crucial to report this finding promptly to the health care provider for appropriate intervention and monitoring.
Blood glucose level of 175 mg/dL: While an elevated blood glucose level can be a concern, especially for individuals with diabetes, it is not the most critical finding in this situation. The client's primary concern is hypertension, and the administration of IV furosemide is aimed at managing blood pressure. The elevated blood glucose level should still be addressed and monitored, but it is not as urgent as the low potassium level.
Orthostatic systolic BP decrease of 12 mm Hg: Orthostatic hypotension refers to a significant decrease in blood pressure upon standing up. While it is important to assess and manage orthostatic changes, a decrease of 12 mm Hg in systolic blood pressure alone may not be considered clinically significant. It could be a normal response for some individuals. However, if the client experiences symptoms such as dizziness or lightheadedness upon standing, further evaluation may be necessary. Nonetheless, it is not as urgent as the low potassium level.
Current blood pressure reading of 166/94 mm Hg: While this blood pressure reading indicates hypertension, it is not the most critical finding to report in this situation. The nurse is preparing to administer furosemide (Lasix), which is a medication commonly used to treat hypertension. It is expected that the blood pressure will be high before administering the medication. The goal is to monitor the blood pressure after the administration to assess the effectiveness of the medication.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
