A nurse is assessing a client with intermittent claudication. What client statement supports this information?
"My feet feel like I have pins and needles."
"When I stand or sit too long, my feet swell."
"My legs get a painful cramp when I walk over 30 minutes."
"I get short of breath when I climb a lot of stairs.”
The Correct Answer is C
The client statement that supports the information of intermittent claudication is: "My legs get a painful cramp when I walk over 30 minutes.": Intermittent claudication is a symptom of peripheral artery disease (PAD) characterized by pain, cramping, or fatigue in the muscles of the lower extremities, typically the calves, thighs, or buttocks. This pain is usually triggered by physical activity, such as walking, and is relieved with rest. The pain is caused by inadequate blood flow and oxygen supply to the muscles due to narrowed or blocked arteries.
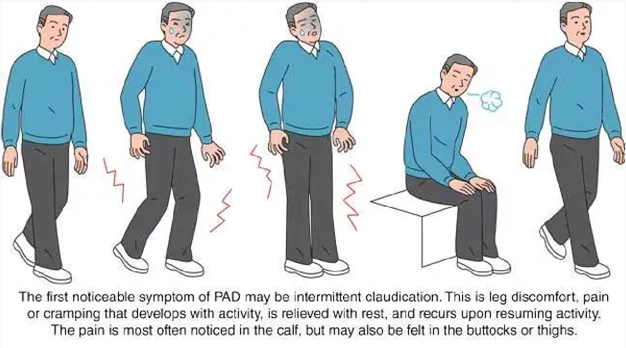
The other client statements do not specifically indicate intermittent claudication:
"My feet feel like I have pins and needles": This sensation of pins and needles is often associated with peripheral neuropathy, which is a condition involving nerve damage and does not directly relate to intermittent claudication.
"When I stand or sit too long, my feet swell": This statement suggests the possibility of venous insufficiency rather than intermittent claudication. Venous insufficiency involves impaired blood return from the legs to the heart and may result in swelling, aching, or heaviness in the legs.
"I get short of breath when I climb a lot of stairs": This symptom is more indicative of cardiovascular or respiratory issues, such as heart or lung disease, rather than intermittent claudication. It suggests that the client may experience exercise intolerance due to cardiopulmonary limitations.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["D","E"]
Explanation
The traces that should require immediate follow-up by the nurse are:
● Pacer spikes occur directly before the T waves.
Pacer spikes occurring on the T waves indicate an issue with the pacemaker's timing or sensing. This could lead to inappropriate pacing or pacing during the refractory period, which can be detrimental to the client's heart function.
● The heart rate is outside of programmed parameters.
If the heart rate is outside of the programmed parameters set for the client's pacemaker, it may indicate a malfunction or failure of the device or a change in the client's cardiac status. It is important for the nurse to assess the client's condition and notify the healthcare provider for further evaluation and intervention.
Let's review the other options and explain why they do not require immediate follow-up:
Pacer spikes are adequate in number: This indicates that the pacemaker is delivering the appropriate number of electrical impulses as programmed. As long as the other parameters are normal, this finding does not require immediate follow-up.
Pacer spikes occur directly before the P waves: This is the desired and expected pattern for a pacemaker in normal sinus rhythm. It indicates proper timing and coordination between the pacemaker and the client's intrinsic electrical activity.
Pacer spikes occur directly before the QRS waves: This is also the desired and expected pattern for a pacemaker in clients with ventricular pacing. It indicates proper timing and coordination between the pacemaker and the client's intrinsic electrical activity.
The heart rate is within programmed parameters: If the heart rate falls within the programmed parameters set for the client's pacemaker, it indicates that the device is functioning appropriately in maintaining the desired heart rate.
Correct Answer is B
Explanation
The most appropriate intervention for a client diagnosed with peripheral arterial insufficiency is: Encourage the client to engage in a moderate amount of exercise. Peripheral arterial insufficiency is a condition characterized by reduced blood flow to the extremities, typically the legs, due to narrowed or blocked arteries. Regular exercise is an important component of managing peripheral arterial insufficiency. Exercise helps improve circulation, promote collateral blood vessel development, and increase the distance a client can walk before experiencing pain (intermittent claudication). Therefore, encouraging the client to engage in a moderate amount of exercise, such as walking, under healthcare provider guidance is crucial.]
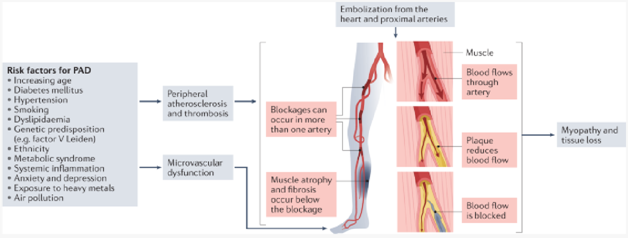
The other options are not appropriate interventions for peripheral arterial insufficiency:
Elevating the legs and arms above the heart when resting: While elevation can be beneficial for certain conditions, such as reducing swelling in venous insufficiency, it is not the primary intervention for peripheral arterial insufficiency. Elevation alone does not improve arterial blood flow and may not effectively address the underlying circulatory issues.
Encouraging extended periods of sitting or standing: Prolonged sitting or standing can further restrict blood flow and exacerbate symptoms in clients with peripheral arterial insufficiency. Encouraging regular movement and avoiding prolonged immobility is important to maintain adequate circulation.
Discouraging walking in order to limit pain: While walking may cause pain or discomfort in clients with peripheral arterial insufficiency (intermittent claudication), it is important to encourage walking as part of an exercise regimen. Walking helps improve symptoms over time and promotes overall cardiovascular health.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
