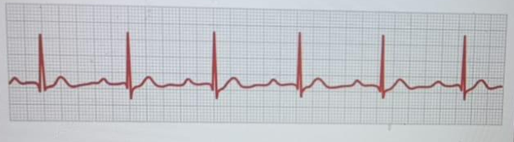
The nurse who is working in the telemetry unit measures the PR interval of the client's rhythm strip depicted below. What is the nurse's analysis of the PR interval?
Atria is taking longer to depolarize and contract
Conduction time is slowed from the SA node to the ventricles
The PR interval is within the normal time limits
Ventricular repolarization is delayed
The Correct Answer is C
A. Atria is taking longer to depolarize and contract: This would be indicated by a prolonged or abnormal P wave, not a normal PR interval. The rhythm strip shows clearly visible, normal-appearing P waves followed by QRS complexes, ruling this out as the correct interpretation.
B. Conduction time is slowed from the SA node to the ventricles: A slowed conduction time would result in a PR interval longer than 0.20 seconds, characteristic of first-degree AV block. The PR interval on this strip measures within the standard range (0.12–0.20 seconds), so this is not accurate.
C. The PR interval is within the normal time limits: The PR interval on the ECG strip spans about 3 to 4 small boxes (0.12–0.16 seconds), which is within the normal range of 0.12 to 0.20 seconds. This indicates normal conduction from the atria through the AV node to the ventricles.
D. Ventricular repolarization is delayed: Delayed ventricular repolarization refers to a prolonged QT interval, not an abnormality in the PR interval. The PR interval evaluates atrial conduction, not ventricular repolarization, so this is an incorrect association.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
A. Review daily the necessity of the central venous catheter: One of the most effective strategies to reduce the risk of catheter-related bloodstream infections is to remove the central line as soon as it is no longer needed. Daily evaluation of necessity prevents prolonged catheter use, which significantly increases infection risk. Removing the source of potential infection is the ultimate preventative action.
B. Maintain a pressure of 300 mm Hg on the flush bag: While maintaining appropriate flush pressure is important for catheter patency and preventing blood clots, it does not play a direct role in preventing bloodstream infections. This action is more related to ensuring adequate line function rather than infection control.
C. Cleanse the insertion site daily with isopropyl alcohol: Current guidelines recommend using chlorhexidine-based solutions rather than isopropyl alcohol for skin antisepsis due to better antimicrobial efficacy. Daily site care is important, but the choice of antiseptic is critical in reducing infection risk.
D. Change the pressurized tubing system and flush bag daily: Tubing and flush systems should be changed typically every 72–96 hours unless contamination is suspected. Changing them daily is not recommended and does not provide added protection against infection it may even increase risk with unnecessary manipulation.
Correct Answer is B
Explanation
A. surgery has caused an episode of supraventricular tachycardia: While stress or surgery can trigger arrhythmias, the ECG shown demonstrates a sinus tachycardia pattern (narrow QRS complexes with identifiable P waves before each QRS), not supraventricular tachycardia (SVT), which typically has a very rapid, regular rhythm often without visible P waves.
B. is febrile which is causing the heart rate to be elevated: The client has a temperature of 102°F (38.8°C), which can increase metabolic demand and lead to sinus tachycardia. Fever is a common and expected cause of elevated heart rate, especially when accompanied by infection, such as the client’s post-op wound infection.
C. is in heart failure and the heart rate is elevated to compensate: There is no evidence from the scenario (no dyspnea, crackles, edema, or reduced BP) that supports heart failure. The elevated HR is more directly related to the fever and infection, not cardiac decompensation.
D. probably has a low oxygen saturation causing an increased respiratory rate: The respiratory rate is slightly elevated (22/min), but there is no mention of hypoxia or oxygen saturation levels. Tachycardia secondary to hypoxia would require clinical indicators of respiratory distress or desaturation, which are not demonstrated.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
