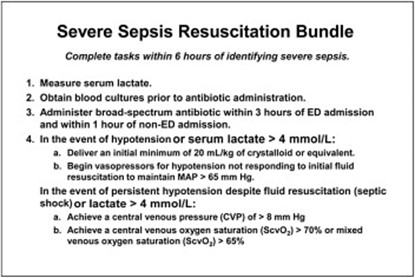
A 29-year-old female patient is admitted to the emergency department with two of the systemic inflammatory response syndrome variables: temperature of 101.2 °F and 14,000 per μL white blood cell count. Which intervention from the sepsis resuscitation bundle does the nurse initiate?
Cooling baths
Broad-spectrum antibiotics
Blood transfusion
NPO status
The Correct Answer is B
The patient's symptoms of fever and elevated white blood cell count suggest a potential infection and sepsis. Broad-spectrum antibiotics should be initiated promptly to cover a wide range of possible pathogens until further diagnostic tests and identification of the specific causative agent are obtained. Early administration of appropriate antibiotics is crucial in sepsis management to target the suspected infection and improve patient outcomes.
A. Cooling baths in (option A) is incorrect because: Cooling baths are typically used in the management of hyperthermia or specific conditions like heatstroke. While the patient has an elevated temperature, it is likely due to the systemic inflammatory response rather than solely hyperthermia.
C. Blood transfusion in (option C) is incorrect because Blood transfusion may be required in certain cases of sepsis if there is evidence of significant anemia or active bleeding. However, based on the information provided, there is no immediate indication of a blood transfusion.
D. NPO status in (option D) is incorrect because NPO status (nothing by mouth) is a general precautionary measure used in various situations, such as prior to surgery or to manage gastrointestinal complications. It is not a specific intervention in the sepsis resuscitation bundle.
Therefore, the nurse should initiate the intervention of administering broad-spectrum antibiotics in this scenario.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
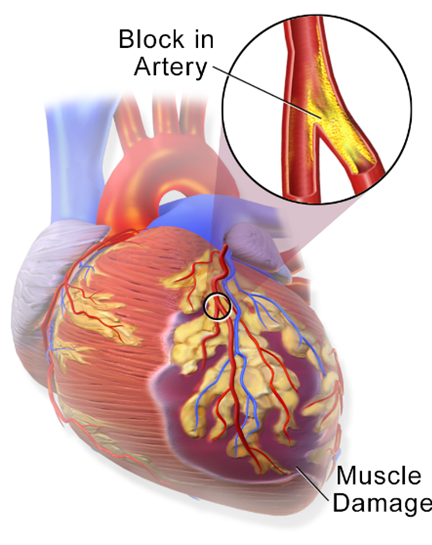
The characteristics described in the monitor strip analysis suggest ventricular tachycardia. The absence of a visible P wave and the wide and distorted QRS complex indicates that the electrical impulse is originating in the ventricles rather than the atria. The ventricular rate of 196 and regular R-R intervals further support the diagnosis of ventricular tachycardia.
B. Atrial fibrillation in (option B) is incorrect because it is characterized by irregularly irregular R-R intervals and the absence of discernible P waves. The QRS complex is typically narrow
C. Atrial tachycardia in (option C) is incorrect because it would have a rapid atrial rate with regular R-R intervals, and P waves may or may not be discernible. The QRS complex is typically narrow.
D. Ventricular fibrillation in (option D) is incorrect because it would present as a chaotic, rapid, and irregular electrical activity with no discernible P waves, QRS complexes, or regular R-R intervals. It is a life-threatening emergency that requires immediate defibrillation.
Therefore, based on the provided information, the nurse would interpret the patient's cardiac rhythm as ventricular tachycardia. However, it is important to note that an accurate interpretation should be made by a qualified healthcare professional, and the patient's clinical context should also be considered.
Correct Answer is B
Explanation
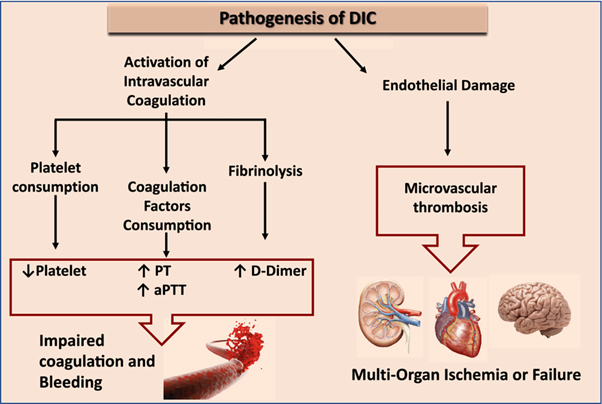
Disseminated Intravascular Coagulation (DIC) is a condition characterized by widespread activation of the coagulation system, leading to both excessive clot formation and consumption of clotting factors and platelets. This process can result in both bleeding and thrombosis.
The manifestations mentioned in option B are commonly seen in DIC:
Decreased platelet counts: DIC leads to platelet consumption and destruction, resulting in low platelet counts (thrombocytopenia).
Increased D-dimer: D-dimer is a fibrin degradation product, and its levels are increased DIC due to the breakdown of fibrin clots.
Increased prothrombin time (PT): DIC can lead to the depletion of clotting factors, resulting in prolonged prothrombin time, indicating impaired coagulation.
The other options mentioned do not represent the typical clinical manifestations of DIC:
A. Decreased hematocrit, increased platelet counts, and increased D-dimer in (option A) are incorrect because While platelet counts and D-dimer are increased in DIC, decreased hematocrit is not a characteristic finding.
C. Decreased Antithrombin III, increased platelet counts, and increased fibrinogen in (option C) is incorrect because: Decreased Antithrombin III can be seen in DIC, but increased platelet counts and fibrinogen levels are not specific to DIC.
D. Decreased D-dimer, increased platelet counts, and increased hemoglobin in (option D) is incorrect because Decreased D-dimer and increased hemoglobin are not typical findings in DIC, while increased platelet counts can be seen in some cases.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
