The nurse is caring for a patient receiving a continuous norepinephrine (Levophed) IV infusion. Which patient assessment information indicates that the infusion rate may be too high?
Mean arterial pressure is 55 mm Hg.
Systemic vascular resistance (SVR) is elevated.
Pulmonary artery wedge pressure (PAWP) is low.
Heart rate is 58 beats/min.
The Correct Answer is D
Norepinephrine is a potent vasoconstrictor and inotropic agent commonly used to increase blood pressure in cases of hypotension or shock. However, if the infusion rate is too high, it can lead to excessive vasoconstriction and potentially compromise organ perfusion.
A heart rate of 58 beats/min suggests bradycardia, which can be an indication of excessive vasoconstriction caused by a high dose or rate of norepinephrine infusion. Excessive vasoconstriction can reduce cardiac output and worsen tissue perfusion.
A. Mean arterial pressure is 55 mm Hg in (option A) is incorrect because A mean arterial pressure of 55 mm Hg may be within an acceptable range for a patient receiving norepinephrine infusion, depending on the patient's baseline blood pressure and clinical condition.
B. Systemic vascular resistance (SVR) is elevated in (option B) is incorrect because An elevated SVR indicates increased peripheral vascular resistance and can be a desired effect of norepinephrine infusion to improve blood pressure and perfusion.
C. Pulmonary artery wedge pressure (PAWP) is low in (option C) which is incorrect because A low PAWP may indicate decreased left ventricular preload, which can be a desired effect of norepinephrine infusion to reduce fluid overload in certain clinical conditions.
It is important for the nurse to carefully monitor the patient's hemodynamic parameters, including blood pressure, heart rate, and organ perfusion when titrating norepinephrine infusion to ensure optimal dosing and minimize potential adverse effects. If concerns arise regarding the infusion rate, the healthcare provider should be promptly notified for further evaluation and adjustment of the treatment plan.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Assessing the patient's level of consciousness is a critical initial step in evaluating a patient with shock. Altered mental status or decreased level of consciousness can be indicative of inadequate cerebral perfusion and may require immediate interventions to address compromised brain function and ensure patient safety.
While all the options mentioned are important in the assessment and management of a patient in shock, checking the level of consciousness takes priority as it provides essential information about the patient's neurological status and helps guide further interventions.
A. Obtaining the blood pressure in (option A) is incorrect because Assessing blood pressure is crucial in evaluating a patient in shock, but it can be done in conjunction with checking the level of consciousness and other vital signs.
C. Administering oxygen in (option C) is incorrect because: Administering oxygen is important in managing shock, as tissue hypoxia is a key concern. However, it can be done simultaneously with assessing the level of consciousness and initiating other interventions.
D. Obtaining a 12-lead electrocardiogram (ECG) in (option D) is incorrect because While an ECG may provide valuable information about the patient's cardiac function, it is not the first priority in a patient with shock of unknown etiology. Assessing the level of consciousness and vital signs takes precedence.
Correct Answer is C
Explanation
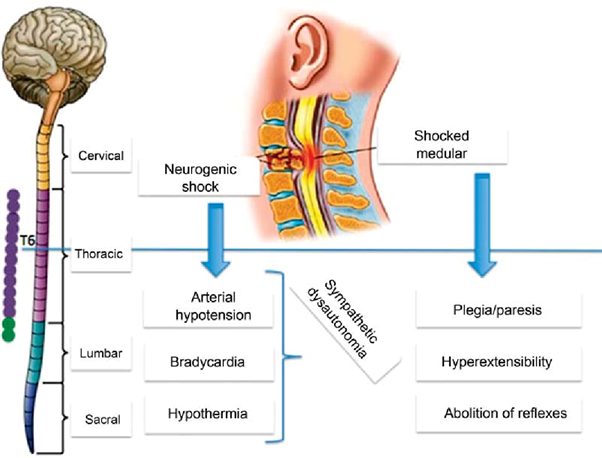
Neurogenic shock is a type of distributive shock that occurs due to the loss of sympathetic nervous system tone after a spinal cord injury or other traumatic brain injuries. This loss of sympathetic tone leads to vasodilation and decreased systemic vascular resistance, resulting in inadequate perfusion to vital organs.
One of the hallmark signs of neurogenic shock is bradycardia (a heart rate less than 60 beats/min) due to the unopposed parasympathetic activity. The parasympathetic system becomes dominant when sympathetic activity is impaired. Therefore, a heart rate of 48 beats/min in this patient suggests the possibility of neurogenic shock.
A. Cool, clammy skin in (option A) is incorrect because Cool, clammy skin is a characteristic of hypovolemic shock, where reduced blood volume leads to vasoconstriction to redirect blood flow to vital organs.
B. BP of 82/40 mm Hg in (option B) is incorrect because: Hypotension is a common finding in both neurogenic shock and hypovolemic shock. A low blood pressure reading alone does not specifically indicate neurogenic shock.
D. Shortness of breath in (option D) is incorrect because Shortness of breath is not specific to neurogenic shock but can occur in various types of shock, including hypovolemic shock. It may result from inadequate oxygenation or impaired respiratory function due to the underlying condition or associated injuries.
Therefore, the heart rate of 48 beats/min suggests the possibility of neurogenic shock in addition to hypovolemic shock in this patient.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
