A 37-year-old patient visits her OBGYN office for a routine check-up. She mentions that she and her partner are trying to conceive.
Which statement indicates that the patient understands infertility?
We should consider fertility treatments if we don’t conceive within a few months.
I know men can’t have fertility issues, so I’m not worried about my partner.
I’m concerned we might struggle to conceive because of my age.
Since my younger sister had infertility issues, I will too.
The Correct Answer is C
Choice A rationale:
This statement suggests that the patient has some awareness of infertility treatments, but it does not necessarily indicate a full understanding of infertility itself.
It's important to consider that a few months of trying to conceive may not be indicative of infertility, as it can take up to a year for healthy couples to achieve pregnancy.
Jumping to fertility treatments without a proper evaluation could lead to unnecessary interventions and potential financial and emotional burdens.
Choice B rationale:
This statement is incorrect. Male factor infertility is a common cause of difficulty conceiving, accounting for about 40% of infertility cases.
It's essential to evaluate both partners when assessing fertility issues.
Choice C rationale:
This statement demonstrates the patient's understanding of the relationship between age and fertility.
Female fertility gradually declines with age, especially after the age of 35, due to a decrease in the number and quality of eggs.
This awareness indicates that the patient is realistic about her chances of conceiving and is prepared to seek appropriate help if needed.
Choice D rationale:
While family history can play a role in infertility, it's not a guarantee that someone will experience the same issues as their relatives.
Each case is unique, and multiple factors can contribute to infertility, including genetics, lifestyle, medical conditions, and environmental factors.
It's important to undergo a thorough evaluation to determine the specific causes of infertility in each individual.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A rationale:
Trisomy 21, also known as Down syndrome, is a genetic condition caused by the presence of an extra copy of chromosome 21.
The nuchal translucency test (NT) is a non-invasive ultrasound screening test that measures the thickness of the fluid-filled space at the back of a developing baby's neck.
Evidence suggests that fetuses with Down syndrome tend to have increased fluid accumulation in this area, resulting in a larger-than-average nuchal translucency measurement.
Therefore, an increased NT measurement can be a marker for an increased risk of Down syndrome.
It's important to emphasize that the NT test is a screening tool, not a diagnostic test.
This means it can only indicate an increased risk of Down syndrome; it cannot definitively diagnose the condition.
To confirm a diagnosis, further testing, such as chorionic villus sampling (CVS) or amniocentesis, is required.
Choice B rationale:
Neural tube defects (NTDs) are birth defects that affect the brain, spine, or spinal cord.
The most common NTDs are spina bifida and anencephaly.
The NT test is not a diagnostic test for NTDs, although it might detect some cases of open spina bifida.
However, it's not specifically designed for this purpose, and other tests, such as alpha-fetoprotein (AFP) screening or detailed ultrasound, are more reliable for diagnosing NTDs.
Choice C rationale:
The NT test is typically performed in the first trimester of pregnancy, between 11 and 14 weeks gestation.
It's not available in the second trimester because the nuchal translucency measurement becomes less reliable after this point in pregnancy.
Choice D rationale:
A nuchal translucency measurement of 3mm or less is generally considered normal.
Measurements greater than 3mm are associated with an increased risk of Down syndrome and other chromosomal abnormalities.
The higher the measurement, the greater the risk.
Correct Answer is A
Explanation
Choice A rationale:
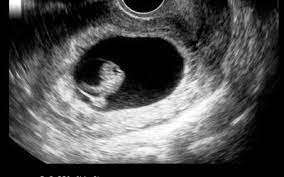
Fetal position during the first trimester is not definitively determined through ultrasound. While the gestational sac and fetal pole can be visualized, the fetus is still quite small and has ample space to move within the amniotic sac. This makes it challenging to accurately ascertain its position.
Reliable assessment of fetal position typically occurs later in pregnancy, usually between 34 and 36 weeks gestation. At this point, the fetus is larger and less mobile, allowing for a clearer assessment of its position through ultrasound.
The early determination of fetal position in the first trimester is not a primary goal of ultrasound. It is more focused on establishing pregnancy viability, gestational age, and detecting any potential abnormalities.
Choice B rationale:
Ultrasound in the first trimester can reliably detect multiple gestations. It can visualize the presence of multiple gestational sacs or fetal poles, clearly indicating whether a woman is carrying twins, triplets, or more.
Early identification of multiple gestations is crucial for optimal pregnancy management. It allows healthcare providers to tailor prenatal care, monitor for potential complications associated with multiple pregnancies, and plan for appropriate delivery. Choice C rationale:
Ultrasound in the first trimester can assist in detecting certain maternal abnormalities that could impact pregnancy. These may include:
Uterine abnormalities, such as fibroids or structural defects
Ovarian cysts
Ectopic pregnancies (where the embryo implants outside the uterus)
Gestational trophoblastic disease (abnormal growth of tissue inside the uterus)
Early identification of these maternal abnormalities allows for timely intervention and management, ensuring the best possible outcomes for both mother and fetus.
Choice D rationale:
Confirming pregnancy is a primary reason for ultrasound in the first trimester. It can visualize the gestational sac, which contains the developing embryo and confirms the presence of a pregnancy.
Ultrasound can also detect the fetal heartbeat, which typically becomes visible between 6 and 8 weeks gestation. This provides further confirmation of a viable pregnancy.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
