A 45-year-old female patient presents with symptoms of weight loss, palpitations, and heat intolerance. Laboratory results reveal elevated T3 and T4 levels and suppressed TSH levels. Considering her clinical presentation and lab results, which of the following treatments is most appropriate for managing her hyperthyroidism?
Methimazole.
Levothyroxine.
Radioactive iodine.
Propranolol.
The Correct Answer is C
Choice A Reason:
Methimazole is an antithyroid medication that inhibits the synthesis of thyroid hormones. It is commonly used to manage hyperthyroidism, especially in patients who are not candidates for radioactive iodine therapy or surgery. Methimazole is effective in reducing thyroid hormone levels and controlling symptoms, but it requires long-term use and regular monitoring of thyroid function tests.
Choice B Reason:
Levothyroxine is a synthetic form of thyroxine (T4) used to treat hypothyroidism, not hyperthyroidism. Administering levothyroxine to a patient with hyperthyroidism would exacerbate the condition by increasing thyroid hormone levels. Therefore, it is not an appropriate treatment for managing hyperthyroidism.
Choice C Reason:
Radioactive iodine is a widely used treatment for hyperthyroidism. It works by destroying overactive thyroid cells, thereby reducing the production of thyroid hormones. This treatment is particularly effective for patients with Graves’ disease, toxic multinodular goiter, or toxic adenoma. Radioactive iodine is a definitive treatment that can lead to a permanent resolution of hyperthyroidism, although it may result in hypothyroidism, which can be managed with levothyroxine.
Choice D Reason:
Propranolol is a beta-blocker that helps manage the symptoms of hyperthyroidism, such as palpitations, tremors, and anxiety. While it is useful for symptomatic relief, it does not address the underlying cause of hyperthyroidism. Propranolol is often used in conjunction with other treatments, such as antithyroid medications or radioactive iodine, to provide immediate symptom control.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A Reason:
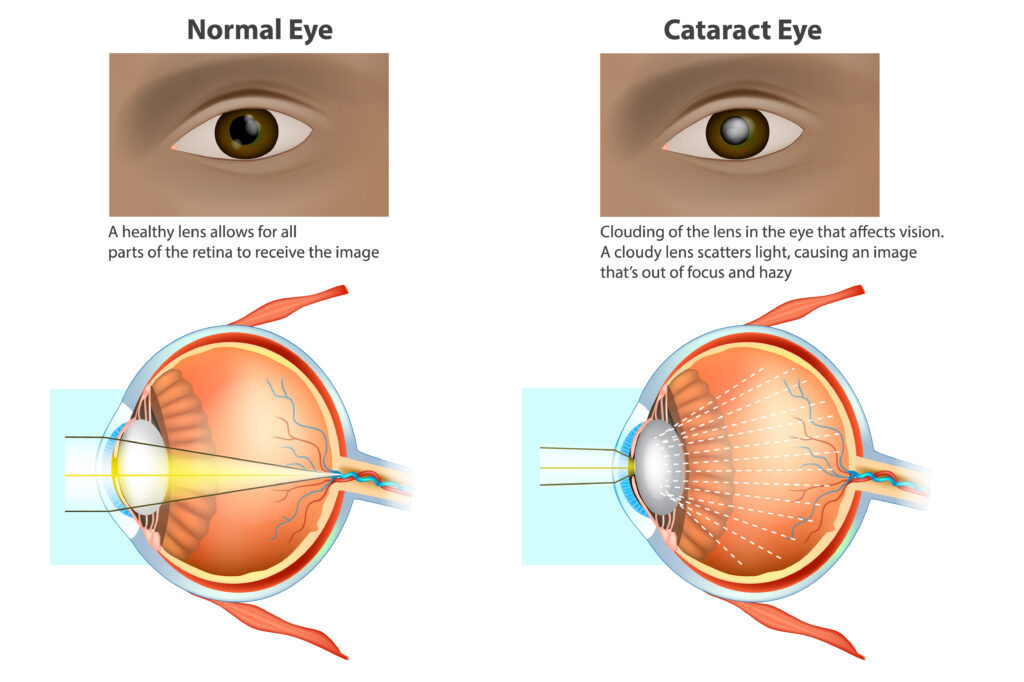
Cloudiness in the lens of the eyes is the hallmark symptom of cataracts. Cataracts cause the lens to become opaque, leading to blurred vision and difficulty seeing clearly. This cloudiness can make it challenging to perform everyday tasks and is the most indicative sign of cataracts.
Choice B Reason:
Double vision in one eye can occur with cataracts, but it is not the most indicative symptom. While cataracts can cause visual disturbances, the primary symptom is the cloudiness of the lens, which directly impacts vision clarity.
Choice C Reason:
Eye pain and redness are not typical symptoms of cataracts. These symptoms are more commonly associated with other eye conditions such as infections or glaucoma. Cataracts primarily cause visual disturbances without significant pain or redness.
Choice D Reason:
Sudden loss of vision is not characteristic of cataracts. Cataracts develop gradually over time, leading to a slow progression of vision impairment. Sudden vision loss is more likely to be associated with acute conditions such as retinal detachment or vascular occlusions.
Correct Answer is D
Explanation
Choice A Reason:
Diabetes Insipidus (DI) is characterized by excessive urination and thirst due to a deficiency of antidiuretic hormone (ADH) or a renal insensitivity to ADH. Patients with DI typically present with hypernatremia (high serum sodium) and low urine osmolality, which contrasts with the findings of low serum sodium and high urine osmolality in this patient.
Choice B Reason:
Adrenal insufficiency can cause hyponatremia and hyperkalemia due to a deficiency in aldosterone and cortisol. However, it usually presents with low serum osmolality and low urine sodium, which does not align with the patient’s laboratory results of high urine osmolality and elevated urine sodium.
Choice C Reason:
Hyperaldosteronism leads to increased sodium reabsorption and potassium excretion, resulting in hypernatremia and hypokalemia. This condition does not match the patient’s findings of hyponatremia and high urine osmolality.
Choice D Reason:
Syndrome of inappropriate Antidiuretic Hormone (SIADH) is characterized by excessive release of ADH, leading to water retention, hyponatremia, and concentrated urine. The patient’s laboratory results of low serum sodium, low serum osmolality, high urine osmolality, and elevated urine sodium are consistent with SIADH. This condition causes the kidneys to reabsorb water, diluting the blood and concentrating the urine.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
