A laboring client is inhaling gas through a mouthpiece just before the onset of her regular contractions.
As they inhale, a valve opens and gas is released.
They continue to inhale the gas slowly and deeply until the contraction starts to subside.
When the inhalation stops, the valve closes.
What is this procedure?
“Likely to be used in the second stage of labor but not in the first stage.”
“A prelude to cesarean birth.”
“Not used much anymore.”
“An application of nitrous Oxide.”
The Correct Answer is D
A rationale:
Incorrect. Nitrous oxide can be used during any stage of labor, not just the second stage. It is often used during the first stage to help manage early labor pain.
Evidence: Studies have shown that nitrous oxide is effective for pain relief during both the first and second stages of labor.
Additional information: The timing of nitrous oxide administration is typically based on the individual's preferences and needs. Some people prefer to use it as soon as labor begins, while others wait until contractions become more intense.
Choice B rationale:
Incorrect. Nitrous oxide is not a prelude to cesarean birth. It is a method of pain relief that can be used during vaginal or cesarean birth.
Evidence: Cesarean birth is a major surgical procedure that is typically performed under regional or general anesthesia. Nitrous oxide is not a type of anesthesia that would be used for this purpose.
Additional information: Cesarean birth is usually only performed when there is a medical reason why a vaginal birth is not possible or safe.
Choice C rationale:
Incorrect. Nitrous oxide is still a commonly used method of pain relief during labor. It is safe and effective, and it has a good safety profile.
Evidence: Nitrous oxide is one of the most widely used methods of pain relief during labor in many countries around the world.
Additional information: The use of nitrous oxide during labor has been increasing in recent years, as more people have become aware of its benefits.
Choice D rationale:
Correct. The procedure described in the question is an application of nitrous oxide. Nitrous oxide is a colorless, odorless gas that has analgesic and anxiolytic properties. It is often used during labor to help manage pain and anxiety.
Evidence: Nitrous oxide is a well-established method of pain relief during labor. It has been used for this purpose for over a century.
Additional information: Nitrous oxide is a safe and effective option for pain relief during labor. It is easy to administer and has few side effects.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A rationale:
A positive contraction stress test (CST) indicates that the fetal heart rate decelerates late in response to uterine contractions, suggesting potential uteroplacental insufficiency. However, the scenario does not describe a CST being performed, as it does not mention any assessment of uterine contractions or their relationship to fetal heart rate changes.
Choice C rationale:
A negative contraction stress test (CST) would demonstrate no late decelerations in response to contractions, suggesting adequate placental function. However, as mentioned earlier, a CST is not the test being performed in this scenario.
Choice D rationale:
A non-reactive nonstress test (NST) means that there were not enough fetal heart rate accelerations (at least 2, each lasting at least 15 seconds and peaking at least 15 beats above baseline) within a 20-minute period. This finding sometimes warrants further evaluation of fetal well-being. However, the scenario clearly states that 3 accelerations meeting the criteria for reactivity were observed.
Choice B rationale:
A reactive nonstress test (NST) is considered reassuring and indicates that the fetal heart rate is responding appropriately to fetal movement, suggesting that the fetus is likely healthy and well-oxygenated. The presence of 3 accelerations meeting the criteria for reactivity within a 20-minute period is the hallmark of a reactive NST.
Correct Answer is A
Explanation
Choice A rationale:
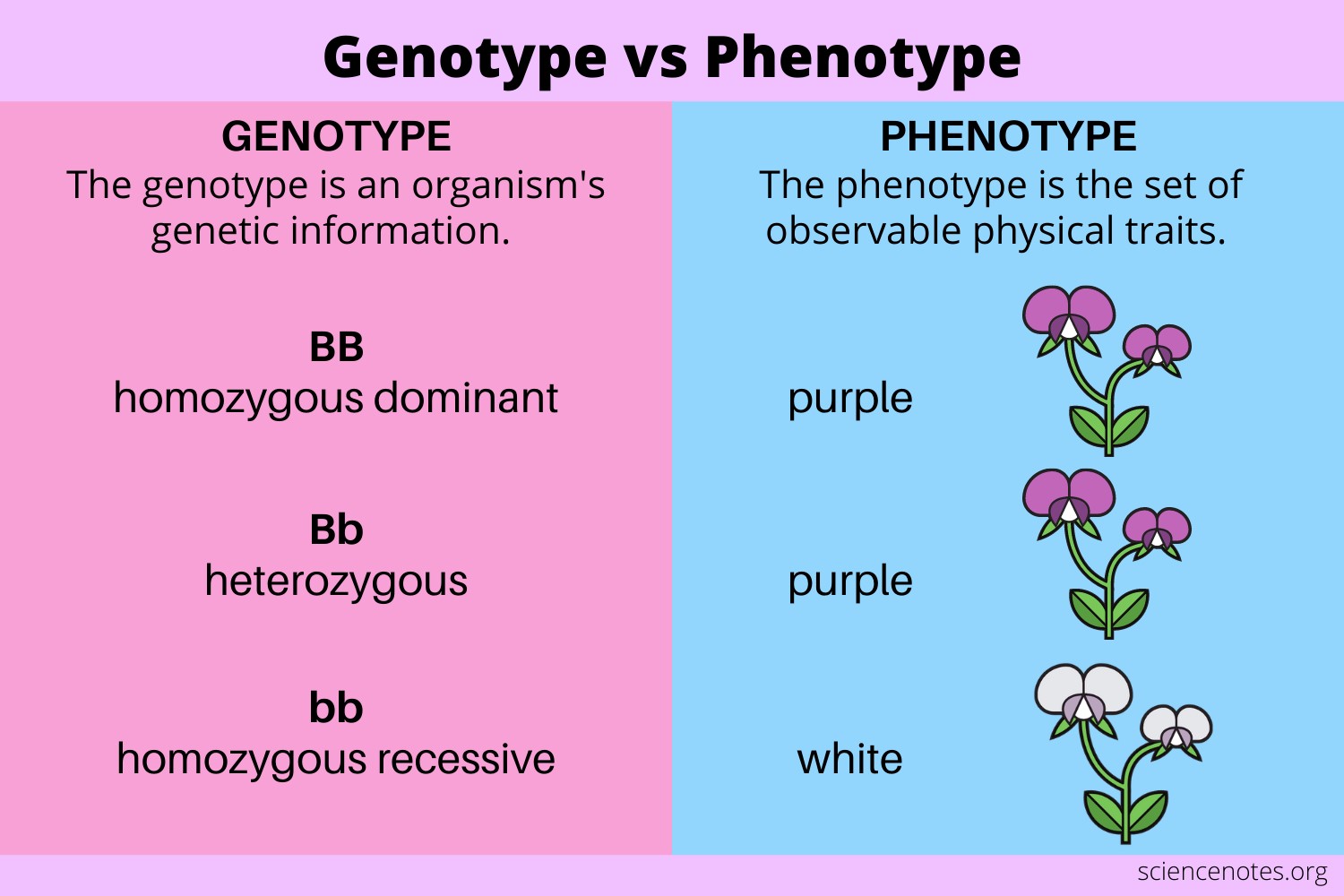
Genotype refers to the complete set of genetic instructions an individual inherits from their parents. It represents the actual genes present within an individual's cells, determining their traits and characteristics.
Genotype is the underlying genetic foundation that shapes an individual's phenotype, which is the observable expression of those genes.
Choice B rationale:
Chromotype is not a commonly used term in genetics. It may occasionally refer to the banding pattern observed on chromosomes during certain staining techniques, but it does not accurately represent an individual's complete genetic makeup.
Choice C rationale:
Phenotype refers to the observable physical or biochemical characteristics of an individual, such as eye color, height, blood type, or susceptibility to certain diseases. It is the result of the interaction between an individual's genotype and their environment.
While phenotype is influenced by genotype, it does not directly represent the underlying genetic code itself.
Choice D rationale:
Karyotype is a visual representation of an individual's chromosomes, arranged in pairs according to size and shape. It is often used to diagnose chromosomal abnormalities or genetic disorders, but it does not provide the full details of an individual's genetic makeup at the gene level.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
