A nurse collects the health history of a 65-year-old client. Which of the following risk factors in the client's history puts the client at the highest risk for embolic stroke?
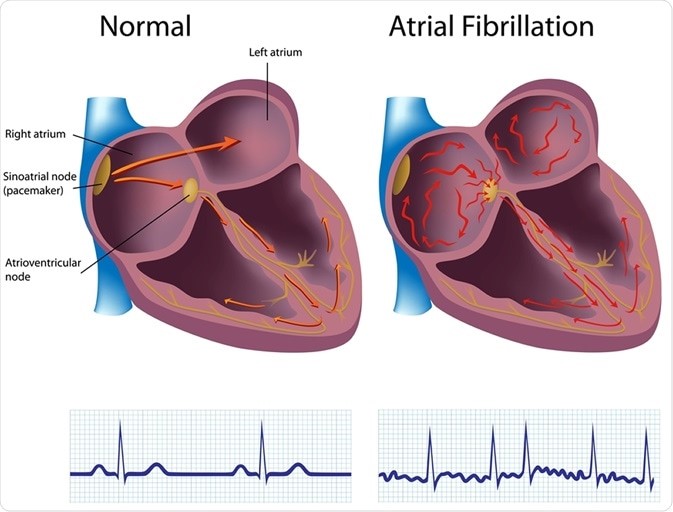
Atrial fibrillation.
Hypertension.
Diabetes.
Alcohol abuse.
The Correct Answer is A
Choice A reason: This is the correct answer because atrial fibrillation is the risk factor that puts the client at
the highest risk for embolic stroke. Atrial fibrillation is an irregular and rapid heart rate that causes poor blood flow and blood pooling in the heart chambers. This can lead to the formation of blood clots that can travel to the brain and block an artery, causing an embolic stroke.
Choice B reason: This is incorrect because hypertension is not the risk factor that puts the client at
the highest risk for embolic stroke. Hypertension is high blood pressure that puts stress on the blood vessels and increases the risk of bleeding or rupture. This can lead to a hemorrhagic stroke, but not an embolic stroke.
Choice C reason: This is incorrect because diabetes is not the risk factor that puts the client at
the highest risk for embolic stroke. Diabetes is a condition that causes high blood sugar levels and damages the blood vessels and nerves. This can lead to poor circulation and increased risk of infection and ulcers, but not an embolic stroke.
Choice D reason: This is incorrect because alcohol abuse is not the risk factor that puts the client at
the highest risk for embolic stroke. Alcohol abuse is excessive consumption of alcohol that affects liver function and blood clotting factors. This can lead to liver disease and bleeding disorders, but not an embolic stroke.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A reason: This is the correct answer because airway obstruction is the risk that is the priority for assessment and intervention for a client who has extensive partial and full-thickness burns of
the head, neck, and chest. Airway obstruction can occur due to edema, inflammation, or inhalation injury of
the upper airway structures. It can compromise oxygenation and ventilation, and lead to respiratory failure or cardiac arrest. The nurse should assess for signs of airway obstruction, such as stridor, hoarseness, dyspnea, or cyanosis, and provide oxygen therapy, humidification, or intubation as needed.
Choice B reason: This is incorrect because fluid imbalance is not the risk that is the priority for assessment and intervention for a client who has extensive partial and full-thickness burns of
the head, neck, and chest. Fluid imbalance can occur due to fluid loss from damaged skin and capillaries, as well as increased capillary permeability and fluid shifts. It can cause dehydration, hypovolemia, shock, or electrolyte imbalances. The nurse should monitor fluid status, vital signs, urine output, and laboratory values, and provide fluid resuscitation as prescribed, but only after ensuring airway patency.
Choice C reason: This is incorrect because paralytic ileus is not the risk that is the priority for assessment and intervention for a client who has extensive partial and full-thickness burns of
the head, neck, and chest. Paralytic ileus is a condition where there is decreased or absent bowel motility due to nerve damage or decreased blood flow to
the gastrointestinal tract. It can cause abdominal distension, nausea, vomiting, or constipation. The nurse should assess bowel sounds, abdominal girth, and stool characteristics, and provide nasogastric suction or laxatives as prescribed, but only after ensuring airway patency and fluid balance.
Choice D reason: This is incorrect because infection is not the risk that is the priority for assessment and intervention for a client who has extensive partial and full-thickness burns of
the head, neck, and chest. Infection can occur due to loss of skin barrier, exposure to microorganisms, or impaired immune system. It can cause fever, increased pain, purulent drainage, or sepsis. The nurse should assess for signs of infection, obtain wound cultures, and administer antibiotics as prescribed, but only after ensuring airway patency, fluid balance, and pain control.
Correct Answer is ["B","E","F"]
Explanation
Choice A Reason: Edema is not a specific finding of a systemic infection, but rather a possible sign of fluid overload or impaired venous return. It can occur due to excessive infusion rate, heart failure, or obstruction of blood flow in or around the central line.
Choice B Reason: This is a correct choice. Purulent drainage at intravenous insertion site is a finding of a local infection that can spread systemically. It indicates bacterial invasion and inflammation of the skin and subcutaneous tissue around the catheter.
Choice C Reason: Redness at insertion site is a finding of a local infection that can spread systemically. It indicates increased blood flow and inflammation of the skin and subcutaneous tissue around the catheter.
Choice D Reason: Nausea is not a specific finding of a systemic infection, but rather a possible side effect of parenteral nutrition or a symptom of another condition. It can occur due to electrolyte imbalance, hyperglycemia, or gastrointestinal disorders.
Choice E Reason: This is a correct choice. Leukocytosis is a finding of a systemic infection that indicates increased production and release of white blood cells in response to infection. It can be detected by a blood test.
Choice F Reason: This is a correct choice. Fever is a finding of a systemic infection that indicates increased body temperature due to activation of the immune system and release of pyrogens. It can be measured by a thermometer.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
