A nurse is caring for a client who is 1 day postpartum and breastfeeding her newborn. The client reports sore nipples. Which of the following actions should the nurse take?
Instruct the client to wait 4 hours between daytime feedings.
Offer supplemental formula between the newborn's feedings.
Have the client limit the length of breastfeeding to 5 minutes per breast.
Assess the newborn's latch while breastfeeding.
Assess the newborn's latch while breastfeeding.
The Correct Answer is D
Sore nipples are a common problem for breastfeeding mothers, especially in the first few days or weeks after delivery. They can cause pain, discomfort, and frustration, and may interfere with breastfeeding success and satisfaction. The most common cause of sore nipples is poor latch, which means that the newborn does not attach to the breast correctly and does not suckle effectively. Poor latch can result from various factors, such as improper positioning, tongue-tie, inverted or flat nipples, engorgement, or thrush.
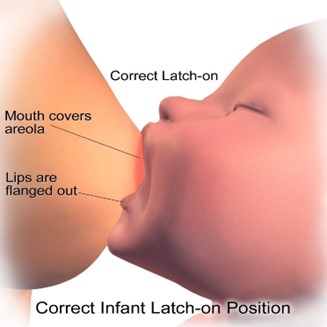
The nurse should assess the newborn's latch while breastfeeding to identify and correct any problems that may cause sore nipples. The nurse should observe the following signs of a good latch:
- The newborn's mouth is wide open and covers most of the areola (the dark area around the nipple).
- The newborn's chin and nose touch the breast, and the cheeks are rounded and not dimpled.
- The newborn's tongue is visible under the lower lip and curls around the breast.
- The newborn's lips are flanged outwards and not tucked inwards.
- The newborn's jaw moves rhythmically and smoothly, and swallowing sounds are audible.
- The mother feels a gentle tugging sensation on the nipple, but no pain or pinching.
The nurse should also teach the mother how to achieve a good latch by using different positions, supporting the breast with her hand, tickling the newborn's lower lip with her nipple, and bringing the newborn to the breast when their mouth is wide open. The nurse should also encourage the mother to seek help from a lactation consultant or a peer support group if she has persistent or severe nipple pain.
a) Instructing the client to wait 4 hours between daytime feedings is not an appropriate action for the nurse to take. This may reduce nipple soreness temporarily, but it can also cause breast engorgement, milk supply reduction, mastitis, or poor weight gain in the newborn. The nurse should advise the client to feed the newborn on demand, usually every 1.5 to 3 hours during the day and every 3 to 4 hours at night.
b) Offering supplemental formula between the newborn's feedings is not an appropriate action for the nurse to take. This may interfere with breastfeeding initiation and establishment, as it can reduce the mother's milk supply, confuse the newborn's sucking pattern, increase the risk of nipple preference or rejection, and expose the newborn to potential allergens or infections. The nurse should support exclusive breastfeeding for the first six months of life, unless there is a medical indication for supplementation.
c) Having the client limit the length of breastfeeding to 5 minutes per breast is not an appropriate action for the nurse to take. This may not be enough time for the newborn to get enough milk, especially the hindmilk that is richer in fat and calories. It may also prevent proper drainage of the breast and lead to engorgement or mastitis. The nurse should advise the client to let the newborn feed until they are satisfied and release the breast on their own, which may take 10 to 20 minutes per breast on average.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
In a newborn, bluish discoloration of the hands and feet may indicate a condition called peripheral cyanosis, which suggests poor oxygenation. It is important to report this finding to the healthcare provider promptly, as it may indicate a respiratory or circulatory problem that requires immediate attention.
Option a) Overlapping of the cranial bones is a common finding in newborns due to the molding of the head during delivery. This is not a priority finding to report unless there are other signs of concern, such as abnormal head shape or signs of trauma.
Option b) Small, distended white sebaceous glands on the face are called milia and are a normal finding in newborns. They are not a priority finding to report and typically resolve on their own within a few weeks.
Option c) Forward and lateral positioning of the ears is a normal finding in a newborn and is not a priority to report. The ears may appear folded or positioned differently due to the pressure and positioning in the womb.
Correct Answer is A, B, D, C
Explanation
- Compressing the bulb syringe before placing it in the newborn's mouth or nose creates a vacuum that allows the suctioning of the mucus¹².
- Placing the bulb syringe in the newborn's mouth first helps clear the oral airway and prevent aspiration of mucus into the lungs¹². The nozzle of the bulb syringe should be gently inserted into the corner of the mouth, not the center, to avoid stimulating the gag reflex¹².
- Using the bulb syringe to suction the newborns nose helps clear the nasal airway and improve breathing¹². The nozzle of the bulb syringe should be gently inserted into one nostril at a time, and not too far, to avoid injuring the nasal mucosa¹².
- Assessing the newborn for reflex bradycardia helps monitor for any adverse effects of suctioning, such as a decrease in heart rate due to vagal stimulation¹³. Reflex bradycardia can cause hypoxia and acidosis in newborns, and may require oxygen administration or resuscitation³. The normal heart rate for a newborn is 120 to 160 beats per minute³.

Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
