A nurse is conducting a class on how to self-manage insulin regimens. A client asks how long a vial of insulin can be stored at room temperature before it "goes bad." What would be the nurse's best answer?
"If a vial of insulin will be used up within 21 days, it may be kept at room temperature."
"If a vial of insulin will be used up within 2 weeks, it may be kept at room temperature."
"If you are going to use up the vial within 1 month, it can be kept at room temperature."
"If a vial of insulin will be used up within 1 week, it may be kept at room temperature."
The Correct Answer is A
A. "If a vial of insulin will be used up within 21 days, it may be kept at room temperature."
This statement suggests a duration of up to 21 days for room temperature storage after the vial is in use. However, most insulins can typically be stored at room temperature for up to 28 days after initial use. This recommendation might be more conservative than necessary for many types of insulin.
B. "If a vial of insulin will be used up within 2 weeks, it may be kept at room temperature."
This choice suggests a timeframe of 14 days for room temperature storage after opening the vial. However, for many insulins, the recommended duration for room temperature storage after opening is up to 28 days.
C. "If you are going to use up the vial within 1 month, it can be kept at room temperature."
This option extends the timeframe to 1 month for room temperature storage after the vial is in use. However, the generally recommended duration for many insulins is up to 28 days after opening.
D. "If a vial of insulin will be used up within 1 week, it may be kept at room temperature."
This choice suggests a very short duration of 7 days for room temperature storage after opening the vial. Most insulins can typically be stored at room temperature for a longer duration after initial use.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["B","C","E"]
Explanation
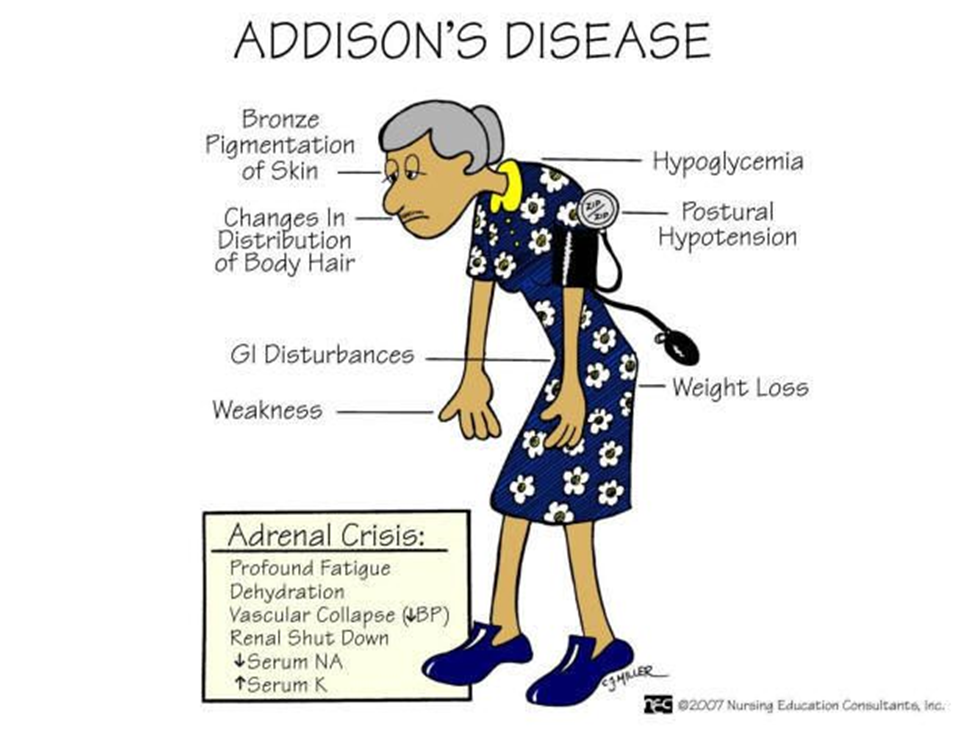
A. Buffalo hump:
Explanation: A buffalo hump is associated with excess cortisol, which is not a typical manifestation of Addison's disease. Instead, patients with Addison's disease may experience weight loss and muscle wasting.
B. Hyponatremia:
Explanation: Correct. Hyponatremia (low sodium levels) can occur in Addison's disease due to the loss of aldosterone, which plays a role in sodium and water balance.
C. Decreased glucose level:
Explanation: Correct. Addison's disease can lead to hypoglycemia (low blood glucose levels) because cortisol, which is important for maintaining blood glucose, is deficient.
D. Weight gain:
Explanation: Weight gain is not a typical manifestation of Addison's disease. Instead, weight loss and muscle wasting may occur.
E. Craving for salt:
Explanation: Correct. Addison's disease can lead to salt craving, as aldosterone deficiency results in increased sodium loss and potassium retention.
Correct Answer is D
Explanation
A. "When I went to the restroom the last few days, my urine smelled odd."
Changes in the smell of urine can be associated with various conditions, including diabetes. However, it's not a specific symptom.
B. "I've always been a fan of sweet foods, but lately I'm turned off by them."
A change in taste preferences may not be directly related to diabetes. It's not a typical symptom.
C. "No matter how much sleep I get, it seems to take me hours to wake up."
Fatigue and difficulty waking up are general symptoms that can be caused by various factors, including diabetes. However, it's not specific to diabetes alone.
D. "Lately, I drink a lot, but I can't seem to quench my thirst."
Excessive thirst (polydipsia) and increased urination (polyuria) are classic symptoms of diabetes, suggesting elevated blood sugar levels.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
