A nurse is performing a vaginal exam on a client who is in active labor. The nurse notes the umbilical cord protruding through the cervix. Which of the following actions should the nurse take?
Administer oxytocin to the client via intravenous infusion.
Apply oxygen at 2 L/min via nasal cannula.
Prepare for insertion of an intrauterine pressure catheter.
Assist the client into the knee-chest position.
The Correct Answer is D
Choice A rationale:
Administering oxytocin to the client via intravenous infusion is not appropriate when the nurse notes an umbilical cord protruding through the cervix. The priority is to relieve pressure on the cord to prevent fetal compromise, and administering oxytocin could worsen the situation.
Choice B rationale:
Applying oxygen at 2 L/min via nasal cannula is not the priority when an umbilical cord prolapse is detected. The focus should be on relieving pressure on the cord and changing the client's position to alleviate the compression.
Choice C rationale:
Preparing for insertion of an intrauterine pressure catheter is not appropriate when there is an umbilical cord prolapse. The immediate concern is the potential compromise of fetal blood flow, and addressing the cord prolapse takes precedence over any other interventions.
Choice D rationale:
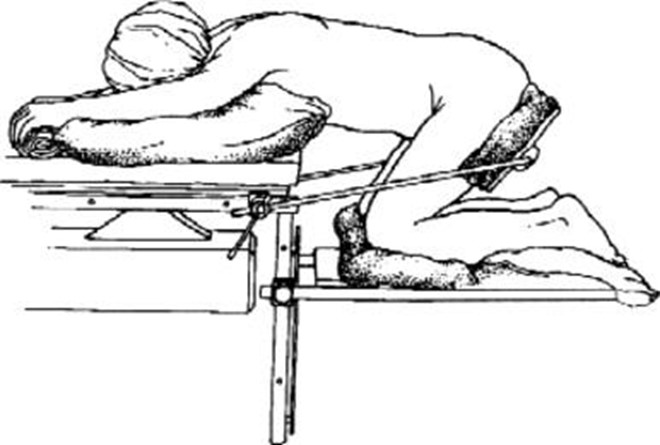
Assisting the client into the knee-chest position is the correct action when an umbilical cord prolapse is observed during a vaginal exam. This position helps to alleviate pressure on the cord by moving the presenting part of the fetus off the cord and can prevent further fetal distress until more definitive interventions can be performed.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
Choice A rationale:
The priority nursing action when the fetal heart rate shows a deceleration after the contraction has started, with the lowest point occurring after the peak of the contraction, is to change the client's position. This deceleration pattern is called "late decelerations,” and it is typically associated with uteroplacental insufficiency, which can be caused by maternal hypotension or impaired blood flow to the placenta. Changing the client's position, such as moving the client to their side or repositioning them, can alleviate pressure on the vena cava and improve blood flow to the placenta, thus potentially resolving or minimizing the late decelerations.
Choice B rationale:
Inserting a scalp electrode (Choice B) is not the priority action in this situation. While a scalp electrode may be used to monitor the fetal heart rate more accurately and continuously, it is not the initial intervention for addressing late decelerations.
Choice C rationale:
Preparing for amnioinfusion (Choice C) may be considered if there are variable decelerations (caused by cord compression) present, but it is not the priority intervention for late decelerations.
Choice D rationale:
Documenting benign decelerations (Choice D) is not appropriate in this scenario since late decelerations are not considered benign and require immediate action.
Correct Answer is A
Explanation
Choice A rationale:
Rh incompatibility occurs when an Rh-negative client is exposed to Rh-positive fetal blood, typically during a prior pregnancy or delivery. The client’s immune system produces anti-Rh antibodies that cross the placenta in subsequent pregnancies, attacking the Rh-positive red blood cells of the fetus. This hemolysis releases bilirubin, leading to hyperbilirubinemia in the newborn.
Choice B rationale:
Rh incompatibility only occurs when the client is Rh-negative and the fetus is Rh-positive. An Rh-positive client will not form antibodies against an Rh-negative fetus, as their immune system recognizes the Rh factor as normal.
Choice C rationale:
This choice is not related to the mechanism of Rh incompatibility. Receiving a transfusion with Rh-negative blood would not cause the mother's immune system to produce anti-Rh antibodies or lead to Rh incompatibility with her newborn.
Choice D rationale:
This choice describes the ABO blood group system, not the Rh factor. ABO incompatibility can occur when a mother with blood type O (producing anti-A and anti-B antibodies) has a newborn with blood type A, B, or AB, leading to hemolysis of the fetal red blood cells. However, the question specifically mentions Rh incompatibility, which involves the Rh factor, not the ABO system.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
