A client with benign prostatic hyperplasia receives a new prescription of tamsulosin. Which intervention should the nurse perform to monitor for an adverse reaction?
Perform a bladder scan.
Monitor blood pressure.
Obtain daily weights.
Assess urine output.
The Correct Answer is B
Choice A reason:
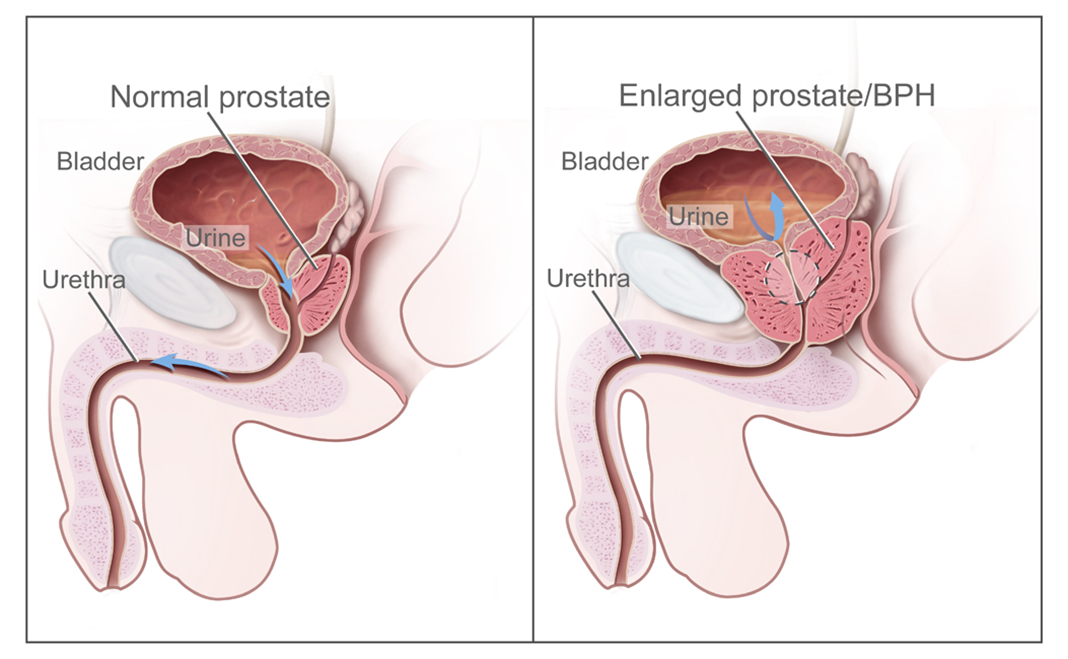
Performing a bladder scan is useful for assessing urinary retention, which can be a symptom of benign prostatic hyperplasia (BPH). However, it is not the primary method for monitoring adverse reactions to tamsulosin. Tamsulosin is an alpha-1 blocker that relaxes the muscles in the prostate and bladder neck, improving urine flow. While it can help reduce urinary retention, the primary concern with tamsulosin is its effect on blood pressure.
Choice B reason:
Monitoring blood pressure is crucial because tamsulosin can cause orthostatic hypotension, a condition where blood pressure drops significantly when a person stands up from a sitting or lying position. This can lead to dizziness, lightheadedness, and even fainting. Regular monitoring of blood pressure helps detect and manage this potential adverse reaction, ensuring the client’s safety.
Choice C reason:
Obtaining daily weights is important for monitoring fluid balance and detecting conditions like heart failure or kidney disease. However, it is not directly related to the adverse reactions of tamsulosin. The primary concern with tamsulosin is its impact on blood pressure, not fluid retention.
Choice D reason:
Assessing urine output is important for evaluating the effectiveness of tamsulosin in relieving urinary symptoms associated with BPH. However, it is not the primary method for monitoring adverse reactions. The main adverse reaction to be aware of with tamsulosin is its potential to cause orthostatic hypotension, making blood pressure monitoring the priority.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is {"dropdown-group-1":"D","dropdown-group-2":"E","dropdown-group-3":"E"}
Explanation
The client is at immediate risk for developing Cardiac arrest, Anaphylaxis, and Arrhythmias.
Choice A: Peripheral Edema
Peripheral edema refers to the swelling of tissues, usually in the lower limbs, due to the accumulation of fluid. While peripheral edema can be a concern in patients with heart conditions, it is not an immediate risk in the context of the patient’s current situation. The primary concerns for this patient, given her history of symptomatic bradycardia and atrial fibrillation, are more acute and life-threatening conditions such as cardiac arrest, anaphylaxis, and arrhythmias. Peripheral edema is typically a chronic condition that develops over time and is not considered an emergent risk in this scenario.
Choice B: Renal Failure
Renal failure, or kidney failure, is a condition where the kidneys lose their ability to filter waste from the blood effectively. While renal failure can be a serious complication, it is not an immediate risk for this patient. The patient’s primary issues are related to her cardiovascular system, specifically her low heart rate and history of atrial fibrillation. The immediate risks in this scenario are more likely to be related to acute cardiovascular events rather than renal complications. Additionally, there is no indication in the patient’s history or current treatment that suggests an imminent risk of renal failure.
Choice C: Necrosis
Necrosis refers to the death of body tissue due to a lack of blood flow or infection. While necrosis can occur in severe cases of prolonged ischemia or infection, it is not an immediate risk for this patient. The patient’s current condition and treatment plan do not indicate a high risk of tissue necrosis. The more pressing concerns are related to her cardiovascular health, specifically the risk of cardiac arrest, anaphylaxis, and arrhythmias. These conditions are more likely to occur suddenly and require immediate medical intervention.
Choice D: Cardiac Arrest
Cardiac arrest is a sudden loss of heart function, leading to a cessation of blood flow to the body’s organs. Given the patient’s history of symptomatic bradycardia and atrial fibrillation, she is at a high risk of developing cardiac arrest. Bradycardia can lead to insufficient blood flow and oxygen delivery to vital organs, potentially resulting in cardiac arrest. Additionally, the stress of the upcoming procedure and the discontinuation of anticoagulants can further increase this risk. Therefore, cardiac arrest is a significant immediate risk for this patient and requires close monitoring and preparedness for emergency intervention.
Choice E: Anaphylaxis
Anaphylaxis is a severe, potentially life-threatening allergic reaction that can occur rapidly. The patient is receiving vancomycin, which is known to cause hypersensitivity reactions, including anaphylaxis, in some individuals. Symptoms of anaphylaxis include difficulty breathing, swelling, hives, and a drop in blood pressure. Given the patient’s current infusion of vancomycin, she is at risk for developing anaphylaxis, which requires immediate medical attention to prevent severe complications or death. The nurse must be vigilant for signs of anaphylaxis and be prepared to administer emergency treatment if necessary.
Choice F: Arrhythmias
Arrhythmias are irregular heartbeats that can range from benign to life-threatening. The patient has a history of atrial fibrillation, a type of arrhythmia, and symptomatic bradycardia, both of which put her at risk for developing further arrhythmias. The stress of the upcoming procedure, changes in medication, and the underlying heart conditions all contribute to the risk of arrhythmias. These irregular heartbeats can lead to decreased cardiac output, syncope, or even progression to more severe arrhythmias like ventricular fibrillation, which can be fatal. Therefore, arrhythmias are an immediate risk for this patient and require continuous cardiac monitoring and readiness to intervene.
Correct Answer is ["A","B","D","E"]
Explanation
Choice A: No known allergies
Reason: The absence of known allergies is crucial when administering any medication, including antibiotics like vancomycin. Allergic reactions to antibiotics can range from mild rashes to severe anaphylaxis, which can be life-threatening. In this case, the patient has reported no known allergies, which significantly reduces the risk of an adverse reaction to vancomycin. This makes it safer to proceed with the administration of the antibiotic. Ensuring that the patient has no known allergies is a standard precaution in medical practice to prevent potential allergic reactions.
Choice B: Dosage in safe range
Reason: The dosage of vancomycin must be within a safe range to avoid toxicity. Vancomycin is typically dosed based on the patient’s weight and renal function. For adults, the usual dose is 15-20 mg/kg, administered every 8-12 hours, depending on the severity of the infection and the patient’s renal function. In this scenario, the prescribed dose is 1 gram in 250 mL of 0.9% sodium chloride, which is within the safe range for an adult patient. Administering the correct dosage is essential to ensure the effectiveness of the antibiotic while minimizing the risk of nephrotoxicity and ototoxicity, which are potential side effects of vancomycin.
Choice C: Potassium 4.4 mEq/L (4.4 mmol/L)
Reason: While the potassium level of 4.4 mEq/L is within the normal range (3.5-5.0 mEq/L), it is not directly related to the safety of administering vancomycin. Potassium levels are more relevant to the overall electrolyte balance and cardiac function but do not specifically impact the administration of vancomycin. Therefore, this choice is not as pertinent to the safety of vancomycin administration as the other options.
Choice D: Peripheral IV in large vein
Reason: Administering vancomycin through a peripheral IV in a large vein is important to reduce the risk of phlebitis and irritation. Vancomycin is known to be irritating to veins, and using a large vein helps to dilute the medication more effectively, reducing the risk of vein inflammation. In this case, the peripheral IV was started in the right antecubital with a 20-gauge catheter, which is appropriate for the administration of vancomycin. Ensuring proper IV placement and using a large vein can help prevent complications associated with IV administration of this antibiotic.
Choice E: Used for prophylaxis
Reason: Vancomycin is being used as a prophylactic measure to prevent endocarditis in this patient. Prophylactic use of antibiotics is common in patients undergoing certain surgical procedures, especially those with a history of heart conditions, to prevent bacterial infections. In this case, the patient is undergoing pacemaker insertion, and the use of vancomycin as prophylaxis is appropriate to prevent potential infections. Prophylactic administration of antibiotics like vancomycin is a standard practice to reduce the risk of postoperative infections, particularly in patients with a higher risk of complications.
Choice F: Blood urea nitrogen 17 mg/dl (6.07 mmol/L)
Reason: The blood urea nitrogen (BUN) level of 17 mg/dL is within the normal range (7-20 mg/dL). While BUN levels are important indicators of renal function, they are not directly related to the safety of administering vancomycin in this context. Vancomycin dosing does need to consider renal function, but the BUN level alone does not provide sufficient information to determine the safety of administration. Therefore, this choice is not as directly relevant as the other options.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
