A nurse in the emergency department is caring for a client who has sustained a head injury. The nurse notes the client's IV fluids are infusing at 125 mL/hr. Which of the following is an appropriate action by the nurse?
Slow the rate to 50 mL/hr.
Increase the rate to 250 mL/hr.
Slow the rate to 20 mL/hr.
Continue the rate at 125 mL/hr.
The Correct Answer is D
Choice A Reason: This choice is incorrect because slowing the rate to 50 mL/hr may not be enough to prevent cerebral edema, which is a common complication of head injury. Cerebral edema is a swelling of the brain tissue due to increased fluid accumulation. It can cause increased intracranial pressure (ICP), which can lead to brain damage or death. Therefore, the nurse should limit the fluid intake of the client with head injury to avoid worsening the condition.
Choice B Reason: This choice is incorrect because increasing the rate to 250 mL/hr may cause fluid overload, which can also increase the ICP and worsen the cerebral edema. Fluid overload is a condition in which the body has too much fluid, which can impair the function of the heart, lungs, and kidneys. Therefore, the nurse should avoid giving too much fluid to the client with head injury.
Choice C reason: Reducing the infusion to 20 mL/hr is excessively low and may cause hypotension or inadequate maintenance of vascular access and medication delivery. Such a drastic decrease could impair perfusion to injured brain tissue and is not an appropriate independent nursing action without a specific order.
Choice D reason: Maintaining the current prescribed infusion rate avoids abrupt volume shifts that could alter intracranial pressure. The nurse should monitor neurologic status and vital signs, ensure the IV is patent, and follow provider orders; only change the rate when clinically indicated or when directed by the prescriber.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is D
Explanation
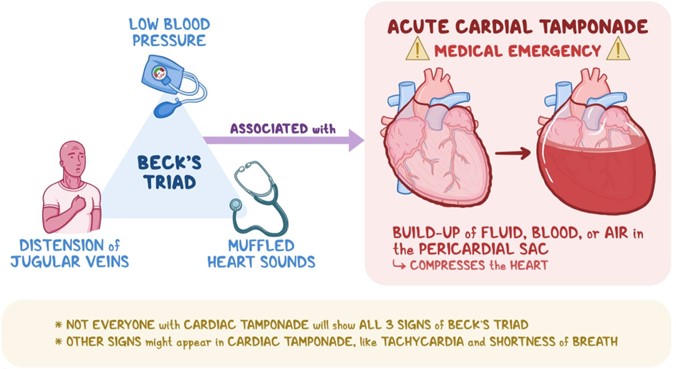
Choice A Reason: This choice is incorrect because flatened neck veins are not a sign of cardiac tamponade. Cardiac tamponade is a condition in which fluid accumulates in the pericardial sac that surrounds the heart, causing compression and impaired filling of the heart chambers. This leads to reduced cardiac output and hypotension. One of the manifestations of cardiac tamponade is distended neck veins due to increased venous pressure and impaired venous return.
Choice B Reason: This choice is incorrect because bradycardia is not a sign of cardiac tamponade. Bradycardia is a condition in which the heart rate is slower than normal (less than 60 beats per minute). It may be caused by various factors such as vagal stimulation, medication side effects, hypothyroidism, or sinus node dysfunction. It may cause symptoms such as fatigue, dizziness, or syncope, but it does not indicate cardiac tamponade.
Choice C Reason: This choice is incorrect because sudden lethargy is not a specific sign of cardiac tamponade. Lethargy is a condition in which the person feels tired, sluggish, or drowsy. It may be caused by various factors such as sleep deprivation, depression, infection, anemia, or hypoglycemia. It may affect the person's mental and physical performance, but it does not indicate cardiac tamponade.
Choice D Reason: This choice is correct because muffled heart sounds are a sign of cardiac tamponade. Muffled heart sounds are heart sounds that are fainter or softer than normal due to reduced transmission of sound waves through fluid-filled pericardial sac. They may indicate that the heart function is compromised by cardiac tamponade and require immediate intervention such as pericardiocentesis (removal of fluid from pericardial sac).
Correct Answer is B
Explanation
Choice A Reason: Preventing musculoskeletal disability is important, but not the priority focus of care. The nurse should first assess and manage the client's life-threatening injuries, such as airway obstruction, bleeding, shock, or brain injury.
Choice B Reason: Airway protection is the priority focus of care for a client with multiple system trauma. The nurse should ensure that the client has a patent airway and adequate ventilation, as any compromise in these areas can quickly lead to hypoxia, respiratory failure, and death.
Choice C Reason: Stabilizing cardiac arrhythmias is also important, but not the priority focus of care. The nurse should monitor the client's cardiac rhythm and treat any arrhythmias that may occur, but only after securing the airway and breathing.
Choice D Reason: Decreasing intracranial pressure is another important goal, but not the priority focus of care. The nurse should assess the client's neurological status and intervene to prevent or reduce increased intracranial pressure, such as elevating the head of the bed, maintaining normothermia, and administering osmotic diuretics. However, these measures are secondary to ensuring adequate oxygenation and perfusion.

Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
