A nurse is caring for a client who is 1 day postoperative following an open thoracotomy. The client is receiving oxygen mist at 40% by face tent. The client's SPO2 is 89-96%. ABG results are: pH 7.31, PaO2 93 mm Hg, PCO2 5O mm Hg, HCO3 25 mEq/L. Which of the following is an appropriate action by the nurse?
Position the client prone and have the respiratory therapist perform postural drainage.
Place the client in high-Fowler's position and encourage the use of incentive spirometer and coughing.
Increase oxygen to 70%.
Switch oxygen to a nonrebreather mask.
The Correct Answer is B
A. Prone positioning and postural drainage are typically not appropriate interventions for a client 1 day postoperative following an open thoracotomy, as this could place stress on the incision site and cause discomfort or injury.
B. High-Fowler's position facilitates lung expansion, which can improve ventilation and oxygenation. Encouraging the use of an incentive spirometer and promoting coughing helps clear secretions and expand the lungs, addressing the mild respiratory acidosis indicated by the ABG results (pH 7.31 and PaCO2 50 mm Hg).
C. Increasing oxygen to 70% is not appropriate, as the PaO2 level is within normal limits (93 mm Hg). The client's issue appears to be related more to ventilation (indicated by the elevated PaCO2) rather than oxygenation, so additional oxygen would not address the underlying cause and could lead to oxygen toxicity if used long-term.
D. A nonrebreather mask delivers a high concentration of oxygen, which is not necessary in this case since the client’s PaO2 is already adequate. The primary issue is not a lack of oxygen but rather the retention of CO2, so promoting ventilation and lung expansion through positioning and respiratory exercises is more appropriate.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
A. Loose connective tissue:
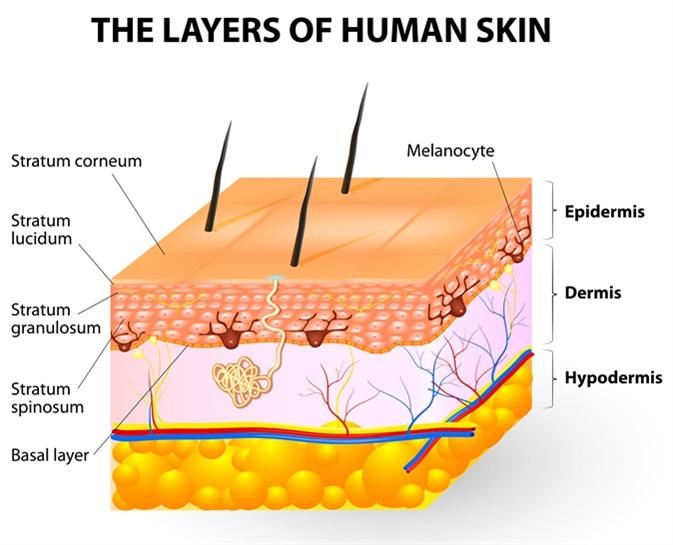
Melanocytes are not typically found in loose connective tissue. Their primary location is within the epidermis, specifically in the basal layer, where they interact with keratinocytes to produce melanin and contribute to skin color. Loose connective tissue contains collagen and elastin fibers, as well as fibroblasts, but it does not house melanocytes.
B. Epidermis:
This is the correct answer. Melanocytes are primarily located in the basal layer of the epidermis, which is the deepest layer of the epidermis. These cells produce melanin, a pigment that helps protect the skin from UV radiation and determines skin color. Melanocytes are interspersed among keratinocytes in the epidermis and transfer melanin to keratinocytes to provide skin pigmentation.
C. Dermis:
The dermis is the layer of skin beneath the epidermis and consists of connective tissue, blood vessels, nerves, hair follicles, and sweat glands. While the dermis plays a crucial role in supporting and nourishing the epidermis, melanocytes are not primarily located in the dermis. They are confined to the basal layer of the epidermis.
D. Superficial fascia:
The superficial fascia, also known as the subcutaneous tissue or hypodermis, lies beneath the dermis and consists of adipose (fat) tissue and connective tissue. It provides insulation, energy storage, and cushioning for underlying structures. However, melanocytes are not typically found in the superficial fascia. They are restricted to the epidermis, specifically the basal layer, where they carry out their function of melanin production.
Correct Answer is C
Explanation
A. Inform the client that the recovery nurse will instruct them how to manage postoperative pain:
This is an important aspect of postoperative care, but it is typically addressed by the post-anesthesia care unit (PACU) or recovery nurse after surgery rather than in the preoperative education phase. While pain management education is crucial, the focus of preoperative education is usually on what to expect before, during, and immediately after surgery.
B. Remind the client they will return to their room after surgery:
This information is part of the preoperative instructions and helps alleviate anxiety by providing clarity about the post-surgical process. However, it may not be the most critical aspect of preoperative education compared to other options.
C. Provide instructions about how to cough and deep breathe effectively:
This is a key nursing intervention to include in preoperative education. Teaching the client how to cough and deep breathe effectively helps prevent postoperative complications such as atelectasis and pneumonia. These breathing techniques are typically taught preoperatively to ensure the client understands and can perform them correctly after surgery.
D. Notify the client that they will receive a food tray in the recovery room:
While it's important for the client to understand the postoperative diet plan, including any dietary restrictions or instructions, this information is usually provided after surgery rather than in the preoperative education phase.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
