A nurse is caring for a client that is immobile. The nurse recognizes that the appearance of non-blanchable erythema on the heels most likely indicates which of the following stages of pressure injuries?
Stage III pressure injury
Stage IV pressure injury
Stage II pressure injury
Stage I pressure injury
The Correct Answer is D
A. Stage III pressure injury
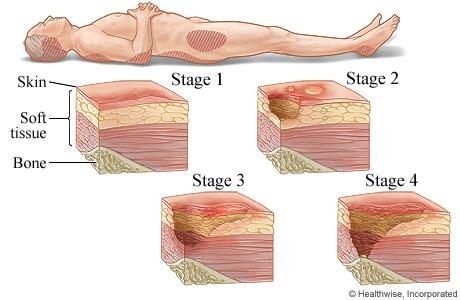
Stage III pressure injuries involve full-thickness skin loss, extending into the subcutaneous tissue but not through the fascia. These wounds typically present as deep craters and may involve undermining or tunneling. Non-blanchable erythema alone without visible skin loss is not characteristic of a Stage III pressure injury.
B. Stage IV pressure injury
Stage IV pressure injuries are the most severe and involve full-thickness tissue loss with exposed bone, tendon, or muscle. These wounds often have extensive tissue damage and can be difficult to manage. Again, non-blanchable erythema without visible skin loss is not indicative of a Stage IV pressure injury.
C. Stage II pressure injury
Stage II pressure injuries involve partial-thickness skin loss with damage to the epidermis and possibly the dermis. These wounds often present as shallow open ulcers or blisters and may have characteristics such as intact or ruptured blisters. While Stage II injuries can present with erythema, non-blanchable erythema specifically indicates a Stage I injury.
D. Stage I pressure injury
Stage I pressure injuries are the earliest stage and involve non-blanchable erythema of intact skin. The skin may be warmer or cooler than surrounding tissue and may have changes in sensation. There is no visible skin loss at this stage, but the area is at risk for further injury if pressure is not relieved. Therefore, non-blanchable erythema on the heels most likely indicates a Stage I pressure injury.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is ["A","B","E"]
Explanation
A. Morbidly obese patient: Obesity is a known risk factor for VTE due to several reasons. Morbidly obese individuals often have impaired mobility, which can lead to venous stasis (sluggish blood flow in the veins). Additionally, obesity is associated with inflammation and changes in blood clotting factors, increasing the risk of developing blood clots in the veins.
B. A woman who smokes and takes oral contraceptives or smokes: Both smoking and oral contraceptive use are independent risk factors for VTE. Smoking can cause damage to blood vessels and alter blood clotting mechanisms, while oral contraceptives can increase the risk of blood clots due to hormonal changes.
C. Wheelchair-bound patient: While being wheelchair-bound alone may not always indicate a high risk for VTE, immobility is a significant risk factor for developing blood clots. Prolonged periods of immobility can lead to blood stasis in the veins, making wheelchair-bound patients susceptible to VTE, especially if other risk factors are present.
D. Patient with a humerus fracture: A humerus fracture on its own may not necessarily increase the risk of VTE significantly. However, if the fracture requires immobilization or surgery, especially if it affects the lower extremities or leads to prolonged immobility, the risk of VTE can increase due to decreased blood flow and stasis.
E. Patient who underwent a prolonged surgical procedure: Prolonged surgical procedures often involve anesthesia, immobility during surgery, and postoperative immobilization, all of which can contribute to venous stasis and increase the risk of developing VTE. Additionally, the surgical trauma itself can trigger inflammatory responses and alterations in blood clotting factors, further elevating the risk of blood clots.
Correct Answer is B
Explanation
A.Prone positioning and postural drainage are typically not appropriate interventions for a client 1 day postoperative following an open thoracotomy, as this could place stress on the incision site and cause discomfort or injury.
B.High-Fowler's position facilitates lung expansion, which can improve ventilation and oxygenation. Encouraging the use of an incentive spirometer and promoting coughing helps clear secretions and expand the lungs, addressing the mild respiratory acidosis indicated by the ABG results (pH 7.31 and PaCO2 50 mm Hg).
C.Increasing oxygen to 70% is not appropriate, as the PaO2 level is within normal limits (93 mm Hg). The client's issue appears to be related more to ventilation (indicated by the elevated PaCO2) rather than oxygenation, so additional oxygen would not address the underlying cause and could lead to oxygen toxicity if used long-term.
D.A nonrebreather mask delivers a high concentration of oxygen, which is not necessary in this case since the client’s PaO2 is already adequate. The primary issue is not a lack of oxygen but rather the retention of CO2, so promoting ventilation and lung expansion through positioning and respiratory exercises is more appropriate.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
