A student nurse asks the RN about the clinical manifestations of a thoracic aortic aneurysm. Which of the following findings should the nurse discuss? (Select all that apply).
Shortness of breath
Difficulty swallowing
Upper chest pain
Diaphoresis
Cough
Hoarseness
Correct Answer : A,B,C,E,F
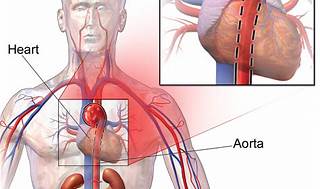
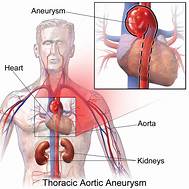
Choice A: Shortness of breath Shortness of breath can occur with a TAA due to the aneurysm compressing the trachea or the lung tissue. As the aneurysm enlarges, it can impinge on respiratory structures, leading to difficulty in breathing. A thoracic aortic aneurysm (TAA) is a bulging or dilation in the wall of the aorta as it passes through the chest cavity. TAAs can be life-threatening if they rupture or dissect and are often difficult to detect because they tend to grow slowly and usually do not cause symptoms until they become large or rupture.
Choice B: Difficulty swallowing Difficulty swallowing, or dysphagia, may be experienced if a TAA exerts pressure on the esophagus. This can happen when the aneurysm is located in the aortic arch, where the esophagus is in close proximity.
Choice C: Upper chest pain Upper chest pain is a common symptom of TAA and may be described as a deep, steady pain that can radiate to the back, neck, or jaw. The pain is caused by the stretching of the aortic wall and may be a warning sign of an impending rupture.
Choice D: Diaphoresis Diaphoresis, or excessive sweating, is not typically a direct symptom of a TAA. However, it can be associated with acute aortic syndromes, such as aortic dissection or rupture, which are medical emergencies.
Choice E: Cough A persistent cough can be a sign of a TAA, especially if the aneurysm is pressing against the trachea or bronchial tubes. The cough may sometimes produce blood if the aneurysm is causing erosion into these structures.
Choice F: Hoarseness Hoarseness can result from a TAA if the aneurysm compresses the recurrent laryngeal nerve, which controls the muscles of the voice box. This is known as Ortner’s syndrome or cardiovocal syndrome.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
Choice A reason:While sharing needles can transmit hepatitis, it is more commonly associated with hepatitis B and C, not hepatitis A.
Choice B reason:Eating shellfish from contaminated water is a well-known route of transmission for hepatitis A, aligning with the client's symptoms.
Choice C reason:Blood transfusions were a risk for hepatitis transmission in the past, but since the 1990s, blood products are screened for hepatitis, making this an unlikely source.
Choice D reason:Unprotected sex can be a route of transmission for hepatitis, but hepatitis A is more commonly spread through ingestion of contaminated food or water, not sexual contact.
Correct Answer is B
Explanation
Choice A reason: The GFR does not recover during the oliguric phase; instead, it is typically reduced, reflecting impaired kidney function.
Choice B reason: Urine output of less than 400 mL per 24 hours is characteristic of the oliguric phase of AKI. This phase can last from 1 to 7 days after kidney injury and is a crucial time for monitoring and managing the patient's fluid and electrolyte balance.
Choice C reason: BUN and creatinine levels do not decrease during the oliguric phase. They usually increase due to reduced kidney function and the inability to excrete these waste products.
Choice D reason: Renal function is not reestablished during the oliguric phase. This phase is part of the course of AKI where renal function is at its lowest, and recovery has not yet begun.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
