H/P
Four hours after her arrival to the emergency department, the patient remains in second-degree type II heart block and her vital signs are stable. She is transferred to a telemetry unit to prepare for insertion of a permanent pacemaker later in the day. When she gets out of bed to use the restroom, she felt faint and had to sit on the floor. The nurse finds her sitting on the floor beside the commode; the patient is awake but somewhat confused. The patient is assisted back to bed. The nurse notes that the ECG monitor shows that the patient's heart rate is at 40 beats/minute and she is now in third degree heart block. The Rapid Response team is called, and preparations are made for the immediate application of a transcutaneous pacemaker (TCP).
Which nursing actions should be included in the plan of care for the patient (Select All that Apply.)
Prepare to administer epinephrine
Monitor vital signs and ECG
Reassure the patient that the Transcutaneous Pacemaker is temporary
Prepare to administer atropine
Place both transcutaneous pacemaker pads on the chest over the heart
Provide analgesia as needed after the transcutaneous pacemaker is placed
Correct Answer : B,C,D,E,F
B. Continuous monitoring of vital signs, including blood pressure, heart rate, respiratory rate, and oxygen saturation, is essential for assessing the patient's hemodynamic status and response to treatment.
Additionally, continuous electrocardiographic (ECG) monitoring allows for real-time assessment of cardiac rhythm and conduction abnormalities.
C. This is an important nursing action to provide comfort and reduce anxiety for the patient. Transcutaneous pacing is often used as a temporary measure to stabilize heart rate and cardiac output until more definitive treatment, such as insertion of a permanent pacemaker, can be performed.
D. Atropine is another medication commonly used in ACLS protocols for symptomatic bradycardia and heart block. It acts to increase heart rate by blocking vagal tone. However, its effectiveness in third- degree heart block may be limited, and transcutaneous pacing is often the preferred intervention in this situation.
E. Correct placement of transcutaneous pacemaker pads is crucial for effective pacing. The pads should be placed on the chest over the heart to deliver electrical impulses and stimulate myocardial contraction. Proper placement ensures optimal pacing effectiveness and patient safety.
F. This nursing action addresses the patient's comfort and pain management following the placement of the transcutaneous pacemaker. The procedure may cause discomfort or pain, and appropriate analgesia should be provided to alleviate any discomfort and promote patient comfort.
A. Epinephrine is a medication commonly used in advanced cardiac life support (ACLS) protocols for bradycardia and heart block. In this scenario, the patient's heart rate has decreased to 40 beats/minute, indicating symptomatic bradycardia and potential hemodynamic instability. Epinephrine may be administered to increase heart rate and improve cardiac output.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is B
Explanation
B. Endotracheal intubation and positive pressure ventilation are indicated in patients with severe respiratory failure who are unable to maintain adequate oxygenation and ventilation on their own. This intervention provides mechanical support to the patient's breathing by delivering positive pressure to the lungs via an endotracheal tube. Given the patient's respiratory rate of 6 breaths/min, low oxygen saturation (SpO2 of 78%), and increasing lethargy, endotracheal intubation and positive pressure ventilation are the most appropriate interventions to ensure adequate oxygenation and ventilation.
A. CPAP is a form of non-invasive positive pressure ventilation that helps keep the airways open and improves oxygenation. However, in a patient with severe respiratory failure and impending respiratory arrest, CPAP alone may not be sufficient to adequately support ventilation and oxygenation. CPAP is typically used in patients with milder forms of respiratory failure or as a step-down therapy from invasive mechanical ventilation.
C. Insertion of a mini-tracheostomy is not typically indicated in a patient with severe respiratory failure and impending respiratory arrest. While tracheostomy may be considered in certain cases for long-term ventilation or airway management, it is not the first-line intervention in an acute situation like this.
Additionally, frequent suctioning may not address the underlying cause of respiratory failure or improve oxygenation.
D. Administering 100% oxygen via a non-rebreather mask can help improve oxygenation temporarily. However, in a patient with severe respiratory failure and impending respiratory arrest, non-invasive oxygen therapy alone may not be sufficient to maintain adequate oxygenation and ventilation.
Endotracheal intubation and positive pressure ventilation are more definitive interventions to ensure adequate support for the patient's breathing.
Correct Answer is B
Explanation
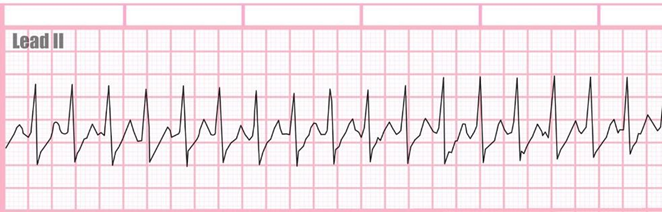
B This maneuver, called the Valsalva maneuver, can sometimes help to restore normal heart rhythm in cases of SVT. It involves blowing forcefully into a syringe or performing a similar action that increases intra-abdominal pressure, which can stimulate the vagus nerve and help to slow down the heart rate.
A Defibrillation is a treatment used for life-threatening cardiac arrhythmias, particularly ventricular fibrillation or pulseless ventricular tachycardia. It involves delivering a therapeutic dose of electrical energy to the heart with a device called a defibrillator.
C Drawing troponin levels may be appropriate if there is suspicion of myocardial infarction as the cause of chest palpitations or if there are other symptoms suggestive of acute coronary syndrome. However, in the context of SVT presenting with chest palpitations and a racing heart, the priority is to address the arrhythmia first
D Amiodarone is an antiarrhythmic medication used to treat various types of cardiac arrhythmias, including ventricular and supraventricular arrhythmias. While it can be effective in certain cases of SVT, it is not typically the first-line treatment or the immediate next step in managing SVT in the emergency department.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
