The nurse is caring for a client with elevated parathyroid hormone levels. Which safety precaution should the nurse include in the plan of care?
Hypothermia.
Aspiration.
Falls.
Suicide.
The Correct Answer is C
Choice A reason: Hypothermia is not typically associated with hyperparathyroidism and does not require specific precautions in this context.
Choice B reason: Aspiration may be a concern for patients with severe hypercalcemia if they have altered mental status, but it is not the primary safety precaution.
Choice C reason: Falls are a significant risk due to potential muscle weakness, skeletal fragility, and possible neuromuscular symptoms caused by hypercalcemia.
Choice D reason: Suicide is not directly related to hyperparathyroidism; however, mental health should always be monitored in patients with chronic conditions.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
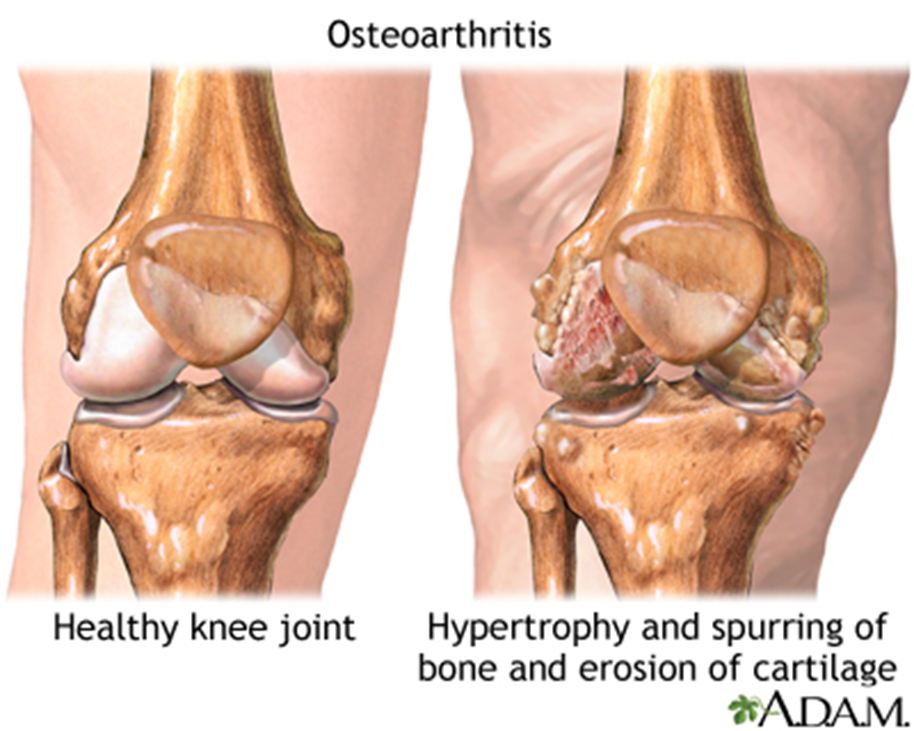
Choice A reason: Asking the client to describe the pain is essential as it provides subjective information about the pain's quality, intensity, and impact on daily activities, which is crucial for assessing osteoarthritis pain.
Choice B reason: Observing body language and movement can offer insights into the pain's impact on function, but it does not replace the client's verbal description of the pain experience.
Choice C reason: Identifying effective pain relief measures is part of managing osteoarthritis but does not directly assess the quality of the client's knee pain.
Choice D reason: Providing a numeric pain scale is a method to quantify pain intensity but may not fully capture the quality or characteristics of the pain.
Correct Answer is A
Explanation
Choice A reason: Understanding the reason for taking aspirin is crucial because it could be for a chronic condition that requires antiplatelet action, which ibuprofen does not provide. Aspirin is often prescribed for its antiplatelet effect to prevent blood clots, while ibuprofen is primarily used for pain and inflammation.
Choice B reason: While the dosage of ibuprofen is important, it is secondary to understanding the purpose of the aspirin therapy. Overdosing on ibuprofen can lead to serious side effects, but the immediate risk of stopping aspirin without a suitable substitute could be more critical.
Choice C reason: Assessing the amount of pain control is important to evaluate the effectiveness of ibuprofen as a substitute for aspirin. However, this does not address the potential risks associated with the cessation of aspirin, especially if it was prescribed for cardiovascular reasons.
Choice D reason: The presence of gastric pain could indicate an adverse reaction to ibuprofen, which is known to cause gastrointestinal issues. However, this information is not as immediately necessary as understanding the reason for aspirin therapy, which could have significant implications for the client's health.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
