A client has not voided eight hours after surgery and says to the nurse, “I don’t think I can urinate.” What should be the first action for the nurse?
Assess the client’s bladder.
Administer pain medication.
Increase the client’s fluid intake.
Inform the surgeon of the client’s status.
The Correct Answer is A
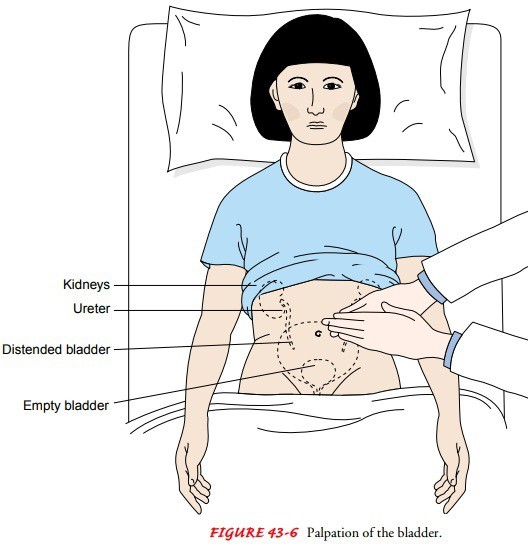
The nurse should first assess the client’s bladder for distention by palpating the lower abdomen between the symphysis pubis and the umbilicus.
This can indicate urinary retention, which is a common postoperative complication. The nurse should also measure the bladder volume using a bladder scanner if available.
Choice B. Inform the surgeon that the client’s status is wrong because the nurse should first assess the client before notifying the surgeon.
The surgeon may order interventions based on the assessment findings.
Choice C. Increasing the client’s fluid intake is wrong because increasing fluid intake may worsen bladder distention and discomfort.
The nurse should encourage fluid intake only after ensuring adequate urinary output.
Choice D. Administering pain medication is wrong because pain medication may not be indicated for urinary retention.
Pain medication may also cause urinary retention by relaxing the bladder muscles and impairing the micturition reflex.
Normal urine output is about 30 mL per hour or 240 mL in eight hours.
The nurse should monitor the client’s intake and output and report any signs of urinary retention to the surgeon.
Urinary retention can lead to infection, bladder damage, and renal impairment if not treated promptly.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
This is the most appropriate action because it respects the client’s right to know and the family’s right to privacy.
It also allows the nurse to collaborate with the family and the healthcare provider to provide the best care for the client.
Choice B is wrong because it violates the client’s autonomy and dignity.
It also prevents the client from making informed decisions about end-of-life care.
Choice C is wrong because it denies the reality of the situation and does not address the client’s concerns.
It also may increase the client’s anxiety and frustration.
Choice D is wrong because it disregards the family’s wishes and cultural values.
It also may cause harm to the client and the family by breaking their trust and creating conflict.
Correct Answer is D
Explanation
A heart murmur is a priority assessment for a toddler who is diagnosed with fetal alcohol syndrome because it may indicate a congenital heart defect, which can affect the child’s growth, development and oxygenation. According to the health search results, fetal alcohol syndrome can cause heart and kidney problems, among other complications.
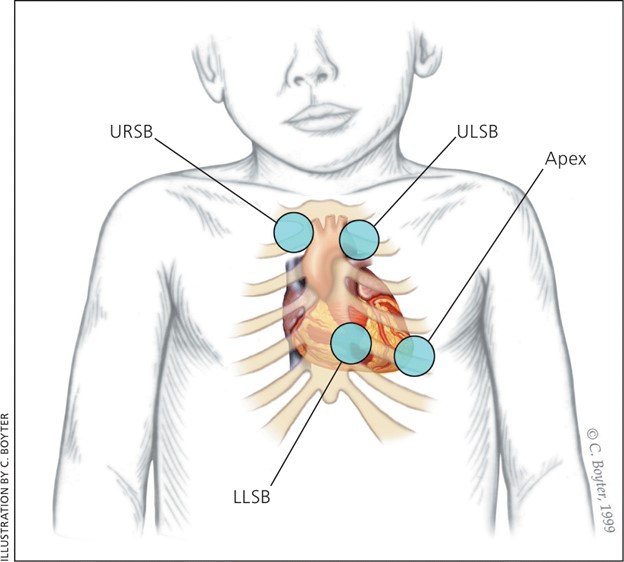
Choice A is wrong because small head size is a common feature of fetal alcohol syndrome, but it is not a priority assessment. It indicates that the child has microcephaly, which is associated with intellectual and learning disabilities.
Choice B is wrong because poor coordination is another common feature of fetal alcohol syndrome, but it is not a priority assessment. It indicates that the child has problems with motor skills and balance.
Choice C is wrong because speech and language delays are also common features of fetal alcohol syndrome, but they are not a priority assessment. They indicate that the child has problems with communication and social skills.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
