The emergency department nurse is assessing a patient who is in the compensatory stage of hypovolemic shock. Which manifestations does the nurse expect? Select all that apply.
Elevated heart rate.
Elevated respiratory rate.
Decreased pulse rate.
Decrease systolic blood pressure.
Decreased urine output.
Bilateral crackles in the lung bases.
Correct Answer : A,B,D,E
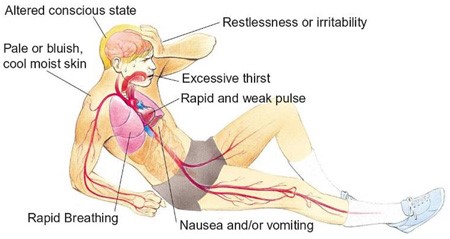
These manifestations occur as compensatory mechanisms in response to decreased blood volume and compromised tissue perfusion. The body attempts to compensate for the inadequate circulating volume by increasing heart rate (A) and respiratory rate (B) to enhance oxygen delivery.
D. The decreased systolic blood pressure (D) is a result of decreased cardiac output and vasoconstriction in an attempt to maintain perfusion to vital organs.
E. The decreased urine output (E) is a result of decreased renal perfusion due to decreased blood volume.
C. Decreased pulse rate in (option C) is incorrect because it is not typically seen in the compensatory stage of hypovolemic shock. The body tries to increase heart rate to maintain cardiac output and compensate for the decreased blood volume.
F. Bilateral crackles in (option F) is incorrect because the lung bases are more commonly associated with conditions such as pulmonary edema or fluid overload, rather than the compensatory stage of hypovolemic shock.
It's important to note that the manifestations of shock can vary depending on individual patient factors and the underlying cause of shock. Therefore, a comprehensive assessment and clinical judgment are necessary to fully evaluate the patient's condition.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is C
Explanation
Hypovolemic shock is a life-threatening condition resulting from severe blood or fluid loss. The patient in this scenario exhibits signs of hypovolemic shock, such as low blood pressure, tachycardia, cool and clammy skin, and decreased urine output.
When assessing the prescription options, the nurse should consider the appropriateness of each intervention for hypovolemic shock. Plasmanate is a type of plasma protein fraction that is used for volume expansion in certain situations. However, in hypovolemic shock, the primary intervention is to restore intravascular volume promptly. Plasmanate alone may not be sufficient for rapid-volume resuscitation.
In hypovolemic shock, the initial management typically involves the administration of crystalloid solutions, such as Lactated Ringers or Normal Saline, to restore intravascular volume. Therefore, the prescription of Plasmanate as the primary intervention raises concerns and should be questioned by the nurse.
A. Dopamine (Intropin) 12 mcg/min in (option A) is incorrect because: Dopamine is a vasopressor medication used to increase blood pressure and cardiac output. It is a suitable option for hypovolemic shock to support blood pressure and tissue perfusion.
B. Dobutamine (Dobutrex) 5 mcg/kg/min in (option B) is incorrect because: Dobutamine is an inotropic medication that helps improve cardiac contractility and cardiac output. It can be beneficial in cases of hypovolemic shock with signs of poor cardiac function.
D. Bumetanide (Bumex) 1 mg IV in (option D) is incorrect because: Bumetanide is a loop diuretic used to promote diuresis. However, in the context of hypovolemic shock, diuretics are generally not the first-line treatment as they can further reduce intravascular volume and worsen the patient's condition.
It is essential for the nurse to consult with the healthcare provider regarding the prescription order of Plasmanate and consider alternative interventions for rapid volume resuscitation in hypovolemic shock.
Correct Answer is D
Explanation
When the low-pressure alarm sounds, it indicates that the pressure being detected by the arterial line is below the set threshold. This could be due to a variety of reasons, such as a loose connection, air bubbles, or a shift in the zero-reference point.
Rezeroing the monitoring equipment involves recalibrating or resetting the baseline reference point for the arterial pressure waveform. This ensures accurate measurement and monitoring of the patient's arterial pressure.
A. Checking the right hand for a rash in (option A) is incorrect because While assessing the patient for any skin changes or rashes is important, it is not the first action to take in response to a low-pressure alarm.
B. Assessing the waveform for under-dampening in (option B) is incorrect because Assessing the waveform characteristics is important in arterial line monitoring, but it may not be the initial action when the low-pressure alarm sounds. Rezeroing the equipment should be performed before assessing waveform characteristics.
C. Assessing for cardiac dysrhythmias in (option C) is incorrect because Assessing for dysrhythmias is an important aspect of patient care, but it may not be directly related to the low-pressure alarm from the arterial line. Rezeroing the monitoring equipment takes precedence.
Therefore, when the low-pressure alarm sounds for a patient with an arterial line, the nurse should first re-zero the monitoring equipment to ensure accurate measurement of arterial pressure.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
