Which of the following clinical manifestations is NOT considered part of Beck's triad (classic indications of cardiac tamponade)?
muffled heart tones
marked hypotension
distended jugular veins
widening pulse pressure
The Correct Answer is D
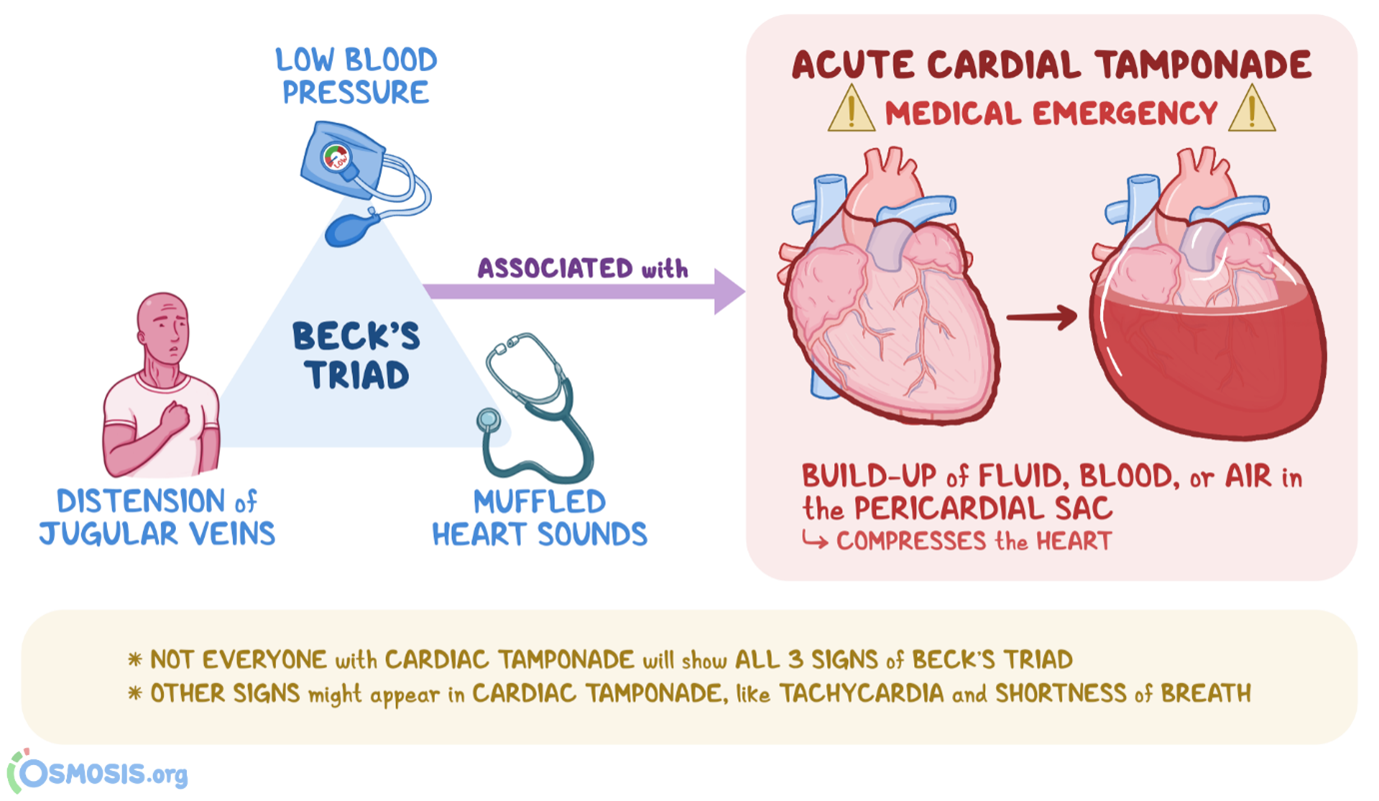
Beck's triad consists of three classic clinical manifestations that are suggestive of cardiac tamponade, which is the compression of the heart by accumulated fluid or blood within the pericardial sac. The three components of Beck's triad include:
A. Muffled heart tones in (option A) are incorrect because Cardiac tamponade can dampen or muffle heart sounds due to the presence of fluid or blood around the heart, which can impair sound transmission.
B. Marked hypotension in (option B) is incorrect because Cardiac tamponade can cause decreased cardiac output, leading to hypotension, which is characterized by low blood pressure.
C. Distended jugular veins in (option C) is incorrect because Elevated venous pressure resulting from impaired filling and elevated right-sided heart pressures can lead to jugular vein distension, which is commonly seen in cardiac tamponade.
However, widening pulse pressure (the difference between systolic and diastolic blood pressure) is not typically part of Beck's triad. Widening pulse pressure is associated with her conditions such as aortic regurgitation, hyperthyroidism, or conditions involving increased stroke volume, rather than cardiac tamponade specifically.
Nursing Test Bank
Naxlex Comprehensive Predictor Exams
Related Questions
Correct Answer is A
Explanation
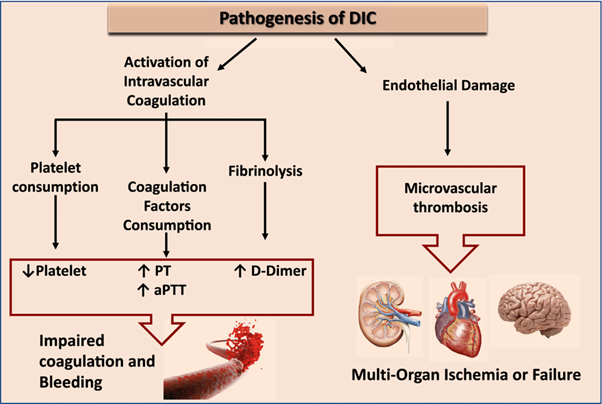
Disseminated intravascular coagulation (DIC) is a condition characterized by both widespread activation of the coagulation system and excessive clotting, leading to the consumption of clotting factors and platelets. This results in a prothrombotic state, which can lead to organ dysfunction and bleeding manifestations.
Elevated D-dimer levels are a characteristic finding in DIC. D-dimer is a fibrin degradation product that is elevated when there is excessive fibrin formation and breakdown. Elevated D-dimer indicates ongoing fibrinolysis and activation of the clotting system.
B. Decreased prothrombin time in (option B) is incorrect because: DIC is characterized by consumption of clotting factors, which can result in prolongation of the prothrombin time (PT) as well as other coagulation tests.
C. Decreased partial thromboplastin time in (option C) is incorrect because Similar to the prothrombin time, the partial thromboplastin time (PTT) can also be prolonged in DIC due to the consumption of clotting factors.
D. Elevated fibrinogen level in (option D) is incorrect because, In DIC, there is consumption of fibrinogen along with other clotting factors. Therefore, elevated fibrinogen levels are not consistent with the pathophysiology of DIC.
Correct Answer is B
Explanation
Fresh frozen plasma (FFP) is a blood product that contains various clotting factors, including factors II, V, VII, VIII, IX, X, XI, and XIII. These clotting factors are essential for the normal coagulation process. In patients with shock, coagulation abnormalities can occur, and administration of FFP can help replenish the deficient clotting factors and restore proper coagulation function.
The other options mentioned are not the primary components replaced by fresh frozen plasma:
A. Red blood cells are in (option A) is incorrect because Red blood cells carry oxygen and are typically replaced by packed red blood cell transfusions in cases of significant blood loss or anemia. Fresh frozen plasma does not contain a significant amount of red blood cells.
C. Platelets in (option C) is incorrect because: Platelets play a role in blood clotting and are typically replaced by platelet transfusions in cases of thrombocytopenia or platelet dysfunction. Fresh frozen plasma may contain a small number of platelets but is not the primary source for platelet replacement.
D. White blood cells in (option D) is incorrect because White blood cells are part of the immune system and are not typically replaced using fresh frozen plasma. Fresh frozen plasma does not contain a significant amount of white blood cells.
Therefore, fresh frozen plasma is primarily administered to patients in shock to replace clotting factors and help restore proper coagulation function.
Whether you are a student looking to ace your exams or a practicing nurse seeking to enhance your expertise , our nursing education contents will empower you with the confidence and competence to make a difference in the lives of patients and become a respected leader in the healthcare field.
Visit Naxlex, invest in your future and unlock endless possibilities with our unparalleled nursing education contents today
Report Wrong Answer on the Current Question
Do you disagree with the answer? If yes, what is your expected answer? Explain.
Kindly be descriptive with the issue you are facing.
