Please set your exam date
Lower Respiratory Tract Infections
Study Questions
Practice Exercise 1
A nurse is caring for a 2-year-old client with acute bronchitis. Which of the following interventions is contraindicated for this client?
Explanation
Acute bronchitis is an inflammation of the bronchi, usually caused by viral infections in children. It presents with cough, fever, fatigue, coarse breath sounds, and sometimes wheezing. The cough is a protective reflex that helps clear mucus from the airways.
Rationale for correct answer:
3. Administering a cough suppressant is contraindicated in young children with bronchitis. Suppressing the cough reflex prevents clearance of secretions, leading to mucus plugging and worsening airway obstruction. Additionally, many over-the-counter cough suppressants have been shown to be unsafe and ineffective in children under 6 years old.
Rationale for incorrect answers:
1. Encouraging oral fluids is a correct intervention. Fluids help thin secretions, prevent dehydration, and improve mucus clearance.
2. Using a cool-mist humidifier soothes inflamed airways, reduces irritation, and eases coughing.
3. Providing acetaminophen for fever is an appropriate intervention since it safely reduces fever and discomfort in children.
Take home points
- Cough suppressants are contraindicated in young children due to risk of respiratory depression and impaired secretion clearance.
- Management of acute bronchitis in children is primarily supportive: hydration, rest, humidified air, and fever control.
- Antibiotics are generally not indicated, as most cases are viral.
A parent asks the nurse why the doctor did not prescribe an antibiotic for their 6-year-old child who was diagnosed with acute bronchitis. What is the nurse's best response?
Explanation
Acute bronchitis in children is usually caused by viral infections such as influenza, parainfluenza, adenovirus, or respiratory syncytial virus (RSV). Treatment is supportive, focusing on hydration, fever management, rest, and airway support.
Rationale for correct answer:
2. "Most cases of bronchitis are caused by viruses, and antibiotics don't kill viruses." This is the best response because it provides accurate education to the parent, explaining that antibiotics are ineffective against viruses and therefore not prescribed for viral bronchitis.
Rationale for Incorrect Answers:
1. "Antibiotics are only used if the fever is very high." Fever severity is not the deciding factor for antibiotic use. The etiology (viral vs. bacterial) is what matters.
3. "The doctor is saving the antibiotics in case your child develops pneumonia." Antibiotics are not “saved” for later; they are prescribed when there is a confirmed or highly suspected bacterial infection.
4. "Antibiotics are contraindicated because they can make a viral infection worse." Antibiotics don’t worsen viral infections; they are simply ineffective and unnecessary.
Take home points
- Most acute bronchitis in children is viral, so antibiotics are not indicated.
- Supportive care (hydration, humidified air, fever control, rest) is the mainstay of management.
- Unnecessary antibiotics increase the risk of resistance, allergic reactions, and side effects.
- Nurses play a key role in parent education to reduce misconceptions about antibiotic use.
Which physical assessment finding is most characteristic of acute bronchitis in an older child?
Explanation
Acute bronchitis in children is usually caused by viral infections such as influenza, parainfluenza, adenovirus, or respiratory syncytial virus (RSV). Treatment is supportive, focusing on hydration, fever management, rest, and airway support.
Rationale for correct answer:
3. Wheezing or coarse rhonchi on auscultation are the most characteristic findings of acute bronchitis. They result from airway inflammation, mucus, and narrowing of the bronchi, which cause turbulent airflow.
Rationale for incorrect answers:
1. Inspiratory stridor indicates upper airway obstruction such as croup, epiglottitis, or foreign body, not bronchitis, which affects the lower airways.
2. A persistent cough is the hallmark symptom of acute bronchitis, not the absence of a cough.
4. Hyperresonance to percussion suggests air trapping or hyperinflation, more characteristic of asthma or emphysema, not acute bronchitis.
Take home points
- The key assessment finding in acute bronchitis is wheezing or coarse rhonchi that may clear with coughing.
- Cough is the hallmark symptom and may last several weeks.
- Bronchitis affects the lower respiratory tract while stridor points to upper airway problems.
- Supportive management remains the mainstay; antibiotics are usually not needed.
The primary goal of nursing management for a child with acute viral bronchitis is:
Explanation
Acute bronchitis in children is usually caused by viral infections such as influenza, parainfluenza, adenovirus, or respiratory syncytial virus (RSV). Treatment is supportive, focusing on hydration, fever management, rest, and airway support.
Rationale for correct answer:
2. Promoting rest and adequate fluid intake is the primary goal in nursing management. Rest helps recovery, while fluids prevent dehydration and thin mucus, making secretions easier to clear. Supportive measures are the cornerstone of care for viral bronchitis.
Rationale for incorrect answers:
1. While important, preventing bacterial superinfection is a secondary concern. The main goal is supportive care, not prophylaxis.
3. Administering a leukotriene modifier are used in chronic asthma, not in acute viral bronchitis.
4. Eradicating the causative organism is not possible with antibiotics since bronchitis is viral. The infection resolves on its own with supportive measures.
Take home points
- Supportive care (rest, fluids, fever management, humidified air) is the cornerstone of managing acute viral bronchitis in children.
- Antibiotics are not effective because the condition is viral.
- Nurses should monitor for signs of worsening respiratory distress or secondary bacterial infection.
Practice Exercise 2
A 5-month-old infant with RSV bronchiolitis is in respiratory distress. The baby has copious secretions, increased work of breathing, cyanosis, and a respiratory rate of 78. What is the most appropriate initial nursing intervention?
Explanation
Respiratory Syncytial Virus (RSV) bronchiolitis is a common viral lower respiratory tract infection in infants that leads to airway inflammation, edema, and excessive mucus production. Infants are at high risk of respiratory distress and failure due to smaller airways and limited reserve. The priority is to maintain a patent airway and adequate oxygenation.
Rationale for correct answer:
3. The infant has copious secretions, cyanosis, tachypnea (RR 78), and increased work of breathing, which indicates severe distress. The first action is to clear the airway with suctioning, then deliver supplemental oxygen to address hypoxemia. The nurse should be prepared for respiratory failure and intubation if the child deteriorates. This directly addresses airway and breathing, which are always the ABCs priority.
Rationale for incorrect answers:
1. Attempting to calm the infant by placing him in his mother's lap and offering him a bottle is unsafe: infants in respiratory distress cannot coordinate sucking, swallowing, and breathing. A bottle increases risk of aspiration and worsens hypoxia.
2. Alerting the physician to the situation and asking for an order for a stat chest radiograph delays immediate, lifesaving interventions. A chest X-ray may confirm diagnosis but is not priority in acute distress.
4. Bring the emergency equipment to the room and beginning bag-valve-mask ventilation is appropriate for respiratory arrest, not initial distress when the infant is still breathing spontaneously. The infant first needs airway clearance and oxygen.
Take home points
- In RSV bronchiolitis, the priority is always airway clearance (suctioning) and oxygen administration.
- Feeding is contraindicated in infants with severe respiratory distress.
- Nurses must anticipate respiratory failure and have emergency equipment ready.
- ABCs guide all decisions: Airway → Breathing → Circulation.
A baby is born 12 weeks preterm. The nurse should determine that which of the following monthly medication injections would be appropriate for this child to receive?
Explanation
Respiratory syncytial virus (RSV) is a common viral infection that primarily affects infants and young children. It causes bronchiolitis and pneumonia, leading to symptoms such as cough, rhinorrhea, wheezing, fever, and respiratory distress.
Rationale for correct answer:
2. Synagis (palivizumab) provides passive immunity against RSV. Given monthly via intramuscular injection during RSV season to reduce the risk of hospitalization in high-risk infants like this preterm baby. This is the standard prophylaxis for preterm infants.
Rationale for incorrect answers:
1. Hepatitis B immune globulin is given to newborns of mothers positive for HBsAg, not specifically to preterm infants for RSV prevention.
3. Pulmozyme (dornase alfa) is a mucolytic used in cystic fibrosis to thin pulmonary secretions, not for RSV prophylaxis.
4. Varicella-zoster immune globulin is given to high-risk, non-immune children after exposure to chickenpox, not routinely for preterm infants.
Take home points
- Palivizumab (Synagis) is the prophylactic drug for RSV prevention in preterm or high-risk infants.
- RSV is a leading cause of bronchiolitis and pneumonia in infants, with severe cases requiring hospitalization.
- Other immune globulins (Hep B, VZIG) are used in specific exposure scenarios, not routine prematurity.
- Nurses should teach parents that Synagis is preventive, not curative, and must be given monthly during RSV season.
In most cases, bronchiolitis is caused by a viral agent, most commonly respiratory syncytial virus (RSV). The nurse should keep in mind which statement regarding RSV infections?
Explanation
Bronchiolitis is a common viral lung infection that primarily affects infants and young children, especially those under 2 years old. It targets the bronchioles, which are the smallest airways in the lungs, causing them to become swollen, irritated, and clogged with mucus, making it hard to breathe.
Rationale for correct answer:
2. RSV primarily infects the epithelial cells of the respiratory tract, damaging cilia and leading to bronchiolar obstruction and wheezing. The virus infects and replicates in the respiratory tract mucosal cells, causing inflammation, edema, and increased mucus production, which leads to airway obstruction.
Rationale for incorrect answers:
1. RSV is most common in late fall, winter, and early spring and is not more prevalent in the summer. This is because lower temperatures help RSV survive longer on surfaces and in the air. Reduced humidity also allows respiratory droplets to linger and travel farther, increasing transmission. Furthermore, indoor crowding during colder months in schools, daycare, and family gatherings boosts close contact and viral spread.
3. RSV primarily affects infants and young children under 2 years, especially preterm infants or those with chronic illness.
4. RSV is highly contagious and spreads easily via droplets, secretions, and contact with contaminated surfaces.
Take home points
- RSV infects respiratory tract mucosa, leading to bronchiolitis and pneumonia.
- Most common in infants under 2 years, especially during winter months.
- RSV is highly contagious and spreads quickly in daycare and household settings.
- Prevention includes handwashing, avoiding exposure to sick contacts, palivizumab for high-risk infants.
Which precaution should a nurse caring for a 2-month-old infant with respiratory syncytial virus (RSV) take to prevent the spread of infection?
Explanation
Respiratory Syncytial Virus (RSV) is a highly contagious viral infection that causes bronchiolitis and pneumonia in infants and young children. It spreads through direct contact with respiratory secretions and droplet transmission. Therefore, the CDC recommends contact and droplet precautions to prevent spread in healthcare settings.
Rationale for correct answer:
2. RSV is transmitted by droplet and contact, so healthcare workers must use gloves, gowns, and masks when caring for infants. It protects against contaminated secretions during suctioning, feeding, or close contact.
Rationale for incorrect answers:
1. Gloves only is insufficient for RSV prevention. RSV spreads via large droplets and surfaces, requiring gown and mask in addition to gloves.
3. RSV is very contagious and is a major cause of hospitalization in infants during winter months.
4. Proper hand washing between clients is essential but not enough on its own. RSV requires contact and droplet precautions in addition to hand hygiene.
Take home points
- RSV prevention requires contact + droplet precautions including gown, gloves, and mask.
- RSV is highly contagious and spreads via secretions, droplets, and contaminated surfaces.
- Hand hygiene remains a critical component of infection control.
- Nurses should cohort RSV-infected infants when single rooms aren’t available.
The nurse teaches parents that the test used to diagnose respiratory syncytial virus (RSV) is:
Explanation
Respiratory syncytial virus (RSV) is a common viral infection that primarily affects infants and young children. It causes bronchiolitis and pneumonia, leading to symptoms such as cough, rhinorrhea, wheezing, fever, and respiratory distress.
Rationale for correct answer:
2. Nasopharyngeal washings is the most accurate and standard diagnostic test for RSV because it provides a specimen rich in respiratory secretions where the virus is present. This method collects secretions directly from the upper airway where the virus replicates which are then tested with antigen detection, PCR, or viral culture.
Rationale for incorrect answers:
1. Blood test is not diagnostic for RSV. Blood may show leukocytosis or other nonspecific findings but cannot confirm RSV.
3. Sputum culture is not reliable since young infants rarely produce sputum. Furthermore, sputum cultures are used for bacterial infections, not RSV.
4. Throat culture detects bacterial pathogens like streptococcus not RSV which requires nasopharyngeal washings for diagnosis.
Take home points
- RSV diagnosis requires nasopharyngeal swab/washings with antigen detection or PCR.
- RSV is the leading cause of bronchiolitis and pneumonia in infants.
- It is highly contagious, requiring strict hand hygiene and contact precautions.
- Diagnosis helps guide isolation and supportive management, since antibiotics are not effective.
Which child would be at increased risk for a respiratory syncytial virus (RSV) infection?
Explanation
Respiratory syncytial virus (RSV) is the leading cause of bronchiolitis and pneumonia in infants. Most healthy infants recover at home, but certain groups are at higher risk for severe disease and hospitalization.
Rationale for correct answer:
2. A 2-month-old child with bronchopulmonary dysplasia: Infants with chronic lung disease (BPD) have impaired airway clearance and reduced lung reserve, making them highly vulnerable to severe RSV infection.
Rationale for incorrect answers:
1. A 2-month-old child managed at home: While young age increases risk, a healthy infant at home is less vulnerable than one with BPD.
3. A 3-month-old child requiring low-flow oxygen: Oxygen dependence suggests chronic illness, but the greatest risk here is specifically linked to bronchopulmonary dysplasia or congenital heart disease.
4. A 2-year-old child: RSV risk decreases as children get older hence severe RSV is far less common after age 2.
Take home points
- High-risk infants such as premature, BPD, congenital heart disease, immunocompromised.
- These children may qualify for RSV prophylaxis with palivizumab (Synagis).
- RSV is usually mild in healthy older infants and toddlers but dangerous in vulnerable populations.
Which medication can help to prevent respiratory syncytial virus (RSV)?
Explanation
Prevention of respiratory syncytial virus (RSV) is especially important in high-risk infants such as the premature, those with bronchopulmonary dysplasia, or congenital heart disease, immunocompromised. They are not treatments for active infection but rather preventive therapies for high-risk infants.
Rationale for correct answer:
4. Respigam is an RSV immune globulin given IV monthly during RSV season to prevent infection in high-risk infants. It helps provide passive immunity. Palivizumab (Synagis), a monoclonal antibody, is also an immunoprophylactic agents used to help prevent RSV infection.
Rationale for incorrect answers:
1. Aminophylline is a bronchodilator used for asthma or apnea of prematurity, not for RSV prevention.
2. Bronchodilators may be used in treatment for wheezing but do not prevent RSV.
3. Corticosteroids are not effective for preventing or treating RSV. It may actually suppress immune response.
Take home points
- Respigam (RSV immune globulin) and palivizumab (Synagis) are used for RSV prevention in high-risk infants.
- These agents do not cure RSV but they only help reduce severity or risk of hospitalization.
- Standard prevention for all children includes handwashing, contact precautions, limiting exposure during RSV season.
Which intervention is most important when monitoring dehydration in an infant with bronchiolitis?
Explanation
Infants with bronchiolitis often caused by RSV are at risk for dehydration because they breathe rapidly increasing insensible fluid loss. They also have difficulty feeding due to respiratory distress and have fatigue and poor appetite limiting oral intake.
Rationale for correct answer:
1. Measurement of intake and output (I&O) is the most important intervention to detect dehydration early. Careful tracking of oral intake, IV fluids, urine, stool, and emesis provides a complete picture of hydration status.
Rationale for incorrect answers:
2. Blood levels every 4 hours are invasive and not necessary unless severe dehydration or electrolyte imbalance is suspected.
3. Urinalysis every 8 hours can detect concentration changes, but it is not a routine or practical method for monitoring hydration.
4. Weighing each diaper is part of I&O measurement, but on their own they don’t provide a full hydration picture.
Take home points
- I&O monitoring is the gold standard for assessing hydration in infants.
- Watch for clinical signs of dehydration: dry mucous membranes, sunken fontanel, poor skin turgor, decreased urine output.
- Supportive care for bronchiolitis includes hydration, oxygen if needed, and suctioning, not antibiotics since the disease is viral not bacterial.
Which nursing diagnosis is the priority for an infant with bronchiolitis?
Explanation
Bronchiolitis, most often caused by RSV, leads to inflammation, edema, and mucus plugging of the small airways (bronchioles). This results in air trapping, wheezing, and hypoxemia, making respiratory compromise the most immediate and life-threatening concern.
Rationale for correct answer:
3. Impaired gas exchange is the highest priority is ensuring adequate oxygenation and ventilation. Infants with bronchiolitis are at risk for hypoxia and respiratory failure, so monitoring oxygen saturation, respiratory effort, and breath sounds is critical.
Rationale for incorrect answers:
1. Imbalanced nutrition: More than body requirements is not inaccurate. Infants with bronchiolitis typically have decreased intake, not excess.
2. Deficient diversional activity is not a priority in acute illness hence safety and survival come first.
4. While isolation precautions are used for RSV, this is not the priority diagnosis compared to respiratory compromise.
Take home points
- Airway and breathing always come first in pediatric respiratory conditions.
- In bronchiolitis, the priority diagnosis is impaired gas exchange.
- Secondary concerns include fluid balance, nutrition, and infection control.
- Nursing interventions focus on: oxygen therapy, hydration, suctioning, and monitoring work of breathing.
Which teaching point is essential for parents caring for a child with bronchiolitis at home?
Explanation
Bronchiolitis, most commonly caused by RSV, is a viral lower respiratory infection in infants and young children. Most cases are mild and can be managed at home with supportive care, but severe respiratory distress can develop quickly, especially in infants. Teaching parents how to identify worsening symptoms is essential for timely medical care.
Rationale for correct answer:
3. Parents must be able to identify danger signs such as rapid breathing, nasal flaring, or retractions, grunting or wheezing that worsens, cyanosis or poor feeding, and lethargy or difficulty arousing
Early recognition allows prompt medical intervention and reduces the risk of respiratory failure.
Rationale for incorrect answers:
1. Placing the child in a prone position for comfort is incorrect. Infants should be placed supine for sleep to reduce SIDS risk.
2. Using warm mist to replace insensible fluid loss is not recommended since mist therapy does not prevent dehydration and may increase infection risk. Fluids should be given orally or IV if necessary.
4. Engaging the child in many activities to prevent developmental delay is not appropriate during acute illness. The child needs rest and supportive care.
Take home points
- Essential teaching: Parents must recognize signs of worsening respiratory distress.
- Home care including fluids, rest, fever management, nasal suctioning, and monitoring breathing.
- Prone sleeping and warm mist are unsafe/outdated practices.
- Seek emergency help if the child shows cyanosis, pauses in breathing, severe retractions, or poor feeding.
Practice Exercise 3
The nurse is teaching the parents of a child with pneumonia about the condition. Which description is correct?
Explanation
Pneumonia is an infection of the pulmonary parenchyma, including alveoli, alveolar ducts, and respiratory bronchioles. It can be caused by bacteria, viruses, fungi, or aspiration. The infection leads to inflammation, fluid or pus accumulation in alveoli, impaired gas exchange, cough, fever, and respiratory distress.
Rationale for correct answer:
3. Inflammation of the pulmonary parenchyma is the accurate definition of pneumonia. The alveoli and lung tissue become inflamed and filled with exudate, causing impaired oxygen exchange.
Rationale for incorrect answers:
1. Inflammation of the large airways refers to bronchitis, not pneumonia.
2. Severe infection of the bronchioles describes bronchiolitis, commonly caused by RSV, not pneumonia.
4. Acute viral infection with maximum effect at the bronchiolar level describes bronchiolitis, not pneumonia.
Take home points
- Pneumonia is an inflammation of pulmonary parenchyma (alveoli + lung tissue).
- Can be viral, bacterial, fungal, or aspiration-related.
- Hallmark signs: fever, cough, tachypnea, chest pain, crackles, decreased breath sounds.
- Treatment depends on cause: antibiotics for bacterial, supportive care for viral.
Which organism is the most common causative agent for bacterial pneumonia?
Explanation
Pneumonia is an infection of the pulmonary parenchyma, including alveoli, alveolar ducts, and respiratory bronchioles. It can be caused by bacteria, viruses, fungi, or aspiration. The infection leads to inflammation, fluid or pus accumulation in alveoli, impaired gas exchange, cough, fever, and respiratory distress. Pneumonia in children can be caused by different pathogens depending on age.
Rationale for correct answer:
3. Streptococcus pneumoniae is the leading cause of bacterial pneumonia in infants and young children. It causes lobar pneumonia, with symptoms such as fever, cough, chest pain, chills, tachypnea, and crackles on auscultation.
Rationale for incorrect answers:
1. Mycoplasma causes atypical pneumonia (“walking pneumonia”), more common in school-aged children and adolescents, not infants.
2. Parainfluenza virus causes viral respiratory infections like croup, not bacterial pneumonia.
4. Respiratory syncytial virus (RSV) is the leading cause of viral bronchiolitis, not bacterial pneumonia.
Take home points
- Streptococcus pneumoniae is the leading cause of bacterial pneumonia in children.
- Mycoplasma pneumoniae is common in older kids/adolescents resulting in atypical pneumonia.
- Viruses (RSV, parainfluenza, influenza) are more common overall in younger children but are causes of viral pneumonia, not bacterial.
The nurse is caring for an 8-year-old child admitted with pneumonia. Based on the child’s age, which type of pneumonia would the nurse suspect?
Explanation
Pneumonia is an infection of the pulmonary parenchyma, including alveoli, alveolar ducts, and respiratory bronchioles. It can be caused by bacteria, viruses, fungi, or aspiration. The infection leads to inflammation, fluid or pus accumulation in alveoli, impaired gas exchange, cough, fever, and respiratory distress. Pneumonia in children can be caused by different pathogens depending on age.
Rationale for correct answer:
2. Mycoplasma pneumonia is the most common pneumonia in school-age children (5–15 years old). It spreads by close contact such as in schools and camps. Symptoms often develop slowly and may mimic a viral infection at first.
Rationale for incorrect answers:
1. Enteric bacilli is a rare cause of pneumonia in healthy children; more common in hospital-acquired infections or immunocompromised clients.
3. Staphylococcal pneumonia can cause severe pneumonia but is less common and usually follows influenza or occurs in very young children and immunocompromised clients.
4. Streptococcal pneumonia is more common in infants, toddlers, and preschool children, not school-age children.
Take home points
- Age helps predict the causative organism in pediatric pneumonia.
- <5 years are more susceptible to viral or Streptococcus pneumoniae.
- ≥5 years (school-age, adolescents) are at increased risk to contract Mycoplasma pneumoniae (“walking pneumonia”).
- Knowing age-related pathogens helps guide empiric treatment before cultures return.
Which child diagnosed with pneumonia would benefit most from hospitalization?
Explanation
Pneumonia is an infection of the lungs that can cause cough, fever, tachypnea, chest pain, and respiratory distress. Children with pneumonia may be treated at home if stable, but hospitalization is indicated when unstable.
Rationale for correct answer:
3. A 15-year-old with vomiting for 3 days and fever cannot tolerate oral intake, putting them at risk for dehydration and electrolyte imbalance. Hospitalization is needed for IV fluids, supportive care, and close monitoring.
Rationale for incorrect answers:
1. A 13-year-old with cough, coarse breath sounds, and poor sleep has uncomfortable symptoms but manageable at home if hydration and oxygenation are adequate.
2. A 14-year-old with fever, tachypnea, and decreased appetite has mild to moderate pneumonia signs. However, if the child can still drink fluids, hospitalization is not required.
4. A 16-year-old with cough, chills, fever, and wheezing has symptoms that are concerning but manageable as an outpatient if oxygen saturation is stable and hydration is adequate.
Take home points
- Hospitalization in pneumonia is needed for:
- Poor oral intake or persistent vomiting → risk of dehydration.
- Significant respiratory distress or hypoxia.
- Infants or children with comorbidities.
- Outpatient care is possible for older, stable children with mild to moderate symptoms.
- Hydration status is as critical as respiratory status when determining the need for hospitalization.
Which position would be most comfortable for a child with left-sided pneumonia?
Explanation
Pneumonia is an infection of the lung tissue that causes inflammation, consolidation, and impaired gas exchange. It can cause symptoms such as can cause cough, fever, tachypnea, chest pain, and respiratory distress. Positioning can affect ventilation-perfusion (V/Q) matching and comfort.
Rationale for correct answer:
3. Since the pneumonia is on the left side, lying on the right side allows the unaffected lung to expand fully, improving oxygenation and comfort. It also reduces pressure on the inflamed left lung, decreasing pain and respiratory effort.
Rationale for incorrect answers:
1. Trendelenburg position places the head lower than the chest, increasing work of breathing and aspiration risk. Not appropriate in pneumonia.
2. Lying on the affected left side compresses the diseased lung, worsening oxygen exchange and increasing discomfort.
4. Supine position decreases lung expansion, may worsen ventilation, and increases risk of secretion pooling and hypoxemia.
Take home points
- In unilateral pneumonia, position with the unaffected lung down to maximize oxygen exchange.
- Comfort and oxygenation guide positioning decisions in respiratory conditions.
- Avoid supine or Trendelenburg in pneumonia because they impair ventilation and secretion clearance.
- General rule: “Good lung down” for improved perfusion and comfort.
A toddler was seen in the emergency department with respiratory distress and is admitted to the nursing unit with a diagnosis of pneumonia. The toddler is still short of breath and rubbing his eyes, as if he is sleepy. The mother wants to lay the client down, but he refuses. Which strategy should the nurse suggest that would be most effective in promoting rest?
Explanation
Pneumonia is a lung infection that causes inflammation, impaired gas exchange, cough, fever, and respiratory distress. In children, rest is essential for recovery, but positioning greatly impacts comfort and breathing.
Rationale for correct answer:
3. Allowing him to sleep in an upright position promotes better lung expansion, decreases respiratory effort, and makes breathing more comfortable. This is the most effective way to help a child with pneumonia rest while minimizing distress.
Rationale for incorrect answers:
1. Rocking the client until asleep may soothe temporarily but laying him flat worsens breathing effort, risking hypoxemia and discomfort.
2. Holding him in a supine position while he sleeps limits chest expansion and may increase airway obstruction or secretion pooling, making breathing harder.
4. Giving an over-the-counter sleeping pill is unsafe and inappropriate for children. Sedatives can depress respirations, worsening respiratory distress.
Take home points
- Positioning is crucial in managing pediatric pneumonia with respiratory distress.
- Upright or semi-upright positions improve comfort and oxygenation.
- Sedatives and forced supine positioning are contraindicated in children with respiratory illness.
- Nursing care should focus on comfort, oxygenation, and parental reassurance.
Practice Exercise 4
Which test is the definitive means of diagnosing tuberculosis (TB)?
Explanation
Pulmonary tuberculosis (TB) is a contagious bacterial infection that primarily affects the lungs, caused by Mycobacterium tuberculosis. It spreads through the air when someone with active TB coughs, sneezes, or speaks, releasing tiny droplets that others can inhale.
Rationale for correct answer:
2. The definitive diagnosis of tuberculosis (TB) is made by identifying Mycobacterium tuberculosis in a sputum sample, through sputum smear microscopy, culture, or nucleic acid amplification testing. Culture of M. tuberculosis is the gold standard, although it takes weeks. Rapid molecular tests are now also used.
Rationale for incorrect answers:
1. Chest X-ray can show infiltrates or cavities suggestive of TB but is not diagnostic since many lung diseases look similar.
3. Tuberculin test (Mantoux test/PPD) detects exposure to TB, not active disease. Cannot confirm TB because it may be positive with latent TB or BCG vaccination.
4. Urine culture is not useful for pulmonary TB diagnosis. It may detect TB in urinary tract TB, but not the standard test.
Take home points
- Definitive TB diagnosis is finding the organism in sputum.
- Tuberculin test is used for screening, not diagnostic.
- Chest X-ray is supportive evidence, not confirmatory.
- Culture and nucleic acid tests are the most accurate.
The nurse is assessing a child who has been admitted to the emergency department with a diagnosis of tuberculosis. Which symptom would the nurse expect to observe?
Explanation
Pulmonary tuberculosis (TB) is a contagious bacterial infection that primarily affects the lungs, caused by Mycobacterium tuberculosis. It spreads through the air when someone with active TB coughs, sneezes, or speaks, releasing tiny droplets that others can inhale.
Rationale for correct answer:
3. Enlarged, firm, and sometimes tender lymph nodes, especially in the neck, are a recognized manifestation of pediatric TB. This symptom reflects the body’s immune response to mycobacterial infection.
Rationale for incorrect answers:
1. Chills can occur in acute infections but are not a hallmark of TB, which has a more insidious onset with low-grade fever and night sweats.
2. Hyperactivity is not associated with TB. Children with TB are more likely to have fatigue, lethargy, or irritability due to chronic illness.
4. TB often causes weight loss or failure to thrive, not weight gain, due to chronic infection and poor appetite.
Take home points
- Lymphadenitis is a common pediatric TB manifestation, often with cervical lymph node enlargement.
- Children with TB often present with chronic cough, fever, weight loss, night sweats, and fatigue.
- Unlike acute infections, TB usually has an insidious, gradual onset.
- Nurses should recognize atypical pediatric presentations, as TB can be pulmonary or extrapulmonary.
Which adverse effect can be expected by the parents of a 2-year-old child who has been started on rifampin (Rifadin) after testing positive for tuberculosis?
Explanation
Pulmonary tuberculosis (TB) is a contagious bacterial infection that primarily affects the lungs, caused by Mycobacterium tuberculosis. It spreads through the air when someone with active TB coughs, sneezes, or speaks, releasing tiny droplets that others can inhale.
Rationale for correct answer:
2. Rifampin is a first-line antitubercular medication often prescribed as part of combination therapy. While effective, it has notable side effects that clients and caregivers must be educated about. One of the most expected and harmless effects is orange discoloration of body fluids such as urine, saliva, sweat, tears. It occurs due to the way the drug is metabolized and excreted.
Rationale for incorrect answers:
1. Hyperactivity is not a known or common adverse effect of rifampin. Behavioral changes are unrelated to the drug.
3. Rifampin can actually cause hepatotoxicity and increase liver enzymes or bilirubin, not decrease them.
4. Rifampin is hepatotoxic and may cause elevated, not decreased, liver enzymes. This requires monitoring but is not the expected everyday effect like orange secretions.
Take home points
- Rifampin causes orange discoloration of body fluids which is harmless but important to teach parents to avoid alarm.
- Hepatotoxicity is a serious adverse effect hence monitoring liver function (AST, ALT, bilirubin) is crucial.
- Parents should be instructed to avoid contact lenses due to the risk of staining.
An infection control nurse receives confirmation from a hospital laboratory that a client has sputum cultures positive for Mycobacterium tuberculosis. According to guidelines issued from the Centers for Disease Control and Prevention (CDC), this is a reportable disease. Which action should be taken by the nurse?
Explanation
Tuberculosis (TB) is a highly contagious disease caused by Mycobacterium tuberculosis. Because of its public health significance, TB is a nationally notifiable disease. Hospitals and providers are required by the CDC and local health departments to report confirmed cases.
Rationale for correct answer:
3. Implementing measures to notify the local or state health department of the case is correct since TB is a reportable disease in every U.S. state. The nurse must follow institutional and CDC guidelines by ensuring timely reporting to public health authorities. This enables contact investigation, follow-up testing, and treatment of exposed individuals.
Rationale for incorrect answers:
1. Issuing a press release to the local news agency violates HIPAA confidentiality and patient privacy. Public health notifications must go through official reporting systems, not the media.
2. Eliminating health-care workers who have negative tuberculin skin tests from caring for this client is incorrect. All healthcare workers, regardless of TB test status, must use airborne precautions such as N95 respirator or negative pressure room. Having a negative test does not disqualify a worker from providing care.
4. Notifying the nearest infectious disease facility and prepare to transfer the client so treatment can be initiated is appropriate. TB is treated in general hospitals and outpatient settings. Transfer is not required unless specialized care is needed. Treatment should begin at the current facility.
Take home points
- TB is a CDC-reportable disease: notify local/state health departments immediately.
- Maintain airborne precautions: negative pressure room, N95 respirators.
- Confidentiality is essential: reporting is done via official channels, not public disclosure.
- Public health measures (contact tracing, prophylaxis for exposed individuals) are crucial for controlling TB spread.
A nurse is planning care for a client being admitted with newly diagnosed active tuberculosis (TB) secondary to AIDS? Which intervention is most important for the nurse to plan?
Explanation
Pulmonary tuberculosis (TB) is a contagious bacterial infection that primarily affects the lungs, caused by Mycobacterium tuberculosis. It spreads through the air when someone with active TB coughs, sneezes, or speaks, releasing tiny droplets that others can inhale.
Rationale for correct answer:
3. Clients with active TB require airborne precautions such as placing them in a negative-pressure isolation room and cared for by staff using N95 respirators. This prevents transmission to healthcare workers and other clients. Infection control is always the first priority in TB management, even before diagnostic or supportive measures.
Rationale for incorrect answers:
1. Monitor for signs of bleeding is not directly associated with TB or AIDS unless the client is on anticoagulants or has another comorbidity. Not the immediate priority.
2. Teach strategies for skin care is important for some AIDS-related conditions (Kaposi sarcoma, fungal infections), but not the priority in a new active TB admission.
4. Assessing CD4 and T-lymphocyte counts is essential for managing HIV/AIDS, but not the immediate nursing priority compared to airborne precautions for TB infection control.
Take home points
- Airborne precautions such as negative pressure room or N95 respirator) are the top priority in active TB.
- AIDS increases risk of TB progression and poor outcomes, but the immediate focus is infection control to protect others.
- After isolation, additional care includes baseline labs (CD4, viral load, LFTs), TB medications, and supportive care.
- In TB + AIDS, nurses must always think ABCs + infection control as first-line priorities.
Comprehensive Questions
A parent asks the nurse how it will be determined whether their child has respiratory syncytial virus (RSV). Which is the nurse’s best response?
Explanation
Respiratory syncytial virus (RSV) is a common viral infection that primarily affects infants and young children. It causes bronchiolitis and pneumonia, leading to symptoms such as cough, rhinorrhea, wheezing, fever, and respiratory distress.
Rationale for correct answer:
3. Nasopharyngeal swab testing is the standard diagnostic method for RSV. A specimen is obtained from the nasal passages and tested for RSV antigens or genetic material. This is quick, non-invasive, and allows for accurate identification of the virus, guiding appropriate care and infection control.
Rationale for incorrect answers:
1. “We will do a simple blood test to determine whether your child has RSV” RSV is not diagnosed by blood testing. Blood work may show general infection markers, but it is not specific for RSV.
2. “There is no specific test for RSV. The diagnosis is made based on the child’s symptoms” There are reliable diagnostic tests such as antigen detection and PCR from nasal swabs.
4. “We will have to send a viral culture to an outside lab for testing” Viral cultures for RSV are possible but rarely used because they are time-consuming and not practical for rapid clinical decision-making.
Take home points
- RSV is the most common cause of bronchiolitis in infants and young children.
- Nasopharyngeal swab is the best method for confirming RSV.
- Rapid diagnostic testing guides isolation precautions and treatment.
- Supportive care such as oxygen, hydration, and suctioning is the mainstay of management, as there is no specific antiviral treatment for most cases.
Which statement indicates the parent needs further teaching on how to prevent his other children from contracting respiratory syncytial virus (RSV)?
Explanation
Respiratory syncytial virus (RSV) is a highly contagious viral infection that spreads through droplets and contact with contaminated surfaces. It can cause bronchiolitis or pneumonia, especially in infants and young children.
Rationale for correct answer:
1. Palivizumab injections are not indicated for healthy children. They are costly and reserved for select high-risk populations such as premature babies, children with congenital heart disease or chronic lung disease. A parent who believes both children should receive Synagis shows a misunderstanding of RSV prevention.
Rationale for incorrect answers:
2. Keeping the infected child away from siblings is correct and helps prevent transmission.
3. Handwashing is the most effective way to prevent RSV spread among household members.
4. Avoiding contact with sick individuals reduces the chance of introducing the virus into the home.
Take home points
- RSV spreads easily by direct contact and droplets.
- Hand hygiene and limiting exposure are the most effective prevention strategies.
- Palivizumab prophylaxis is used only in select high-risk infants, not routinely for all children.
- Education should focus on isolation, hygiene, and avoiding sick contacts rather than unnecessary medication use.
Which child is at highest risk for requiring hospitalization to treat respiratory syncytial virus (RSV)?
Explanation
Respiratory syncytial virus (RSV) is a highly contagious viral infection that spreads through droplets and contact with contaminated surfaces. It can cause bronchiolitis or pneumonia, especially in infants and young children.
Rationale for correct answer:
1. A 2-month-old who was born at 32 weeks: This child is at the highest risk because of both young age (under 6 months) and prematurity. These factors significantly increase the likelihood of severe respiratory distress, apnea, dehydration, and hospitalization.
Rationale for incorrect answers:
2. A 16-month-old with a tracheostomy: This child is vulnerable, but age >12 months reduces RSV severity risk. While tracheostomy care poses challenges, hospitalization risk is not as high as in very young premature infants.
3. A 3-year-old with a congenital heart defect: congenital heart disease increases risk, but at age 3, RSV is usually milder compared to the first year of life.
4. A 4-year-old who was born at 30 weeks: Past prematurity matters less after infancy. At age 4, lung and immune development are more mature, lowering the risk compared to a young premature infant.
Take home points
- The highest risk groups for RSV hospitalization:
- Premature infants (especially <35 weeks)
- Infants under 6 months of age
- Children with chronic lung disease or congenital heart disease
- Immunocompromised children
- Age is a critical factor, younger infants face more severe disease.
- Prevention for high-risk infants may include palivizumab (Synagis) during RSV season.
How will a child with respiratory distress and stridor who is diagnosed with RSV be treated?
Explanation
Respiratory syncytial virus (RSV) is a viral infection that causes bronchiolitis and can progress to lower respiratory tract involvement. In some cases, upper airway swelling may cause stridor and respiratory distress. Stridor indicates significant airway obstruction due to inflammation/edema.
Rationale for correct answer:
3. Nebulized racemic epinephrine directly reduces airway swelling and stridor, improving airflow and relieving distress. It is the best immediate treatment for children with RSV who develop upper airway compromise.
Rationale for incorrect answers:
1. Intravenous antibiotics are not indicated for RSV management since the disease is viral, not bacterial. Antibiotics are only indicated in case of a secondary bacterial infection.
2. Intravenous steroids are not recommended for routine RSV treatment since they have limited effectiveness in bronchiolitis.
4. Alternating acetaminophen and ibuprofen are used to treat fever and discomfort but do not address airway swelling, stridor, or respiratory distress.
Take home points
- RSV treatment is primarily supportive including oxygen, hydration, and suctioning.
- Nebulized racemic epinephrine is used when stridor or upper airway obstruction is present.
- Antibiotics and steroids are not routinely used in RSV.
- Fever control (acetaminophen/ibuprofen) may help comfort but does not treat airway compromise.
Which statement about pneumonia is accurate?
Explanation
Pneumonia is an infection of the lung parenchyma that can be caused by bacteria, viruses, fungi, or other organisms. It causes the alveoli to become inflamed and fill with pus and fluid, making it difficult and painful to breath.
Rationale for correct answer:
2. Children with bacterial pneumonia are usually sicker than children with viral pneumonia.
Bacterial pneumonia often presents with abrupt onset, high fever, productive cough, chest pain, and more severe clinical findings compared to viral pneumonia, which typically develops gradually with cough, low-grade fever, and diffuse infiltrates on imaging. Symptoms of viral pneumonia are often milder and self-limiting.
Rationale for incorrect answers:
1. “Pneumonia is most frequently caused by bacterial agents.” This is incorrect since in children, viral causes are more common, especially RSV, influenza, parainfluenza, and adenovirus.
3. “Children with viral pneumonia are usually sicker than children with bacterial pneumonia.” Viral pneumonia tends to be less severe with symptoms being milder and self-limiting unlike bacterial pneumonia which requires treatment with antibiotics.
4. “Children with viral pneumonia must be treated with a complete course of antibiotics.” Antibiotics are not effective against viruses and are not indicated for viral pneumonia. Management of viral pneumonia is supportive with oxygen, antipyretics, and adequate hydration.
Take home points
- Viral pneumonia is more common in children than bacterial pneumonia.
- Bacterial pneumonia is typically more severe, with higher fevers and sicker presentations.
- Viral pneumonia is managed with supportive care, not antibiotics.
- Correct differentiation between viral and bacterial pneumonia guides treatment and prevents unnecessary antibiotic use.
A nurse monitoring a preterm baby with RSV bronchiolitis notes that the baby is exhibiting signs of respiratory distress. Which of the following signs did the nurse observe? Select all that apply
Explanation
RSV bronchiolitis in preterm infants is dangerous because their smaller, underdeveloped airways and limited lung capacity make them more prone to respiratory distress and failure. Nurses must be able to recognize early and late signs of distress to intervene promptly.
Rationale for correct answers:
2. Tachypnea, rapid breathing, is one of the first signs of respiratory distress, reflecting increased effort to compensate for hypoxemia.
3. Nasal flaring is a classic sign of infant respiratory distress. It indicates increased work of breathing as the infant attempts to draw in more air.
4. Expiratory grunting is a compensatory mechanism to keep alveoli open and improve oxygenation. It signals significant distress and impending respiratory failure if unresolved.
5. Intercostal retractions occur when the infant uses accessory muscles to breathe due to increased airway resistance and difficulty moving air.
Rationale for incorrect answer:
1. Huffing is not a recognized clinical sign of infant respiratory distress. The key signs are tachypnea, nasal flaring, grunting, and retractions.
Take home points
- Early signs of respiratory distress: tachypnea, nasal flaring, retractions.
- Worsening signs: expiratory grunting, cyanosis, apnea.
- Immediate priorities: maintain airway (suction), provide oxygen, and anticipate respiratory failure.
- Preterm infants are at higher risk of rapid deterioration and must be closely monitored.
Which goal should a nurse deem as essential when caring for a 14-month-old infant with bronchiolitis?
Explanation
Bronchiolitis, most often caused by Respiratory Syncytial Virus (RSV), leads to inflammation, increased mucus production, and airway obstruction in infants and toddlers. Because infants breathe faster and have copious secretions, they are at risk of dehydration from poor oral intake, fever, and insensible fluid loss from tachypnea.
Rationale for correct answer:
1. Promoting and maintaining adequate hydration is the essential goal because hydration keeps mucus secretions thin and prevents further respiratory compromise. Infants with bronchiolitis often cannot feed well due to difficulty coordinating sucking, swallowing, and breathing. Ensuring adequate hydration is both therapeutic and preventive for complications.
Rationale for incorrect answers:
2. Setting up and facilitating the use of a mist tents are largely outdated and not considered effective. Supportive care with humidified oxygen and suctioning is preferred.
3. Bronchiolitis is caused by a virus (RSV), so antibiotics are not appropriate unless there is a confirmed secondary bacterial infection.
4. Providing a cough suppressant as necessary is contraindicated in infants and toddlers. Coughing is a protective mechanism that helps clear secretions. Suppressing it may worsen obstruction.
Take home points
- Hydration is the top nursing goal in bronchiolitis to thin secretions and prevent worsening distress.
- Supportive care including hydration, oxygen, and suctioning is the mainstay; antibiotics and cough suppressants are not indicated.
- Infants should be closely monitored for respiratory failure signs such as apnea, cyanosis, grunting, and retractions.
A child with severe cerebral palsy is admitted to the hospital with aspiration pneumonia. What is the most beneficial educational information that the nurse can provide to the parents?
Explanation
Aspiration pneumonia occurs when food, liquids, or secretions are inhaled into the lungs, leading to infection. Children with severe cerebral palsy are at increased risk because of poor swallowing coordination, weak cough reflex, and impaired mobility. Aspiration can be recurrent and life-threatening.
Rationale for correct answer:
4. Teaching parents strategies to prevent aspiration such as upright positioning during and after feeding, using thickened feeds if prescribed, proper suctioning techniques, and feeding modifications provides the greatest long-term benefit. This empowers parents to reduce future episodes and complications.
Rationale for incorrect answers:
1. Education on signs and symptoms of aspiration pneumonia is helpful but reactive. By the time symptoms appear, pneumonia has already developed hence education on the prevention strategies is most beneficial.
2. Education on the treatment plan for aspiration pneumonia is important for current management, but it does not reduce the risk of recurrence.
3. Education on the risks associated with recurrent aspiration pneumonia is educational but not as useful as teaching practical prevention strategies that address the root cause.
Take home points
- Children with cerebral palsy are at high risk for aspiration pneumonia due to swallowing and airway protection difficulties.
- Prevention is the priority and includes upright positioning, careful feeding techniques, and possible use of feeding modifications (e.g., gastrostomy).
- Education should empower parents to reduce recurrence rather than only focusing on recognition or treatment.
- Preventing aspiration leads to fewer hospitalizations, improved quality of life, and better outcomes.
The mother of an infant diagnosed with bronchiolitis asks the nurse what causes this disease. The nurse’s response would be based on the knowledge of which cause of the majority of infections leading to bronchiolitis?
Explanation
Bronchiolitis is a lower respiratory tract infection that primarily affects infants and young children. It causes inflammation, edema, and mucus plugging of the small airways (bronchioles), leading to wheezing, crackles, respiratory distress, and hypoxemia.
Rationale for correct answer:
3. The most common cause of bronchiolitis is respiratory syncytial virus (RSV). RSV is highly contagious and the leading cause of bronchiolitis in infants under 2 years. Outbreaks often occur in winter and early spring, and infection may range from mild cold-like symptoms to severe respiratory distress requiring hospitalization.
Rationale for incorrect answers:
1. Klebsiella infection is a bacterial pathogen, not the usual cause of bronchiolitis. It is more associated with severe bacterial pneumonia.
2. Mycoplasma pneumoniae is an atypical bacterial that causes pneumonia in older children and adolescents, not bronchiolitis in infants.
4. Haemophilus influenzae is a bacterial pathogen associated with epiglottitis and pneumonia, not bronchiolitis.
Take home points
- RSV is the leading cause of bronchiolitis in infants and young children.
- Bronchiolitis is viral, so antibiotics are not effective.
- Supportive care including oxygen, fluids, and suctioning is the mainstay of treatment.
- Prevention includes hand hygiene, avoiding sick contacts, and palivizumab prophylaxis for high-risk infants (e.g., premature, chronic lung disease, congenital heart disease).
A nurse is preparing to admit a client with a confirmed case of tuberculosis. Which action is essential to infection control for this client?
Explanation
Tuberculosis (TB) spreads through airborne transmission by inhaling droplet nuclei that remain suspended in the air for long periods. Infection control measures are essential to protect healthcare workers and visitors. The CDC recommends airborne precautions for all clients with confirmed or suspected TB.
Rationale for correct answer:
3. Using a NIOSH-approved N95 respirator mask is essential because TB is an airborne pathogen. Surgical masks are not sufficient to filter droplet nuclei. Visitors and staff must wear an N95 (or higher-level respirator) whenever entering the client’s room.
Rationale for incorrect answers:
1. Providing a positive-pressure airflow room is incorrect. TB requires a negative-pressure room, which prevents contaminated air from escaping into hallways. Positive pressure would spread the infection.
2. Wearing gown and gloves when handling the client’s stool or urine is incorrect since TB is not spread via stool or urine. Standard precautions apply, but the key infection control focus is airborne transmission.
4. Initiating antibiotic therapy is important, but precautions must begin immediately upon admission, not delayed until after medication is started. The client should remain in airborne isolation until considered noninfectious, usually after several weeks of effective therapy and negative sputum smears.
Take home points
- Airborne precautions including a negative-pressure room + N95 respirators are essential for TB.
- TB spreads through inhalation of airborne particles, not by contact with body fluids.
- Isolation continues until the client is deemed noninfectious after 3 consecutive negative sputum smears.
- Nurses must prioritize infection control to protect others before initiating additional interventions.
An infant is being admitted to the pediatric unit with respiratory syncytial virus infection at change of shift. The charge nurse could appropriately assign which other children to the nurse who will be admitting this infant? Select all that apply
Explanation
Respiratory syncytial virus (RSV) is a highly contagious viral infection that spreads through droplets and contact with contaminated surfaces. It can cause bronchiolitis or pneumonia, especially in infants and young children. Strict hand hygiene and infection-control precautions are essential in RSV care.
Rationale for correct answers:
2. A school-aged client with a fractured femur in traction has a noninfectious condition and is not immunocompromised, so it is safe for the same nurse to care for them along with the RSV infant.
4. Although impetigo is contagious, it is a bacterial skin infection, not a respiratory or droplet-spread illness like RSV. With contact precautions, the same nurse can safely care for both clients.
Rationale for incorrect answers:
1. A toddler with neuroblastoma on chemotherapy is immunocompromised and is at very high risk if exposed to RSV. Should not be assigned to the same nurse.
3. An infant with immunodeficiency is immunosuppressed hence highly vulnerable to RSV and must not share care assignments with an RSV patient.
5. A toddler with aplastic anemia is immunocompromised and is at a very high risk for severe RSV complications. The child should not be cohorted with a child with RSV.
Take home points
- RSV is highly contagious hence nurses must avoid assigning immunocompromised clients with RSV patients.
- Safe to assign RSV alongside noninfectious conditions or non-respiratory infectious conditions.
- Immunosuppressed children such as those undergoing chemotherapy, with immunodeficiency, or aplastic anemia, require strict protection from RSV exposure.
- Nursing assignments must always consider both infection control and client vulnerability.
A pre-school client with bacterial pneumonia is crying and says it hurts when he coughs. Which instruction should the nurse give to the child?
Explanation
Bacterial pneumonia in children causes inflammation of the lungs, leading to fever, cough, chest pain, and respiratory distress. Coughing is necessary to clear secretions and maintain airway patency, but it can be painful. Nurses should teach splinting techniques to reduce chest pain while allowing effective coughing.
Rationale for correct answer:
1. Hugging his teddy bear when he coughs is a form of splinting. Holding something against the chest provides support, reduces pain, and makes coughing more tolerable, while still promoting secretion clearance. It is developmentally appropriate for a preschooler.
Rationale for incorrect answers:
2. Asking for pain medicine before he coughs may help overall discomfort but are not practical for each coughing episode. Pain medication should not be timed specifically before coughing.
3. Taking a sip of water before coughing may help soothe the throat but do not relieve chest pain associated with pneumonia-related coughing.
4. Trying very hard not to cough is unsafe. Coughing is essential to clear secretions and prevent worsening infection or atelectasis. Suppressing cough could cause complications.
Take home points
- Splinting such as hugging a pillow or teddy bear reduces chest pain while allowing effective coughing.
- Children should be encouraged to cough and deep breathe to clear secretions, not suppress cough.
- Pain control is important but must not interfere with airway clearance.
- Teaching strategies should be age-appropriate and comforting such as a teddy bear for preschoolers.
What is the best position for a nurse to place a 3-year-old child with right lower lobe pneumonia?
Explanation
Pneumonia is an infection of the lung tissue that causes inflammation, consolidation, and impaired gas exchange. It can cause symptoms such as can cause cough, fever, tachypnea, chest pain, and respiratory distress. Positioning can affect ventilation-perfusion (V/Q) matching and comfort.
Rationale for correct answer:
2. Placing the child on the left side, which is the unaffected lung down allows for optimal ventilation and perfusion. This maximizes oxygen exchange and eases breathing effort.
Rationale for incorrect answers:
1. Placing the child on the right side places the diseased lung down, impairing oxygenation because blood flow is directed to poorly ventilated lung tissue.
3. Supine position can compromise lung expansion, increase risk of pooling secretions, and make breathing more difficult in pneumonia.
4. While prone positioning may help in severe ARDS, it is not the best choice for unilateral pneumonia in a 3-year-old child. It may also be uncomfortable and unsafe.
Take home points
- In unilateral pneumonia, place the unaffected lung down to optimize gas exchange.
- Positioning improves comfort, oxygenation, and secretion clearance.
- Supine or prone positions are less effective and may worsen respiratory distress in children.
A nurse is explaining bronchiolitis to the parents of an infant admitted with the condition. Which explanation by the nurse would be the most accurate?
Explanation
Bronchiolitis is a lower respiratory tract infection, most often caused by respiratory syncytial virus (RSV). It results in symptoms such as cough, rhinorrhea, wheezing, fever, and respiratory distress.
Rationale for correct answer:
1. Acute inflammation and obstruction of the bronchioles is the hallmark of bronchiolitis. The small bronchioles become swollen and filled with mucus, which impedes airflow, especially during expiration.
Rationale for incorrect answers:
2. Airway obstruction from aspiration of a solid object describes foreign body aspiration, not bronchiolitis.
3. Inflammation of the pulmonary parenchyma refers to pneumonia, not bronchiolitis.
4. Acute highly contagious croup-like syndrome refers to croup (laryngotracheobronchitis), which involves the upper airway, not the bronchioles.
Take home points
- Bronchiolitis refers to lower airway inflammation and obstruction of bronchioles.
- Usually caused by RSV and seen in infants and toddlers.
- Presents with wheezing, cough, nasal flaring, and retractions.
- Management is largely supportive: oxygen, hydration, suctioning, and sometimes bronchodilators.
A 2-month-old infant is brought to the emergency department and a preliminary diagnosis of bronchiolitis is given. Which symptom should a nurse expect to find on assessment?
Explanation
Bronchiolitis is a common viral lung infection that primarily affects infants and young children, especially those under 2 years old. It targets the bronchioles, which are the smallest airways in the lungs, causing them to become swollen, irritated, and clogged with mucus, making it hard to breathe.
Rationale for correct answer:
3. Wheezing on auscultation is the classic finding in bronchiolitis due to narrowing and obstruction of the bronchioles. Other common signs include tachypnea, nasal flaring, retractions, and cough.
Rationale for incorrect answers:
1. Infants with bronchiolitis usually present with tachycardia due to fever, hypoxia, or distress. Bradycardia is a late, pre-arrest sign of severe hypoxia.
2. Infants typically have a decreased appetite/poor feeding due to respiratory distress and fatigue.
4. Bronchiolitis usually begins with nasal congestion, rhinorrhea, and cough, which are signs of an upper respiratory infection before progressing to lower airway involvement.
Take home points
- Wheezing is the hallmark finding in bronchiolitis.
- Bronchiolitis typically follows upper respiratory symptoms such as runny nose and cough.
- Watching for respiratory distress signs such as tachypnea, nasal flaring, retractions, and hypoxia.
- Infants may have poor feeding due to difficulty coordinating breathing and sucking.
Exams on Lower Respiratory Tract Infections
Custom Exams
Login to Create a Quiz
Click here to loginLessons
 Naxlex
Just Now
Naxlex
Just Now
Notes Highlighting is available once you sign in. Login Here.
Objectives
- Understand the common lower respiratory tract infections (LRTIs) in children.
- Differentiate between bronchitis, bronchiolitis, pneumonia, and pulmonary tuberculosis based on clinical presentation and pathophysiology.
- Identify appropriate diagnostic evaluations for each condition.
- Describe therapeutic management strategies, including pharmacologic and supportive care.
- Recognize key nursing care interventions and patient education for each LRTI.
- Discuss preventive measures, including immunizations and prophylactic medications.
- Identify potential complications associated with these infections.
Introduction
- Lower respiratory tract infections (LRTIs) are a significant cause of morbidity and mortality in the pediatric population worldwide.
- These infections affect the airways below the larynx, including the trachea, bronchi, bronchioles, and alveoli.
- Children are particularly vulnerable due to their smaller airway size, immature immune systems, and higher respiratory rates, making them more susceptible to obstruction and respiratory distress.
- Infections in this region can range from mild and self-limiting to severe and life-threatening, particularly in vulnerable populations such as infants and immunocompromised individuals.
- Understanding these conditions is crucial for effective nursing care and improved outcomes.
- Always remember that a child's respiratory status can deteriorate rapidly. Early recognition of signs of respiratory distress is paramount.
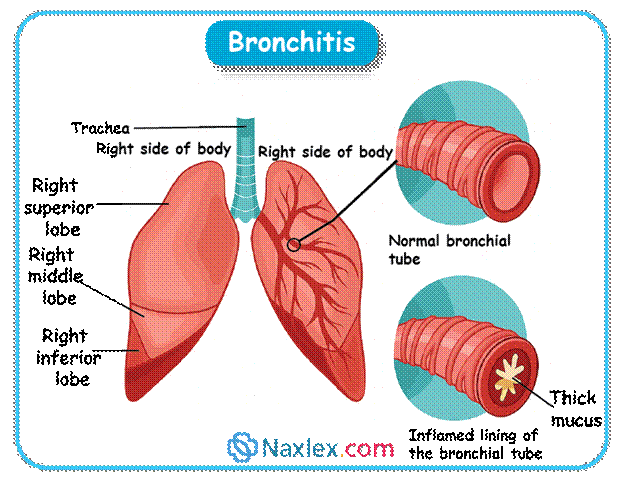
Bronchitis
- Bronchitis is an inflammation of the large airways (bronchi), characterized by a cough. While often benign and self-limiting, it can be distressing for both the child and parents.
Incidence:
- Acute bronchitis is very common in children, typically occurring during colder months.
- Often follows a viral upper respiratory tract infection (URTI).
- Less common in infants than in older children and adolescents.
Pathophysiology:
- The primary event is inflammation and irritation of the bronchial lining.
- This leads to increased mucus production and swelling of the bronchial walls.
- The inflamed airways narrow, making it difficult to clear secretions and leading to coughing.
- Bronchospasm can sometimes occur.
Etiology:
- Viruses: The most common cause (e.g., influenza virus, parainfluenza virus, respiratory syncytial virus (RSV), adenovirus, rhinovirus).
- Bacteria: Less common, but can include Mycoplasma pneumoniae and Bordetella pertussis (whooping cough).
- Irritants: Exposure to smoke, pollutants, or allergens can also cause or exacerbate bronchitis.
Clinical Manifestations:
- Persistent cough: This is the hallmark symptom, often dry and hacking initially, progressing to productive with sputum (clear, yellow, or green). Can last for 1-3 weeks.
- Sore throat, runny nose, fatigue: Often precede the cough, as bronchitis frequently follows a URI.
- Low-grade fever: May or may not be present.
- Chest discomfort or soreness: From persistent coughing.
- Wheezing or rhonchi: May be heard on auscultation, indicating airway narrowing and secretions.
Diagnostic Evaluation:
- Clinical diagnosis: Primarily based on history and physical examination.
- Chest X-ray: Usually normal; typically not needed unless pneumonia is suspected (e.g., persistent fever, focal lung sounds).
- Sputum culture: Rarely indicated unless a bacterial cause is strongly suspected.
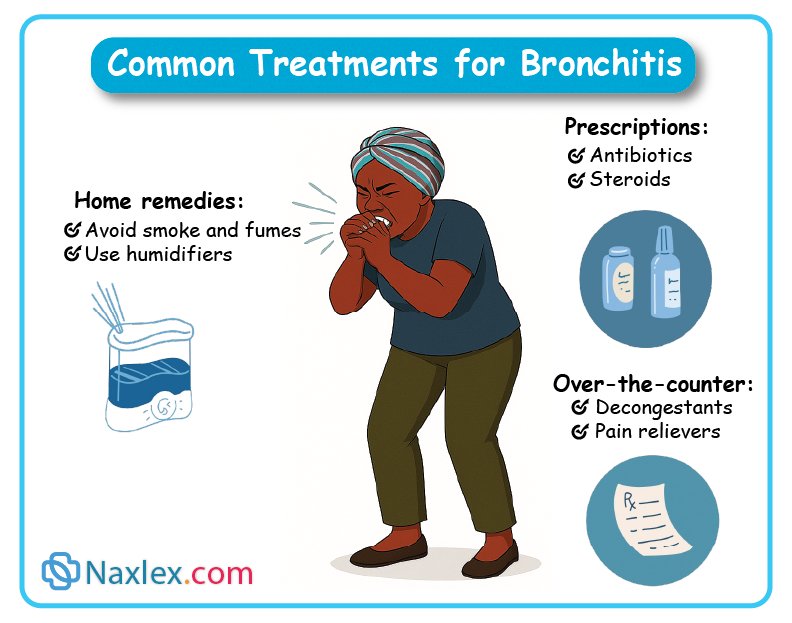
Therapeutic Management:
- Supportive care: The cornerstone of treatment as most cases are viral.
- Hydration: Encourage oral fluids to thin secretions.
- Rest: Important for recovery.
- Humidity: Cool-mist humidifier can help soothe irritated airways and loosen secretions.
- Antipyretics/Analgesics: Acetaminophen or ibuprofen for fever and discomfort.
- Cough suppressants/expectorants: Generally not recommended for children, especially under 6 years old, as they are often ineffective and can have side effects. Coughing is important for clearing secretions.
- Antibiotics: Only prescribed if a bacterial infection is confirmed or strongly suspected (e.g., Mycoplasma pneumoniae).
- Bronchodilators: May be used if significant wheezing or bronchospasm is present.
Prevention:
- Hand hygiene: Frequent hand washing to prevent spread of viral infections.
- Avoidance of irritants: Protect children from secondhand smoke and other air pollutants.
- Vaccinations: Annual influenza vaccine can prevent influenza-related bronchitis.
Nursing Care Management:
- Assess respiratory status: Monitor cough characteristics, respiratory rate, effort, oxygen saturation, and lung sounds.
- Promote comfort: Elevate head of bed, encourage rest, offer warm fluids.
- Hydration: Teach parents the importance of adequate fluid intake.
- Education:
- Explain the viral nature of most bronchitis cases and the limited role of antibiotics.
- Advise against over-the-counter cough and cold medications for young children.
- Educate on signs of worsening condition (e.g., difficulty breathing, high fever, signs of dehydration) and when to seek medical attention.
- Infection control: Emphasize hand hygiene to prevent spread within the family.
Nursing Insight: Differentiating bronchitis from bronchiolitis in very young children can be challenging. Bronchiolitis often presents with more pronounced respiratory distress and wheezing.
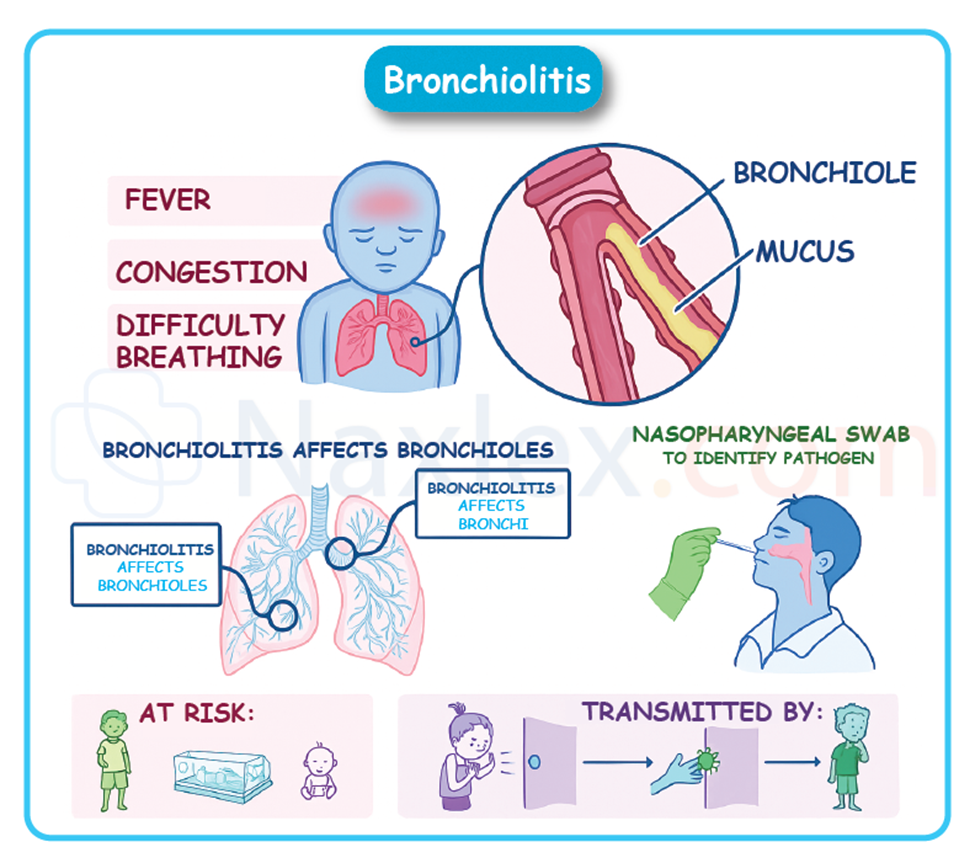
Respiratory Syncytial Virus And Bronchiolitis
Bronchiolitis is an acute inflammatory illness of the small airways (bronchioles), most commonly caused by Respiratory Syncytial Virus (RSV). It is the leading cause of hospitalization for infants in the United States.
Incidence:
- Most common in infants and young children, typically under 2 years of age.
- Peak incidence during winter and early spring months.
- Almost all children are infected with RSV by age 2.
- Risk factors for severe disease: prematurity, congenital heart disease, chronic lung disease, immunodeficiency, male gender, exposure to secondhand smoke.
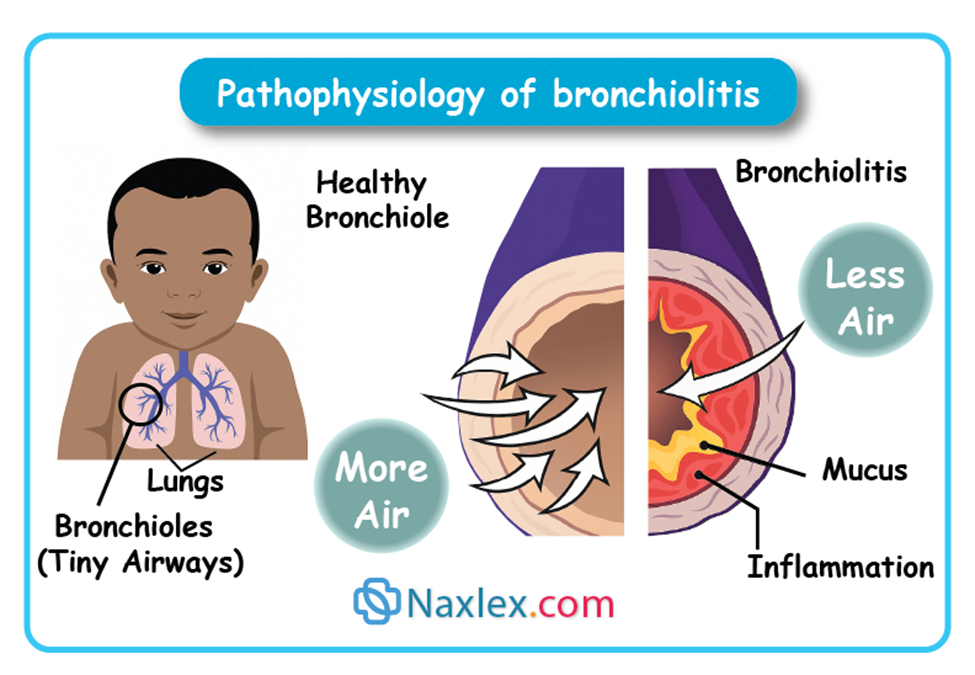
Pathophysiology:
- RSV infects the epithelial cells of the small airways, causing necrosis and sloughing.
- This leads to edema, increased mucus production, and bronchospasm.
- The narrowed bronchioles trap air (air trapping) and interfere with gas exchange.
- Inflammation also impairs ciliary function, making it harder to clear secretions.
- The small size of infant airways makes them highly susceptible to obstruction.
Etiology/Various Causes per Age:
- RSV: Accounts for 50-80% of bronchiolitis cases.
- Other viruses: Human metapneumovirus, parainfluenza virus, adenovirus, influenza virus, rhinovirus.
- Bacterial co-infection is rare but can occur.
Clinical Manifestations:
- Initial: Upper respiratory symptoms (rhinorrhea, sneezing, low-grade fever, cough) for several days.
- Progressive respiratory distress:
- Tachypnea: Rapid breathing.
- Wheezing: High-pitched whistling sound on expiration, often diffuse.
- Crackles: Heard on auscultation.
- Retractions: Subcostal, intercostal, suprasternal, supraclavicular.
- Nasal flaring: Widening of nostrils with inspiration.
- Grunting: Short, low-pitched sound on expiration, indicating effort to keep alveoli open.
- Cough: Persistent, often paroxysmal.
- Irritability/Lethargy: Due to hypoxemia.
- Poor feeding: Due to respiratory effort.
- Apnea: Can be the presenting symptom in very young infants (especially <1-2 months) and premature infants.
- Cyanosis: A late and ominous sign.
Diagnostic Evaluation:
- Clinical diagnosis: Primarily based on history and physical examination.
- Rapid RSV test: Nasal aspirate or swab can confirm RSV infection but usually doesn't change management.
- Chest X-ray: May show hyperinflation, atelectasis, or peribronchial thickening, but often not necessary unless complications like pneumonia are suspected.
- Pulse oximetry: Essential to monitor oxygen saturation.
Therapeutic Management:
- Supportive care: No specific antiviral treatment for RSV is routinely recommended.
- Oxygen therapy: To maintain SpO2 >90-92% (target may vary).
- Hydration: Oral fluids if tolerated, otherwise IV fluids.
- Nasal suctioning: Crucial for infants to clear thick secretions, especially before feeds.
- Antipyretics: For fever.
- Medications (controversial/limited efficacy):
- Bronchodilators (e.g., albuterol): May be used for a trial if wheezing is significant, but often show limited benefit in RSV bronchiolitis. If no response, discontinue.
- Corticosteroids: Not routinely recommended.
- Ribavirin: Antiviral agent, rarely used due to questionable efficacy, side effects, and cost; considered only for severely immunocompromised children or those with specific underlying conditions.
- Hypertonic saline nebulization: Some evidence suggests it may reduce hospital stay, but not universally adopted.
Prevention (Prophylactic Medications):
- Hand hygiene: Most effective method to prevent spread.
- Palivizumab (Synagis):
- Type: Monoclonal antibody.
- Administration: Given monthly IM injections during RSV season (typically October-March).
- Target population: High-risk infants, including:
- Infants born ≤29 weeks 0 days gestation during their first RSV season.
- Infants with hemodynamically significant congenital heart disease.
- Infants with chronic lung disease of prematurity (bronchopulmonary dysplasia) requiring medical support (e.g., oxygen, diuretics, bronchodilators) within 6 months of RSV season start, for their first two RSV seasons.
- Severe immunodeficiency.
- Mechanism: Provides passive immunity against RSV.
- RSV Immunoglobulin (RespiGam):
- Type: Polyclonal antibody derived from human plasma.
- Administration: IV.
- Note: Palivizumab has largely replaced RespiGam due to its easier administration (IM vs. IV) and improved safety profile. RespiGam is rarely used today.
Nursing Care Management:
- Respiratory assessment: Frequent monitoring of respiratory rate, effort, oxygen saturation, heart rate, and lung sounds. Recognize early signs of decompensation.
- Airway management:
- Nasal suctioning: Teach parents proper technique. Bulb syringe for home, nasal aspirator/catheter for hospital.
- Humidified oxygen: As ordered, using appropriate delivery device (nasal cannula, hood, mask).
- Positioning:
- Semi-Fowler's: Elevate head of bed to promote lung expansion.
- Unilateral pneumonia (less common with pure bronchiolitis, but important if co-occurring): If a child has unilateral pneumonia, positioning the child with the unaffected lung down can sometimes improve ventilation-perfusion matching, as the good lung receives more blood flow. However, in children, position of comfort and ability to breathe effectively often takes precedence. Always prioritize open airway and comfort.
- Hydration and nutrition: Encourage small, frequent feeds if able; IV fluids if respiratory distress interferes with oral intake.
- Infection control: Strict hand hygiene, contact precautions (gown, gloves). Cohorting of RSV patients.
- Rest and comfort: Minimize disturbances, cluster care.
- Education:
- Signs of worsening respiratory distress.
- Importance of suctioning and hydration.
- Prevention strategies (hand hygiene, avoiding sick contacts, no smoking).
- Discuss palivizumab if indicated.
Complications:
- Apnea (especially in infants <2 months).
- Respiratory failure requiring mechanical ventilation.
- Dehydration.
- Secondary bacterial pneumonia.
- Otitis media.
- Persistent reactive airway disease/wheezing (some link between severe RSV and later asthma).
Nursing Insight: Infants with RSV can quickly become exhausted from the effort of breathing. Watch for decreasing respiratory rate and effort after a period of tachypnea, as this can be a sign of impending respiratory failure, not improvement.
Pneumonia
Pneumonia is an acute inflammation of the lung parenchyma (alveoli and bronchioles), leading to impaired gas exchange. It can be bacterial, viral, or less commonly, fungal.
Incidence:
- Common in pediatric populations globally, especially in developing countries.
- Second most common infectious disease causing death in children under 5 years worldwide.
- Incidence varies with age, season, and vaccination status.
Pathophysiology:
- Pathogen invades the lower respiratory tract, typically via aspiration or inhalation.
- Triggers an inflammatory response in the alveoli.
- Fluid, pus, and cellular debris accumulate in the alveolar spaces, consolidating lung tissue.
- This impairs oxygen diffusion across the alveolar-capillary membrane, leading to hypoxemia.
- The affected lung tissue becomes less compliant, increasing the work of breathing.
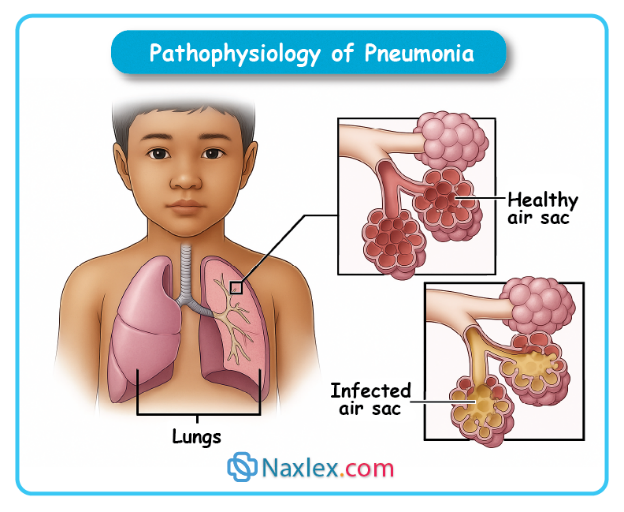
Etiology:
- Viral (most common in infants and young children): RSV, parainfluenza, influenza, adenovirus, metapneumovirus. Often presents milder.
- Bacterial (more common in older children, typically more severe):
- Streptococcus pneumoniae (Pneumococcus) - most common bacterial cause.
- Haemophilus influenzae type b (Hib) - significantly reduced due to vaccination.
- Mycoplasma pneumoniae - "walking pneumonia," common in school-aged children and adolescents.
- Staphylococcus aureus - can cause severe, necrotizing pneumonia.
- Chlamydia trachomatis - typically in infants 1-3 months of age, acquired perinatally.
- Fungal/Aspiration: Less common in healthy children.
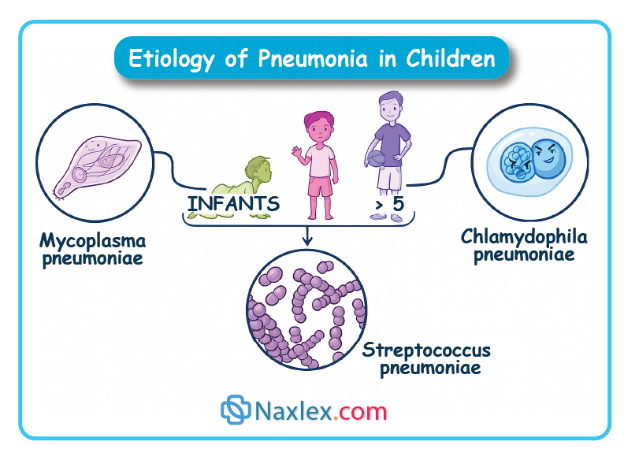
Clinical Manifestations:
- Fever: Often high in bacterial pneumonia.
- Cough: May be dry, hacking, or productive with sputum (purulent in bacterial, clear in viral).
- Tachypnea: Rapid breathing is a key sign in children.
- Increased work of breathing: Nasal flaring, retractions, grunting.
- Crackles/rales: Heard over affected lung fields.
- Diminished breath sounds: Over consolidated areas.
- Dullness to percussion: Over consolidated areas.
- Chest pain: Especially with pleuritic involvement.
- Abdominal pain: Can be referred pain from diaphragmatic irritation, especially in lower lobe pneumonia.
- Malaise, fatigue, poor feeding.
- Infants: May present with irritability, lethargy, poor feeding, apnea, or minimal cough.
Diagnostic Evaluation:
- Clinical suspicion: Based on signs and symptoms.
- Chest X-ray: Confirms diagnosis, identifies location (lobar, interstitial, patchy), and can differentiate between bacterial (lobar consolidation) and viral (diffuse interstitial infiltrates, hyperinflation) patterns.
- Pulse oximetry: To assess oxygenation.
- Blood cultures: May be positive in bacterial pneumonia, especially if severe, but often low yield.
- CBC with differential: May show elevated WBC count in bacterial infection.
- Sputum culture/nasopharyngeal aspirate: To identify specific pathogen, especially if severe or not responding to initial treatment.
- Rapid antigen tests: For influenza, RSV, etc.
Therapeutic Management:
- Bacterial pneumonia:
- Antibiotics: Oral for mild cases (e.g., amoxicillin for suspected S. pneumoniae). IV for severe cases or those requiring hospitalization (e.g., ceftriaxone, cefotaxime). Duration typically 7-10 days, or longer for atypical pathogens (Mycoplasma – azithromycin).
- Viral pneumonia:
- Supportive care: Oxygen, hydration, fever management.
- Antivirals (e.g., oseltamivir for influenza) may be used if appropriate.
- General supportive care:
- Oxygen therapy: If SpO2 <90-92%.
- Hydration: Oral or IV.
- Antipyretics: For fever and discomfort.
- Chest physiotherapy: May be beneficial to help clear secretions, especially in children with underlying conditions.
- Pain management: For pleuritic chest pain.
Prevention:
- Vaccinations:
- Pneumococcal conjugate vaccine (PCV13): Protects against Streptococcus pneumoniae.
- Hib vaccine: Protects against Haemophilus influenzae type b.
- Influenza vaccine: Annual flu shot.
- Measles vaccine: Measles can lead to severe pneumonia.
- Pertussis vaccine (DTaP): Can prevent pertussis-related pneumonia.
- Hand hygiene.
- Avoidance of secondhand smoke.
- Breastfeeding: Offers passive immunity to infants.
Nursing Care Management:
- Respiratory assessment: Frequent monitoring of all respiratory parameters.
- Administer medications: Antibiotics, oxygen, antipyretics, as ordered.
- Hydration and nutrition: Encourage fluids, monitor intake/output. Small, frequent meals.
- Positioning: Position for comfort, usually semi-Fowler's. If unilateral, positioning with the good lung down can improve ventilation/perfusion, but assess child's comfort.
- Pain management: For chest pain.
- Fever management: Antipyretics, cool compresses.
- Chest physiotherapy and postural drainage: As prescribed, especially for tenacious secretions.
- Education:
- Importance of completing antibiotic course.
- Signs of worsening condition.
- Preventive measures (vaccinations, hygiene).
- When to return to school/daycare.
Complications:
- Pleural effusion: Fluid accumulation in the pleural space.
- Empyema: Pus in the pleural space.
- Necrotizing pneumonia: Destruction of lung tissue.
- Lung abscess.
- Sepsis.
- Respiratory failure.
Nursing Insight: Children with pneumonia, especially bacterial, can look very sick. Ensure aggressive supportive care, vigilant monitoring for deterioration, and prompt administration of antibiotics.
Pulmonary Tuberculosis
- Pulmonary tuberculosis (TB) is a chronic bacterial infection primarily affecting the lungs, caused by Mycobacterium tuberculosis. While less common in children than adults, pediatric TB is a significant global health issue and can be more severe in young children due to their immature immune systems.
Incidence:
- Higher incidence in areas with high prevalence of TB, crowded living conditions, and among immunocompromised individuals.
- Children often acquire TB from an infected adult household contact.
- Children typically have paucibacillary disease (fewer bacteria), making diagnosis challenging and infectivity lower than adults.
Pathophysiology:
- Exposure: Child inhales aerosolized M. tuberculosis bacilli from an infected person.
- Primary Infection: Bacilli reach the alveoli, where macrophages attempt to engulf them. If macrophages fail to kill the bacteria, they replicate.
- Ghon Focus: A primary lesion forms in the lung, often in the mid-lower lobes, along with regional lymph node involvement (hilar lymphadenopathy). This combination is called the Ghon complex.
- Immune Response: Within 2-10 weeks, cell-mediated immunity develops, leading to granuloma formation (tubercles) that contain the infection.
- Latent TB Infection (LTBI): Most children successfully contain the infection and are asymptomatic. They have positive TB tests but no active disease. They are not infectious.
- Active TB Disease: If the immune system is weak or overwhelmed, the granulomas break down, and bacteria multiply and spread.
- Primary Progressive TB: Occurs shortly after primary infection, especially in young infants, immunocompromised children, or those with large inoculums.
- Reactivation TB: Less common in children than adults; occurs when latent infection reactivates years later.
- Miliary TB: Widespread dissemination of bacteria through the bloodstream to multiple organs, forming tiny granulomas resembling millet seeds. Very severe.
- TB Meningitis: Spread to the central nervous system, life-threatening.
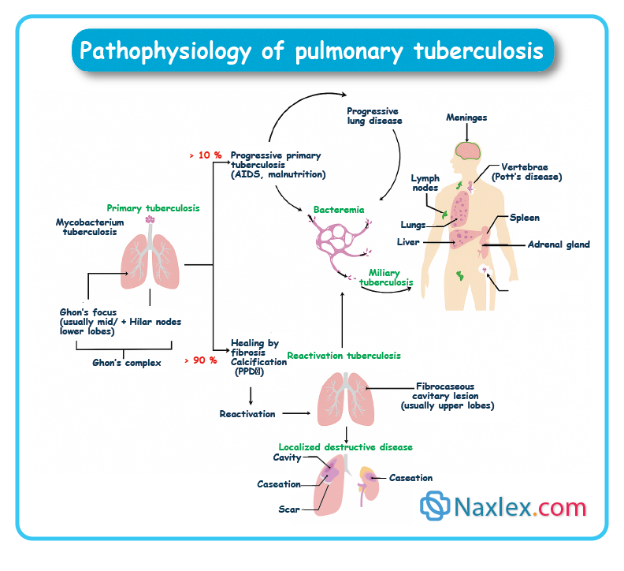
Etiology:
- Mycobacterium tuberculosis is the sole cause.
- Risk factors for progression from LTBI to active disease:
- Age <2 years.
- Immunosuppression (e.g., HIV, malnutrition, corticosteroids).
- Close contact with an adult with active, infectious TB.
- Co-morbidities (e.g., diabetes).
Clinical Manifestations:
- Latent TB: Asymptomatic.
- Active TB in children (can be non-specific):
- Chronic cough: Often non-productive, lasting >2-3 weeks.
- Low-grade fever: May be intermittent or persistent.
- Weight loss or failure to thrive.
- Fatigue, decreased activity levels.
- Night sweats: Less common in children than adults.
- Lymphadenopathy: Enlarged, firm, non-tender cervical or supraclavicular lymph nodes. Hilar lymphadenopathy often seen on CXR.
- Respiratory distress: In more severe cases (e.g., large pleural effusions, miliary TB).
- Extrapulmonary symptoms: Depending on spread (e.g., stiff neck/seizures in TB meningitis, bone pain in skeletal TB).
Diagnostic Evaluation:
- Tuberculin Skin Test (TST)/Mantoux test:
- Intradermal injection of PPD.
- Read 48-72 hours later; measure induration (hard swelling), not redness.
- Interpretation depends on risk factors (e.g., >5mm induration is positive in close contacts, immunocompromised; >10mm in high-risk groups; >15mm in low-risk).
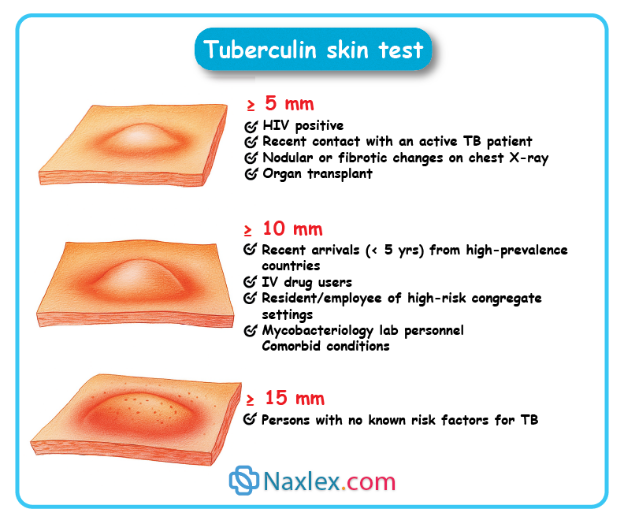
- Interferon-Gamma Release Assays (IGRAs) - e.g., QuantiFERON-TB Gold, T-SPOT.TB:
- Blood tests that measure immune response to TB antigens.
- More specific than TST, not affected by prior BCG vaccination.
- Can be used in children, but TST is still widely used, especially in young children.
- Chest X-ray (CXR):
- Essential for diagnosing active pulmonary TB.
- May show hilar lymphadenopathy (classic in children), consolidation, infiltrates, pleural effusion, or miliary pattern.
- Microbiologic confirmation (the gold standard):
- Gastric aspirates: Often required for young children who cannot produce sputum. Collect early morning samples on 3 consecutive days.
- Sputum induction/bronchoscopy with lavage: For older children or those unable to produce gastric aspirates.
- Culture: Takes 3-6 weeks to grow M. tuberculosis.
- Nucleic Acid Amplification Tests (NAATs): Rapid detection of TB DNA/RNA, providing results within hours; can also detect drug resistance.
- Contact investigation: Crucial to identify the source case (usually an adult).
Therapeutic Management:
- Pharmacologic treatment: A multi-drug regimen is essential to prevent resistance and ensure eradication. Treatment duration is long.
- Latent TB Infection (LTBI):
- Isoniazid (INH): Daily for 6-9 months.
- Rifampin (RIF): Daily for 4 months (alternative, especially if INH resistance suspected or poor adherence anticipated).
- INH + Rifapentine: Weekly for 12 weeks (for children ≥2 years).
- Active TB Disease (Standard Regimen):
- Initial intensive phase (2 months): Four drugs: Isoniazid (INH), Rifampin (RIF), Pyrazinamide (PZA), and Ethambutol (EMB).
- Continuation phase (4 months): Two drugs: Isoniazid (INH) and Rifampin (RIF).
- Total treatment duration: 6 months for most pulmonary TB. Longer for severe forms (e.g., TB meningitis - 9-12 months).
Side Effects of Drugs Used for Management:
- Isoniazid (INH): Peripheral neuropathy (prevented with pyridoxine/Vitamin B6), hepatotoxicity (monitor LFTs), optic neuritis.
- Rifampin (RIF): Hepatotoxicity, orange discoloration of urine, tears, sweat, and contact lenses (educate patient/parents), flu-like symptoms, rash. Many drug interactions (e.g., oral contraceptives).
- Pyrazinamide (PZA): Hepatotoxicity, hyperuricemia (gout), arthralgia, rash.
- Ethambutol (EMB): Optic neuritis (red-green color blindness, decreased visual acuity) - monitor vision, especially in older children who can report symptoms. Not used in very young children who cannot be monitored.
Prevention:
- Early identification and treatment of active TB cases: Especially adult contacts.
- Contact investigation: Essential to find and treat infected individuals.
- Isoniazid (INH) prophylaxis: For children with latent TB, especially those <5 years, to prevent progression to active disease.
- Bacille Calmette-Guérin (BCG) Vaccine:
- Purpose: Live attenuated vaccine, primarily used in countries with high TB incidence to prevent severe forms of TB in infants and young children (e.g., miliary TB, TB meningitis).
- Not routinely used in the US or other low-incidence countries: Due to variable efficacy against adult pulmonary TB, and it interferes with TST interpretation.
- Does not prevent primary infection.
Nursing Care Management:
- Identification of contacts:
- Crucial role in contact tracing and screening for TB.
- Notify relevant authorities: Public health department must be notified for all active TB cases to facilitate contact investigation and surveillance.
- Medication administration and adherence:
- Directly Observed Therapy (DOT) is the gold standard, where a healthcare worker observes the patient taking their medications.
- Educate parents on the importance of completing the entire course of medication, even after symptoms improve, to prevent drug resistance.
- Teach about potential side effects and when to report them.
- Administer pyridoxine with INH.
- Nutritional support: High-calorie, high-protein diet to combat weight loss and promote healing.
- Respiratory support: As needed for active disease.
- Infection control:
- Children with active pulmonary TB are generally considered less infectious than adults due to paucibacillary disease.
- However, airborne precautions may be initiated in hospitalized children until infectivity is ruled out or treatment is effective.
- Educate family on infection control (cough etiquette, ventilation).
- Psychosocial support: Long treatment, fear, stigma. Provide emotional support to child and family.
- Monitoring:
- Regular follow-up appointments.
- Monitoring for medication side effects (e.g., LFTs, vision screening for EMB).
- Repeat sputum/gastric aspirate cultures to document conversion to negative.
Complications:
- Respiratory failure.
- Miliary TB: Disseminated disease.
- TB Meningitis: Severe, often with neurological sequelae.
- Pott's disease: TB of the spine.
- Pericardial effusion/Tamponade.
- Drug-resistant TB: A major global concern, highlighting the importance of adherence.
Nursing Insight: TB treatment is long and challenging. Building trust and providing consistent education and support to the family is vital for treatment adherence and successful outcomes.
Summary
- Lower respiratory tract infections pose significant health challenges, ranging from the common, self-limiting acute bronchitis to severe, life-threatening conditions like pneumonia and pulmonary tuberculosis.
- Each infection has distinct etiologies, pathophysiological processes, and clinical presentations, demanding specific diagnostic and therapeutic approaches.
- Acute Bronchitis: Primarily viral, managed with supportive care; antibiotics are rarely indicated.
- Bronchiolitis (RSV): Common in infants, causes inflammation and obstruction of small airways; managed with supportive care, nasal suctioning, and oxygen. Palivizumab is a crucial prophylactic agent for high-risk infants.
- Pneumonia: Infection of lung parenchyma, caused by various pathogens; diagnosis by chest X-ray and sputum studies; treated with targeted antimicrobial therapy and aggressive supportive care. Prevention via vaccination is vital.
- Pulmonary Tuberculosis: Chronic bacterial infection, requires lengthy multi-drug regimen; highly contagious when active; adherence to DOT and strict infection control measures are critical to prevent drug resistance and transmission.
- Nurses play a pivotal role across the continuum of care for these patients, from accurate assessment and implementation of therapeutic interventions to patient education, infection control, and advocating for public health.
- Understanding the nuances of each condition and applying evidence-based nursing care is essential for improving patient outcomes and preventing the spread of these infectious diseases.
Naxlex
Videos
Login to View Video
Click here to loginTake Notes on Lower Respiratory Tract Infections
This filled cannot be empty
Join Naxlex Nursing for nursing questions & guides! Sign Up Now


