Please set your exam date
Upper Respiratory Tract Infections
Study Questions
Practice Exercise 1
A school-age child has been diagnosed with nasopharyngitis. The parent is concerned because the child has had little or no appetite for the last 24 hours. Which is the nurse’s best response?
Explanation
Nasopharyngitis (common cold) is an inflammation of the nasal passages and the pharynx. It is caused primarily by viruses, especially rhinoviruses, though other viruses like RSV, adenovirus, and coronavirus can also cause it. It is a self-limiting viral infection.
Rationale for correct answer:
2. Adequate fluids are the most important nursing focus in a child with nasopharyngitis. Appetite loss is temporary, but dehydration poses a greater risk. Reassuring parents that appetite will return helps reduce their anxiety while emphasizing fluid intake ensures safety.
Rationale for incorrect answers:
1. “Do not be concerned; it is common for children to have a decreased appetite during a respiratory illness.” While true, this dismisses the parent’s concern without providing guidance or reassurance about what to do.
3. “Try offering favorite foods. Maybe that will improve the appetite.” This may help later, but the immediate priority is hydration, not forcing food. Favorite foods alone don’t address the risk of dehydration.
4. “You need to force your child to eat whatever you can; adequate nutrition is essential.” This is not therapeutic. Forcing food may increase stress, lead to negative associations with eating, and doesn’t address the main concern which is adequate hydration.
Take home points
- Hydration is the top priority in viral respiratory infections with poor appetite.
- Appetite usually improves as symptoms resolve.
- Parents should be reassured while given clear guidance on safe home care.
- Forcing food is not appropriate; instead, encourage fluids and small, tolerable meals once the child is ready.
What information should the nurse provide the parent of a child diagnosed with nasopharyngitis?
Explanation
Nasopharyngitis (common cold) is an inflammation of the nasal passages and the pharynx. It is caused primarily by viruses, especially rhinoviruses, though other viruses like RSV, adenovirus, and coronavirus can also cause it. It is a self-limiting viral infection.
Rationale for correct answer:
3. Nasopharyngitis (common cold) is a viral infection, so antibiotics are not indicated. Treatment is supportive care with rest, fluids, fever control (acetaminophen/ibuprofen if appropriate), and comfort measures such as saline nasal drops, humidified air, and adequate hydration.
Rationale for incorrect answers:
1. Antibiotics are not indicated for viral infections. Antibiotics do not treat the common cold and may contribute to resistance.
2. Avoiding day care is not realistic or necessary unless the child has a fever or severe symptoms. Children can return when they are comfortable and fever-free.
4. Clear liquids restriction is not required. Children should continue their normal diet with increased fluids if tolerated. Restricting diet does not improve recovery.
Take home points
- Nasopharyngitis is a viral self-limiting illness.
- Management is comfort-based: fluids, rest, nasal saline/suction, humidifier, acetaminophen or ibuprofen for fever/discomfort.
- Antibiotics are not indicated unless a secondary bacterial infection develops.
- Parents should watch for complications such as ear pain, persistent high fever, and breathing difficulties.
A child is complaining of throat pain. Which statement by the mother indicates that she needs more education regarding the care and treatment of her child’s pharyngitis?
Explanation
Pharyngitis is the inflammation of the pharynx. It may be viral or bacterial. Viral pharyngitis does not require antibiotics, while bacterial pharyngitis (commonly group A strep) requires confirmation by rapid strep test or throat culture before antibiotics are prescribed.
Rationale for correct answer:
4. Asking for amoxicillin without testing shows a misunderstanding. Antibiotics are not indicated unless the child tests positive for bacterial strep. Education should stress the importance of diagnostic confirmation before treatment.
Rationale for incorrect answers:
1. Gargling with salt water is appropriate supportive measure to soothe throat discomfort and reduce inflammation.
2. Offering ice chips is helpful for hydration and numbing throat pain. This is safe and recommended.
3. Giving Tylenol every 4–6 hours as needed is correct for pain relief and fever management, within safe dosing guidelines.
Take home points
- Not all sore throats need antibiotics; viral pharyngitis is managed with comfort care.
- Antibiotics are prescribed only after confirmation of strep throat by diagnostic testing.
- Supportive measures (fluids, salt water gargles, ice chips, analgesics) are effective for symptom relief.
- Parent education should highlight judicious use of antibiotics to prevent resistance and complications.
A child’s parent asks the nurse what treatment the child will need for the diagnosis of strep throat. Which is the nurse’s best response?
Explanation
Streptococcal pharyngitis (strep throat) is a bacterial infection caused by group A beta-hemolytic streptococcus (GABHS). Spread through respiratory droplets through coughing, sneezing, or sharing utensils. It is highly contagious especially in schools, daycares, and communal settings.
Rationale for correct answer:
3. Oral penicillin for 10 days is the standard treatment. Symptoms typically improve within 24–48 hours, but completing the entire course is essential to prevent recurrence and serious complications.
Rationale for incorrect answers:
1. Bedrest without intervention is incorrect. Strep throat requires antibiotics and untreated cases risk rheumatic heart disease and kidney involvement.
2. Tonsil removal is not the first-line treatment. Tonsillectomy is reserved for recurrent infections or complications, not a single episode.
4. Hospital admission with IV antibiotics is reserved for severe cases, inability to tolerate oral medications, or complications. Routine strep throat can be safely treated at home with oral antibiotics.
Take home points
- A full 10-day course of oral antibiotics (penicillin or equivalent) is the gold standard for strep throat.
- Symptoms improve quickly, but finishing treatment is crucial to prevent complications.
- Tonsillectomy and hospitalization are not routine treatments.
- Parent education should focus on medication adherence and monitoring for signs of complications.
A school-age child has been diagnosed with strep throat. The parent asks the nurse when the child can return to school. Which is the nurse’s best response?
Explanation
Streptococcal pharyngitis (strep throat) is a bacterial infection caused by group A beta-hemolytic streptococcus (GABHS). Spread through respiratory droplets through coughing, sneezing, or sharing utensils. It is highly contagious especially in schools, daycares, and communal settings.
Rationale for correct answer:
2. Streptococcal pharyngitis (strep throat) is contagious until the child has received at least 24 hours of antibiotic therapy. This is the CDC and AAP recommendation. Once antibiotics have been started and the child is afebrile, they may safely return to school.
Rationale for incorrect answers:
1. Forty-eight hours after the first documented normal temperature is too restrictive. The key factor is antibiotic therapy, not just temperature.
3. Forty-eight hours after the first dose of antibiotics is unnecessarily long. 24 hours after initiation of antibiotics is sufficient for the child to return to school.
4. Twenty-four hours after the first documented normal temperature overlooks the role of antibiotics in halting infectivity.
Take home points
- Children with strep throat are no longer contagious 24 hours after starting antibiotics.
- Returning to school is safe if the child is afebrile and well enough to participate.
- Parent teaching should emphasize: complete the full 10-day antibiotic course, replace the child’s toothbrush after 24–48 hours on antibiotics, and monitor for complications such as rheumatic fever.
Practice Exercise 2
A school-age child is admitted to the hospital for a tonsillectomy. During the nurse’s postoperative assessment, the child’s parent tells the nurse that the child is in pain. Which of the following observations would be of most concern to the nurse?
Explanation
Tonsillectomy is a surgical procedure to remove the tonsils. It is indicated for recurring and chronic tonsillitis, enlarged tonsils causing difficulty swallowing or breathing, and tonsillar abscesses unresponsive to treatment.
Rationale for correct answer:
4. Excessive swallowing indicates possible bleeding in the oropharynx. After a tonsillectomy, the most serious postoperative complication is hemorrhage. Because blood often trickles down the throat rather than being coughed up, excessive swallowing is a key early sign of bleeding. Prompt recognition and intervention are crucial to prevent airway compromise and hypovolemic shock.
Rationale for incorrect answers:
1. Elevated heart rate and blood pressure may reflect pain or anxiety. While concerning, it is not the most critical finding compared to potential hemorrhage.
2. Complaining of sore throat is expected after tonsillectomy. This should be managed with analgesics.
3. Refusal to eat solid foods is expected after tonsillectomy. Children often prefer soft or cool foods initially. This is not a danger sign.
Take home points
- Excessive swallowing is the earliest and most important sign of postoperative bleeding after tonsillectomy.
- Pain, sore throat, and poor appetite are expected findings and managed supportively.
- Nurses must closely monitor for bleeding and notify the provider immediately if suspected.
- Family teaching should include watching for frequent swallowing, vomiting bright red blood, or increased restlessness at home.
The nurse is reviewing discharge instructions with the parents of a child who had a tonsillectomy a few hours ago. The parents tell the nurse that the child is a big eater, and they want to know what foods to give the child for the next 24 hours. What is the nurse’s best response?
Explanation
Tonsillectomy is a surgical procedure to remove the tonsils. It is indicated for recurring and chronic tonsillitis, enlarged tonsils causing difficulty swallowing or breathing, and tonsillar abscesses unresponsive to treatment.
Rationale for correct answer:
2. During the first 24 hours, the safest diet is clear, cool, non-irritating liquids such as water, apple juice, popsicles, and broth. They are soothing, easy to swallow, and least likely to irritate the surgical site. This minimizes pain, reduces risk of trauma, and helps prevent postoperative bleeding.
Rationale for incorrect answers:
1. Lack of dietary restriction is unsafe since regular foods can traumatize the surgical site and cause bleeding.
3. While cold fluids are soothing, ice cream/dairy is avoided in the immediate period due to mucus formation and possible throat clearing which can result in bleeding from the surgical site.
4. Soft foods are appropriate after the first 24 hours, once the child tolerates liquids and healing has begun. Providing this diet within the first 24hours is too early at this stage.
Take home points:
- For the first 24 hours after tonsillectomy, the diet should be restricted to clear, cool liquids.
- Avoid dairy, red-colored fluids which may mask blood, and solid foods initially.
- Gradually advance to soft foods after 24 hours as tolerated.
- Parent teaching should emphasize monitoring for bleeding signs such as frequent swallowing, vomiting blood, restlessness.
A parent asks how to care for a child at home who has the diagnosis of viral tonsillitis. Which is the nurse’s best response?
Explanation
Viral tonsillitis is caused by a virus such as rhinovirus, influenza, coronavirus, respiratory syncytial virus (RSV), and adenovirus. The symptoms include sore throat and painful swallowing, fever, chills, lymphadenopathy, and erythematous swollen tonsils. Most cases resolve within 3 to 7 days.
Rationale for correct answer:
3. Acetaminophen for pain/fever is safe and effective for managing discomfort associated with viral tonsillitis. Dosing every 4–6 hours as needed provides symptom relief and helps the child rest.
Rationale for incorrect answers:
1. Prescribed antibiotic for 10 days is incorrect since antibiotics treat bacterial infections like strep throat, not viral tonsillitis.
2. Scheduling a follow-up in 2 weeks as a routine follow-up isn’t required unless symptoms worsen or complications develop.
4. Warm towels around the neck is not evidence-based or effective in treating throat pain. Cool fluids and analgesics are more appropriate.
Take home points
- Viral tonsillitis is treated with supportive care only, not antibiotics.
- Acetaminophen or ibuprofen can be used for pain and fever.
- Encourage hydration, rest, and soft/cool foods for comfort.
- Parent teaching: return to the provider if symptoms persist >7–10 days, worsen, or if signs of bacterial infection appear such as high fever, exudates, and difficulty swallowing.
Which nursing interventions is appropriate when providing care for a client after a tonsillectomy?
Explanation
Tonsillectomy is a common pediatric surgical procedure. Postoperative care is crucial to prevent complications such as airway obstruction, bleeding, and pain. Nursing interventions should focus on airway maintenance, bleeding precautions, comfort measures, and gradual diet advancement.
Rationale for correct answer:
1. Positioning the child on the side-lying or prone position helps facilitate drainage of secretions, reduces the risk of aspiration, and maintains airway patency. This is the priority nursing intervention immediately after a tonsillectomy.
Rationale for incorrect answers:
2. Frequent or aggressive suctioning can traumatize the surgical site and increase the risk of bleeding. Suctioning should only be done if necessary and with extreme caution.
3. Fruit juices, especially citrus or red-colored drinks, are irritating to the throat and can mask bleeding. Clear, cool liquids like water or ice chips are preferred.
4. Heat may increase vasodilation and the risk of bleeding. Cold compresses or ice collars are recommended for comfort and to reduce swelling.
Take home points
- Airway maintenance is the top priority after a tonsillectomy. The nurse should place the child side-lying or prone.
- Avoid red-colored fluids, acidic/citrus juices, and spicy foods.
- Use cold therapy such as ice collar and cold fluids instead of heat to reduce swelling and pain.
- Monitor for frequent swallowing, which can indicate bleeding.
A child is being sent home after a tonsillectomy. Which of the following actions should the nurse educate the parents to perform?
Explanation
Tonsillectomy is a surgical procedure to remove the tonsils. It is indicated for recurring and chronic tonsillitis, enlarged tonsils causing difficulty swallowing or breathing, and tonsillar abscesses unresponsive to treatment.
Rationale for correct answer:
1. After a tonsillectomy, the most serious postoperative risk is hemorrhage. Continuous or frequent swallowing, even while asleep, is an early and important sign of bleeding, as the child may be swallowing blood trickling from the surgical site. Parents should be instructed to observe for this and report it immediately.
Rationale for incorrect answers:
2. Warm compresses around the neck is not recommended; may increase blood flow and risk of bleeding. Comfort is achieved better with ice collar/cold therapy.
3. Citrus juices such as orange and lemonade are acidic and irritating to the throat, increasing discomfort and risk of bleeding. The child should be offered cool, clear, non-irritating fluids such as water, ice chips, and apple juice.
4. Supine positioning is dangerous after tonsillectomy, as it increases the risk of airway obstruction and aspiration of blood. The child should be positioned on the side-lying or prone position to facilitate drainage until fully awake.
Take home points
- Excessive swallowing indicates possible hemorrhage after tonsillectomy.
- Avoid irritants like citrus and hot/spicy foods.
- Position side-lying or prone, not supine, in the immediate postop period.
- Provide comfort with ice collar and acetaminophen, not aspirin or codeine.
Practice Exercise 3
Which would be appropriate nursing care management of a child with the diagnosis of mononucleosis?
Explanation
Infectious mononucleosis, caused by the Epstein–Barr virus, spreads primarily through saliva and close contact. Nursing care focuses on preventing transmission, managing symptoms such as fever, sore throat, and fatigue, and avoiding complications like splenic rupture.
Rationale for correct answer:
1. Limiting exposure to only family visitors reduces the chance of spreading the infection to others, since mononucleosis is contagious through saliva and close personal contact. The nurse should make every effort to prevent a secondary infection by counseling the adolescent to limit exposure to persons outside the family, especially during the acute phase of illness.
Rationale for incorrect answers:
2. Bedrest is no longer recommended. Children should rest as needed but can gradually resume normal activities once fatigue improves. Strict bedrest is unnecessary. However, the nurse should encourage the affected individual to curtail activities that are strenuous until splenomegaly is resolved.
3. Clear liquids are not required unless the child has severe sore throat or swallowing difficulties. A soft diet with adequate hydration is encouraged.
4. Limited daily fluid intake is incorrect. Fluids should actually be encouraged to prevent dehydration and support recovery.
Take home points
- Visitor restriction helps prevent spread of mononucleosis, especially in healthcare or group settings.
- Management is supportive: rest as needed, hydration, analgesics for throat pain, and activity restriction (especially contact sports) if splenomegaly is present.
- Nurses should teach families about the contagious nature of the illness and the importance of avoiding saliva-sharing behaviors such as kissing and sharing utensils.
A college health nurse is providing education to a student athlete who is diagnosed with infectious mononucleosis. The student asks, “Will I be able to play soccer after I rest up for a few weeks?” Which should be the best response by the nurse?
Explanation
Infectious mononucleosis, caused by the Epstein-Barr virus, is common among adolescents and young adults. While it’s not as contagious as the common cold, it spreads primarily through saliva, which is why kissing, sharing drinks, or utensils can pass it along. A major complication is splenomegaly, which increases the risk of splenic rupture.
Rationale for correct answer:
3. The spleen is often enlarged with mononucleosis, making it vulnerable to rupture from trauma. Soccer, football, wrestling, or any contact sport should be avoided until cleared by a healthcare provider after spleen size has returned to normal. This safety measure is critical regardless of how well the student feels.
Rationale for incorrect answers:
1. “You may not be physically active for 2 to 3 months.” This is too restrictive and not evidence-based. Activity can be resumed once cleared by the provider.
2. “You may be as active as you wish as long as you are not feeling fatigued.” This is incorrect, because splenic rupture risk exists even if the student feels well.
4. “There are no limitations on activity with this diagnosis.” This is dangerous misinformation since it ignores the risk of splenic rupture.
Take home points
- Splenomegaly is the biggest risk in infectious mononucleosis.
- No contact sports until cleared by a healthcare provider, often 3–4 weeks or longer, depending on spleen size.
- Nurses must emphasize safety over symptoms, since splenic rupture can be life-threatening but may occur without warning.
Who is at the highest priority to receive the flu vaccine?
Explanation
The influenza vaccine is recommended for nearly everyone ≥6 months of age, but certain groups are at highest priority due to their increased risk of influenza-related complications. Infants, the elderly, immunocompromised clients, and those in group settings are emphasized.
Rationale for correct answer
1. Infants and young children (6–59 months) are at the highest risk of serious complications from influenza such as pneumonia, dehydration, hospitalization, and death. This risk is further increased in a day care setting where exposure is frequent. The CDC specifically prioritizes children 6–59 months for influenza vaccination.
Rationale for incorrect answers
2. Although a 3-year-old who is undergoing chemotherapy is high-risk, live vaccines are contraindicated in immunocompromised children. They benefit from herd immunity, but the child themselves may not safely receive the vaccine depending on their regimen.
3. A healthy 7-year-old who attends public school should receive the vaccine, but this age group is not the highest priority compared to infants.
4. An 18-year-old in a college dormitory is at increased risk due to close living quarters, but the risk of severe complications is lower than in infants.
Take home points
- Children 6–59 months are among the highest-priority groups for influenza vaccination.
- Immunocompromised individuals benefit most from herd immunity; their ability to receive vaccines depends on treatment status.
- Congregate living (schools, dorms) increases transmission risk, but severe disease risk is greatest in the very young, elderly, and chronically ill.
The parent of a child with influenza asks the nurse when the child is most infectious. Which is the nurse’s best response?
Explanation
Influenza is highly contagious and spreads via respiratory droplets. The infectious period begins about 1 day before symptom onset and lasts until about 5–7 days after becoming sick. Young children and immunocompromised individuals may remain infectious for longer.
Rationale for correct answer:
1. Twenty-four hours before and after onset is correct. People can transmit influenza before they even realize they are ill, making early spread common in households, schools, and communities.
Rationale for incorrect answers:
2. Twenty-four hours after onset is incorrect since people are already infectious before symptoms appear, so this underestimates risk.
3. One week after onset is incorrect. Infectivity usually decreases well before this point, though children may shed virus longer.
4. One week before onset is incorrect since the virus does not spread this far in advance; incubation is usually 1–4 days.
Take home points
- Children with influenza are infectious 1 day before symptoms and up to 7 days after illness onset.
- This explains why influenza spreads so rapidly in schools and households.
- Prevention strategies: annual vaccination, hand hygiene, covering coughs, and staying home when sick.
A 6-week-old is admitted to the hospital with influenza. The child is crying, and the father tells the nurse that his son is hungry. The nurse explains that the baby is not allowed to have anything by mouth. The parent does not understand why the child cannot eat. Which is the nurse’s best response to the parent?
Explanation
Influenza, commonly called the flu, is a highly contagious viral infection that affects your respiratory system, including the nose, throat, and lungs. It’s caused by influenza viruses, primarily types A and B, which circulate seasonally and can lead to widespread outbreaks.
Rationale for correct answer:
2. Infants with respiratory illnesses like influenza are at high risk of aspiration because they have small, narrow airways and poor coordination of sucking, swallowing, and breathing when congested or in distress. Withholding oral feeds until safe helps prevent further respiratory compromise and aspiration pneumonia. This explains to the parent in clear terms why NPO (nothing by mouth) is needed during acute respiratory distress.
Rationale for incorrect answers:
1. “We are giving your child intravenous fluids, so there is no need for anything by mouth.” This is true about hydration, but it does not address the safety concern (aspiration risk), so it’s incomplete and not the best explanation.
3. “When your child eats, he burns too many calories; we want to conserve the child’s energy.” While conserving energy is important, this is not the main reason for NPO status in respiratory distress.
4. “Your child has too much nasal congestion; if we feed the child by mouth, the distress will likely increase.” Congestion can increase feeding difficulty, but the key issue is airway protection and aspiration risk, not just distress.
Take home points
- Infants with significant respiratory distress are often kept NPO to prevent aspiration.
- IV fluids maintain hydration until it is safe to resume oral feeds.
- Parental education should always connect the restriction to airway safety, not just comfort.
- Once the child’s breathing improves, oral feeds can be reintroduced gradually.
Comprehensive Questions
Which intervention is most appropriate to teach the mother of a 3-year-old child diagnosed with a URI and a dry, hacking cough that prevents him from sleeping?
Explanation
Upper respiratory infections (URIs) are common in children and often present with cough, nasal congestion, and fever. While most URIs are viral and self-limiting, supportive care is important for comfort and recovery.
Rationale for correct answer:
4. Honey is a safe and effective home remedy for children over 1 year old. It helps soothe the throat, reduces irritation, and suppresses nighttime coughing. Studies have shown honey to be as effective as some OTC cough medicines in improving sleep and reducing cough frequency.
Rationale for incorrect answers:
1. Cough suppressants are not recommended in young children due to lack of proven benefit and potential adverse effects.
2. Expectorants are not effective in children and may cause gastrointestinal side effects.
3. Cold and flu medications are contraindicated in children under 6 years; associated with risk of overdose, toxicity, and minimal therapeutic value.
Take home points
- Honey is recommended for soothing cough in children older than 1 year.
- Supportive measures such as humidified air, saline drops with suctioning, and hydration can ease URI symptoms.
- Avoid OTC cough and cold medications in young children.
- Never give honey to infants under 12 months due to the risk of infant botulism.
Which is the nurse’s best response to a parent who asks what can be done at home to help an infant with upper respiratory infection (URI) symptoms and a fever get better?
Explanation
Upper respiratory tract infections (URTIs) in children are among the most common illnesses they experience, especially in early childhood. These infections affect the nose, throat, sinuses, and ears, and are usually caused by viruses, not bacteria.
Rationale for correct answer:
1. Fluids encourages hydration, thins secretions, prevents dehydration from fever and rapid breathing. This is safe, effective, and evidence-based advice for infants with URIs.
Rationale for incorrect answers:
2. Over the counter (OTC) cough suppressants such as Robitussin are not recommended for infants; they can cause side effects and do not improve outcomes.
3. Aspirin is contraindicated in children with viral infections because of the risk of Reye’s syndrome, which can be life-threatening.
4. Cold medicines are not safe for infants. They can cause serious adverse effects and are not effective in this age group.
Take home points
- Management of URI in infants is supportive: fluids, rest, fever control with acetaminophen (not aspirin), and nasal saline with suction for congestion.
- OTC cough and cold medications are not recommended in children under 6 years, especially infants.
- Always educate caregivers on red flag signs such as increased work of breathing, poor feeding, dehydration, and lethargy that require medical attention.
When an infant has an upper respiratory infection, which action should a nurse take before feeding the child?
Explanation
Infants with upper respiratory infections (URIs) often experience nasal congestion that interferes with feeding, since they are obligate nose breathers for the first several months of life. The nurse’s role is to ensure the airway is clear prior to feeding to reduce aspiration risk and help the infant feed more effectively.
Rationale for correct answer:
4. Instilling saline drops and gently suctioning the nares clears secretions and improves nasal airflow. This intervention is especially important before feeding and sleep, as it helps the infant breathe more comfortably, decreases aspiration risk, and promotes adequate intake.
Rationale for incorrect answers:
1. Chest physiotherapy and postural drainage is not indicated for a simple URI; it is used for conditions like cystic fibrosis or bronchiolitis with retained lower airway secretions.
2. Elevating the head may help breathing but does not address nasal congestion directly, so it is not the most effective initial step before feeding.
3. Give an antitussive is not recommended for infants. Cough medicines are ineffective and unsafe in young children.
Take home points
- Infants with URIs need nasal suctioning with saline drops before feeding to maintain airway patency.
- Always avoid antitussives and OTC cough medicines in infants.
- Feeding an infant with a congested nose can increase risk of aspiration and poor intake if suctioning is not done first.
A 12-year-old child is in the urgent care clinic with a complaint of fever, headache, and sore throat. A diagnosis of group A β-hemolytic streptococcus (GABHS) pharyngitis is established with a rapid-strep test, and oral penicillin is prescribed. The nurse knows that which of the following statements about GABHS is correct?
Explanation
Group A β-hemolytic streptococcus (GABHS) pharyngitis is a common cause of sore throat in school-aged children. While the infection itself is usually self-limiting, untreated or inadequately treated cases can lead to serious nonsuppurative complications.
Rationale for correct answer:
3. GABHS infections can trigger autoimmune responses after untreated or inadequately treated infections. Rheumatic fever develops from an abnormal immune response affecting the heart, joints, and nervous system. Glomerulonephritis results from immune complex deposition in the kidneys. Antibiotic treatment is essential to reduce these risks.
Rationale for incorrect answers:
1. Reinfection is common because immunity is not long-lasting; children can get strep throat multiple times.
2. Follow-up throat culture is not routinely recommended after treatment unless the child remains symptomatic, is at high risk, or has a history of rheumatic fever.
4. Increased risk for rheumatoid arthritis is incorrect. GABHS does not cause rheumatoid arthritis. Rheumatoid arthritis is an autoimmune condition unrelated to strep infection.
Take home points
- GABHS pharyngitis carries risks of acute rheumatic fever and post-streptococcal glomerulonephritis if untreated.
- Antibiotics such as penicillin for 10 days reduce symptoms, transmission, and risk of complications.
- No lasting immunity is provided hence reinfections are common.
- Routine follow-up throat cultures are not necessary unless symptoms persist or special circumstances exist.
A 5-year-old is recovering from a tonsillectomy and adenoidectomy and is being discharged home with his mother. Home care instructions should include which of the following? Select all that apply
Explanation
Tonsillectomy and adenoidectomy are common pediatric procedures performed for recurrent throat infections or obstructive sleep apnea. Postoperative care focuses on preventing complications such as bleeding and airway obstruction, while also providing adequate hydration, pain control, and comfort measures.
Rationale for correct answers:
1. Continuous swallowing may indicate bleeding, especially from the surgical site; it is a priority to monitor.
2. Cool, clear liquids promote hydration, are soothing to the throat, and reduce swelling and bleeding risk.
4. Restlessness/difficulty breathing are signs of airway obstruction or hemorrhage and require immediate attention.
6. Acetaminophen is safe and effective for pain relief. It helps maintain comfort and encourage fluid intake.
Rationale for incorrect answers:
3. Codeine elixir is contraindicated in children due to risk of respiratory depression and even fatal outcomes (FDA warning).
5. Cough every 4–5 hours can dislodge clots, cause bleeding, and increase discomfort. Therefore, coughing should be avoided.
Take home points
- After tonsillectomy, monitor for bleeding (continuous swallowing) and airway obstruction (restlessness, difficulty breathing).
- Encourage cool, clear fluids; avoid citrus, hot, spicy, or red-colored liquids.
- Provide acetaminophen for pain control. Codeine should be avoided in children.
- Avoid coughing, clearing the throat, straws, or vigorous activity to prevent bleeding.
A 7-year-old child has been prescribed penicillin V for streptococcal pharyngitis. Which of the following information should the nurse teach the parents regarding the medication?
Explanation
Streptococcal pharyngitis (strep throat) is commonly treated with penicillin V, which effectively eradicates the infection, reduces symptoms, and prevents complications such as rheumatic fever and glomerulonephritis. Parent teaching is critical to ensure adherence, prevent recurrence, and reduce spread.
Rationale for correct answer:
2. Completing the entire antibiotic course ensures full eradication of group A strep bacteria, prevents recurrence, and reduces the risk of serious complications like rheumatic fever. Even if the child feels better, discontinuing antibiotics early may allow bacteria to persist.
Rationale for incorrect answers:
1. Once the child starts the medication, he will no longer be contagious: This statement is incorrect. The child remains contagious until at least 24 hours after starting antibiotics.
3. The child’s fever may persist until all the medicine is taken: This statement is incorrect. Fever typically resolves within 24–48 hours of starting treatment, not after the full 10-day course.
4. If given with food, the medicine will be ineffective: This statement is incorrect. Penicillin V can be taken with or without food; food may actually help reduce stomach upset.
Take home points
- Teach parents: complete the full antibiotic course.
- The child is contagious until 24 hours after starting therapy and being afebrile.
- Symptoms such as fever and sore throat should improve within 1–2 days.
- Antibiotics are key to preventing rheumatic fever and glomerulonephritis.
The throat culture of an 8-year-old child grew out 4 bacteria. The nurse should request the primary health-care provider to prescribe an antibiotic for the child to treat which of the following bacteria?
Explanation
Throat cultures in children may reveal a mix of normal flora and potential pathogens. However, antibiotic treatment is only indicated for specific organisms known to cause bacterial pharyngitis and associated complications.
Rationale for correct answer:
2. Streptococcus pyogenes is the causative agent of strep throat and requires prompt antibiotic therapy. Treating this infection reduces symptom duration, prevents spread, and most importantly, prevents complications such as acute rheumatic fever and post-streptococcal glomerulonephritis. First-line therapy is typically penicillin or amoxicillin.
Rationale for incorrect answers:
1. Hemophilus influenzae is more commonly associated with otitis media, sinusitis, or epiglottitis, not simple pharyngitis. Throat colonization does not require treatment unless clinically indicated.
3. Streptococcus pneumoniae is a normal colonizer of the nasopharynx. Treatment is not indicated unless the child has pneumonia, otitis media, or sinusitis.
4. Mycoplasma pneumoniae typically causes atypical pneumonia in older children/adolescents, not isolated pharyngitis. Antibiotics would not be prescribed for a throat culture finding alone.
Take home points
- Antibiotic therapy for pharyngitis is indicated only when Streptococcus pyogenes (Group A strep) is identified.
- Colonization with other bacteria such as S. pneumoniae and H. influenzae does not warrant antibiotics without clinical disease.
- Treating strep throat prevents not only local infection but also serious systemic complications.
- Always correlate culture results with clinical presentation before initiating antibiotics.
A 7-month-old has a low-grade fever, nasal congestion, and a mild cough. What should the nursing care management of this child include? Select all that apply
Explanation
Nursing care management for infants with mild upper respiratory infections such as viral URI or early bronchiolitis, focuses on relieving nasal congestion, ensuring adequate hydration and oxygenation, and keeping the child comfortable. Supportive care is the mainstay, since antibiotics are not indicated for viral causes.
Rationale for correct answers:
3. Infants are obligate nose breathers, so nasal congestion can significantly impair feeding and breathing. Saline drops loosen secretions, and gentle suctioning clears the airway.
5. Humidity helps moisten airways and ease breathing. Elevating the head of the bed reduces postnasal drip, eases congestion, and promotes comfort.
Rationale for incorrect answers:
1. Maintaining strict bedrest is not necessary for infants with mild URI. In these children, activity is self-limited by fatigue.
2. Avoiding contact with family members isolates the child which is unnecessary. Good hand hygiene and limiting exposure to vulnerable people is more appropriate.
4. Keeping the head of the bed flat worsens congestion and increases difficulty breathing. Elevation of the head of the bed is preferred.
Take home points
- Supportive care is the cornerstone of managing mild respiratory illness in infants.
- Nasal saline and suctioning are first-line to maintain airway patency.
- Humidity and elevating the head improve comfort and breathing.
- Avoid unnecessary restrictions (strict bedrest, family isolation) that don’t benefit recovery.
A 16-year-old child is seen in the pediatric clinic with signs and symptoms of the flu. To prevent further disease, the nurse educates the parents and the teenager to refrain from performing which of the following treatment practices?
Explanation
Influenza is a highly contagious viral illness that commonly affects children and adolescents. While most cases resolve with supportive care, complications can arise when inappropriate medications or management strategies are used. One critical nursing role is educating parents and teens on safe home care practices to promote recovery and prevent complications.
Rationale for correct answer:
4. Children and adolescents with viral infections such as influenza should not be given aspirin due to the risk of Reye’s syndrome, a rare but life-threatening condition involving acute encephalopathy and liver dysfunction. Instead, acetaminophen or ibuprofen should be used for fever or discomfort.
Rationale for incorrect answers:
1. Avoiding dairy products is a myth, not evidence-based. Dairy may thicken secretions slightly but does not worsen influenza or spread disease.
2. Avoiding the sun is not relevant to influenza management. Sun exposure does not worsen the illness.
3. While rest is important, light movement is not contraindicated. Exercise is limited naturally by fatigue, but it does not worsen the disease.
Take home points
- Do not give aspirin to children or teens with influenza or varicella-like illnesses due to the risk of Reye’s syndrome.
- Safe alternatives such as acetaminophen and ibuprofen should be used.
- Encourage hydration, rest, and comfort measures.
In which position should a nurse place a child postoperative tonsil and adenoidectomy (T&A)?
Explanation
Tonsillectomy is a surgical procedure to remove the tonsils. It is indicated for recurring and chronic tonsillitis, enlarged tonsils causing difficulty swallowing or breathing, and tonsillar abscesses unresponsive to treatment.
Rationale for correct answer:
3. Side-lying positioning allows secretions and blood to drain out of the mouth instead of pooling in the throat, which helps reduce the risk of aspiration and airway obstruction. It is the safest initial position during the immediate postoperative period when the child may still be drowsy from anesthesia.
Rationale for incorrect answers:
1. Semi-Fowler with the head turned to the side is not the standard immediate postop position; while elevating the head can help with comfort later, side-lying is safer initially.
2. High Fowler, head slightly forward and to the side is not recommended for immediate postop because it may cause flexion and compromise the airway.
4. Supine positioning increases the risk of aspiration if bleeding or secretions occur.
Take home points
- The side-lying or prone position is preferred immediately after a tonsillectomy to promote drainage.
- Once the child is fully awake and alert, they may transition to an upright position for comfort and airway support.
- Monitoring for excessive swallowing, restlessness, or airway obstruction is a critical nursing responsibility post-T&A.
A nurse is formulating a preoperative plan of care for a 5-year-old child who is scheduled for a tonsiland adenoidectomy (T&A). Which nursing diagnosis is priority?
Explanation
Children scheduled for surgery often experience fear, anxiety, and separation distress, especially at 5 years old. Preoperative nursing care focuses on preparing the child and family emotionally and psychologically, while ensuring understanding of the procedure.
Rationale for correct answer:
4. At the preoperative stage, the child has not yet experienced surgical pain, airway issues, or nutritional imbalance. The priority diagnosis is anxiety, as children at this age often fear separation, loss of control, and the unknown. Addressing anxiety helps build trust, improves cooperation, and prepares the child for postoperative recovery.
Rationale for incorrect answers:
1. Imbalanced nutrition is not priority preoperatively; nutrition concerns may arise after surgery when throat pain limits intake.
2. Pain related to surgery is anticipated, but not yet present before the procedure.
3. Ineffective airway clearance is a postoperative risk, not a preoperative problem.
Take home points
- Pre-op priority includes psychosocial needs (anxiety, fear, coping).
- Post-op priority includes physiologic needs (airway, pain, bleeding, nutrition).
- Always tailor nursing diagnoses to the stage of care (before vs. after surgery).
A nurse is caring for a 3-year-old client who is postoperative tonsil and adenoidectomy (T&A) surgery. The nurse should suspect complications when assessing:
Explanation
Tonsillectomy is a surgical procedure to remove the tonsils. It is indicated for recurring and chronic tonsillitis, enlarged tonsils causing difficulty swallowing or breathing, and tonsillar abscesses unresponsive to treatment.
Rationale for correct answer:
3. Frequent swallowing and throat clearing are early signs of hemorrhage after a tonsillectomy and adenoidectomy (T&A). Children may swallow blood trickling down the throat instead of spitting it out, making this a subtle but critical finding that requires immediate intervention.
Rationale for incorrect answers:
1. Sore throat and difficulty swallowing is expected postoperative findings due to surgical site trauma; not a complication.
2. Secretions and dried blood at the corners of the mouth is normal after surgery. It indicates minor oozing during or after the procedure.
4. Some secretions, particularly dried blood from surgery, are common. Dark brown (old) blood is usually present in the emesis, as well as in the nose and between the teeth. The priority is catching early bleeding signs such as excessive swallowing.
Take home points
- Hemorrhage is the most serious complication after T&A, especially within the first 24 hours and again 7–10 days later (when scabs slough).
- The earliest and most reliable sign is frequent swallowing or throat clearing.
- Nurses should closely monitor for restlessness, tachycardia, pallor, or bright red blood, which indicate active bleeding.
A nurse is caring for an 8-year-old child following a tonsillectomy. The nurse identifies the nursing diagnosis of Impaired swallowing related to inflammation and pain. Which fluids should the nurse plan to administer?
Explanation
Tonsillectomy is a surgical procedure to remove the tonsils. It is indicated for recurring and chronic tonsillitis, enlarged tonsils causing difficulty swallowing or breathing, and tonsillar abscesses unresponsive to treatment.
Rationale for correct answer:
1. Cool fluids and ice pops are soothing to the throat, help reduce inflammation, and encourage hydration. They are nonirritating and allow easy observation for blood in case of postoperative bleeding.
Rationale for incorrect answers:
2. Red or brown fluids should be avoided because they may mask signs of bleeding if vomiting occurs.
3. Colored citrus drinks are acidic and irritating to the surgical site; can increase pain and discomfort.
4. Dairy products such as ice cream may coat the throat and increase mucus production, leading to coughing and possible disruption of the surgical site.
Take home points
- Best fluids after tonsillectomy: clear, cool, nonirritating (water, apple juice, flavored ice pops).
- Avoid: red/brown fluids (mask bleeding), citrus (irritating), and dairy (increases secretions).
- Adequate hydration is critical for recovery, but fluids must be chosen carefully to prevent complications.
Which should the nurse instruct children to do to stop the spread of influenza in the classroom? Select all that apply
Explanation
Influenza spreads through respiratory droplets and contaminated surfaces. The most effective ways to stop transmission in schools are hand hygiene, respiratory etiquette, and annual vaccination. Staying hydrated supports general health but does not prevent transmission.
Rationale for correct answers:
1. Staying home if they have a runny nose and cough prevents spreading infection in crowded environments like classrooms.
3. Washing their hands after sneezing interrupts transmission of respiratory droplets that carry the influenza virus.
4. Having a flu shot annually is the most effective method of preventing influenza and community outbreaks.
Rationale for incorrect answers:
2. Washing their hands after using the restroom is important for general hygiene but not specific to influenza prevention.
5. Drinking lots of water during the day helps hydration but does not reduce transmission risk.
Take home points
- Influenza spreads mainly through respiratory droplets (coughing, sneezing, close contact).
- Best prevention: staying home when sick, handwashing after contact with secretions, and annual vaccination.
- Supportive habits like hydration are good for recovery but do not stop the spread.
- Nurses should focus on infection control education for children, families, and schools to limit outbreaks.
A nurse is working at a telephone health service. Which advice should the nurse give to a client who has had 3 days of symptoms that strongly suggest influenza?
Explanation
Influenza, commonly called the flu, is a highly contagious viral infection that affects your respiratory system, including the nose, throat, and lungs. It causes fever, cough, malaise, sore throat, and body aches. It’s caused by influenza viruses, primarily types A and B, which circulate seasonally and can lead to widespread outbreaks.
Rationale for correct answer:
2. Supportive care is the primary management at this stage. Rest and adequate hydration help the body fight the infection, reduce fever, and prevent complications such as dehydration. Antivirals would no longer be effective since symptoms started more than 48 hours ago.
Rationale for incorrect answers:
1. Return to work after another day of rest is too soon. Clients with influenza should remain home until at least 24 hours after the fever resolves without antipyretics, to prevent spreading infection.
3. Use over-the-counter antihistamines may reduce nasal symptoms but are not first-line advice. Hydration and rest are more important.
4. The flu vaccine is preventive, not therapeutic. It cannot help once the infection is present.
Take home points
- Best advice for influenza after 3 days: rest, hydration, and supportive care.
- Antivirals are only effective if started within 48 hours of symptom onset.
- Clients should avoid returning to work/school until fever-free for 24 hours without medications.
Exams on Upper Respiratory Tract Infections
Custom Exams
Login to Create a Quiz
Click here to loginLessons
 Naxlex
Just Now
Naxlex
Just Now
Notes Highlighting is available once you sign in. Login Here.
Objectives
- Understand the common upper respiratory tract infections (URTIs) in children, including their etiology, pathophysiology, and clinical manifestations.
- Differentiate between various URTIs, such as acute viral nasopharyngitis, streptococcal pharyngitis, tonsillitis, infectious mononucleosis, and influenza, based on their unique signs and symptoms.
- Understand the diagnostic evaluation and therapeutic management for each specific URTI, including the appropriate use of antibiotics for bacterial infections and supportive care for viral illnesses.
- Understand the indications for tonsillectomy and adenoidectomy, and the comprehensive pre-operative, intra-operative, and post-operative care required.
- Identify and implement key nursing care management strategies for children with URTIs.
- Understand the critical complications associated with specific URTIs, such as rheumatic fever, post-streptococcal glomerulonephritis, and splenic rupture in infectious mononucleosis.
- Educate caregivers on home care measures, prevention strategies, and when to seek immediate medical attention for worsening symptoms or complications.
- Identify key nursing diagnoses and interventions for children with URTIs.
Introduction
- Upper Respiratory Tract Infections (URTIs) are a group of the most prevalent acute illnesses affecting the pediatric population, accounting for a significant number of doctor visits, hospitalizations, and school absences.
- These infections target the anatomical structures of the upper airway, including the nose, paranasal sinuses, pharynx, larynx, and tonsils.
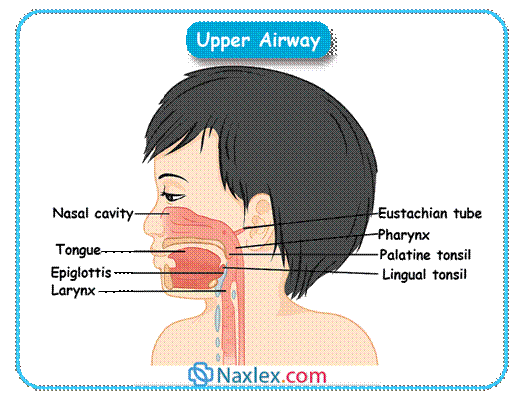
- While URTIs are generally self-limiting, they can lead to serious complications and distress for both the child and their caregivers.
- Understanding these illnesses is paramount for any healthcare professional, especially nurses, who are often the first point of contact and play a crucial role in assessment, management, and family education.
- While most URTIs are viral and self-limiting, some can be bacterial and require specific treatment to prevent serious complications.
- Children, especially those in daycare or school, are highly susceptible to URTIs due to their developing immune systems and close contact with peers. Hand hygiene is paramount in the prevention of spread of URTIs.
- While URTIs share some overlapping symptoms, their etiologies, potential complications, and management strategies differ significantly.
Acute Viral Nasopharyngitis
- Acute viral nasopharyngitis, commonly known as the common cold, is the most frequent infectious disease in humans.
Incidence
- Very High: Children experience an average of 6-10 colds per year, with infants and toddlers having even more. This frequency decreases with age as immunity develops.
- Seasonal Peaks: More common during colder months (e.g., in Kenya, during long rainy seasons like March-May and short rainy seasons like Oct-Dec), but can occur year-round.
Pathophysiology
- The virus enters the respiratory tract, primarily through the nasal passages or conjunctiva, and replicates in the epithelial cells of the nasopharynx. This leads to an inflammatory response, causing local tissue edema, increased mucus production, and vasodilation.
Etiology
- Viruses: Over 200 different viruses can cause the common cold.
- Rhinoviruses: Most common (30-80%).
- Coronaviruses: (10-15%).
- Adenoviruses, Respiratory Syncytial Virus (RSV), Parainfluenza viruses, Enteroviruses, Metapneumovirus: Also significant contributors.
Clinical Manifestations
Symptoms typically appear 1-3 days after exposure and last for about 7-10 days, though some can linger for weeks.
- Initial:
- Sore throat or "scratchy" throat.
- Rhinorrhea (runny nose): Clear, watery discharge initially, becoming thicker and sometimes yellowish/greenish.
- Sneezing.
- Irritability (in infants/young children).
- Progressive:
- Nasal congestion: Leading to mouth breathing, especially in infants.
- Cough: Often develops later, can be mild to severe.
- Low-grade fever: More common in infants and young children.
- Decreased appetite.
- Headache, muscle aches (malaise): More common in older children and adults.
Diagnostic Evaluation
- Clinical Diagnosis: Primarily based on characteristic signs and symptoms. No specific laboratory tests are routinely needed.
- Exclusion: Rule out other conditions with similar symptoms such as allergies, influenza, bacterial infections.
Therapeutic Management
- Supportive Care: No cure for the common cold; treatment focuses on symptom relief.
- Hydration: Encourage oral fluids (water, juice, electrolyte solutions) to prevent dehydration and thin secretions.
- Rest: Promote adequate rest.
- Humidification: Cool-mist humidifier in the child's room can soothe irritated airways and loosen secretions.
- Nasal Saline Drops/Spray: To loosen mucus, followed by suctioning for infants/young children.
- Antipyretics/Analgesics: Acetaminophen or ibuprofen for fever, aches, and pain. Aspirin is contraindicated in children due to the risk of Reye's syndrome.
- Avoid: Over-the-counter (OTC) cough and cold medications (decongestants, antitussives) are generally not recommended for children under 6 years old due to potential serious side effects and lack of proven efficacy.
- Honey: Can be used for cough relief in children over 1 year of age. Honey should be avoided in infants due to the risk of infantile botulism.
Prevention
- Hand Hygiene: Frequent and thorough handwashing with soap and water is the most effective prevention.
- Avoid Touching Face: Discourage touching eyes, nose, and mouth.
- Avoid Sick Individuals: Limit exposure to people with colds.
- Good Nutrition & Rest: Support a healthy immune system.
- Vaccinations: Keep up-to-date with routine childhood immunizations.
Nursing Care Management
- Assessment:
- Monitor respiratory status (rate, effort, presence of retractions, nasal flaring).
- Assess hydration status (mucous membranes, urine output, fontanelles in infants).
- Temperature monitoring.
- Assess for complications (e.g., ear pain, worsening cough, difficulty breathing).
- Interventions:
- Airway Management: Nasal saline and suctioning for infants; elevate head of bed for older children.
- Hydration: Offer fluids frequently.
- Comfort: Administer antipyretics as ordered. Provide a cool-mist humidifier.
- Education:
- Teach caregivers about symptom management at home.
- Emphasize hand hygiene.
- Advise on when to seek medical attention (e.g., difficulty breathing, high fever, signs of ear infection, lethargy).
- Dispelling myths about antibiotics for viral infections.
- Nursing Insight: Educate parents that green or yellow nasal discharge does not automatically mean a bacterial infection; it's a normal progression of a viral cold.
Acute Streptococcus Pharyngitis
- Acute streptococcal pharyngitis is a bacterial infection of the pharynx caused by Group A Streptococcus (Streptococcus pyogenes). It's important to treat to prevent complications like rheumatic fever and post-streptococcal glomerulonephritis.
Incidence
- Common in School-aged Children: Most prevalent in children 5-15 years old. Less common under 3 years.
- Seasonal: Peaks in late fall, winter, and early spring.
Pathophysiology
The bacteria adhere to the pharyngeal epithelium, releasing toxins and enzymes that cause inflammation and tissue damage. This leads to the characteristic symptoms of strep throat.
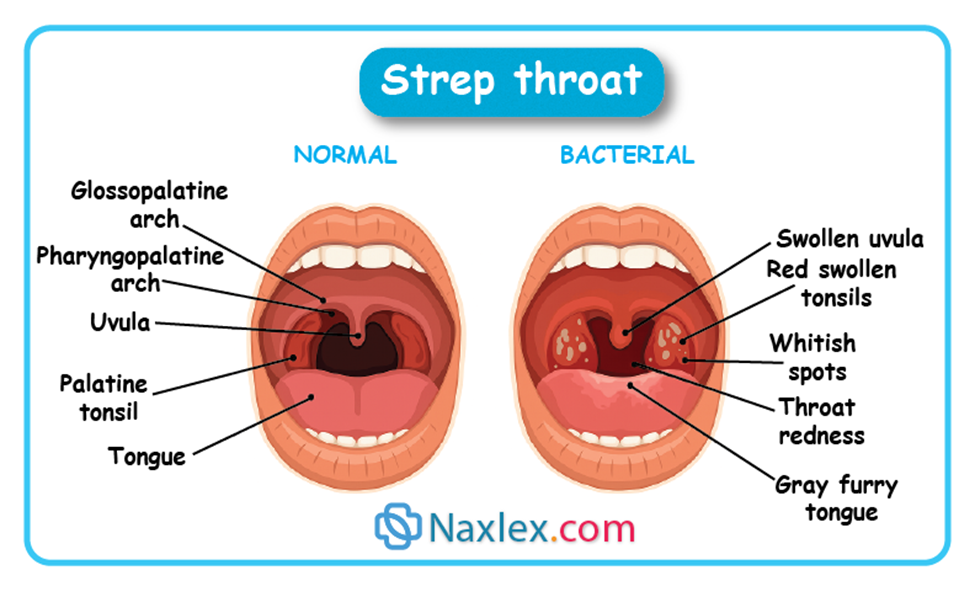
Etiology
- Bacteria: Group A β-hemolytic Streptococcus (Streptococcus pyogenes).
- Transmission: Droplet transmission from respiratory secretions of infected individuals (coughing, sneezing).
Clinical Manifestations
Symptoms usually have an abrupt onset.
- Abrupt onset of sore throat.
- Pain on swallowing.
- Fever (often high).
- Headache.
- Abdominal pain, nausea, vomiting: Common in younger children.
- Beefy red pharynx.
- Palatal petechiae: Small red spots on the soft palate.
- White or yellow exudate (pus) on tonsils and pharynx.
- Swollen, tender anterior cervical lymph nodes.
- Absent cold symptoms: (e.g., runny nose, cough, hoarseness) – this helps differentiate from viral infections.
- Scarlatiniform rash (Scarlet Fever): Fine, sandpaper-like rash, especially on the trunk and extremities, with flushed cheeks and circumoral pallor (pale area around the mouth). This is a complication of strep throat.
Diagnostic Evaluation
- Rapid Strep Test (Rapid Antigen Detection Test - RADT):
- Detects GAS antigens from a throat swab.
- Results within minutes.
- High specificity, but variable sensitivity.
- Positive RADT: Confirms strep throat, treatment initiated.
- Negative RADT in children: Should be confirmed with a throat culture due to potential for false negatives and the importance of treating GAS infections. Adults with a negative RADT generally do not require a confirmatory culture.
- Throat Culture:
- Gold standard for diagnosis.
- Takes 24-48 hours for results.
Nursing Insight: Ensure proper technique for throat swab collection to get an adequate sample. Touch both tonsils and posterior pharynx.
Therapeutic Management
- Antibiotics: Crucial to prevent complications.
- Penicillin V: Drug of choice (10 days orally).
- Amoxicillin: Often preferred for taste and once-daily dosing.
- Penicillin G Benzathine (Bicillin L.A.): Single intramuscular injection for non-compliant patients or if oral adherence is a concern. Very painful injection, often mixed with lidocaine.
Drug Alert: Never administer penicillin G procaine or penicillin G benzathine suspensions intravenously; they may cause embolism or toxic reaction with ensuing death in minutes. Instead, administer these medications deep into the muscle tissue to decrease localized reactions and pain.
-
- Erythromycin or Azithromycin: For penicillin-allergic patients.
- Symptomatic Relief:
- Analgesics/Antipyretics: Acetaminophen or ibuprofen for pain and fever.
- Warm salt water gargles: For older children.
- Cool or warm drinks, soft foods.
Nursing Care Management
- Assessment:
- Monitor for signs of dehydration.
- Assess pain level.
- Observe for rash (Scarlet Fever).
- Monitor for complications (e.g., worsening symptoms, joint pain, dark urine - signs of rheumatic fever or glomerulonephritis).
- Interventions:
- Administer antibiotics as prescribed: Emphasize completing the full 10-day course, even if symptoms improve, to prevent complications.
- Pain Management: Offer analgesics, provide soothing liquids/foods.
- Hydration: Encourage fluids.
- Infection Control: Educate on hand hygiene, avoiding sharing utensils/drinks.
- Education:
- Explain the importance of antibiotic adherence.
- When the child can return to school (usually 24 hours after starting antibiotics and fever-free).
- Signs and symptoms of potential complications (e.g., rheumatic fever - joint pain, cardiac issues; glomerulonephritis - dark urine, swelling).
Prevention
- Hand Hygiene: Frequent handwashing.
- Avoid Sharing: Do not share eating utensils, cups, or food.
- Stay Home When Sick: Prevent spread, especially during the first 24 hours of antibiotic treatment.
- Prompt Treatment: Early diagnosis and treatment prevent complications and reduce transmission.
Tonsillitis
- Tonsillitis is an inflammation or infection of the palatine tonsils. It can be viral or bacterial.
Incidence
- Common in Children: Especially school-aged children. Declines with age.
- Viral: More common.
- Bacterial: Often Group A Streptococcus.
Pathophysiology
Infection of the tonsils leads to inflammation, edema, and sometimes exudate. The tonsils are lymphoid tissues that play a role in immunity, trapping pathogens entering the respiratory tract. When overwhelmed, they become infected.
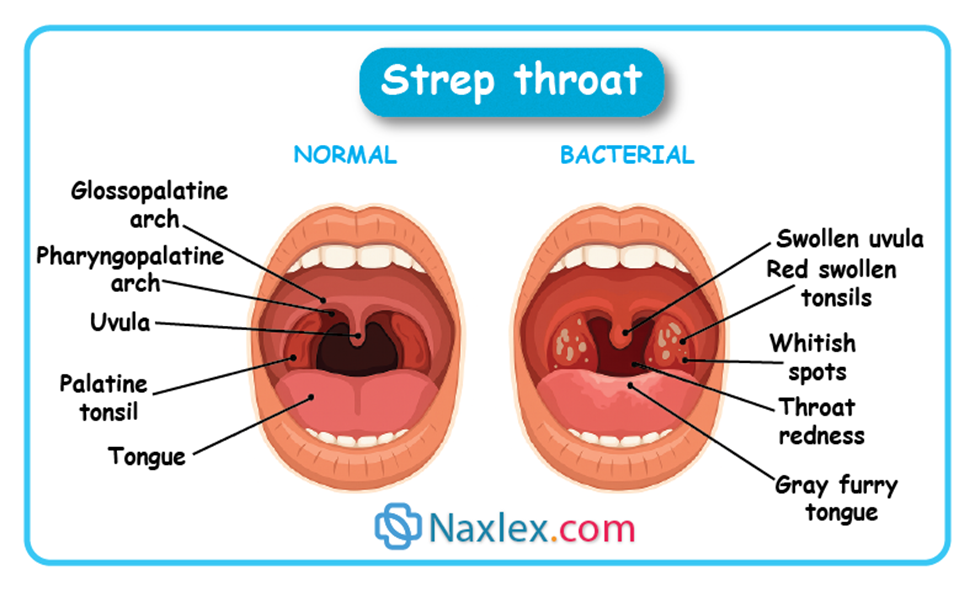
Etiology
- Viruses: Adenoviruses, Epstein-Barr virus (EBV), enteroviruses, influenza, parainfluenza.
- Bacteria: Most commonly Streptococcus pyogenes (Group A Strep), but also Staphylococcus aureus, Haemophilus influenzae, Mycoplasma pneumoniae.
Clinical Manifestations
Symptoms vary depending on the cause (viral vs. bacterial) and the child's age.
- Sore throat: Often severe, making swallowing difficult.
- Difficulty swallowing (dysphagia).
- Fever: Can be high.
- Headache.
- Mouth breathing: Due to enlarged tonsils obstructing the airway.
- Snoring/Obstructive sleep apnea: In severe cases with significant tonsillar hypertrophy.
- Muffled voice.
- Halitosis (bad breath).
- Abdominal pain, nausea, vomiting: Especially in younger children with strep tonsillitis.
- Enlarged, red tonsils: May have white or yellow exudate (pus).
- Tender, enlarged cervical lymph nodes.
Diagnostic Evaluation
- Clinical Examination: Visual inspection of the throat.
- Rapid Strep Test/Throat Culture: To rule out or confirm Group A Strep infection.
- Monospot Test: If infectious mononucleosis is suspected (e.g., older child with lymphadenopathy, fatigue, splenomegaly).
Therapeutic Management
A. Medical Treatment
- Viral Tonsillitis:
- Supportive Care: Similar to the common cold.
- Pain relief: Acetaminophen or ibuprofen.
- Hydration: Encourage fluids.
- Rest.
- Warm salt water gargles: For older children.
- Bacterial Tonsillitis (Strep):
- Antibiotics: Penicillin V or amoxicillin for 10 days. Erythromycin for penicillin-allergic individuals.
- Symptomatic relief: As above.
B. Surgical Treatment: Tonsillectomy and Adenoidectomy (T&A)
Removal of the palatine tonsils (tonsillectomy) and pharyngeal tonsils (adenoids) (adenoidectomy).
Indications for T&A:
- Recurrent Tonsillitis:
- 7 or more episodes in the preceding year.
- 5 or more episodes per year in the preceding 2 years.
- 3 or more episodes per year in the preceding 3 years.
- Definition of episode: Sore throat and one of the following: fever >38.3°C, cervical lymphadenopathy (>2cm), tonsillar exudate, or positive Group A Strep test.
- Obstructive Sleep Apnea (OSA): Due to tonsillar and/or adenoidal hypertrophy causing upper airway obstruction. This is the most common indication for T&A in children today.
- Peritonsillar Abscess: Not responding to antibiotics or recurrent.
- Malocclusion/Oronasal facial growth abnormalities: Due to chronic mouth breathing from enlarged adenoids.
- Chronic Otitis Media with Effusion (OME): Adenoidectomy alone or with T&A can improve Eustachian tube function.
- Chronic Tonsillitis: Persistent sore throat, halitosis, and cryptic tonsils that are not responsive to medical management.
Pre-operative Care:
- Assessment:
- Complete history and physical examination.
- Allergies, current medications.
- Bleeding disorders (e.g., hemophilia, von Willebrand disease), family history of bleeding.
- Ask specifically about NSAID use (ibuprofen, aspirin) in the past 1-2 weeks due to increased bleeding risk.
- Loose teeth (risk of aspiration during intubation).
- Baseline vital signs.
- Diagnostic Tests:
- Complete Blood Count (CBC) with differential.
- Coagulation studies (PT, PTT, INR) if a bleeding disorder is suspected or patient on anticoagulants.
- Type and screen (rarely needed unless high bleeding risk).
- Preparation:
- NPO (Nothing by Mouth): For specified time before surgery (usually 6-8 hours for solids, 2-4 hours for clear liquids) to prevent aspiration.
- Education: Explain the procedure simply to the child (if age-appropriate) and parents. Discuss expectations for recovery, pain, and diet.
- Consent: Ensure informed consent is signed.
Intra-operative Care:
- Positioning: Supine with head extended (Rose position) to provide clear surgical field.
- Anesthesia: General anesthesia.
- Procedure: Tonsils and/or adenoids are removed using various techniques (e.g., electrocautery, laser, microdebrider). Meticulous hemostasis is crucial.
Post-operative Care (Immediate):
- Positioning:
- Initially prone or side-lying: To facilitate drainage of secretions and prevent aspiration.
- Once fully awake and stable: Head of the bed elevated.
- Vital Signs: Monitor frequently (every 15-30 minutes initially) for stability, signs of hemorrhage such as increased pulse, decreased BP, and pallor, or respiratory distress.
- Airway Management:
- Observe for signs of respiratory obstruction such as stridor, retractions, and nasal flaring.
- Keep suction available but avoid deep suctioning unless necessary to prevent trauma to the surgical site.
- Hemorrhage:
- Most critical complication.
- Signs: Frequent swallowing, even while sleeping, is the earliest sign of bleeding. Also, bright red vomiting, pallor, restlessness, increased heart rate, decreased blood pressure (late sign).
- Intervention: Report immediately to surgeon. Position on side. Prepare for potential return to OR.
- Pain Management:
- Administer prescribed analgesics (e.g., acetaminophen with codeine, ibuprofen after initial bleeding risk passes, hydrocodone).
- Avoid aspirin or NSAIDs initially due to increased bleeding risk.
- Ice collar to the neck.
- Hydration/Diet:
- Start with clear, cool liquids (water, clear juice, ice chips) once fully awake and gag reflex returns. This should be provided within the first 24 hours. Avoid red-colored liquids as they can mimic blood.
- Advance to soft, bland foods such as pudding, gelatin, mashed potatoes, well-cooked pasta, 1-2 days postoperative.
- Avoid: Hot foods, spicy foods, acidic juices, crunchy foods (chips, toast, pretzels) that can irritate the surgical site or dislodge clots. Avoid milk products such as milk, ice cream, and pudding initially because they coat the throat causing the child to cough to clear the throat.

- Nausea/Vomiting: Common. Administer antiemetics as ordered.
Pre-operative Nursing Diagnoses:
- Anxiety (child and parents) related to surgical procedure and unfamiliar environment.
- Deficient Knowledge related to surgical procedure and post-operative care.
Intra-operative Nursing Diagnoses:
- Risk for Aspiration related to NPO status and general anesthesia.
- Risk for Injury related to surgical procedure and positioning.
Post-operative Nursing Diagnoses:
- Acute Pain related to surgical incision.
- Risk for Hemorrhage related to surgical site.
- Risk for Deficient Fluid Volume related to decreased oral intake and potential bleeding.
- Impaired Oral Mucous Membrane related to surgical trauma.
- Risk for Ineffective Airway Clearance related to edema or bleeding.
- Deficient Knowledge (caregiver) related to home care and signs of complications.
Caregiver Education (Home Care):
- Pain Management: Administer prescribed pain medication regularly, even if the child seems okay, to stay ahead of the pain. Use a timer for doses.
- Hydration: Emphasize fluid intake to prevent dehydration.
- Diet:
- Day 1-2: Clear, cool liquids, ice pops, popsicles, diluted juice, bland pureed foods.
- Day 3-7: Soft, bland foods, like mashed potatoes, scrambled eggs, well-cooked pasta, soft cereals, pudding, cooked vegetables.
- Avoid for 2 weeks: Crunchy, hard, spicy, acidic, or hot foods. Examples to avoid: chips, pretzels, toast, crackers, highly acidic juices (orange, grapefruit), carbonated drinks.
- Activity:
- Rest for the first few days.
- Avoid strenuous activity, heavy lifting, or vigorous play for 1-2 weeks.
- Avoid blowing nose vigorously or clearing throat frequently.
- Bleeding:
- Most critical warning sign: Frequent swallowing. Teach parents to check the back of the throat with a flashlight if concerned.
- When to call: Any signs of bleeding (bright red blood, frequent swallowing, vomiting bright red blood), fever, increased pain not controlled by medication, refusal to drink.
- Do not give the child any straws, forks, or sharp objects that can be put into the mouth.
- Bad breath/Ear pain: Common for about a week. Ear pain is referred pain from the throat.
- Fever: Low-grade fever is common for 1-2 days. Report persistent high fever.
- Follow-up: Schedule follow-up appointment with the surgeon.
Nursing Insight: Using a straw creates negative pressure in the mouth and throat. This suction can dislodge clots that are forming at the surgical site (tonsillar beds). If the clot is disturbed, it can lead to hemorrhage, one of the most serious postoperative complications of a tonsillectomy. Furthermore, the sucking motion can irritate the healing tissues in the oropharynx. This delays healing and increases discomfort.
Complications of Surgery:
- Hemorrhage:
- Primary (within 24 hours): Most common. Typically due to dislodgement of clot or inadequate hemostasis.
- Secondary (5-10 days post-op): Occurs when the scab separates. Can be severe.
- Management: Return to OR for cauterization or ligation.
- Dehydration: Due to pain making swallowing difficult.
- Infection: Local wound infection.
- Airway Obstruction: Due to edema or bleeding.
- Voice Change: Temporary, usually resolves. Rarely permanent.
- Pharyngeal Stenosis: Rare, due to excessive tissue removal.
Nursing Insight: For a child post-tonsillectomy, "frequent swallowing" is a red flag, even if they're sleeping. Wake them gently and observe the back of their throat if you suspect bleeding.
Drug Alert: Codeine is contraindicated in pediatric patients post tonsillectomy and adenoidectomy. In 2012 the US Food and Drug Administration issued a Drug Safety Communication that codeine use in certain children after tonsillectomy and/or adenoidectomy may lead to rare but life-threatening adverse events or death. In 2013 a boxed warning (the Food and Drug Administration’s strongest) was added to codeine drug labels to warn about the risks associated with it and to contraindicate its use in this population.
Infectious Mononucleosis
- Infectious mononucleosis is an acute infectious disease caused by the Epstein-Barr Virus (EBV), primarily affecting adolescents and young adults.
Incidence
- Common in Adolescents/Young Adults: Peaks between 15-24 years of age.
- Rare in Young Children: If infected, often asymptomatic or mild.
Pathophysiology
- EBV is a herpesvirus that primarily infects B lymphocytes and epithelial cells of the oropharynx. The virus remains latent in B cells throughout life. During primary infection, there is a proliferation of infected B cells and a robust cytotoxic T-cell response, leading to characteristic symptoms.
Etiology
- Epstein-Barr Virus (EBV): A type of herpesvirus.
- Transmission: Primarily through saliva ("kissing disease"), but also through sharing drinks, utensils. Less contagious than the common cold.
- Incubation Period: Long, 30-50 days.
Clinical Manifestations
Highly variable. The classic triad of symptoms includes:
- Fever: Often prolonged (weeks).
- Pharyngitis: Severe sore throat, often with exudative tonsillitis.
- Lymphadenopathy: Generalized, especially posterior cervical, axillary, and inguinal nodes. Nodes are often tender.
- Fatigue/Malaise: Profound and can be debilitating, lasting for weeks to months.
- Splenomegaly: Enlarged spleen (in 50-60% of cases).
- Hepatomegaly: Enlarged liver (in 10-15% of cases).
- Rash: Maculopapular rash, especially if treated with ampicillin or amoxicillin.
- Palatal petechiae: Small red spots on the soft palate.
- Periorbital edema: Swelling around the eyes.
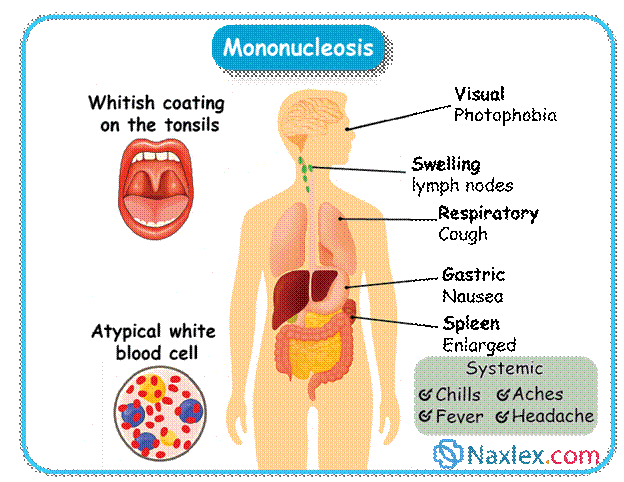
Diagnostic Evaluation
- Monospot Test (Heterophile Antibody Test):
- Detects heterophile antibodies, which appear during the first 2-3 weeks of illness.
- Positive: Confirms mono in older children/adults.
- Negative in young children: May need further testing as young children don't always produce heterophile antibodies.
- EBV-Specific Antibody Tests:
- Detect specific antibodies (e.g., VCA-IgM, VCA-IgG, EBNA) to confirm EBV infection, especially in uncertain cases or young children.
- Complete Blood Count (CBC):
- Lymphocytosis: Increased white blood cells, predominantly lymphocytes.
- Atypical Lymphocytes: Characteristic abnormal lymphocytes seen on blood smear.
- Liver Function Tests (LFTs): May be elevated due to liver involvement.
Therapeutic Management
- Supportive Care: No specific antiviral treatment.
- Rest: Crucial for recovery, especially during the acute phase. Activity should be gradually increased.
- Hydration: Encourage fluids.
- Pain Relief: Acetaminophen or ibuprofen for fever, sore throat, and body aches.
- Corticosteroids: May be used in severe cases (e.g., significant airway obstruction from tonsillar hypertrophy, severe thrombocytopenia, hemolytic anemia, CNS involvement) to reduce inflammation.
- Avoid:
- Antibiotics: Ineffective against viruses. Avoid ampicillin/amoxicillin as they cause a widespread rash in mononucleosis patients.
Prognosis
- Self-limiting: Most individuals recover within 2-4 weeks.
- Fatigue: Can persist for several months.
- Full recovery: Common, but the virus remains latent.
Complications
- Splenic Rupture: Most serious complication, though rare. Occurs due to splenomegaly, making the spleen fragile. Can be spontaneous or result from trauma.
- Symptoms: Sudden severe abdominal pain (especially left upper quadrant), left shoulder pain (Kehr's sign), signs of hypovolemic shock.
- Management: Medical emergency.
- Resumption of Contact Sports: Crucial education point. Avoid contact sports and strenuous activities for at least 3-4 weeks from the onset of symptoms, or until splenomegaly has resolved (confirmed by physical exam or ultrasound). Some recommend longer (up to 6-8 weeks).
- Airway Obstruction: Due to massive tonsillar and adenoidal hypertrophy.
- Neurological Complications: Meningitis, encephalitis, Guillain-Barré syndrome (rare).
- Hematologic Complications: Hemolytic anemia, thrombocytopenia (rare).
- Hepatitis: Mild liver inflammation is common.
- Peritonsillar Abscess.
Nursing Care Management
- Assessment:
- Monitor for signs of respiratory distress (if tonsils are enlarged).
- Assess for splenomegaly/hepatomegaly (gentle palpation).
- Monitor for abdominal pain (signs of splenic rupture).
- Assess fatigue level and activity tolerance.
- Interventions:
- Rest: Emphasize the importance of adequate rest.
- Pain Relief: Administer analgesics.
- Hydration: Encourage fluids.
- Education:
- Explain the viral nature of the illness and the importance of supportive care.
- Educate on avoidance of contact sports and strenuous activity (3-4 weeks or until spleen size normalizes) to prevent splenic rupture.
- Advise on symptom progression and when to seek medical attention (e.g., severe abdominal pain, worsening breathing, yellow skin/eyes).
- Explain the contagiousness and importance of not sharing drinks/utensils.
- Discuss the prolonged fatigue.
- Nursing Insight: Always ask about contact sports when educating a teen with mono. This seemingly benign instruction can prevent a life-threatening emergency!
Influenza
- Influenza is a highly contagious acute viral infection of the respiratory tract caused by influenza viruses.
Incidence
- Seasonal Epidemics: Occur annually, typically in colder months. In Kenya, this can align with rainy seasons.
- Pandemics: Can occur periodically when new, highly virulent strains emerge.
- Impact: Causes significant morbidity and mortality, especially in young children, elderly, and those with chronic health conditions.
Pathophysiology
- Influenza viruses primarily target and replicate in the respiratory epithelial cells, causing cellular destruction and inflammation. This leads to the characteristic symptoms and can predispose individuals to secondary bacterial infections.
Etiology
- Influenza Viruses:
- Type A: Most common and causes severe epidemics/pandemics.
- Type B: Causes less severe, more localized epidemics.
- Type C: Causes mild illness, not associated with epidemics.
- Transmission: Droplet transmission (coughing, sneezing) and direct contact with contaminated surfaces. Highly contagious.
- Incubation Period: 1-4 days.
Clinical Manifestations
Symptoms are typically more severe and abrupt in onset than the common cold.
- Abrupt onset of:
- Fever: Often high (39-40°C), chills.
- Headache.
- Myalgia (muscle aches): Often severe.
- Malaise/Fatigue: Profound.
- Sore throat.
- Dry, hacking cough: Can be severe and persistent.
- Nasal congestion/Rhinorrhea: Less prominent than common cold.
- Nausea, vomiting, diarrhea: More common in children.
Diagnostic Evaluation
- Rapid Influenza Diagnostic Tests (RIDTs):
- Detect influenza viral antigens from nasal swab, throat swab, or nasal aspirate.
- Results within 15-30 minutes.
- Limitations: Variable sensitivity (can have false negatives), better specificity. A negative RIDT doesn't rule out flu, especially during peak season.
- Reverse Transcription Polymerase Chain Reaction (RT-PCR):
- More sensitive and specific than RIDTs.
- Used for definitive diagnosis, especially in hospitalized patients or for public health surveillance.
- Results take longer.
- Clinical Diagnosis: Often based on characteristic symptoms during flu season, especially if other community members are infected.
Therapeutic Management
- Antiviral Medications:
- Neuraminidase Inhibitors: Oseltamivir (Tamiflu), Zanamivir (Relenza), Peramivir (Rapivab).
- Mechanism: Inhibit viral replication.
- Effectiveness: Most effective when started within 48 hours of symptom onset. Can shorten duration of illness, reduce severity, and prevent complications.
- Indications: High-risk individuals (young children, elderly, chronic medical conditions), severe illness, hospitalized patients.
- Supportive Care:
- Rest: Ample rest.
- Hydration: Encourage fluids to prevent dehydration.
- Antipyretics/Analgesics: Acetaminophen or ibuprofen for fever, headache, muscle aches.
- Humidifier: To soothe cough.
Prevention
- Influenza Vaccine:
- Annual vaccination: Recommended for everyone 6 months of age and older.
- Types: Inactivated influenza vaccine (IIV) via injection, or Live Attenuated Influenza Vaccine (LAIV) via nasal spray (for healthy individuals 2-49 years old, not pregnant).
- Timing: Best administered before the flu season begins (e.g., by October/November in the Northern Hemisphere).
- Even if the vaccine doesn't completely prevent flu, it significantly reduces the severity of illness and risk of complications.
- Hand Hygiene: Frequent handwashing with soap and water or alcohol-based hand sanitizer.
- Avoid Touching Face: Reduce self-inoculation.
- Avoid Sick Individuals: Limit close contact.
- Cover Coughs and Sneezes: Use a tissue or inner elbow.
- Stay Home When Sick: To prevent spreading the virus.

Nursing Care Management
- Assessment:
- Monitor respiratory status (rate, effort, oxygen saturation).
- Assess for dehydration.
- Monitor temperature and pain.
- Observe for signs of complications (e.g., secondary bacterial pneumonia, otitis media, worsening respiratory distress).
- Interventions:
- Administer antiviral medications: If prescribed, emphasize starting within 48 hours.
- Symptom Management: Provide antipyretics, analgesics, cool mist humidifier.
- Hydration: Offer fluids frequently.
- Rest: Encourage rest.
- Infection Control: Isolation precautions if hospitalized, educate on hand hygiene, cough etiquette, staying home when sick.
- Education:
- Importance of annual flu vaccination.
- Symptom management at home.
- When to seek medical attention (e.g., difficulty breathing, chest pain, sudden dizziness, severe vomiting, signs of dehydration).
- Differentiation between cold and flu symptoms.
- Nursing Insight: When a child presents with sudden high fever, severe body aches, and fatigue during flu season, consider influenza even if initial rapid tests are negative.
Summary
- Upper Respiratory Tract Infections (URTIs) are a broad category of illnesses affecting the nose, pharynx, larynx, and tonsils, representing some of the most common reasons for healthcare visits, especially in children.
- The Common Cold (Acute Viral Nasopharyngitis) is the most frequent URTI, caused by over 200 viruses, predominantly rhinoviruses. Its incidence is highest in young children (6-10 colds/year), decreasing with age. Antibiotics are ineffective, and OTC cough/cold medications are discouraged in young children due to safety concerns. Prevention hinges on rigorous hand hygiene and avoiding touching the face.
- Acute Streptococcal Pharyngitis (Strep Throat) is a bacterial infection caused by Group A Streptococcus (Streptococcus pyogenes), primarily affecting school-aged children. It's significant due to its potential for serious non-suppurative complications like rheumatic fever and post-streptococcal glomerulonephritis. Antibiotic therapy, typically penicillin or amoxicillin for 10 days, is essential to eradicate the bacteria, prevent complications, and reduce contagiousness.
- Tonsillitis, the inflammation of the palatine tonsils, can be viral or bacterial. It presents with a severe sore throat, difficulty swallowing, fever, and sometimes mouth breathing due to enlarged tonsils. Medical management is supportive for viral cases and antibiotics for bacterial. Surgical management (Tonsillectomy and Adenoidectomy - T&A) is considered for specific indications.
- Infectious Mononucleosis ("Mono"), caused by the Epstein-Barr Virus (EBV), primarily affects adolescents and young adults. It's known for its classic triad of fever, severe pharyngitis (often with exudative tonsillitis), and generalized lymphadenopathy. Splenomegaly is common and is the basis for the most serious complication: splenic rupture.
- Influenza (Flu) is a highly contagious viral infection that causes annual epidemics. Symptoms are abrupt and more severe than the common cold, including high fever, chills, headache, severe myalgia, profound fatigue, and a dry, hacking cough. Antiviral medications (e.g., oseltamivir) are effective if started within 48 hours of symptom onset, especially in high-risk individuals, to reduce severity and complications. Supportive care (rest, hydration, analgesics) is also essential. The most effective preventive measure is annual influenza vaccination for all individuals 6 months and older.
Naxlex
Videos
Login to View Video
Click here to loginTake Notes on Upper Respiratory Tract Infections
This filled cannot be empty
Join Naxlex Nursing for nursing questions & guides! Sign Up Now


