Ati Concept Of Nursing Proctored Exam 2
Ati Concept Of Nursing Proctored Exam 2
Total Questions : 47
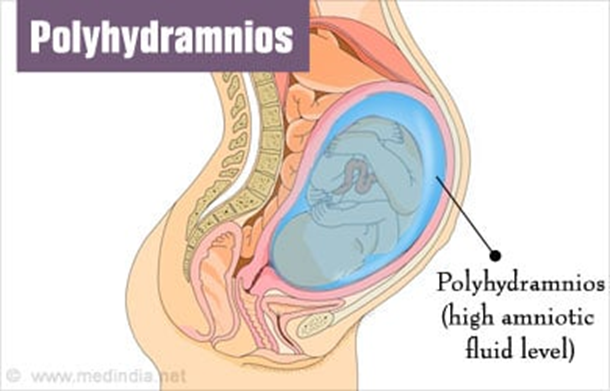
Showing 10 questions Sign up for moreA nurse is caring for a client who was admitted to the maternity unit at 38 weeks of gestation and who is experiencing polyhydramnios. The nurse should recognize that this diagnosis means which of the following?
Explanation
Explanation:
A. An excessive amount of amniotic fluid is present.
Polyhydramnios is defined as an excessive accumulation of amniotic fluid within the amniotic sac surrounding the fetus. This condition can occur due to various factors, including fetal abnormalities, maternal health conditions such as diabetes or gestational diabetes, multiple gestations (twins, triplets, etc.), or idiopathic causes where no specific underlying condition is identified. The increased volume of amniotic fluid can be detected through ultrasound examinations, where amniotic fluid index (AFI) measurements are taken to assess the quantity of fluid present. Polyhydramnios is typically diagnosed when the AFI exceeds a certain threshold.
B. The client is carrying more than one fetus.
While it's true that multiple gestations, such as twins or triplets, can sometimes lead to polyhydramnios, the presence of polyhydramnios does not automatically indicate a multiple pregnancy. Polyhydramnios can occur in singleton pregnancies as well, particularly due to other factors like fetal anomalies, maternal health issues, or idiopathic reasons.
C. The fetus is likely to have a congenital anomaly, be growth-restricted, or demonstrate fetal distress during labor.
Polyhydramnios can be associated with various fetal and maternal conditions, but it does not directly indicate specific fetal issues like congenital anomalies, growth restriction, or fetal distress during labor. However, polyhydramnios can sometimes coexist with these conditions or be a result of them. For example, certain fetal abnormalities, such as gastrointestinal obstructions, can lead to polyhydramnios due to impaired swallowing and absorption of amniotic fluid.
D. There is an elevated level of alpha-fetoprotein (AFP) in the amniotic fluid.
Elevated levels of alpha-fetoprotein (AFP) in the amniotic fluid are typically associated with neural tube defects (such as spina bifida) or abdominal wall defects (like gastroschisis or omphalocele) in the fetus. However, AFP levels are not directly related to the presence of polyhydramnios. AFP testing is usually done separately as part of prenatal screening tests to assess the risk of certain fetal abnormalities.
A nurse is preparing to measure the fundal height of a client who is at 22 weeks of gestation. At which location should the nurse expect to palpate the fundus?
Explanation
Explanation:
A. Slightly below the umbilicus:
Around 16-20 weeks of gestation, the fundal height is typically palpated slightly below the umbilicus. This corresponds to the level of the fundus before it starts rising significantly above the umbilicus as the pregnancy progresses.
B. 3 cm above the umbilicus:
At 22 weeks of gestation, the fundal height is expected to be approximately 3 cm above the umbilicus. This is a common estimation for the fundal height at this stage of pregnancy, as the uterus continues to grow and the fundus ascends in a predictable manner.
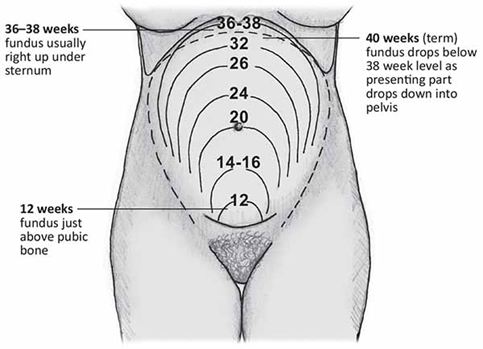
C. 3 cm below the umbilicus:
Palpating the fundus 3 cm below the umbilicus would typically correspond to an earlier gestational age, such as around 16-18 weeks. As pregnancy advances, the fundal height increases, and by 22 weeks, it should be well above the level of the umbilicus.
D. Slightly above the umbilicus:
This location is closer to where the fundal height is expected to be at later gestational ages, such as 24-26 weeks. However, at 22 weeks of gestation, the fundal height should not be palpated slightly above the umbilicus but rather around 3 cm above it.
Explanation
Explanation:
A. "Daily jogging for up to 30 minutes is fine throughout the pregnancy."
This response suggests that moderate-intensity exercise like jogging is safe throughout pregnancy. However, it's important to note that individual exercise recommendations can vary based on the woman's health status, pre-pregnancy fitness level, any pregnancy complications, and guidance from her healthcare provider. While moderate exercise is generally encouraged during pregnancy, it's crucial for the client to consult her healthcare provider for personalized recommendations.
B. "Activities that raise the body temperature, such as saunas and hot tubs, are safe until the third trimester."
This response addresses the importance of avoiding activities that can lead to overheating, such as using saunas or hot tubs, especially during the first trimester when fetal development is particularly sensitive. However, it doesn't specifically address general exercise guidelines.
C. "It is recommended that pregnant clients limit their exercise routine to stretching activities on a mat several times a week."
This response suggests a very conservative approach to exercise during pregnancy, focusing primarily on stretching activities. While stretching can be beneficial, it's important for pregnant individuals to engage in a variety of exercises, including aerobic and strength-training activities, as long as they are safe and appropriate for their pregnancy status.
D. "Exercising during pregnancy is not recommended."
This response is not accurate. Exercise during pregnancy is generally recommended and has numerous benefits for both the mother and baby, including improved cardiovascular health, reduced risk of gestational diabetes, enhanced mood, and better overall well-being. However, the type, intensity, and duration of exercise should be tailored to the individual's needs and guided by healthcare providers.
Explanation
Explanation:
A. "Don't worry. You will be fine once the baby is born."
This response may inadvertently dismiss the client's feelings of doubt and uncertainty. It assumes that the client's concerns will automatically resolve after childbirth, which may not be the case for everyone. It lacks acknowledgment of the client's current emotional state and does not offer meaningful support or guidance.
B. "Ambivalent feelings are quite common for women early in pregnancy."
This response acknowledges the client's feelings of doubt and uncertainty as valid and common experiences during early pregnancy. It normalizes her emotions, letting her know that she is not alone in feeling this way. By providing this validation, the nurse creates a supportive environment where the client can feel understood and accepted.
C. "Perhaps you should see a counselor to discuss these feelings further."
Suggesting counseling is a proactive and supportive approach. It recognizes that the client's emotions are complex and may benefit from professional guidance. Counseling offers a safe space for the client to explore her feelings, understand their root causes, and develop coping strategies. It demonstrates the nurse's commitment to the client's emotional well-being and encourages seeking help when needed.
D. "Have you spoken to your mother about these feelings?"
While seeking support from family members can be valuable, this response may not fully address the client's emotional needs. It assumes that talking to her mother will automatically resolve her concerns, which may not always be the case. Additionally, some clients may prefer discussing sensitive issues with a neutral third party or a trained counselor who can offer unbiased support and guidance.
Explanation
Explanation:
A. "This will occur between the fourth and fifth months of pregnancy."
This response is accurate and aligns with the typical timeframe for quickening, which is the first perception of fetal movements by the pregnant person. Quickening commonly occurs between the 16th and 20th week of pregnancy, corresponding to the fourth and fifth months. However, it's essential to note that the exact timing can vary from person to person and pregnancy to pregnancy.
B. "This will happen by the end of the first trimester of pregnancy."
This response is not entirely accurate. Quickening typically occurs later than the end of the first trimester. While some women, particularly those who have been pregnant before, may feel fetal movements toward the end of the first trimester, it's more common to experience quickening during the second trimester.
C. "This will happen once the uterus begins to rise out of the pelvis."
This response is not directly related to quickening. The rising of the uterus (fundus) out of the pelvic cavity is a physical change that occurs as the pregnancy progresses, but it doesn't signify the onset of fetal movements (quickening). Quickening is specifically about feeling the baby's movements, not the position of the uterus.
D. “This will occur during the last trimester of pregnancy."
This response is incorrect. Quickening typically occurs much earlier, specifically during the second trimester, around the 16th to 20th week of pregnancy. Waiting until the last trimester to feel fetal movements would be unusual and might prompt further evaluation or discussion with a healthcare provider.
Explanation
Explanation:
A. Shortly after giving birth
This timing is not recommended for rubella immunization during pregnancy. Rubella vaccination should ideally occur before conception or during the postpartum period, but not immediately after giving birth.
B. Immediately
Immunization for rubella is not typically recommended immediately during pregnancy. It is preferred to administer rubella vaccination before pregnancy or during the postpartum period.
C. During her next attempt to get pregnant
This option is closer to the recommended timing. Women who lack immunity to rubella should receive the rubella vaccine after giving birth but before attempting to get pregnant again. This approach helps ensure protection against rubella during future pregnancies.
D. In the third trimester
Administering rubella immunization during the third trimester of pregnancy is not recommended. Vaccination against rubella should ideally occur either before pregnancy or after delivery, as giving it during pregnancy can pose risks to the fetus.
Explanation
Explanation:
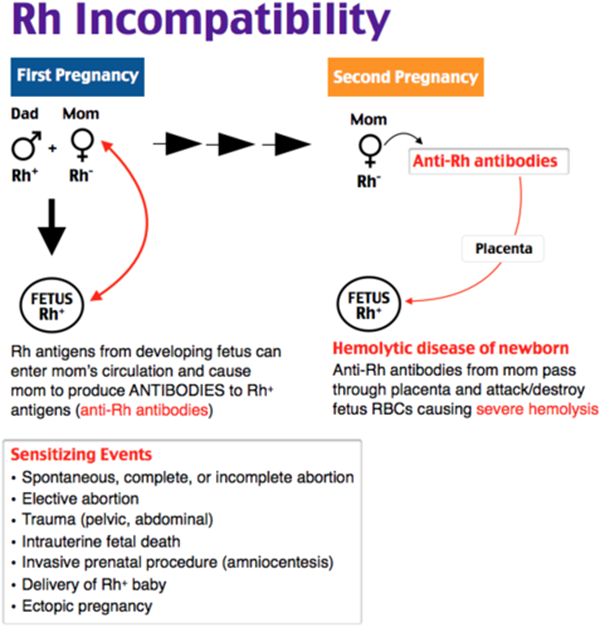
A. It destroys Rh antibodies in newborns who are Rh positive.
This statement is incorrect. Rh immunoglobulin does not destroy Rh antibodies in newborns. It is given to Rh-negative mothers to prevent the formation of Rh antibodies in response to exposure to Rh-positive fetal blood cells.
B. It destroys Rh antibodies in mothers who are Rh negative.
This statement is inaccurate. Rh immunoglobulin does not destroy Rh antibodies in mothers. Instead, it acts by binding and neutralizing Rh-positive fetal blood cells that enter the maternal circulation, preventing the mother's immune system from producing Rh antibodies against these cells.
C. It prevents the formation of Rh antibodies in newborns who are Rh positive.
This statement is not entirely correct. Rh immunoglobulin is administered to Rh-negative mothers to prevent them from developing Rh antibodies in response to exposure to Rh-positive fetal blood cells during pregnancy or childbirth. It does not directly prevent the formation of Rh antibodies in newborns.
D. It prevents the formation of Rh antibodies in mothers who are Rh negative.
This statement is accurate. Rh immunoglobulin works by preventing the Rh-negative mother's immune system from producing Rh antibodies against Rh-positive fetal blood cells. By doing so, it reduces the risk of Rh isoimmunization and its potential complications in subsequent pregnancies.
A nurse is instructing a woman who is contemplating pregnancy about nutritional needs. To reduce the risk of giving birth to a newborn who has a neural tube defect, which of the following information should the nurse include in the teaching?
Explanation
Explanation:
A. Limit alcohol consumption:
Alcohol consumption during pregnancy is associated with various risks, including fetal alcohol spectrum disorders (FASDs). However, in the context of reducing the risk of NTDs specifically, the focus is on nutritional factors, particularly folic acid intake, rather than alcohol consumption.
B. Consume foods fortified with folic acid:
This choice is the correct recommendation. Folic acid is crucial for the prevention of neural tube defects. Women of childbearing age, especially those planning pregnancy, are advised to consume foods fortified with folic acid or take folic acid supplements to ensure adequate intake before and during early pregnancy. This is a key preventive measure endorsed by healthcare professionals worldwide.
C. Increase intake of iron-rich foods:
Iron is important during pregnancy to prevent anemia and support fetal growth and development. However, iron intake is not directly linked to reducing the risk of neural tube defects. While overall nutritional health is essential during pregnancy, focusing on iron-rich foods alone does not specifically address the prevention of NTDs.
D. Avoid foods containing aspartame:
Aspartame is an artificial sweetener found in many foods and beverages. While there may be general recommendations regarding artificial sweetener consumption during pregnancy, avoiding foods with aspartame is not directly related to reducing the risk of neural tube defects. The primary focus for NTD prevention lies in adequate folic acid intake.
Explanation
Explanation:
G - Gravida: The number of pregnancies, including the current one.
T - Term births: The number of pregnancies carried to term, typically considered 37 weeks or more.
P - Preterm births: The number of pregnancies delivered between 20 and 37 weeks.
A - Abortions: The number of pregnancies terminated before 20 weeks, including elective abortions and miscarriages.
L - Living children: The number of living children.
Now let's analyze the client's history:
Elective abortion at 9 weeks (terminated pregnancy): This counts as an abortion (A).
Birth of twins at 36 weeks (term births): This counts as two term births (T).
Spontaneous abortion at 15 weeks (miscarriage): This also counts as an abortion (A).
Based on the information provided, the client's GTPAL status would be:
Gravida: 4 (1 terminated pregnancy + 1 twin birth + 1 miscarriage + 1 current pregnancy)
Term births: 2 (1 twin birth)
Preterm births: 0
Abortions: 2 (1 terminated pregnancy + 1 miscarriage)
Living children: 2 (1 twin birth)
Explanation
Explanation:
A. Congenital heart defects:
Smoking during pregnancy has been linked to an increased risk of congenital heart defects in newborns. Maternal smoking can affect the development of the baby's heart, leading to structural abnormalities in the heart's formation. These defects can range from mild to severe and may require medical intervention after birth.
B. Hearing loss:
Although there is some evidence suggesting a possible association between maternal smoking and hearing problems in children, the link is not as well-established as other complications such as intrauterine growth restriction or congenital heart defects. More research is needed to confirm the direct impact of maternal smoking on hearing loss in newborns.
C. Type 1 diabetes mellitus:
Maternal smoking during pregnancy is not directly linked to an increased risk of Type 1 diabetes mellitus in newborns. Type 1 diabetes is an autoimmune condition that is not typically influenced by maternal smoking during pregnancy.
D. Intrauterine growth restriction (IUGR):
This is the correct choice. Smoking during pregnancy is a well-known risk factor for intrauterine growth restriction (IUGR). It can lead to inadequate fetal growth and lower birth weight than expected for gestational age due to restricted oxygen and nutrient supply to the fetus. Babies born with IUGR may experience various health issues and developmental challenges.
You just viewed 10 questions out of the 47 questions on the Ati Concept Of Nursing Proctored Exam 2 Exam. Subscribe to our Premium Package to obtain access on all the questions and have unlimited access on all Exams. Subscribe Now



